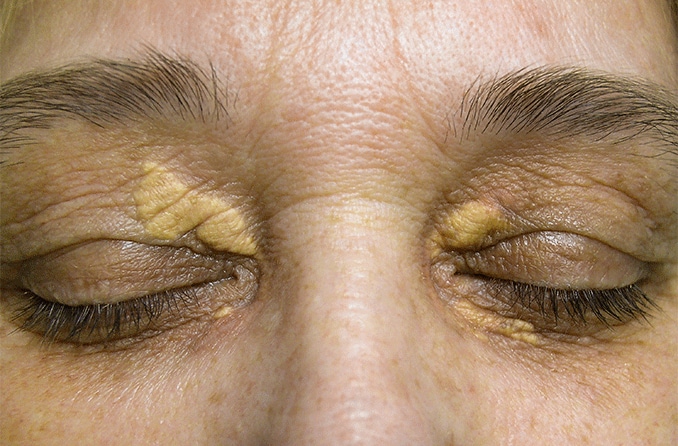
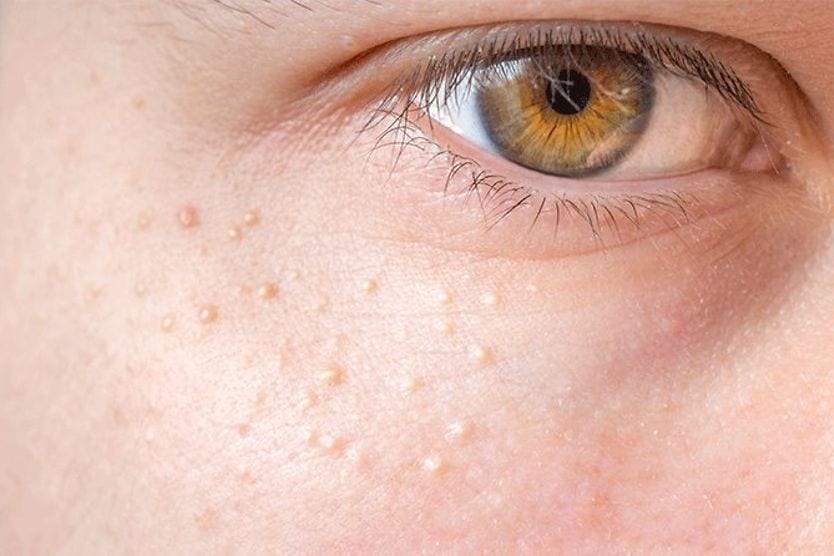
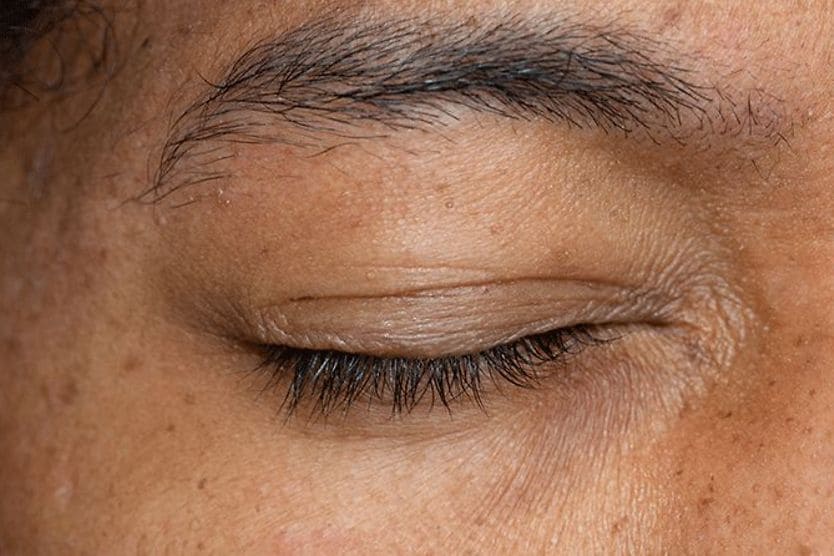
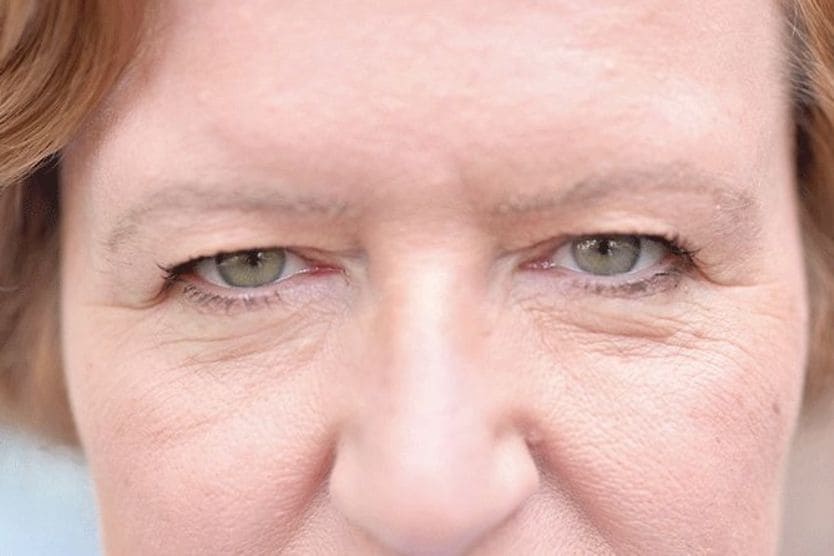
Xanthelasma (pronounced "zan-thuh-LAZ-muh") is a condition characterized by soft, yellowish growths that develop on the eyelids and around the eyes. These growths consist of fat deposits that collect under the skin and form a raised, bumpy patch.
While xanthelasmas alone are not dangerous, painful or irritating, their presence may indicate a more serious underlying condition.
Xanthoma vs. xanthelasma
Xanthoma (pronounced “zan-THOE-muh”) is the term used to describe the accumulation of cholesterol or fat beneath the skin.
Xanthomas can vary in size — from the tip of a pen to the size of a grape. They may appear as a single growth, or as multiple growths that cluster together to create a bumpy, textured appearance.
Xanthomas can appear anywhere on the body, though the more common locations include:
- Hands
- Feet
- Heels
- Buttocks
- Behind knees and elbows
Xanthelasma is a common subtype of xanthoma that develops around the inner portion of the eyelids, near the nose. Xanthelasmas are typically small and, though they can be raised, do not protrude as dramatically as xanthoma.
Xanthelasma causes
Many people who exhibit xanthelasma suffer from a lipid disorder. Lipids, also known as cholesterol, are fats that circulate through your bloodstream. There are two types: low-density lipids (“bad” cholesterol) and high-density lipids (“good” cholesterol).
Low-density lipids (LDL) make up the majority of your cholesterol. High LDL levels can raise your risk of xanthelasma, stroke and heart disease.
High-density lipids (HDL) work by absorbing LDL and carrying them to the liver, where they’re flushed from the body. Having high levels of HDL lowers your risk for stroke, heart disease and xanthelasma.
High levels of LDL or low levels of HDL are typically responsible for xanthelasma development. Lipid abnormalities can result from:
- Metabolic disorders that affect how fats are processed within the body.
- Genetic conditions that cause the body to produce too much LDL or too little HDL.
- Consuming excessive amounts of saturated fats.
- Inactivity.
Risk factors
While xanthelasma can affect anyone, the risks of developing the condition are greater if you:
- Have abnormally high lipid levels.
- Are obese.
- Are diabetic.
- Have high blood pressure.
- Are a woman.
- Smoke.
- Are between 30 and 50 years old.
- Have Asian or Mediterranean ancestry.
It’s important to note that you may have one or more of these traits and never develop xanthelasma. However, the presence of these characteristics puts you at a higher risk.
Diagnosis
Diagnosing xanthelasma is fairly simple, as the symptoms of the condition are visible. In fact, xanthelasma is frequently diagnosed because the patient notices it themselves and brings it up to the eye doctor.
Your doctor will examine the skin around your eyes to make an official diagnosis. They may also choose to draw blood and run some tests to assess your lipid levels.
Xanthelasma treatment
Treatment for xanthelasma is typically sought for cosmetic reasons, as the pockets of fat are not harmful and rarely affect vision. However, it’s possible for ptosis (droopy eyelids) to develop if the xanthelasma grows and begins to weigh on the eyelid.
Because xanthelasma removal is considered a cosmetic procedure, it is recommended to check with your eye doctor's office to understand insurance coverage.
Xanthelasmas can be removed using the following methods:
Medication – Studies have shown a prescription medication called simvastatin can successfully lower cholesterol levels, which may alleviate xanthelasma.
Chemical peels – A non-invasive treatment that removes the top layer of skin and reveals new skin cells below.
Laser surgery – A specific method of laser resurfacing called fractional CO2, which removes layers of tissue.
Chemical cauterization – A topical treatment using chlorinated acetic acids to create proteins and dissolve lipids, essentially dissolving the xanthelasma.
Electrodesiccation – An electric needle is used to scrape or burn off xanthelasma.
Cryotherapy – A procedure where xanthelasma is frozen off using liquid nitrogen or other chemicals.
Conventional surgery – A surgeon uses a knife or scalpel to remove the xanthelasma.
While these methods can successfully remove xanthelasma, it’s important to note that each of the procedures can cause some level of scarring. Also, it’s very possible for xanthelasma to reoccur or to develop elsewhere after these procedures are performed.
For best results, it’s important to consult with an oculoplastic surgeon, dermatologist or cosmetic surgeon who is experienced in performing these procedures.
Xanthelasma prevention
Preventing xanthelasma may be difficult for individuals who are genetically predisposed to having high cholesterol. However, there are steps that can be taken to lower your cholesterol and your risk of developing xanthelasma, including:
- Quitting (or avoiding) smoking.
- Limiting your alcohol intake.
- Reducing your consumption of saturated fats, such as milk, butter, baked goods and processed meats like sausage and bacon.
- Consuming foods that contain “good” cholesterol, such as whole grains, beans and legumes, olive oil and fatty fish.
- Maintaining a healthy weight.
- Exercising for a minimum of 30 minutes per day with moderate to vigorous activity.