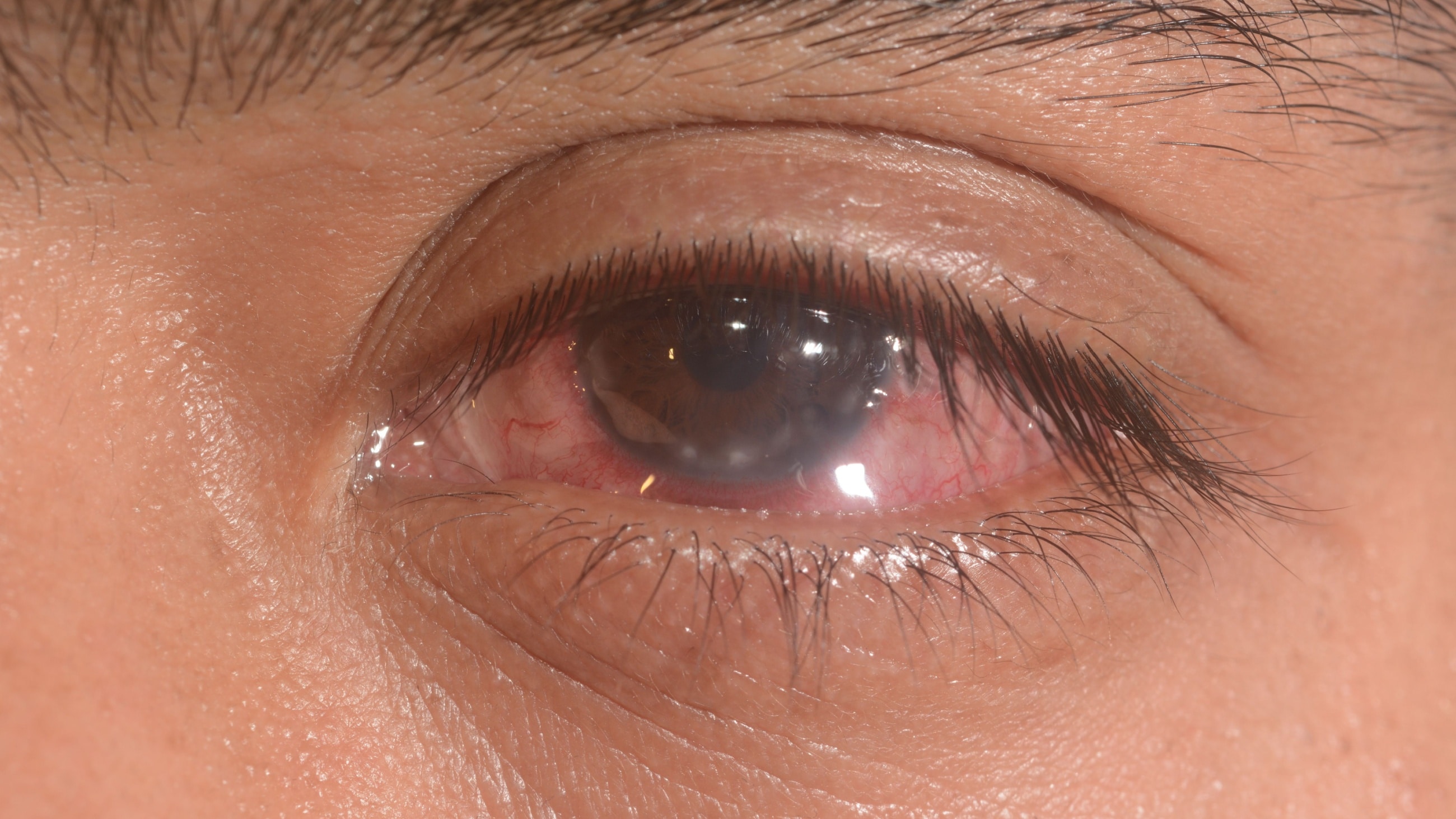
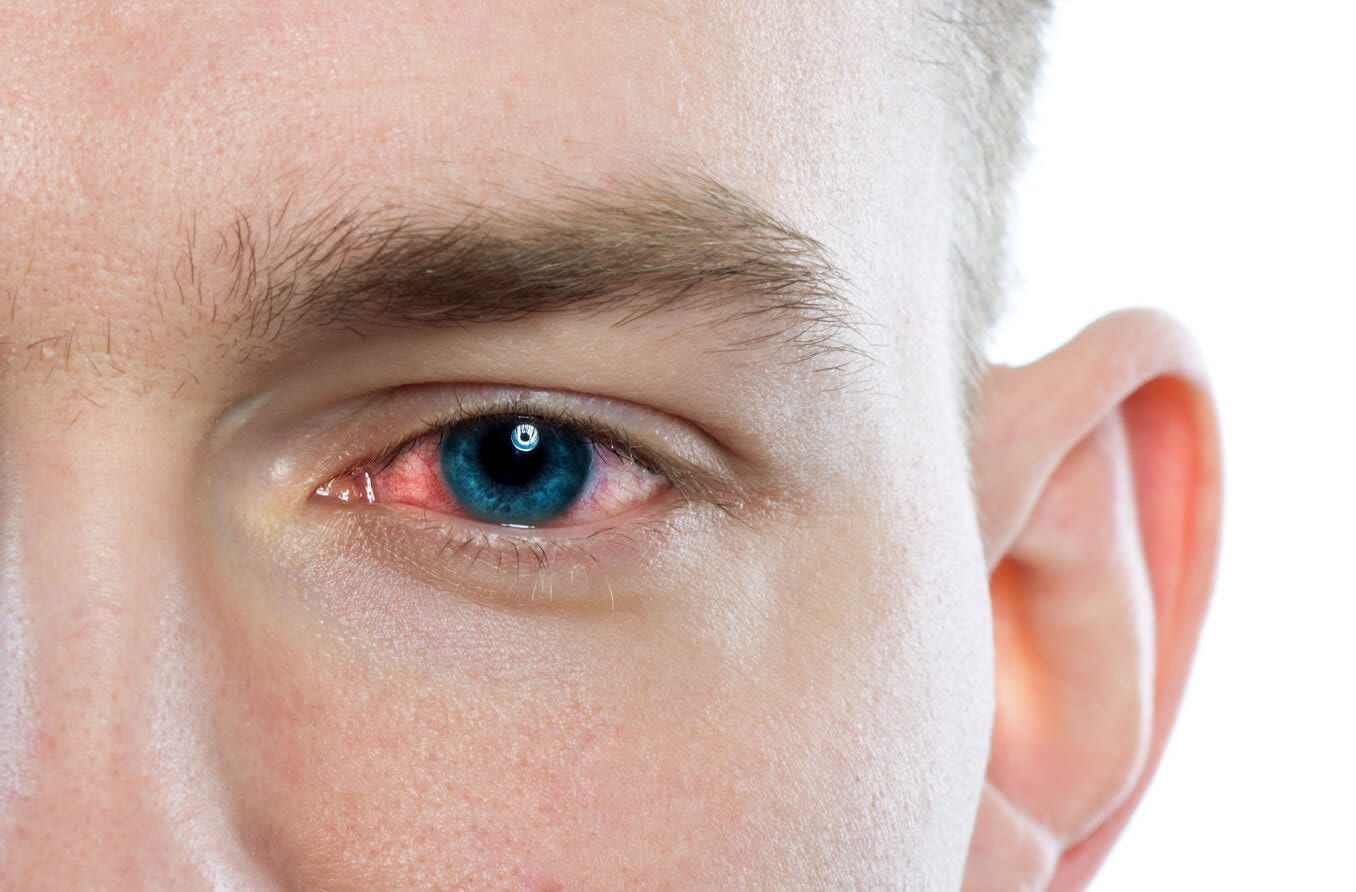
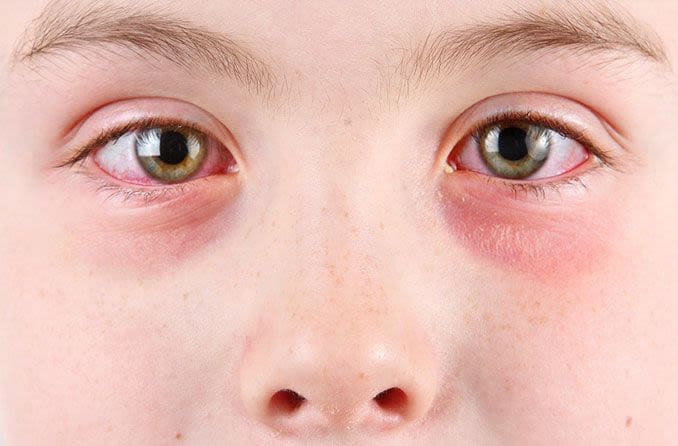
Keratoconjunctivitis refers to a group of conditions that cause dry eyes in some capacity. These conditions affect both the surface of the cornea and the conjunctiva. Underlying causes of keratoconjunctivitis can include bacteria, viruses, allergies, chemicals and even genetics.
Because of the wide range of causes, some people are more likely to have a certain type of keratoconjunctivitis. Each case can also vary in symptoms, severity and treatment.
Types of keratoconjunctivitis
The many types of keratoconjunctivitis include:
- Keratoconjunctivitis sicca (KCS), often referred to as dry eye syndrome
- Atopic keratoconjunctivitis (AKC)
- Vernal keratoconjunctivitis (VKC)
- Epidemic keratoconjunctivitis (EKC), also known as viral or adenoviral keratoconjunctivitis
Superior limbic keratoconjunctivitis (SLK)
- Phlyctenular keratoconjunctivitis
- Herpetic keratoconjunctivitis
- Neurotrophic keratoconjunctivitis (NK)
Each of these sub-conditions can range from mild to severe. Some people are more likely to get certain types of keratoconjunctivitis than others.
Causes and risk factors
Keratoconjunctivitis has a variety of causes among each form of the condition. Some common causes across types include:
- Seasonal allergies
- Environmental factors, such as dry climates, smoke, pollution, pollen or pet dander
Bacteria
- Viruses
- Toxins or chemicals
- Genetics
- Underlying conditions, including thyroid disease, diabetes, Sjogen’s syndrome, rheumatoid arthritis and lupus
Additionally, certain medications such as antidepressants, antihistamines, diuretics and oral contraceptives can have side effects that lead to dry eyes. Symptoms are more likely when medications are taken over a long period of time.
Other risk factors to be aware of that may be associated with keratoconjunctivitis are:
- Eye surgeries, including refractive surgery or a cornea transplant (keratoplasty)
- An imbalance in hormones, especially for those who are going through or have gone through menopause [see article on dry eye after menopause.]
- Skin conditions, such as eczema
READ MORE: Follicular Conjunctivitis
Symptoms of keratoconjunctivitis
Keratoconjunctivitis symptoms can vary based on type, and the severity may be different for each person. Some common across-the-board symptoms of the various forms of keratoconjunctivitis include:
- Dryness
- Itching
- Irritation
- Redness
- Sensitivity to light
- Blurry vision that may come and go
- Watery eyes or a watery eye discharge
- A foreign body sensation in your eye
- Swollen eyelids
Tell your eye doctor if you experience any of these symptoms so that your eyes can be properly evaluated. Not everyone will experience each of these issues, and some may be worse than others.
A breakdown of the keratoconjunctivitis types
Each type of keratoconjunctivitis comes with its own set of causes and complications. This includes the following:
Keratoconjunctivitis sicca (KCS)
Also known as dry eye syndrome, KCS is one of the more common forms of keratoconjunctivitis. It occurs when both the cornea and conjunctiva of the eye experience dryness or inflammation.
KCS can be caused by underlying medical conditions. Insufficient tear production, side effects of certain medications and other factors can also cause KCS. Women and older adults are more likely to get KCS than other demographics.
Atopic keratoconjunctivitis (AKC)
Atopic keratoconjunctivitis (AKC) is a type of allergic keratoconjunctivitis. AKC is caused by a genetic disorder called atopy. Atopy causes the immune system to produce extra antibodies to fight off an allergy.
People with atopy have more serious allergic reactions when they come in contact with allergens. Allergens include food or environmental factors.
When the eyes are affected by this response, it can trigger AKC and cause the conjunctiva that lines the eyelids to become red and swollen. In many cases, the lower lid is impacted more so than the upper lid. Symptoms may also seem worse in the winter.
AKC can lead to more serious eye problems if it is not treated, such as scarring, ulceration, cataracts or keratoconus (abnormal thinning of the cornea that causes it to bulge forward). More men are affected by AKC than women.
Vernal keratoconjunctivitis (VKC)
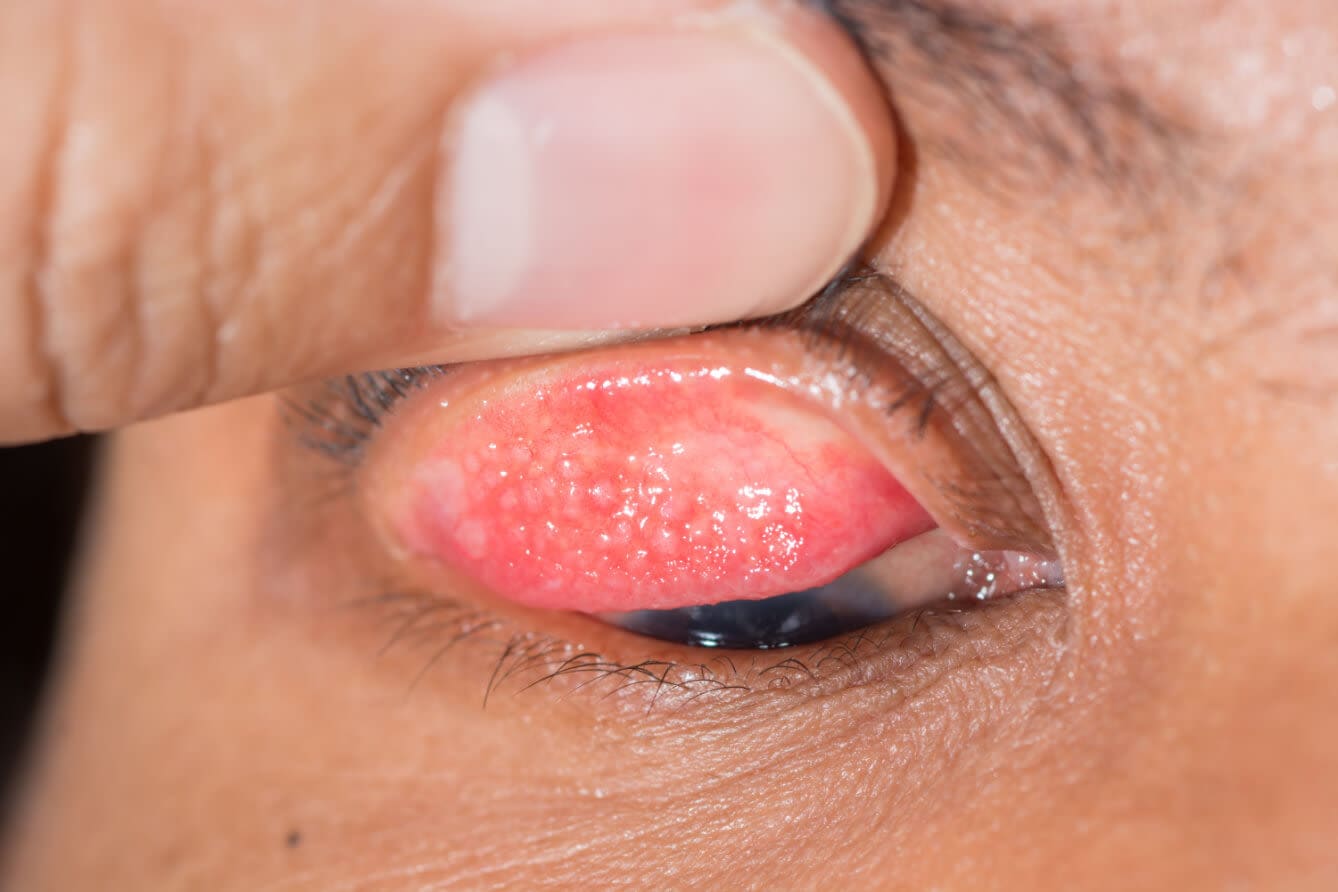
Vernal keratoconjunctivitis (VKC) is another type of allergic keratoconjunctivitis. VKC is associated with chronic and severe allergies. The condition causes notable features such as hard, cobblestone-like bumps located on the upper eyelid. These bumps may be accompanied by swelling or mucous discharge.
VKC affects the eyes on a seasonal basis — most commonly during the late spring and summer months when it is dry and warm. It may also reoccur during the winter.
Unlike atopic keratoconjunctivitis, vernal keratoconjunctivitis affects the upper eyelid more than the lower.
A portion of the treatment for VKC often involves managing allergies to prevent flare-ups. VKC is rare (affecting 0.1 to 0.5% of eye conditions). It mainly affects males between the ages of 3 and 20. In many cases, symptoms subside after puberty.
Epidemic keratoconjunctivitis (viral/adenoviral keratoconjunctivitis)
Epidemic keratoconjunctivitis (EKC) is also known as viral keratoconjunctivitis or adenoviral keratoconjunctivitis. It is a very contagious viral infection caused by a group of viruses called “adenoviruses.” These also cause infections such as the common cold.
You can get EKC by coming into contact with another person who currently has the virus and then touching your eyes. Touching objects or surfaces that are contaminated with the virus and then touching your eyes can also cause you to become infected.
Because EKC is so easily spread, washing your hands frequently is highly recommended during an outbreak.
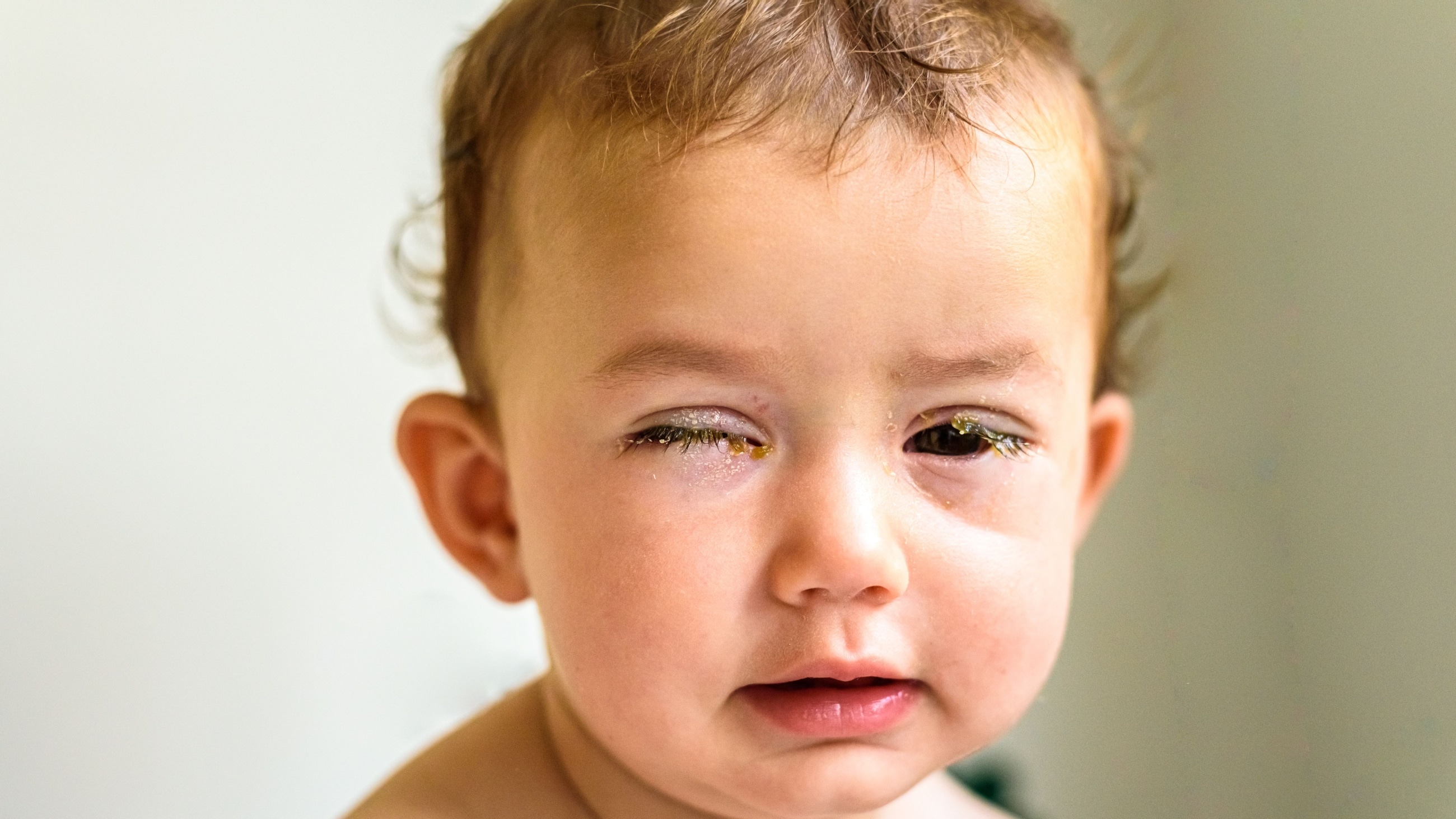
EKC can cause the same symptoms associated with other types of keratoconjunctivitis. These include eyelid swelling, discharge and redness. On some occasions, it can also cause a fever, fatigue, headache or swollen lymph nodes.
Symptoms may be relieved with the use of artificial tears or cold compresses, but there are currently no effective treatments for EKC. The virus usually resolves on its own within two weeks.
Superior limbic keratoconjunctivitis (SLK)
Superior limbic keratoconjunctivitis (SLK) is chronic and recurrent. SLK affects the following parts of the eye:
Superior bulbar conjunctiva — the clear layer over the eyeball and the sclera (the white of the eye)
Tarsal conjunctiva — the clear layer lining the eyelids
The area above the cornea
There is no known cause of SLK, though it is sometimes associated with rheumatoid arthritis and thyroid disease. SLK most often affects women between the ages 20 and 70. It is also known to slowly develop over a time period of 1 to 10 years.
Phlyctenular keratoconjunctivitis
Phlyctenular keratoconjunctivitis is an inflammation of the cornea and conjunctiva. This type of keratoconjunctivitis is caused by an antigen. A common antigen is staphylococcus aureus bacteria (which causes staph infections). Another is mycobacterium tuberculosis (which causes tuberculosis).
Other types of bacteria can cause it, but these are the most common.
Key indicators of phlyctenular keratoconjunctivitis are conjunctival or corneal lesions or nodules. These can measure between 1 and 2 millimeters.
This type of keratoconjunctivitis commonly occurs in children ages 6 months to 16 years. It is also found more often in girls than boys and tends to occur more frequently in the springtime.
Herpetic keratoconjunctivitis
The herpes simplex virus (HSV) can affect the eyes and cause a viral infection such as herpetic keratoconjunctivitis. This condition can cause swelling, eye sores or discharge, among other symptoms.
Infections associated with ocular herpes are mainly caused by type I of HSV. This is the same type that causes cold sores. It’s possible to contract the condition after touching a cold sore near your mouth and then touching your eye. Type II of HSV, which is sexually transmitted, can affect the eye as well, but this is rare.
Herpetic keratoconjunctivitis may be treated with an antiviral medication in the form of eye drops, ointment or pills. It’s important to get treated for herpetic keratoconjunctivitis promptly to avoid worsening eye problems in the future.
Neurotrophic keratoconjunctivitis (NK)
Neurotrophic keratoconjunctivitis (NK) is a rare disease of the cornea that causes a reduction or loss of feeling in the cornea. This occurs when the trigeminal nerve becomes impaired or damaged. The trigeminal nerve is responsible for sensory feedback.
Since it causes the cornea to become less sensitive and lose feeling, pain is not usually reported in patients. Some may experience blurred vision though. NK is a degenerative eye disease, meaning it gets worse over time. For this reason, early detection is important in the treatment process.
Diagnosing keratoconjunctivitis
Your eye doctor will ask you about any underlying conditions that could contribute to your symptoms of dry eyes. Conditions include autoimmune diseases or changes in hormones (if you are taking birth control, hormone treatments or have gone through menopause). A family history of dry eye problems is also important to disclose.
Let your doctor know if you wear contacts or use any ophthalmic solutions, ointments, cosmetics or other products that may cause irritation.
After discussing your symptoms and medical history with your doctor, some testing may be done to further investigate what might have caused your condition. This can include procedures such as:
A general physical eye examination
An exam using an instrument called a slit lamp to examine the tear film quality on the surface of the eyes
The Schirmer’s test, which involves placing special filter paper inside each of the lower eyelids to measure the amount of tears the eyes are able to produce in five minutes
Treatment for keratoconjunctivitis
The course of treatment depends on the type of keratoconjunctivitis that is present. Some may require prescribed medication. Others may find relief from an over-the-counter fix or through lifestyle changes.
Artificial tears and other topical solutions or ointments can be used to lubricate the eyes.
A cool compress may be used to soothe discomfort associated with the condition.
Avoiding allergens and irritants as much as possible can help prevent dry eyes.
Adjusting or changing any medications that could cause dry eyes may help improve symptoms.
Special medications may be prescribed to treat the specific condition in the eyes. They may also treat the underlying disease in the body that contributed to the eye problem. This can include topical antihistamines or corticosteroids.
Surgery may be recommended for severe forms or cases of keratoconjunctivitis.
Some forms of keratoconjunctivitis, such as those that are viral, may resolve on their own.
Sometimes, a combination of these treatments is needed in order to achieve a full recovery. If symptoms do not go away with treatment, or if they worsen, let your doctor know so that your condition can be reevaluated.
Be sure to schedule regular eye exams on a yearly basis to ensure that your eye health and general vision are in good shape. Routine comprehensive eye exams are the best way to assess and prevent further eye problems for children as well as adults.
SEE RELATED: Eye exams: 5 reasons they are important
Dogs can get keratoconjunctivitis, too
It’s true — like humans, dogs can also develop keratoconjunctivitis sicca (KCS). The condition in canines is more often seen in breeds such as pugs, Cocker Spaniels, Boston Terriers and English Bulldogs.
The symptoms of KCS present similarly in dogs and people. Diagnosing and treating the condition can also be similar for both animal species.
Whether it’s you or your furry friend who is experiencing dry eyes, it’s important to get medical help as soon as possible. This will help ensure you are on the right road to recovery.
READ MORE: Symblepharon