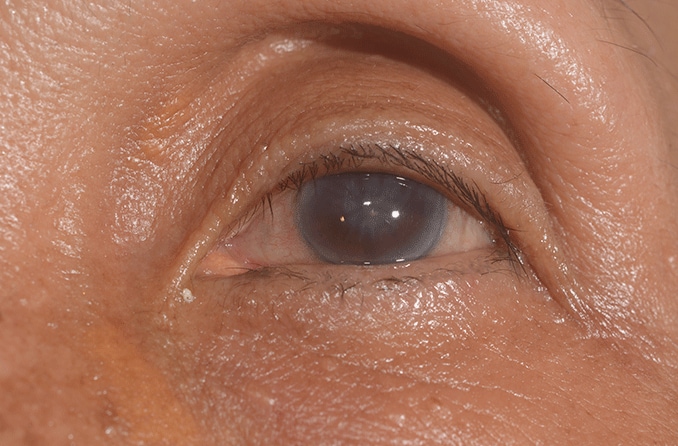
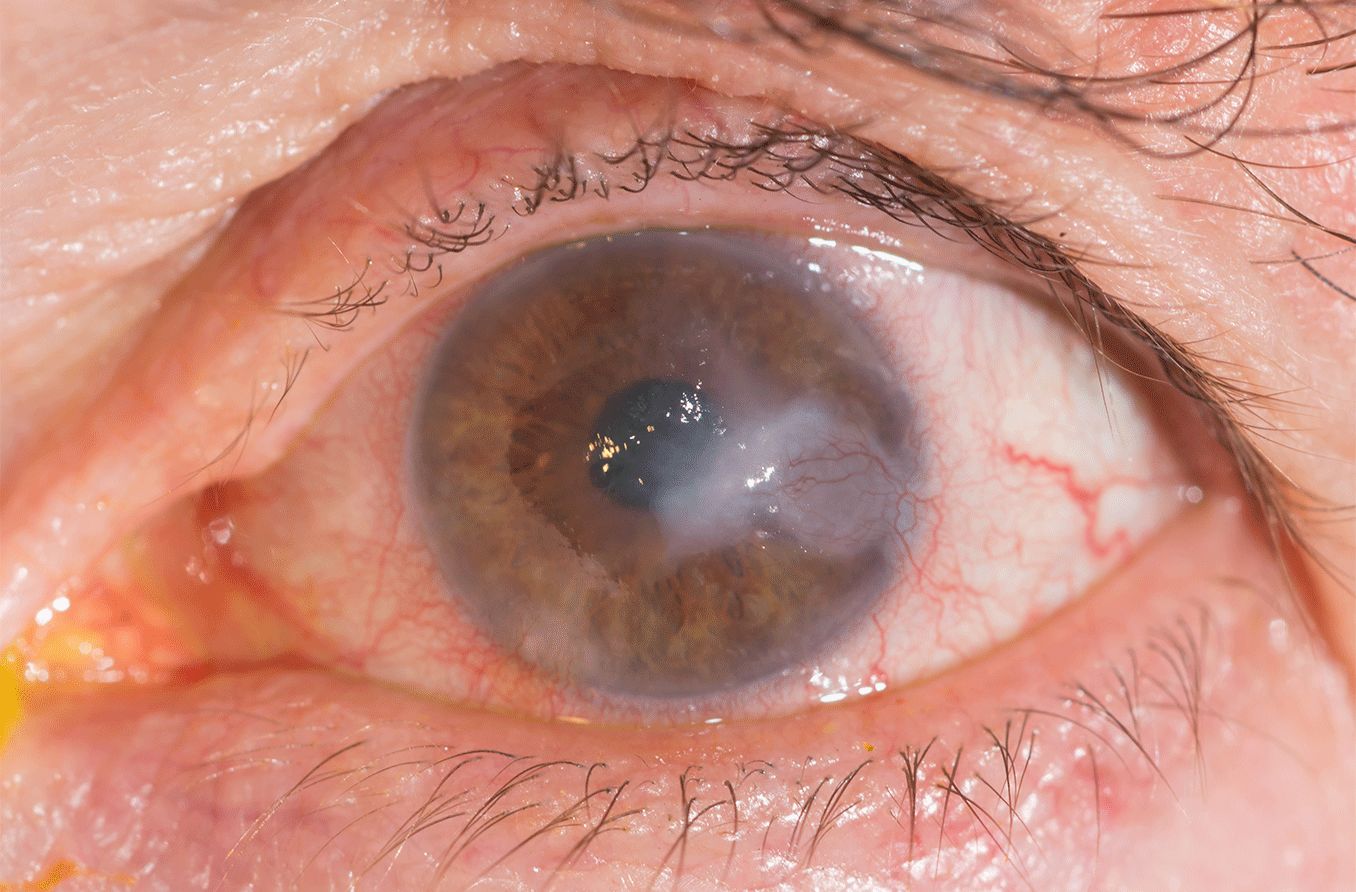
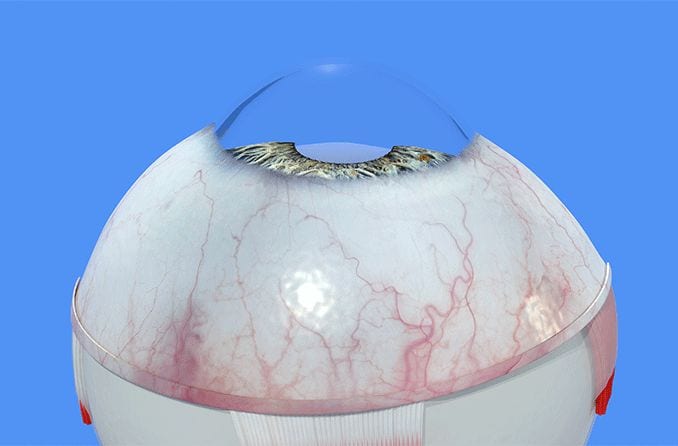
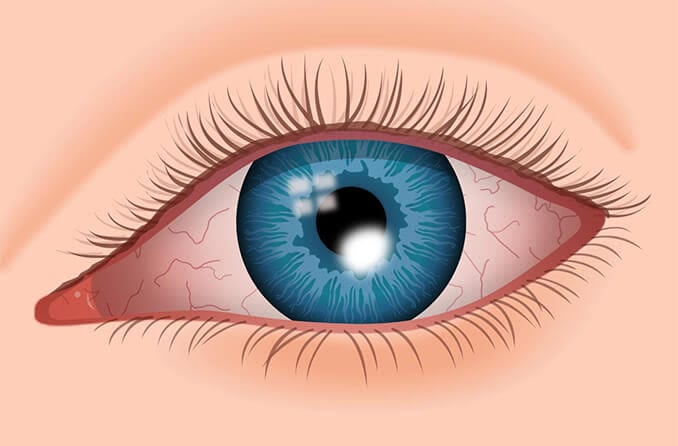
Corneal edema is the swelling of the cornea, or the clear front surface of the eye that lets light in to enable vision. This corneal swelling can occur due to infection, inflammation, injury or following eye surgery. Certain eye diseases may also trigger corneal edema.
If left untreated, corneal edema can affect vision, particularly causing cloudiness, discomfort or light sensitivity. It is recommended to see an eye doctor as soon as possible if you believe you are experiencing corneal edema or any other condition that obstructs your vision.
Corneal edema causes
Corneal edema is essentially caused by fluid buildup in the cornea. This can be the result of a number of factors, including:
- Trauma or injury
- Eye infection
- Eye inflammation
- Glaucoma, which can cause high internal eye pressure and damage to the optic nerve
- Complications after cataract surgery, referred to as pseudophakic corneal edema (PCE)or pseudophakic bullous keratopathy (PBK)
- Severe cases of posterior polymorphous corneal dystrophy (PPCD or Schlichting dystrophy), a rare corneal condition
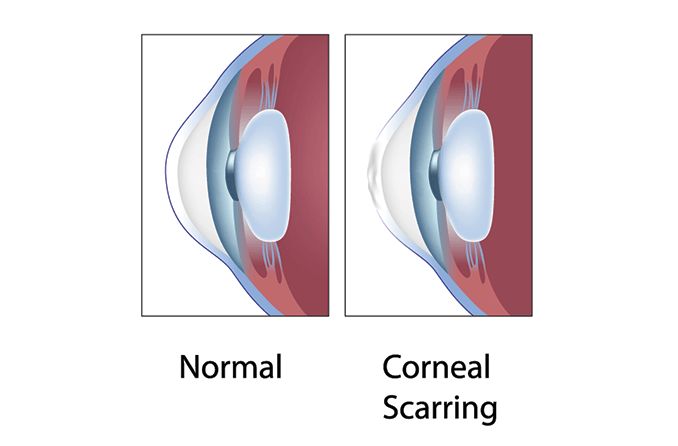
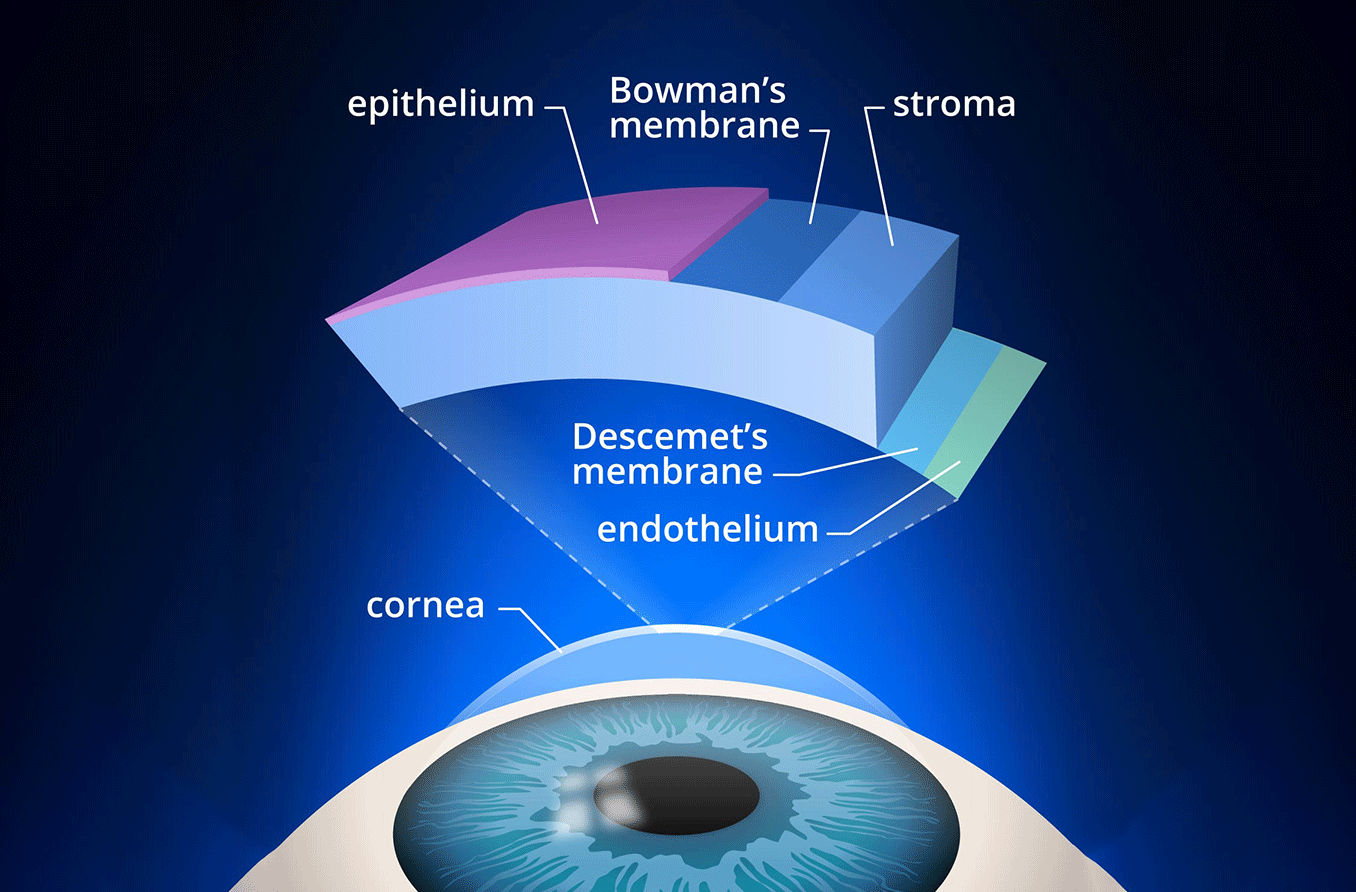
What causes this fluid buildup in the first place? There are several layers of tissue that make up the cornea and help it function properly. The innermost layer is a single layer of cells called the endothelium. These cells prevent the cornea from swelling by removing excess fluid. This is important for keeping the cornea transparent.
If the endothelium becomes damaged, fluid begins to build up in the cornea. This excess fluid, or edema, results in the cornea becoming cloudy, decreasing vision in the process. That said, there are certain conditions that can damage the endothelial cells and lead to corneal edema, including:
- Fuchs’ dystrophy – an inherited eye disease caused by deteriorating endothelial cells
- Chandler’s syndrome (CS)– a rare eye condition that causes the endothelial cells to multiply too quickly
- Endotheliitis (inflammation of the endothelium)– can be triggered by viruses such as herpes simplex virus (HSV), mumps or cytomegalovirus (CMV), as well as bacterial origins
Certain substances and drugs can also cause corneal edema. This includes:
- Amantedine, a medication used to treat patients with Parkinson’s disease
- Benzalkonium chloride, a preservative found in topical eye drops and anesthetics
- Chlorhexidine, a topical antiseptic used to clean the skin in preparation for surgery or an injection
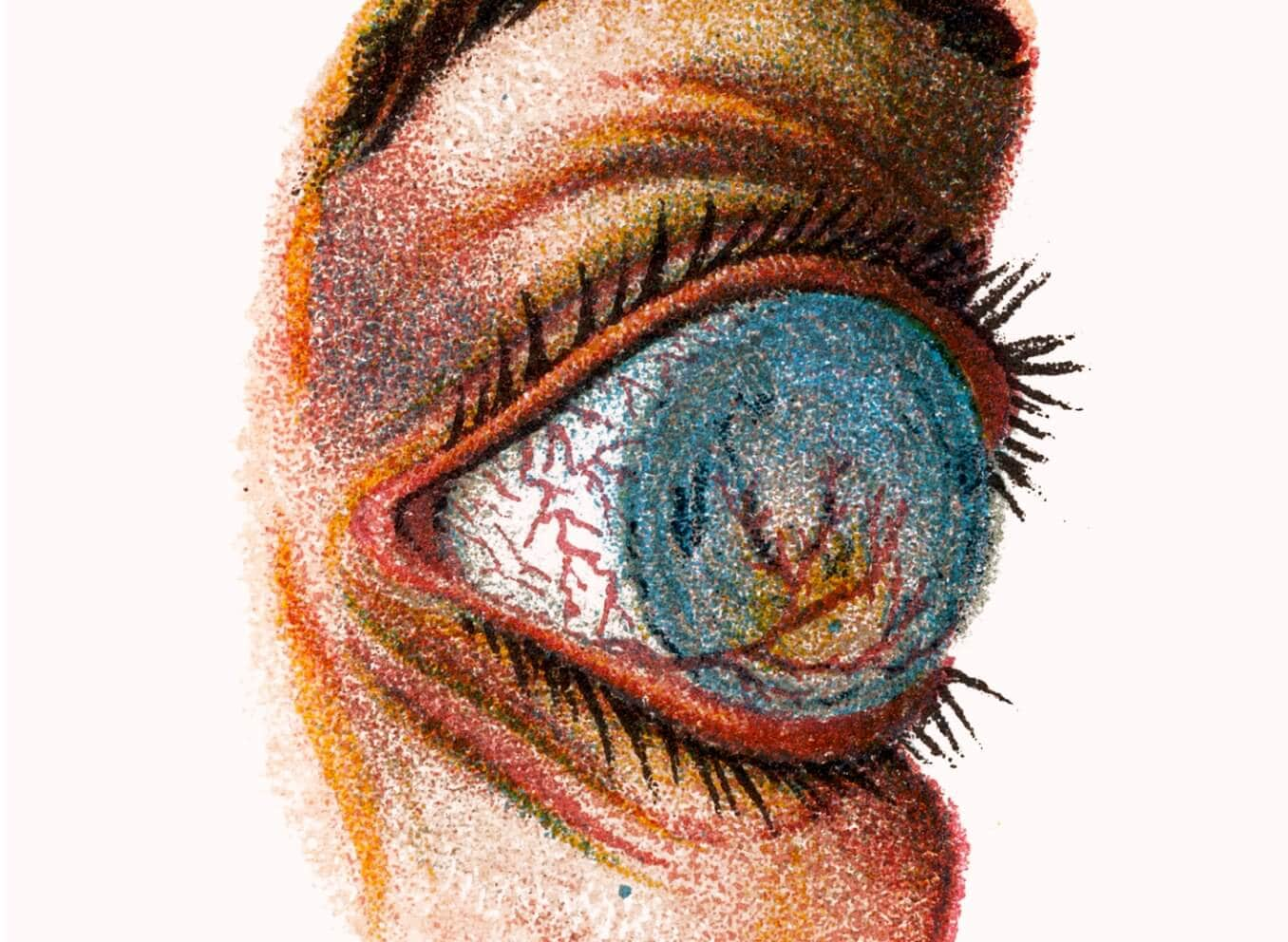
Corneal edema symptoms
Symptoms commonly associated with corneal edema include:
- Blurred or cloudy vision
- Eye pain
- A sensation of something being stuck in your eye
- Halos surrounding sources of light
- Light sensitivity
These symptoms are often worse in the morning after you wake up but usually lessen during the day as your eyes remain open, and the fluid buildup in the cornea is able to evaporate more effectively.
Corneal edema treatment
While options can involve eye drops, hair dryers and surgery, the ideal treatment for corneal edema depends on the underlying cause of the condition.
It is important to address the underlying cause of edema, in addition to treating the symptoms. This is true whether the underlying condition is acute (such as an injury, infection or product of surgery)or chronic (such as glaucoma, Fuchs’ dystrophy or another disease).
Mild cases of corneal edema may not require treatment, though your eye doctor may prescribe eye drops to help reduce swelling. Some doctors might also recommend using a hair dryer to blow air on your eyes, as it may help increase tear evaporation and reduce swelling. (Never use the hair dryer method before talking to your eye doctor, and follow your doctor’s instructions closely to avoid any potential dangers to your eyes.)
Surgery for corneal edema
If your condition is severe enough to interfere with your vision, your eye doctor may recommend a surgical procedure to replace the cornea via a corneal transplant (keratoplasty). Another option is to replace the endothelial layer via DSEK surgery (Descemet’s stripping endothelial keratoplasty).
During a corneal transplant procedure, an eye surgeon removes the central corneal tissue and replaces it with healthy tissue from a donor. The new tissue is called a “graft.” You will be given steroid eye drops for several months following the procedure to help your body get used to the graft and to treat any swelling or discomfort and to control infection.
In DSEK surgery, the surgeon only removes and replaces the flawed endothelial layer of the cornea. The procedure and the recovery time are shorter with DSEK than with a full corneal transplant. You will also be given steroid eye drops as part of your treatment following a DSEK surgery.
Beyond treatment
It’s important to care for your eye health, whether or not you experience a condition that may lead to corneal edema. Though it is not life-threatening, it’s critical to contact an eye doctor as soon as you notice any signs of corneal edema.
In addition, be sure to have a comprehensive eye exam annually to ensure your vision is clear, and your eyes are healthy and well-functioning. Regular eye exams are the most effective way to pinpoint any problems that could impact your vision in the short-term and long-term.
READ NEXT: Eye exams: 5 reasons they are important