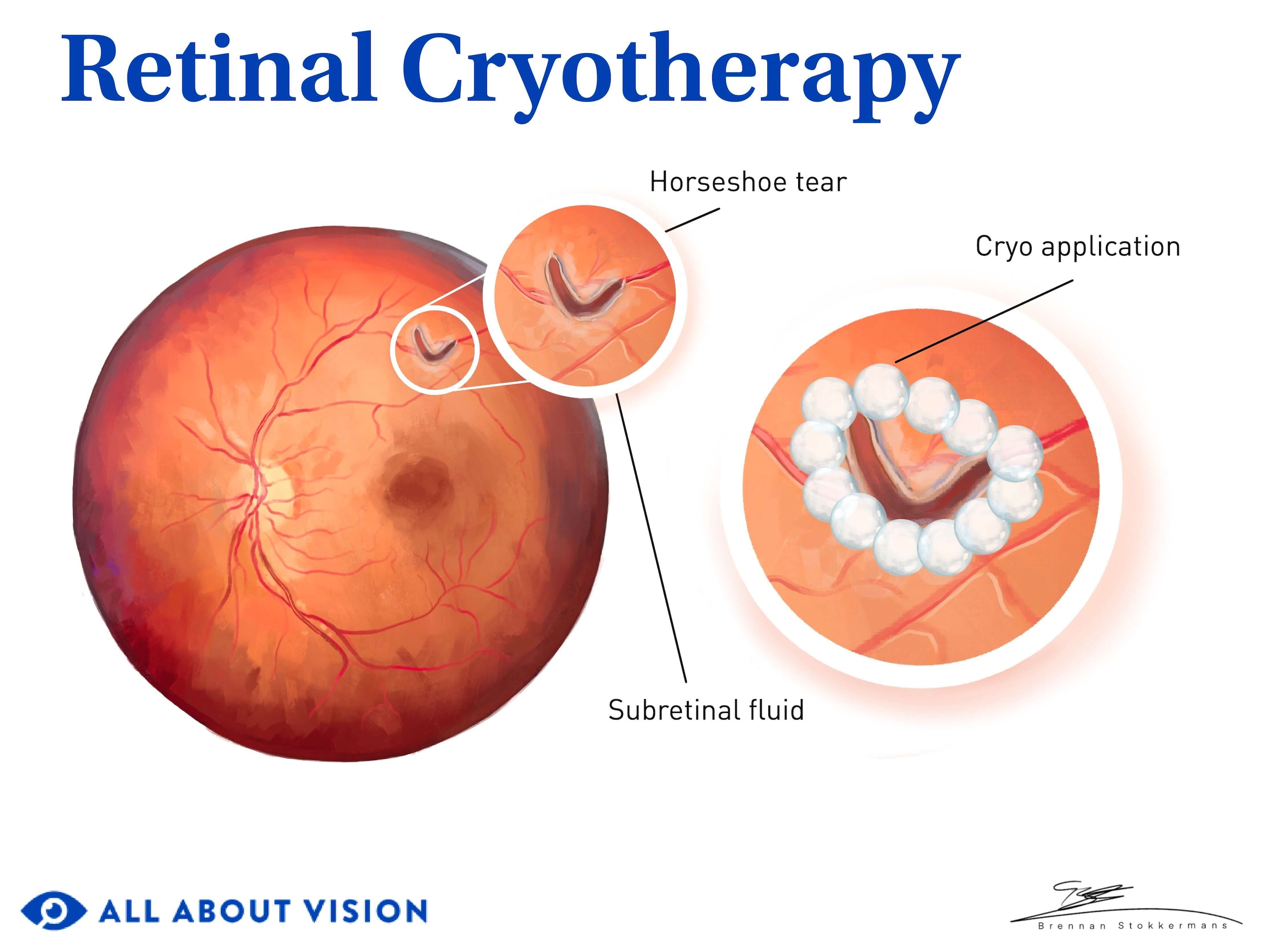
What is cryopexy (retinal cryotherapy)?
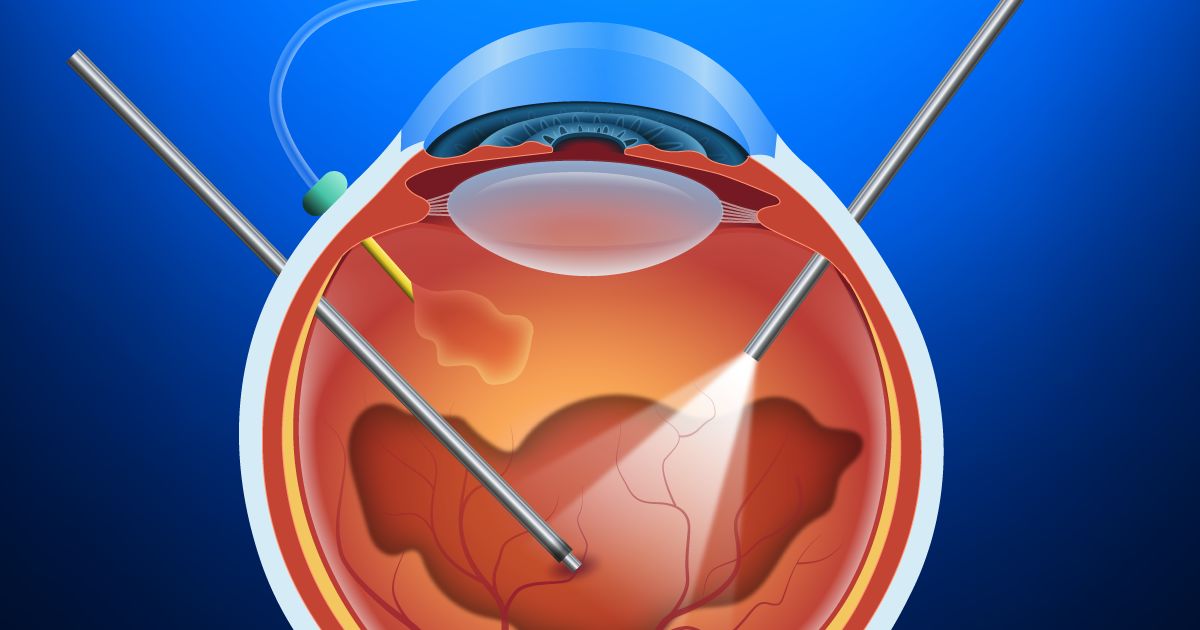
Cryopexy is a procedure to seal retinal tears or holes. A nitrogen-cooled probe is applied to the outside of the eye to freeze the area near the break. It stimulates scar tissue and creates an adhesion to the underlying layer. This helps reattach the retina and prevent fluid from leaking underneath.
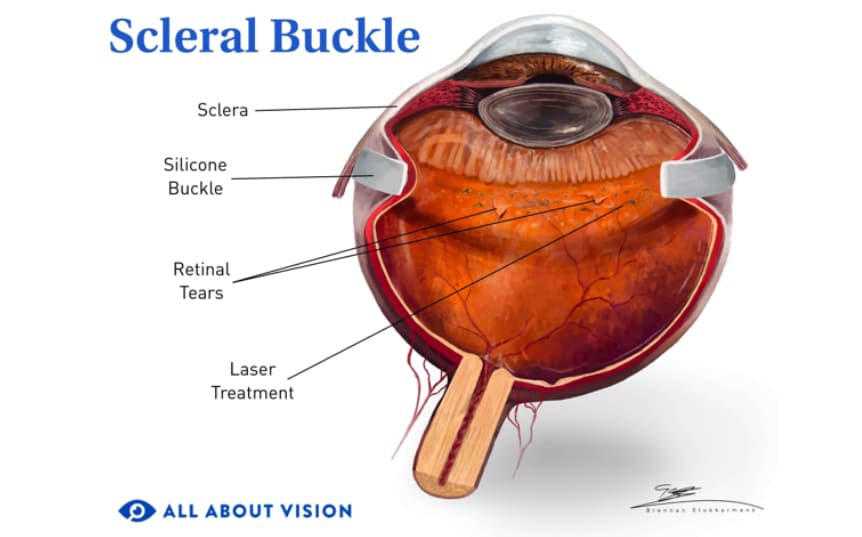
Cryopexy is also sometimes called retinal cryotherapy. It may be performed alone or with other procedures, such as pneumatic retinopexy, laser retinopexy (retinal laser photocoagulation) or scleral buckle surgery.
READ MORE: Laser photocoagulation eye surgery: Uses, benefits and what to expect
If retinal cryotherapy is performed without an additional surgery that requires an incision, it is typically an outpatient procedure. The sealing adhesions that result from cryopexy take about one to two weeks to form. People who undergo the procedure should avoid strenuous activity during that time.
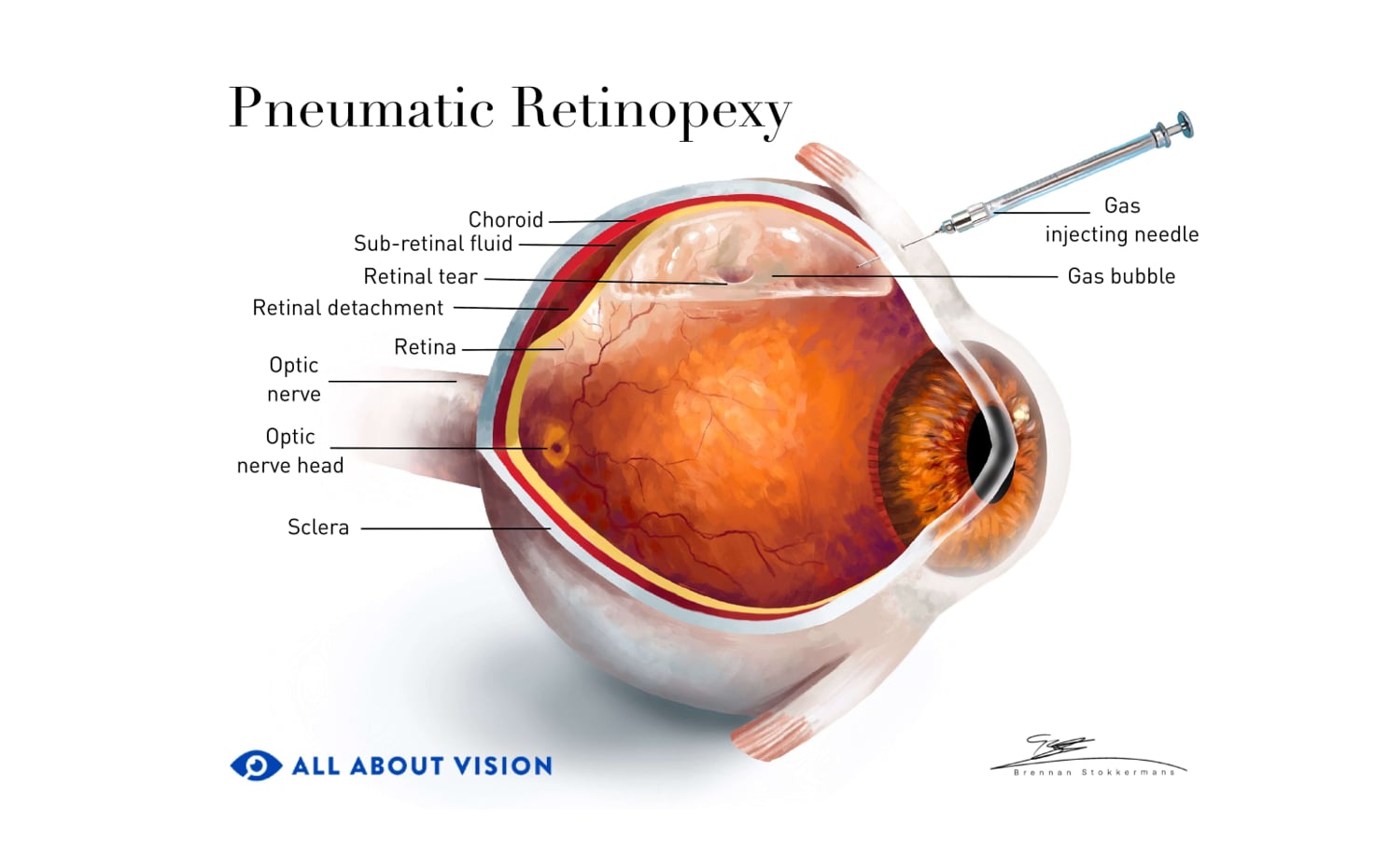
In cases of retinal detachment, a two-step treatment may be performed in which cryopexy (or in some cases laser retinopexy) is used to seal a retinal break in addition to a pneumatic retinopexy procedure. This is an in-office procedure that uses a gas bubble to provide pressure against the retina, promoting reabsorption of fluid under the retina, helping it to reattach.
Why do I need cryopexy?
Eye doctors recommend retinal cryotherapy to keep a retinal break, such as a retinal tear or hole, from progressing to a retinal detachment. It may also be used to treat small retinal detachments. Your eye doctor will evaluate whether to treat a tear or hole or monitor it closely. Depending on the location and severity, treating a retinal break early may decrease the risk of future complications.
A retinal tear or hole is a break or rip in the retina. The retina is the layer of tissue at the back of the eye that contains specialized nerve cells that turn light entering the eye into signals that are sent to the brain. Your eye doctor will determine whether to treat a retinal break or monitor it depending on several factors such as location, size and severity.
Retinal tear
An eye injury can cause a retinal tear. But in most cases, tears occur when the vitreous — a clear, gel-like substance in the back of the eye — pulls on the retina and tears it. With age, the vitreous shrinks and eventually separates from the retina. This is common as you get older — most people have it by age 70. This is called a posterior vitreous detachment, or PVD. Typically, a PVD does not cause any issues. In some cases, however, the vitreous can stick and tear the retina when it pulls away.
Retinal hole
Retinal holes can also sometimes occur due to a PVD. In addition, some people have areas of thinning, known as lattice degeneration, at the edges of their retina. These areas of thinning can sometimes develop into a retinal hole. Typically, retinal holes and lattice degeneration do not cause vision symptoms and are only detected during a dilated eye examination.
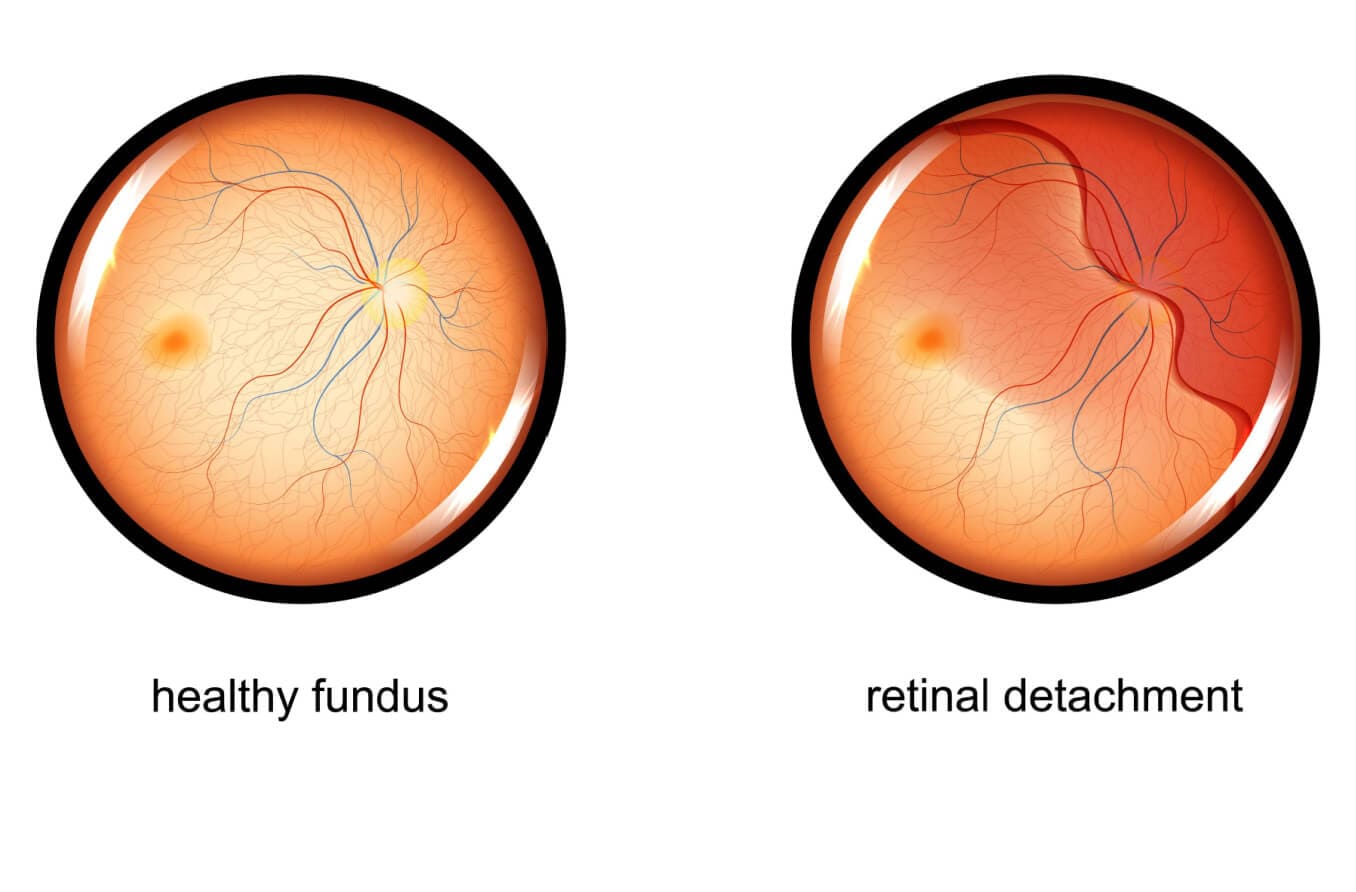
Rhegmatogenous retinal detachment
An untreated break in the retina may lead to detachment and blindness. Specifically, a retinal break is treated to prevent a rhegmatogenous retinal detachment, which can lead to severe vision impairment — especially when it is in the central retina.
This type of detachment occurs when a tear or hole allows fluid to seep underneath the retina. This can cause the retina to peel away from the choroid — the nourishing tissue that lies beneath it. When it peels away from the choroid, the retina is starved of nourishment and can become permanently damaged, leading to vision loss.
READ MORE: Scleral buckle surgery: Everything you need to know
What are the treatment options for retinal holes and tears?
Retinal breaks, such as a tear or a hole, can generally be treated with two types of in-office procedures that have similar results:
- Cryopexy (retinal cryotherapy) – This procedure uses a probe to freeze and damage the tissue surrounding a retinal break, stimulating the development of scar tissue to seal the area and reattach the retina into place.
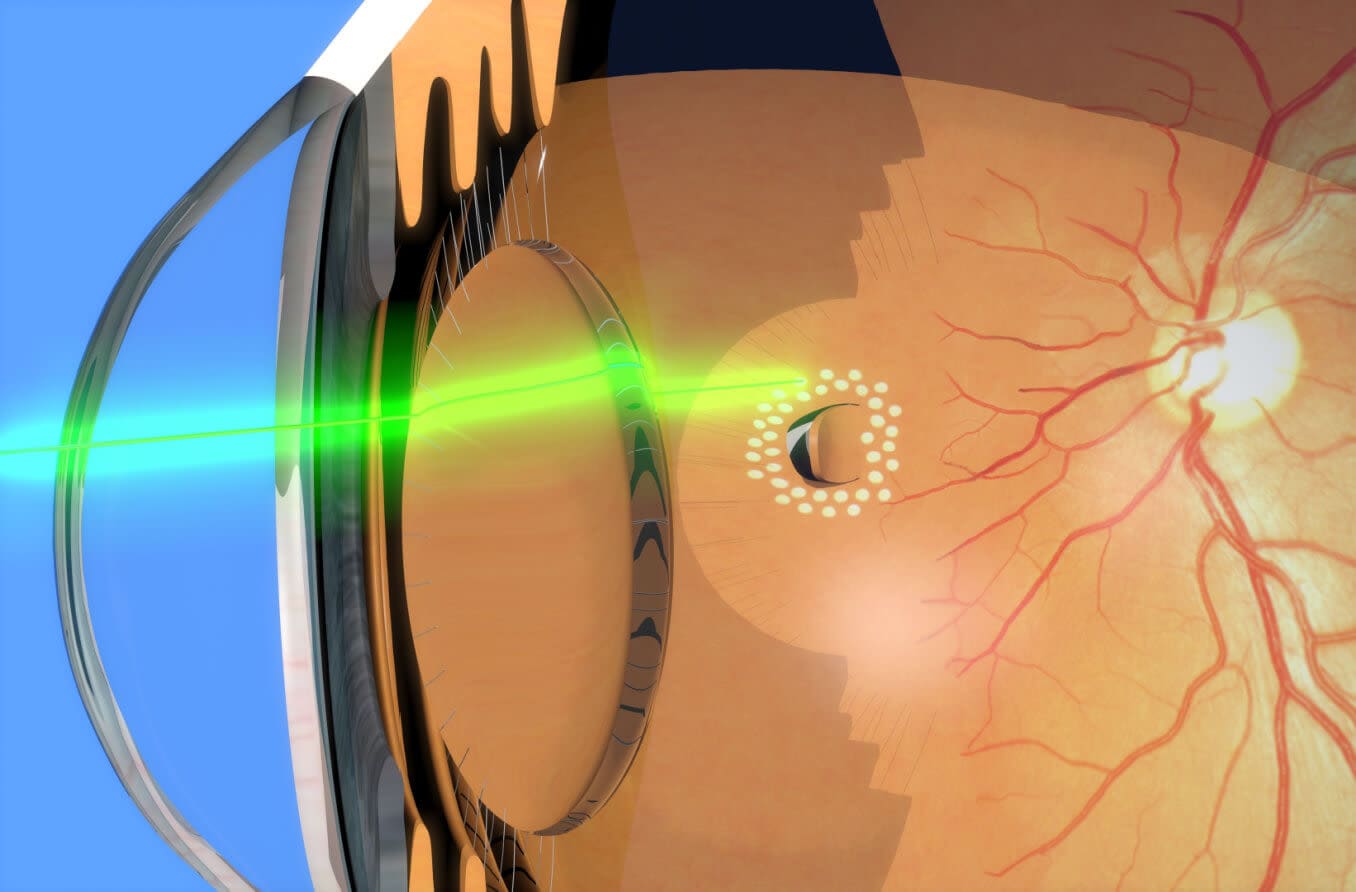
- Laser retinopexy (retinal laser photocoagulation) – This procedure uses a laser to generate heat and damage the tissue surrounding a retinal break, stimulating the development of scar tissue to seal the area and reattach the retina into place.
Both are non-invasive outpatient procedures and do not require an incision. They are usually performed at an ophthalmology office or clinic.
Why does my doctor recommend cryopexy?
If a retinal hole, tear or small detachment is detected, your eye doctor will determine the appropriate procedure or procedures to treat it. There are advantages to each type of procedure, and your eye doctor will recommend the treatment that is most likely to seal the break or reattach the retina successfully.
Your surgeon will consider factors such as:
- The location and configuration of the break
- The size of the break
- How visible the break is
- What type of eye surgeries you have had in the past
It may be easier to perform retinal cryopexy for breaks in the peripheral retina or if a laser cannot reach the hole or tear.
READ MORE: Retinal detachment: Symptoms, causes and treatment
What can I expect during a cryopexy procedure?
If retinal cryotherapy is the only treatment necessary, it can be performed at an ophthalmology office or clinic. The treatment may take about 10 to 15 minutes. Because the procedure does not require an incision, you should be able to return home the same day after a period of in-office recovery.
How to prepare for the procedure:
- Make sure to arrange for someone to accompany you to the doctor’s office and drive you home.
- Arrange for someone to help you at home if needed.
- Stop taking any medication that you have been told to discontinue before surgery.
- Limit your intake of food and liquids as advised by your eye doctor.
What to expect during the procedure:
Cryopexy is sometimes performed as part of a two-step process with pneumatic retinopexy.
If cryopexy treatment alone is required, the procedure will generally follow these steps:
- Your eye doctor will explain the procedure to you and ask if you have any questions.
- You will be given eye drops to dilate the eye and another to numb the eye, as well as a local anesthetic injection.
- Your doctor will use a specialized instrument called a binocular indirect ophthalmoscope (BIO) to see the retina at the back of the eye. It allows them to locate the exact area where the cryoprobe should be placed for treatment.
- A cryoprobe will be placed on the outside of your eye around the location of the retinal tear or hole.
- The eye doctor will turn on the cryoprobe and freeze several areas around the retinal break to seal it.
- You may experience a freezing sensation or discomfort while the cryoprobe is on.
Note that children will typically require a general anesthetic for this procedure. The treatment should take less than an hour, but they will need to stay in the hospital overnight.
What is recovery from cryopexy like?
After the treatment, your eye doctor may put an antibiotic ointment in the eye to prevent infection, and they may provide a patch for the eye. They may also prescribe topical steroid drops. This will help prevent inflammation.
You should rest after the procedure. This will help your eye to heal and form strong adhesions that will seal the break and reattach the retina. After the procedure, you may experience a continuing feeling of cold in the eye or a headache caused by the freezing sensation. If you experience a headache or discomfort, take an over-the-counter painkiller or apply a cold compress.
For a few days after the procedure, you may continue to have increased sensitivity and blurry vision. Your eye may look red and puffy for a few weeks. This is normal and will go away on its own.
Recovery usually takes about one to two weeks, during which you should avoid vigorous activity or heavy lifting. You may then resume your normal daily activities.
What are the risks and complications of cryopexy?
There is a chance of complications with any surgery. Your eye doctor will discuss the specific complications that you may be at risk for. In general, since cryotherapy does not require an incision, most people recover fairly quickly, within a week or two. There is typically a low risk of complications, such as unexpected damage to the tissue surrounding the treated area.
However, if you notice any of the following symptoms after your procedure, contact an eye doctor immediately:
- A dark curtain falling across your vision
- A total loss of vision or sudden onset of blurry vision
- A sudden onset of — or increase in — floaters (dark spots appear across your vision)
- Flashes of light
When to contact your doctor
Follow your eye doctor’s recommendations and ensure that you go to all scheduled follow-up appointments so that your doctor can monitor your progress. In some cases, more than one cryopexy procedure may be required.
It is normal to experience a headache or slight discomfort after the surgery and to have swelling and redness for a week or two after cryopexy. Contact your eye doctor right away if you notice any of the unusual symptoms listed above. If you have additional questions about the recovery process, contact your doctor’s office so they can address your specific concerns.
READ MORE: Types of eye surgery and the conditions they treat