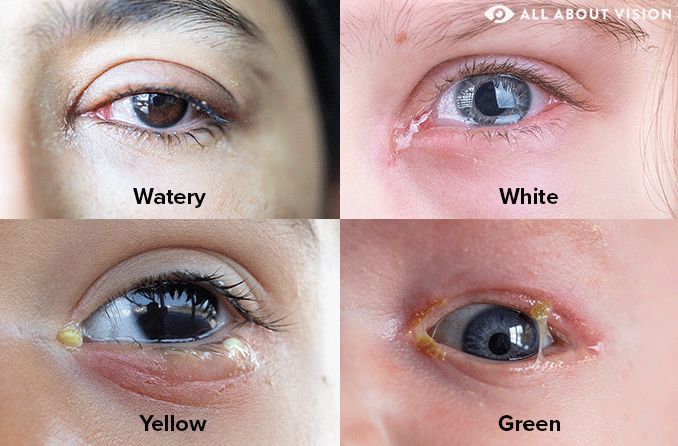
Eye discharge (also called eye boogers, goop, gunk and sleep) in small amounts is a normal part of having healthy eyes. While it’s common to wake up to a bit of eye mucus in the corner of your eyes, it might be time to schedule a doctor’s appointment if the discharge changes in color, consistency or amount.
Normal discharge
A small amount of clear, white or ivory-colored eye discharge is considered normal (as long as it isn’t sticky). This is the product of your tear film clearing the surface of your eyes from dust and other cellular debris. Some of this discharge may be the oil and mucus of the tear film that remains after the watery component of your tears evaporates.
Watery discharge
Excessive watery discharge , referred to as “reflex tearing,” is the temporary overproduction of the watery component of normal tears that is used to flush away:

- Irritants, such as chemicals or pollutants
- Allergens, such as pollen or pet dander
- Dryness from wind, arid environmental conditions or dry eye syndrome
While reflex tearing is a normal bodily defense mechanism used to flush the eyes clear or alleviate acute dryness, having excessively watery eyes should be temporary and not occur frequently.
White discharge

Green or yellowish-green discharge is also typically the result of a bacterial infection, such as bacterial keratitis, bacterial conjunctivitis, stye or periorbital cellulitis (a bacterial infection of the eyelids and tissues around the eye). Infection (and associated discharge) may be related to scratches or abrasions to the cornea, contact lens wear or other underlying causes.
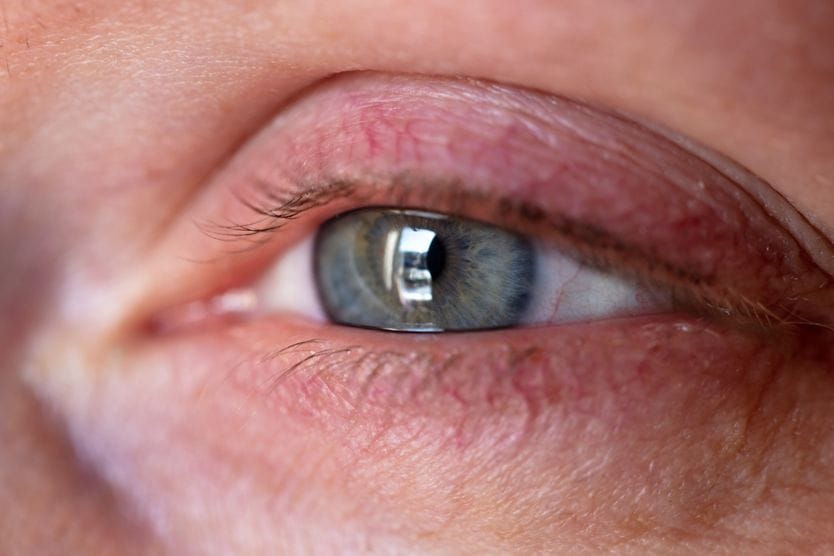
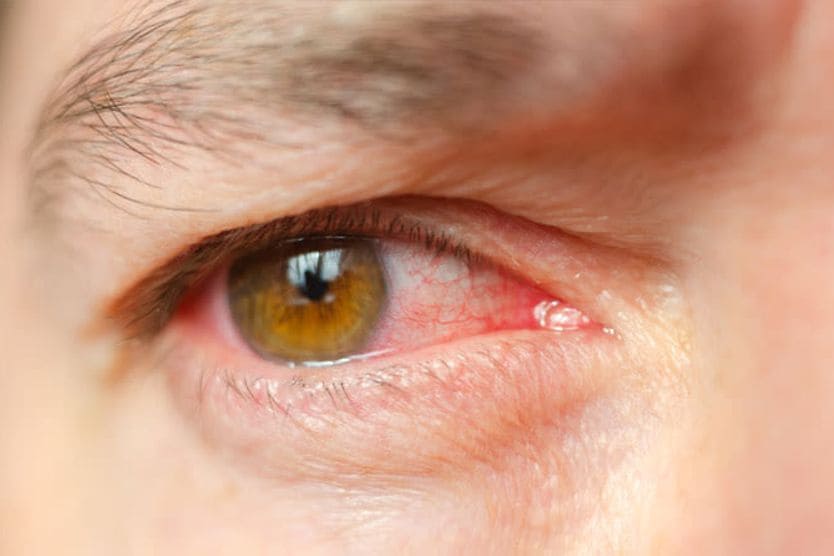
In addition to causing thick, sticky, green discharge , bacterial eye infections can also cause eye redness , sensitivity to light , swollen eyelids and excessive tearing, along with dried discharge on the eyelashes and eyelids.
Yellow discharge
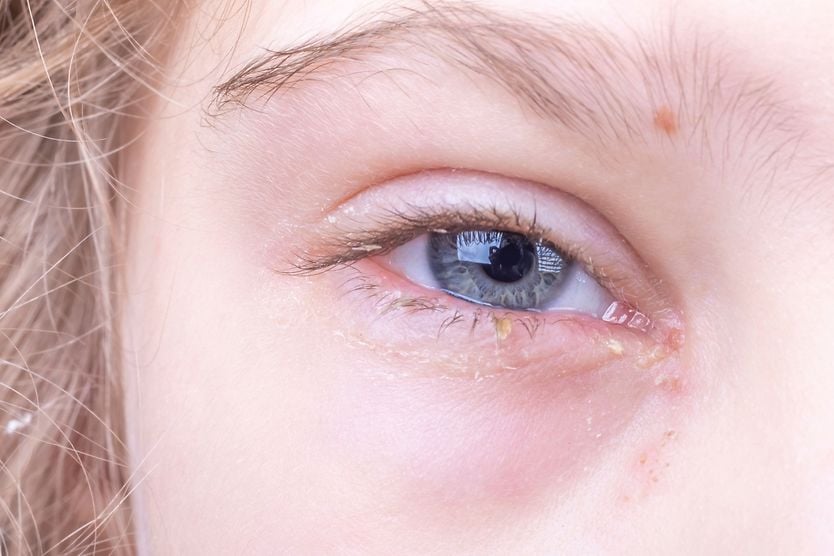
Yellow discharge is usually due to bacterial infection, which may accompany tear duct obstruction, blepharitis, meibomian gland dysfunction, a stye or bacterial conjunctivitis.

Yellow or white mucus balls in watery tears are often a sign of dacryocystitis , an infection of the tear duct or tear drainage system. Other symptoms may include eye redness, facial pain and drainage from the puncta (the opening of the tearduct). If this condition is not treated quickly with antibiotics, it can become serious.
Crusty debris or flakes along the base of the eyelashes may be a symptom of blepharitis — inflammation that occurs when there is excess oil or bacteria around the eyelids — or meibomian gland dysfunction .
The appearance of yellow mucus may be the sign of a stye — a painful red bump that develops on or under the eyelid when eyelash follicles or oil glands get clogged and infected. The yellow spot in the center of the stye — which sometimes looks like a pimple — can contain yellow pus, but don’t try to pop it! Most styes resolve on their own, but if popped, the infection can spread.
Thick yellow discharge may be caused by bacterial conjunctivitis, which is very contagious. This discharge is often sticky and may also appear white or green.
Green discharge
At-home care
If you notice any changes in your eye discharge, it’s important to limit any possible infection or damage. You should:
- Wash your hands thoroughly and frequently.
- Avoid touching your eyes and face.
- Stop wearing contact lenses and makeup.
- Wash pillowcases, bedding and washcloths in hot water on a regular basis, and refrain from sharing these articles with others.
- Never wear contacts for longer than prescribed.
Following these protocols will help address any current infection, keep it from spreading further and help avoid new issues.
When to call a doctor
If you notice any significant increase in discharge from your eyes, it could be an indication of something serious. If it doesn’t clear up in a day or two, see an eye doctor for evaluation and treatment.
If you also experience eye pain or blurry vision , see your eye doctor immediately.