How to prevent macular degeneration
Age-related macular degeneration (AMD) is the leading cause of irreversible vision loss in older adults. It can have debilitating effects, including severe visual and quality-of-life impacts. While there is no cure for AMD, taking preventive steps may reduce your chances of developing this disease.
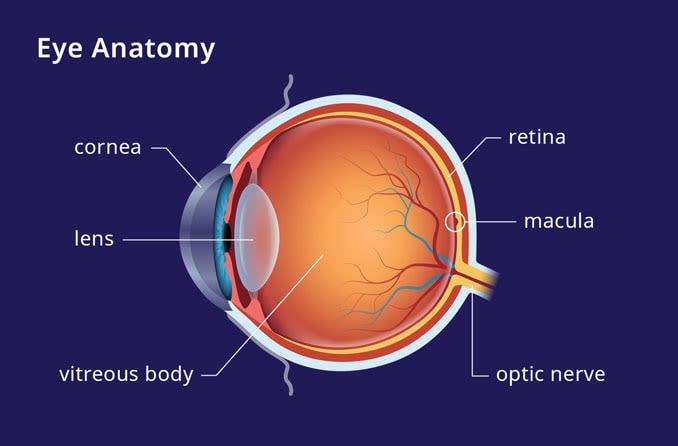
AMD causes the loss of central vision, which is responsible for helping you see in your direct line of sight. It does not affect peripheral vision (also referred to as side or indirect vision). The progressive loss of central vision impacts your ability to do everyday tasks. Such tasks include driving, reading, recognizing faces and seeing objects in fine detail.
Blind spots (scotoma) may develop, which can also impair your visual function. AMD may lead to legal blindness in some cases.
Taking steps to prevent the condition may help preserve your vision and maintain your quality of life. The first step in preventing macular degeneration is understanding factors that may contribute to its onset. Knowing your personal risks for developing AMD may also aid in its prevention.
Understanding AMD: Causes and genetics
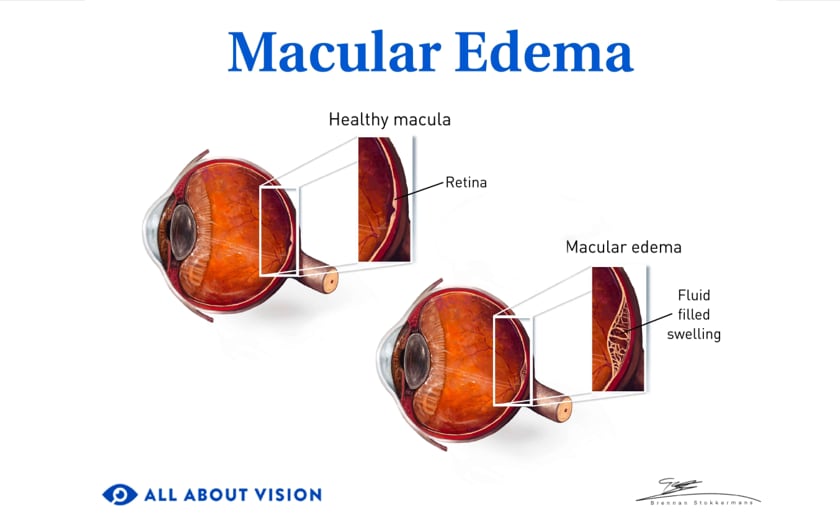
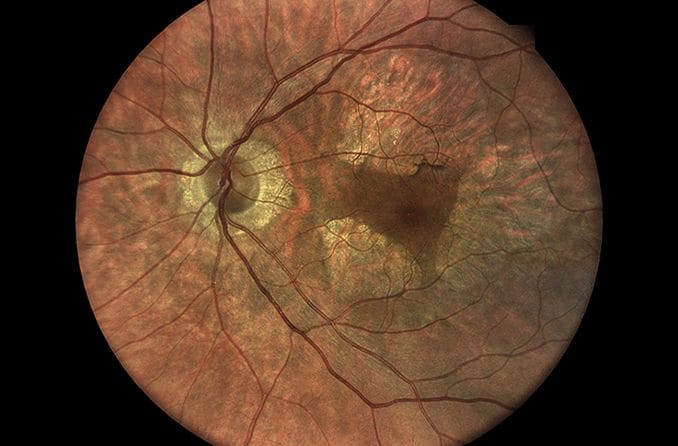
Age-related macular degeneration results from changes in or damage to the macula, the center part of the retina. AMD may occur in one of two general forms: dry AMD or wet AMD.
Although the exact cause of AMD is unknown, it has been linked to certain genetic, health, environmental and lifestyle factors. Some of these factors are modifiable, meaning they can be changed. Others are beyond your control and cannot be altered or improved.
Non-modifiable AMD risk factors
Some risk factors for age-related macular degeneration are genetic or otherwise unmodifiable. These include:
Age
Age is the primary risk factor for AMD. The disease is most common in those aged 50 and over.
Genetics
A person’s risk for developing AMD may be genetic. Macular degeneration can be hereditary and may run in families. You may be more likely to get the condition if a first-degree relative (such as a parent or sibling) has had it.
Ethnicity
The prevalence and risk of AMD are higher in white populations. Genetic, lifestyle and environmental factors may also influence AMD development in some ethnicities.
Gender
Age-related macular degeneration is slightly more common in women than men. This could be because women tend to live longer than men. Women are more likely to experience long-term inflammation, which could be a contributing factor to the onset of AMD. Other factors that may be related include changes in estrogen levels during menopause.
Modifiable AMD risk factors
Additional factors have been linked to AMD and may increase the chance of developing the condition. These are generally modifiable and include:
Smoking
Cigarette smoking may significantly increase the chance of developing AMD. If you smoke, your risk of experiencing AMD may be up to four times higher than that of a non-smoker.
Studies have been conducted to examine the link between AMD and cannabis smoking. Some researchers have found that smoking cannabis may lower the risk of macular degeneration. However, there is evidence to suggest that it could cause some people to get the condition at a younger age.
Physical activity
A lack of physical activity or a sedentary lifestyle is another risk factor for AMD. Studies indicate that regular exercise can boost your cardiovascular health. This, in turn, can help ensure an adequate supply of nutrients and oxygen for your eyes. Doing moderate-intensity activities (like brisk walking or ballroom dancing) at least three hours a week may lower your risk of AMD. You may need to consult your physician before beginning any new exercise routine.
Certain health conditions
Some medical conditions may increase the risk of age-related macular degeneration. These include:
High blood pressure (hypertension) – High blood pressure reduces blood flow in the vessels, including those in the eyes. This can prevent the proper delivery of vital nutrients to eye tissues. Hypertension may damage blood vessels in the retina, increasing the risk of AMD.
Cardiovascular disease – Cardiovascular disease (such as heart disease) impairs the flow of blood throughout the body, including to the eyes. This disruption in blood flow can lead to retinal damage and possibly macular degeneration.
High cholesterol – Studies have shown that high cholesterol may increase the chance of developing AMD. Cholesterol is a fatty substance found in the body. It can cause plaque buildup in the blood vessel walls, which blocks or reduces blood flow. Fragments of this plaque can detach and become lodged in small blood vessels throughout the body, including those in the retina.
Obesity – Obesity and being overweight may elevate the risk of AMD. Having a body mass index (BMI) over 30 can more than double the chance of experiencing the condition.
Sleep apnea – Sleep apnea is a medical condition that causes a person to stop breathing during sleep. It deprives the body of oxygen and may cause inflammation throughout the body. This process can then affect the blood supply in the retina. Researchers believe there could be a link between sleep apnea and certain types of dry AMD.
Ultraviolet light
Ultraviolet light (UV) from the sun or manmade sources can increase the risk of AMD. It can damage the retina, which can affect a person’s vision. The cumulative effect of UV exposure over time may be a factor in the development of AMD.
Other AMD risk factors
Inflammation
Inflammation within the body may play a role in both wet and dry AMD. It can damage tissues within the eye, leading to dry AMD. Inflammation has also been associated with the development of new abnormal blood vessels in and under the retina, found in wet AMD. Research is underway to see if anti-inflammatory drugs might reduce the inflammation associated with macular degeneration.
Pollution
People exposed to air pollution over the long term may have a higher chance of developing AMD. It is believed that air pollutants lead to oxidative stress and inflammation, which can damage the retina.
Alzheimer’s disease and dementia
Studies show that dementia may increase the risk of age-related macular degeneration. They have also found that AMD may elevate the chance of developing Alzheimer’s disease.
AMD has been linked to Alzheimer’s disease (a form of dementia) in numerous studies. Those with AMD seem to have a greater chance of developing dementia and Alzheimer’s disease.
Key strategies for macular degeneration prevention
Understanding your risks can help you take steps to prevent macular degeneration. The strategies below may also be helpful if you are seeking information on how to stop macular degeneration from progressing.
Dietary supplements and vitamins for AMD prevention
Taking vitamins and minerals may be good for many aspects of your health, including your eyes. Certain dietary supplements may be helpful for the prevention of macular degeneration.
Vitamins and minerals that may help prevent age-related macular degeneration include:
Lutein, zeaxanthin and beta-carotene (the precursor to Vitamin A)
Zinc
Selenium
Anthocyanins are another nutrient that may be beneficial for eye health. These are a type of flavonoid and are responsible for the rich pigmentation in blue, purple, black and red plant-based foods.
Certain supplements for macular degeneration interfere with some medications. The effects of this could be dangerous for your health. Be sure to speak with your doctor about potential health risks before taking nutritional supplements.
Your doctor can help determine which supplements are ideal for your needs or if you should take certain vitamins for macular degeneration prevention.

Certain nutritional supplements have been shown to help stop the progression of macular degeneration, or prevent it.
AREDS and AREDS2 nutritional supplements
If you already have AMD, certain dietary supplement formulations may help prevent its progression.
Two large clinical trials sponsored by the National Eye Institute studied the effects of specific vitamins and minerals on AMD and cataracts. These studies are known as AREDS and AREDS2. They found that certain nutritional supplements may lessen the risk or slow the progression of AMD. (The formulations did not have any significant effect on the development or progression of cataracts.)
The original AREDS formulation includes:
Vitamin C – 500 mg
Vitamin E – 400 IU
Beta-carotene – 15 mg
Zinc – 80 mg
Copper – 2 mg (as cupric oxide)
The second study aimed to determine if altering the original formula offered more benefits to AMD patients. Researchers changed the original formula based on AREDS2 results. The AREDS2 formula includes:
Vitamin C – 500 mg
Vitamin E – 400 IU
Lutein – 10 mg
Zeaxanthin – 2 mg
Zinc – 80 mg
Copper – 2 mg (as cupric oxide)
Lutein and zeaxanthin were added, as the research suggested they could lower the chance of AMD progression. Beta-carotene was removed from the original formula. (The research indicated that taking this supplement in high doses may raise the risk of lung disease in smokers.)
SEE RELATED: How to choose eye and vision supplements
Diet and nutrition for eye health
Diet and nutrition are factors to consider when exploring how to avoid macular degeneration. Modifying your dietary habits may help protect your eyes from this eye disease.
Eating foods rich in antioxidants may help with macular degeneration prevention and progression. These foods include:
Dark, leafy greens – Eating plenty of dark, leafy greens may help with macular degeneration prevention. These foods are often high in zeaxanthin and lutein. Examples include kale, spinach and collard greens.
Fish – Some studies have indicated that eating fish at least two times a week may lower the risk of developing AMD. Fatty fish is high in omega-3 fatty acids, which may aid in preventing macular degeneration. Examples of fatty fish include salmon and sardines.
Fruits and vegetables – Many fruits and vegetables are rich in antioxidants and may provide benefits for overall eye health. Eating fruits and vegetables that are yellow, orange and other vibrant colors may help reduce the risk of AMD.
Foods with a low glycemic index – Eating foods with a low glycemic index may help prevent macular degeneration. These include items like brown rice, whole-grain bread, oatmeal, nuts and sweet potatoes.
Following the Mediterranean diet may also be helpful in age-related macular degeneration prevention. This diet, centered around plant-based foods and seafood, includes items such as:
Whole grains
Healthy fats
Vibrantly colored fruits
Green, leafy vegetables
Lentils
Tree nuts
Moderate amounts of dairy
Fish high in omega-3 fatty acids
READ MORE: 5 fish oil benefits for eye and vision health
Lifestyle changes to reduce the risk of AMD
Preventing macular degeneration involves reducing your chance of developing the disease. Some factors, such as genetics, ethnicity and gender, cannot be altered. However, others may be modified by adopting a healthier lifestyle or avoiding certain risks.
Quit smoking
Quitting smoking is important for all aspects of your health, including your eyes. Tobacco contains thousands of highly toxic chemicals, which damage tissues throughout the body. Individuals who smoke and who have certain genes may be even more susceptible to developing AMD. This makes quitting smoking important for preventing macular degeneration. Your doctor can help you develop a plan for smoking cessation.

If you are a smoker, stop now. Smoking is a major risk factor for developing macular degeneration.
Eat a healthy diet
Eating a healthy, balanced diet can benefit your eyes and general health. Ensuring your diet is rich in nutrients like antioxidants (like Vitamins A, C and E), omega-3 fatty acids, whole grains and the minerals copper and zinc can help support your eye health. Avoiding fatty, sugary or processed foods may lower your chance of AMD.
Get plenty of exercise
Exercising regularly and getting heart-healthy, aerobic physical activity may help prevent macular degeneration or its progression. Leading an active lifestyle promotes blood flow throughout your eyes and the rest of your body, supporting your cardiovascular health.
Maintain a healthy weight
Since obesity is a risk factor for AMD, maintaining a healthy weight may help prevent the onset of the condition. This can also lower the risk of other conditions associated with AMD, such as high blood pressure, heart disease and sleep apnea.
Control high blood pressure and cholesterol
Taking steps to control high blood pressure and cholesterol levels is another way to help prevent macular degeneration. This may improve blood flow through the vessels in your eyes and reduce your chance of AMD. See your physician to determine the best way to keep your blood pressure and cholesterol in check.
Protect your eyes from UV radiation
Wearing sunglasses that block 100% of UVA and UVB rays can aid in age-related macular degeneration prevention. Sunglasses that have a darker tint and wrap around the sides of your eyes offer additional benefits. Wearing a wide-brimmed hat in addition to sunglasses can block the overhead sun and further protect your eyes from UV rays.
There may be other steps you can take to protect your eye health and vision. See your eye doctor for more on how to reduce your risk of macular degeneration.

The importance of regular eye check-ups
People at risk of AMD often ask questions like “Can you prevent macular degeneration?” or “Can you stop the progression of macular degeneration?” A key step in understanding how to reduce your macular degeneration risk is to have your eyes examined regularly. Most cases of the disease develop slowly, and symptoms may not be noticeable until it advances.
Getting regular eye exams is important for your overall eye health. In fact, the American Optometric Association recommends having comprehensive eye exams each year. Exams may be recommended more frequently for those with certain eye conditions or who are at a higher risk for eye disease.
Routine eye exams allow your eye doctor to diagnose conditions like macular degeneration as early as possible. Your eye doctor can also help you identify steps to preserve your vision if you are diagnosed with AMD.
During the exam, your eye doctor may use various techniques to screen for AMD. These techniques include:
Pupil dilation – Special eye drops are placed in your eyes to dilate your pupils. This allows your eye doctor to evaluate your macula, retina and other eye structures.
Optical imaging – Various imaging techniques, such as optical coherence tomography, may be used to take pictures of the retina and macula. Optical imaging allows your doctor to see detailed pictures of your eye to look for signs of AMD.
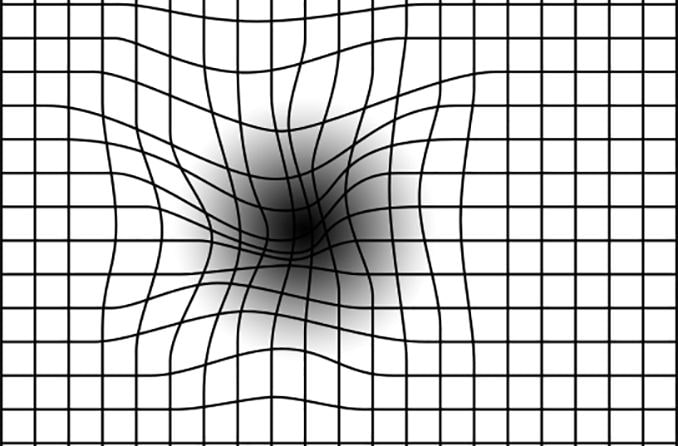
Amsler grid test – This test involves an eye chart that looks like graph paper with a dot in the center. If the lines in the grid appear distorted or wavy, it could indicate the presence of macular degeneration.
If you are diagnosed with AMD, your eye doctor may suggest monitoring your vision at home with a daily vision check. Your doctor may provide you with an Amsler grid chart, or you can download one online and print it for use at home.
To use the Amsler grid at home, position the chart about 12-14 inches away from your face, wearing your reading prescription. Cover one of your eyes and look directly at the dot in the grid with the other eye. Repeat the process with the other eye. If any of the lines look blurry, wavy or distorted, contact your eye doctor promptly, as this could be a sign that AMD is worsening.
SEE RELATED: Treating age-related macular degeneration
Latest research and findings on AMD prevention
Research is being conducted to identify ways to prevent macular degeneration and its progression. Through ongoing studies, researchers seek to better understand how AMD develops, which could help develop prevention methods.
Retinal injury and recovery
One such study involves replicating the process of retinal damage from focused light. Performed in a lab setting, this approach may help researchers better understand how such damage affects retinal cells. The hope is that the results of the study lead to the development of preventive measures.
Gene therapy
Gene therapy is another potential way to prevent macular degeneration. This approach encourages the eye to produce anti-VEGF medication on its own. Researchers are exploring gene therapy to better understand how AMD develops and if it might prevent or slow the progression of AMD. Gene therapy is currently being studied for the treatment of macular degeneration.
Metformin
Another recent AMD prevention approach involves the use of metformin. This drug is largely prescribed to treat type 2 diabetes but has been used off-label for several other health conditions. There is some evidence that metformin has anti-aging properties, which is the mechanism under study for age-related macular degeneration prevention.
Artificial intelligence/Machine learning
Artificial intelligence (AI) is also being developed as an AMD prevention tool. Machine learning models may be able to help predict AMD development and progression. This could allow for timely intervention and the potential for slowing the advancement of the disease.
These models combine data such as retinal images, environmental factors and genetics. At least three of them have shown promise in early studies:
iPredict, developed by iHealthScreen
A yet-unnamed prototype developed by the NIH
Orusight, developed by RetiNov
Using specialized algorithms, they’ve been able to predict late AMD with high-level accuracy.
The NIH prototype and iPredict designs are only for in-clinic use by physicians. But RetiNov plans to launch an interactive digital platform for use with Orusight. Users would be able to learn more about their risk, motivating them to take preventive action.
In addition to AMD prevention, researchers hope to find more effective ways to treat the disease and lower the chances of vision loss.
Raising awareness about AMD
The month of February is dedicated to raising awareness of age-related macular degeneration. The American Academy of Ophthalmology takes this opportunity to increase awareness of AMD and remind individuals that detecting the disease early on is the first step in protecting their sight.
Even outside of this time of year, you can take steps to learn about AMD and lower your disease risks. Visit an eye doctor for more on how to prevent macular degeneration and its progression.
READ NEXT: 8 ways to protect your eyesight