What is choroidal neovascularization?
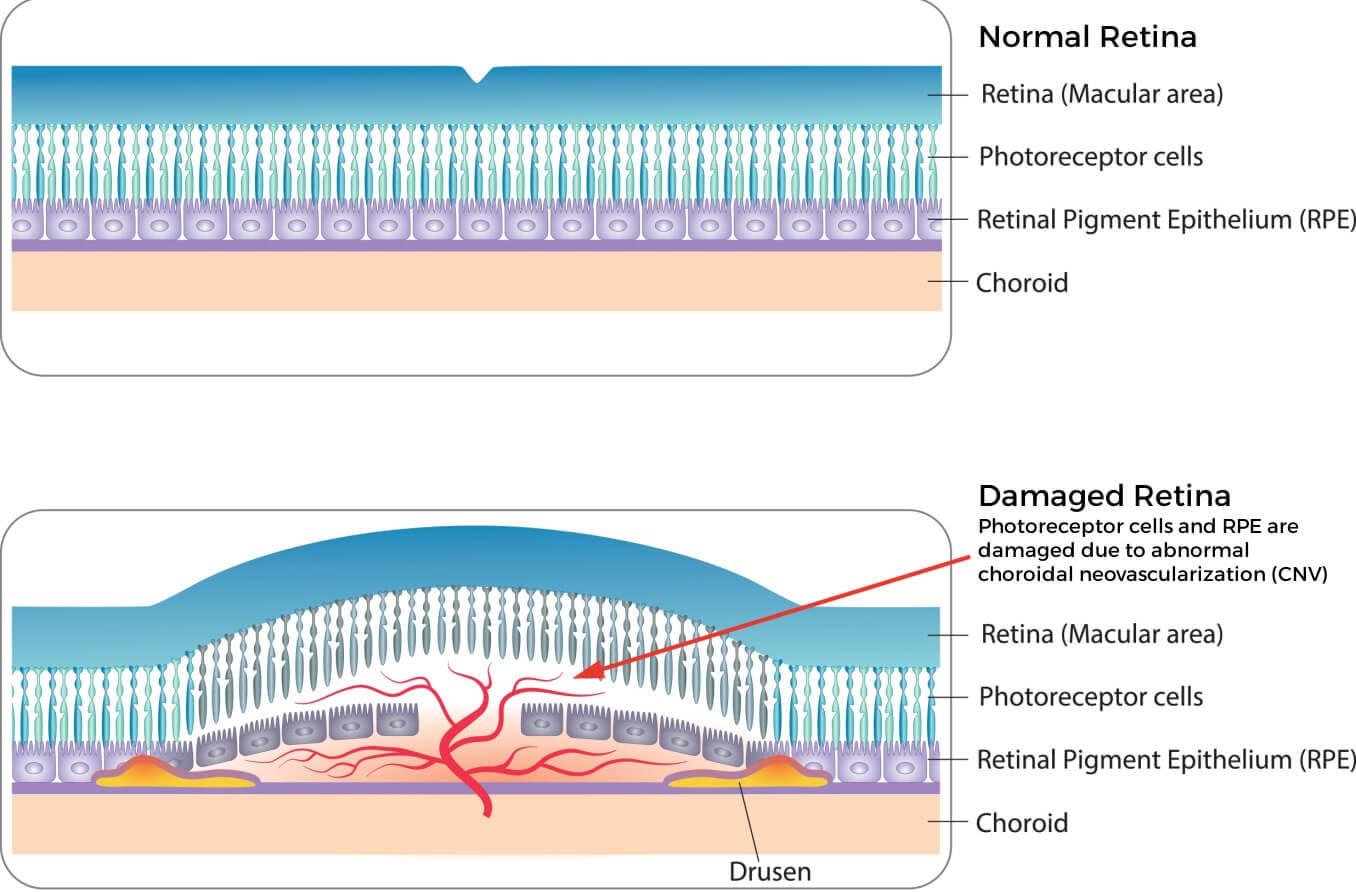
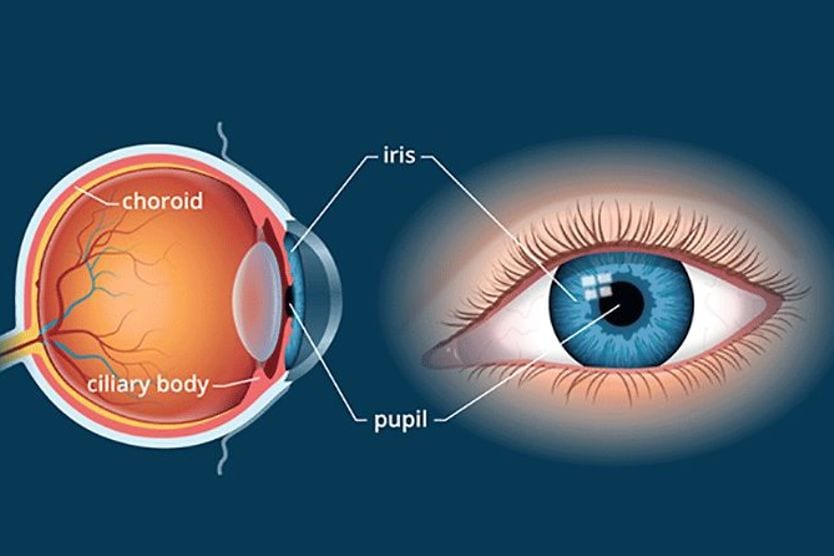
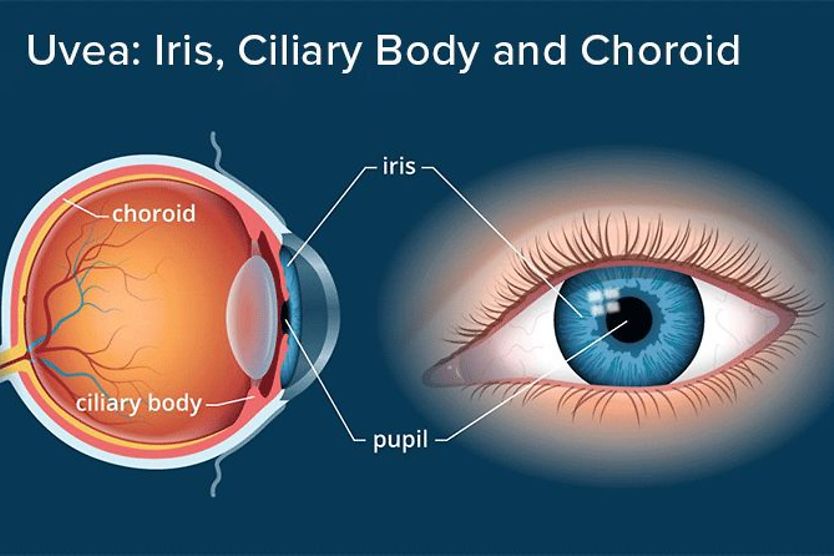
Choroidal neovascularization (CNV) is the growth of abnormal blood vessels in the choroid. The choroid is the blood vessel-filled middle layer of the eye, which lies between the sclera and retina. These abnormal blood vessels can leak fluid and blood, damaging the retina and causing vision loss.
What causes choroidal neovascularization?
The exact mechanism of the development of CNV is not fully understood. It is believed that a protein called vascular endothelial growth factor (VEGF) is released in excess by a thin layer of cells called the retinal pigmented epithelium (RPE).
The RPE is located in the outermost layer of the retina. The retina is the inner light-sensitive tissue in the back of the eye that converts light into signals that are sent to the brain for processing.
VEGF is normally found in the eye and helps to maintain the retina. However, low levels of oxygen, inflammation or other stressors can cause excess production of VEGF by the RPE.
The excess VEGF stimulates the growth of new, abnormal and fragile blood vessels in the choroid. The choroid is a thin layer of blood vessels that helps to maintain the outer layers of the retina, providing oxygen and nutrients and carrying away waste.
In addition to producing VEGF, the RPE — along with a membrane called Bruch’s membrane — forms a barrier between the choroid and retina. When too much VEGF is produced, abnormal blood vessels form and break through this barrier, leaking fluid and blood into the spaces between the choroid and retina.
This results in injury to the retina, particularly the photoreceptor cells known as rods and cones. These specialized photoreceptor cells are critical to vision because they transform light into electrical signals that the brain processes as images. Damage to the rods and cones can lead to vision loss.
READ MORE: Choroid of the eye: Anatomy and function
Symptoms of choroidal neovascularization
An individual may not at first notice that their vision has been affected because symptoms of CNV are typically painless and can occur in one eye only. These symptoms may include:
- Central vision that is blurry and dim
- A blind spot or dark spot in the center, or near the center, of vision
- Distortion of images
- The appearance of straight lines as irregular or wavy
- Change in color perception
- Lights flickering in the center of vision
The first symptoms of choroidal neovascularization are often blurred vision and distorted images. An individual may also notice that faces seem to appear blurry. As choroidal neovascularization progresses, a blind spot may appear in the center of vision. Side vision is usually not affected.
An Amsler grid consists of straight lines, with a reference dot in the center. Click to open.
If you have a condition that puts you at risk for developing choroidal neovascularization, your eye doctor may give you an Amsler grid to help monitor your vision at home. This is a grid that checks for wavy, dark or blurred areas of vision and helps to monitor for any changes.
If you notice a sudden change in your vision, it is important to contact your eye doctor right away.
Conditions that may cause choroidal neovascularization
With increasing age, the risk of developing CNV increases. The reason for this is that wet age-related macular degeneration (ARMD) is the most common cause of choroidal neovascularization. However, CNV can also occur in other conditions due to trauma, inflammation or other factors.
Wet AMD
There are two types of age-related macular degeneration (AMD) — dry and wet. Dry AMD is a slow-progressing condition in which areas of the macula get thinner with age. Clumps of a protein called drusen accumulate around the macula. About 80% of people with macular degeneration have a dry form of AMD.

Healthy eye as compared to an eye with dry macular degeneration and wet macular degeneration.
Wet AMD is also known as exudative or neovascular AMD. This type is called “wet” because of the blood and fluid that leak from choroidal neovascularization. About 1 in 10 people with dry AMD go on to have CNV, developing into wet AMD. Vision loss usually occurs more rapidly with the exudative form of AMD.
Reducing the risk of developing wet AMD and choroidal neovascularization will reduce the risk of vision loss. There are lifestyle habits that can decrease this risk, including:
- Not smoking
- Eating a healthy diet, including fruits and vegetables
- Maintaining a healthy weight
- Regular exercise
- Wearing UV-filtering sunglasses when outdoors
Other conditions that can cause CNV
Conditions that break down Bruch’s membrane are associated with choroidal neovascularization. These can include:
- Injury to the choroid due to trauma
- Injury to the choroid after laser surgery
- Angioid streaks
Conditions that disrupt the retina and choroid can result in choroidal neovascularization as well, such as:
- Myopic macular degeneration
- Presumed ocular histoplasmosis syndrome
- Inflammatory conditions, such as sarcoidosis
- Tumors in the choroid
People with high myopia who go on to develop pathologic (degenerative) myopia are at risk for myopic macular degeneration. Myopia-control strategies that slow down the progression of myopia can decrease this risk.
Diagnosis of choroidal neovascularization
Choroidal neovascularization must be diagnosed by an eye doctor. A comprehensive, dilated eye exam and imaging procedures such as fluorescein angiography and optical coherence tomography help the doctor make this diagnosis.
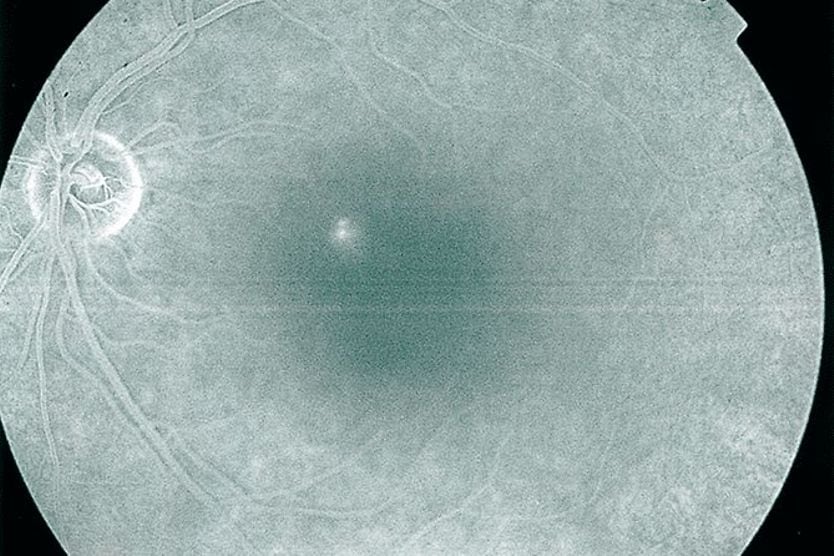
Fluorescein angiography (FA)
For this test, fluorescein dye is injected into the arm and travels to the blood vessels of the eyes. As the dye moves through the eye’s blood vessels, images are taken. The dye lights up areas with choroidal neovascularization. This allows the eye doctor to identify where leaking blood vessels in the retina are located.
A network of abnormal, leaky blood vessels in the choroid is referred to as a choroidal neovascular membrane (CNVM). It can generally be classified as occult (type 1) or classic (type 2). The difference between the types of CNVM is based on factors such as location and how it presents during fluorescein angiography.
Optical coherence tomography (OCT)
This is a procedure that provides high-quality 3D images of cross-sections of the retina. It is painless and does not require an injection. The presence of choroidal neovascular membranes is confirmed by analyzing the cross-sectional images provided by OCT.
Treatment of choroidal neovascularization
Depending on the underlying condition, treatment will vary. One or a combination of treatments may be recommended.
Anti-VEGF treatment
Since vascular endothelial growth factor drives the development of CNV, eye doctors inject anti-VEGF drugs directly into the eye to block the excessive production of VEGF. Multiple injections are often required.
The aim of anti-VEGF treatment is to:
- Reduce the growth of choroidal neovascular membranes.
- Decrease leakage of fluid and blood.
- Slow loss of vision.
- Potentially improve vision that has worsened.
Photodynamic therapy (PDT)
PDT uses a laser and an injected drug that work in combination to decrease fluid leakage. The drug is injected into the arm and travels to the leaky blood vessels of the choroidal neovascular membrane. The drug is then activated by a low-power laser that is directed at the leaky blood vessels. This procedure damages these blood vessels, reducing the amount of fluid and blood they leak.
Laser photocoagulation
While PDT uses a low-energy laser, laser photocoagulation uses a high-energy laser. It creates a burn in the area it is targeting and seals off the abnormal blood vessels, decreasing fluid and blood leakage.
When to see a doctor
If you notice a sudden onset of visual symptoms such as blurry, distorted or missing areas in your vision, it is important to immediately contact an eye doctor for evaluation.
Patients with AMD, high myopia, or other conditions that are associated with CNV should be routinely followed by an eye doctor with comprehensive eye exams. Depending on the type and severity of choroidal neovascularization, there are a number of different treatments that can slow down its progression and preserve vision.
READ NEXT: Pathologic myopia: What does it mean if myopia is degenerative?