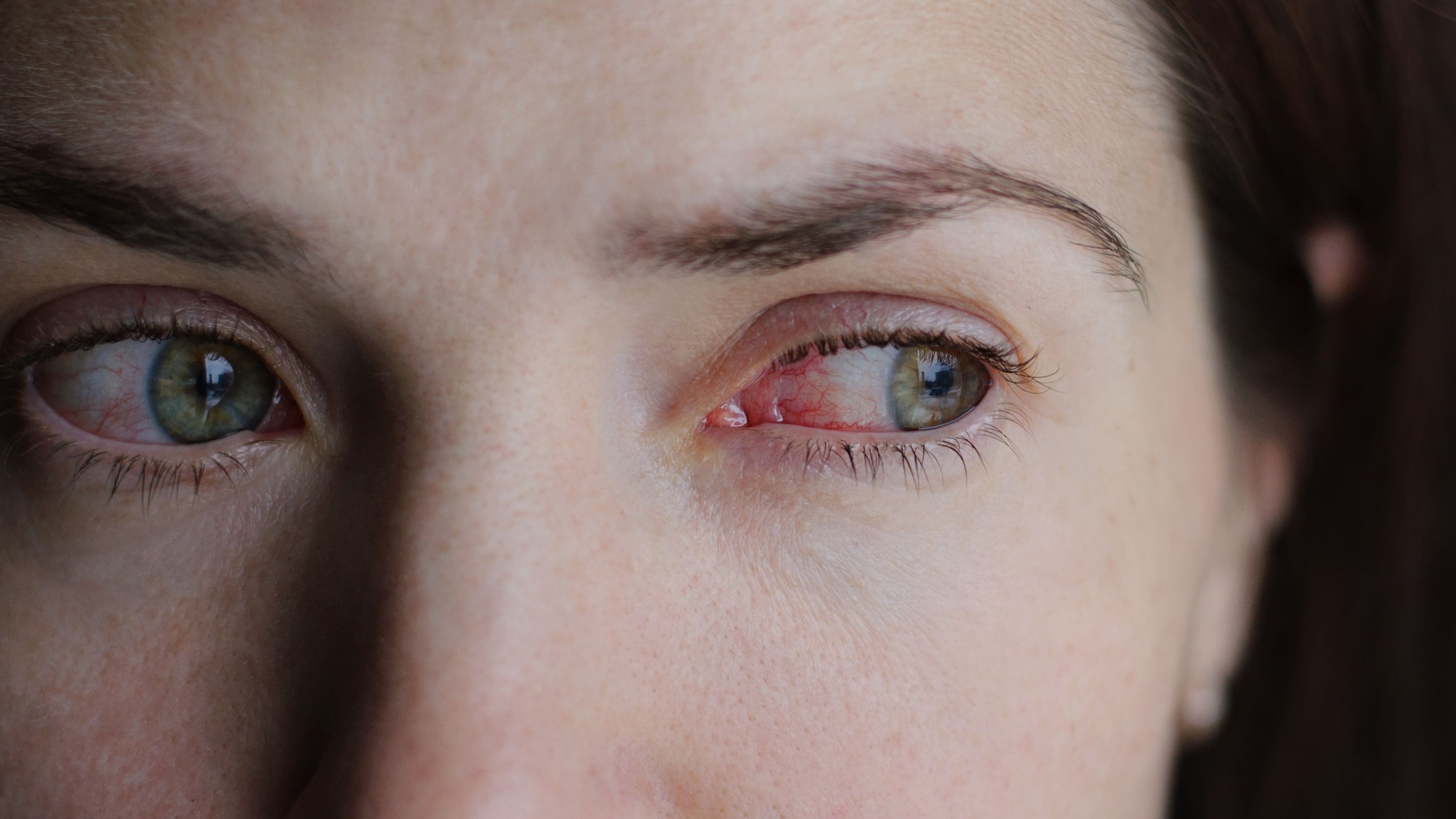
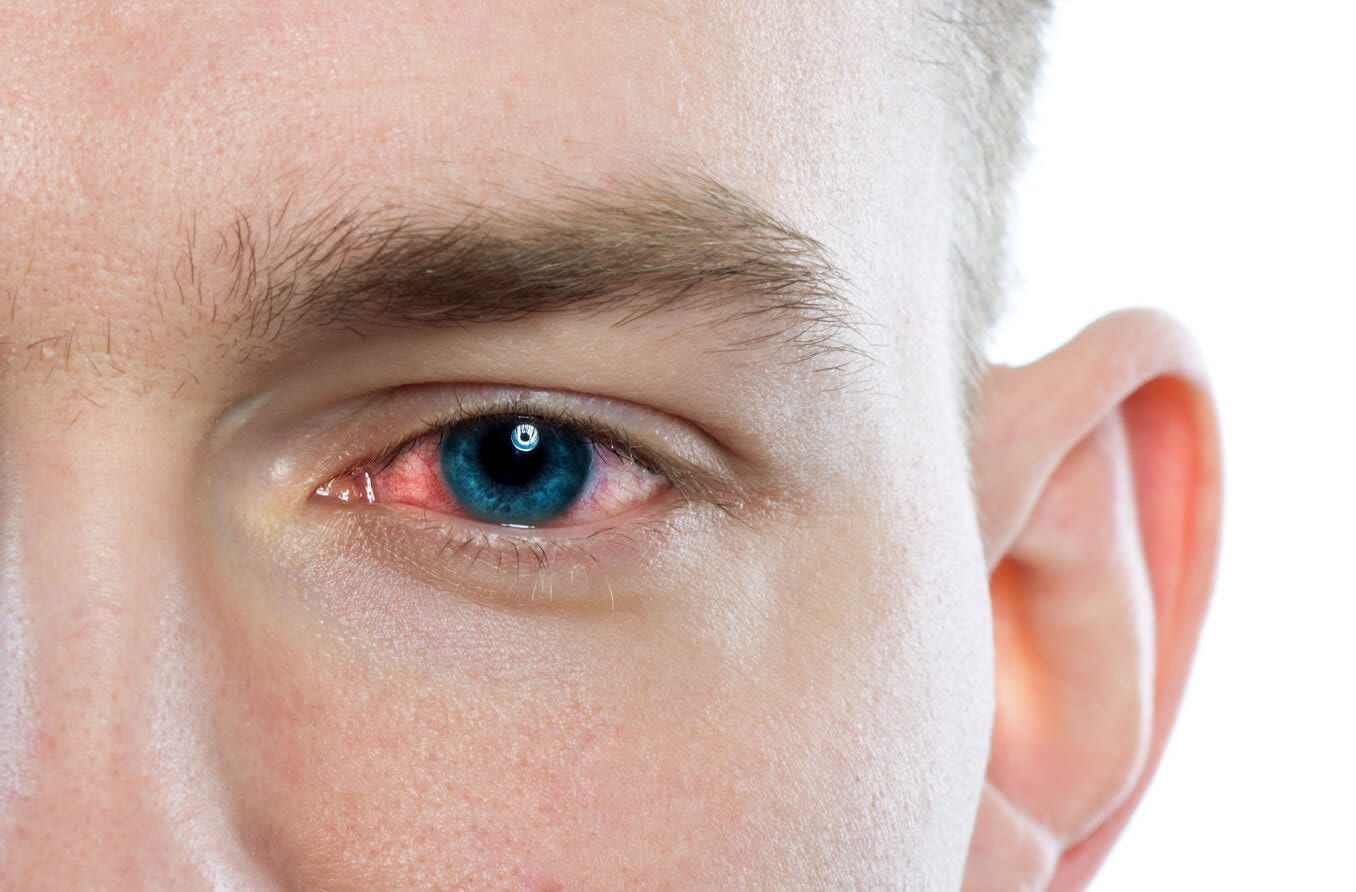
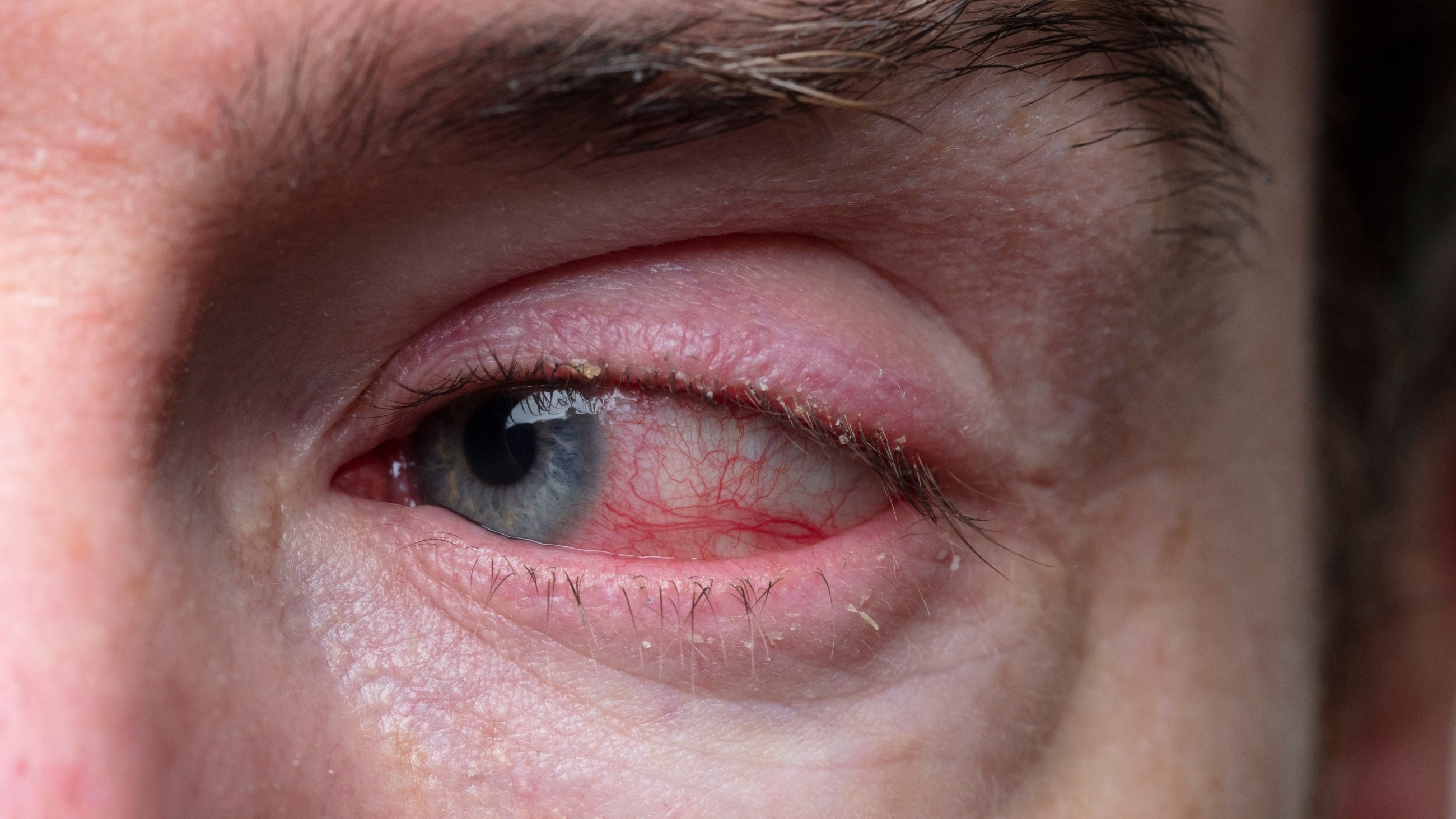
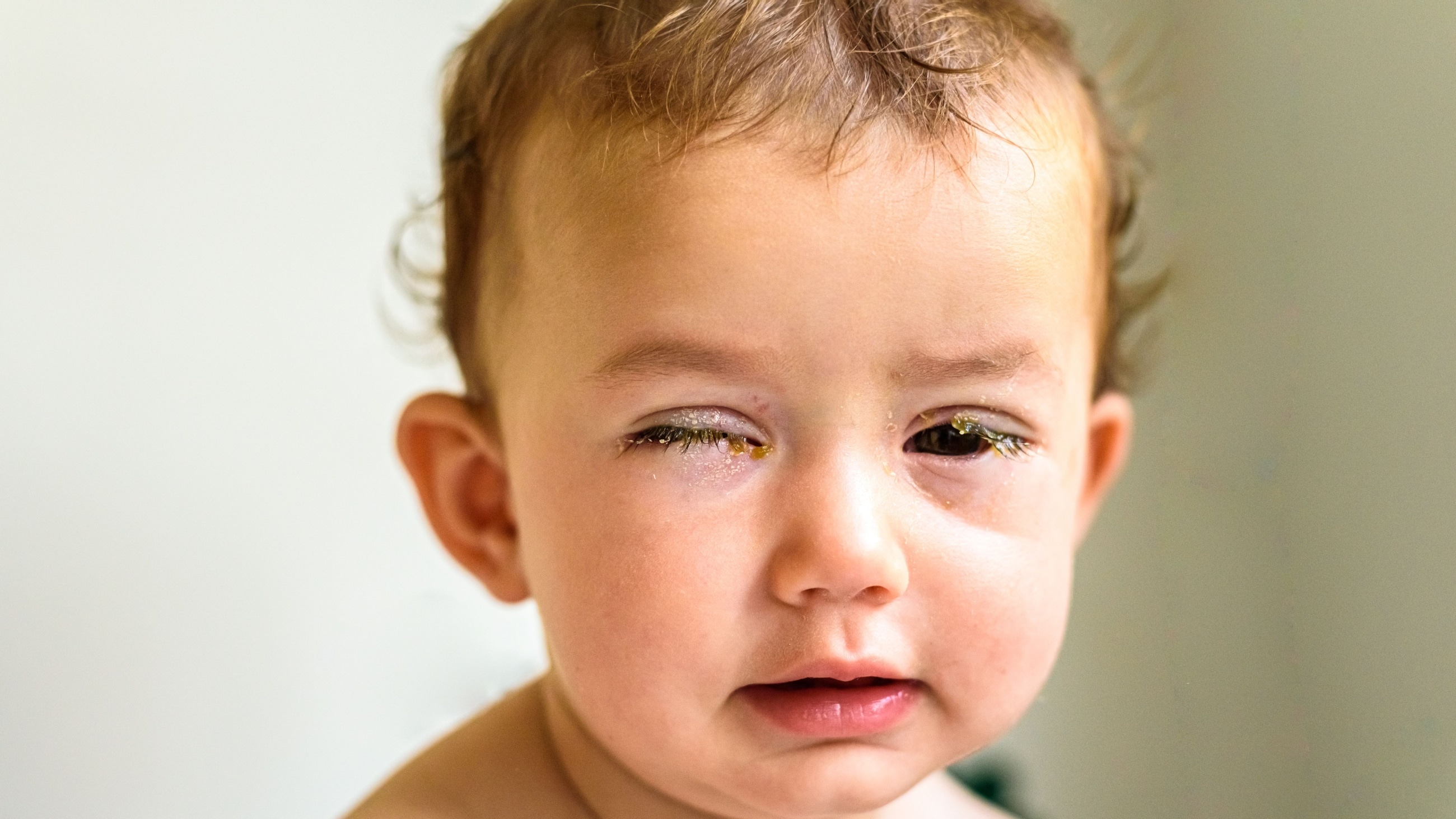
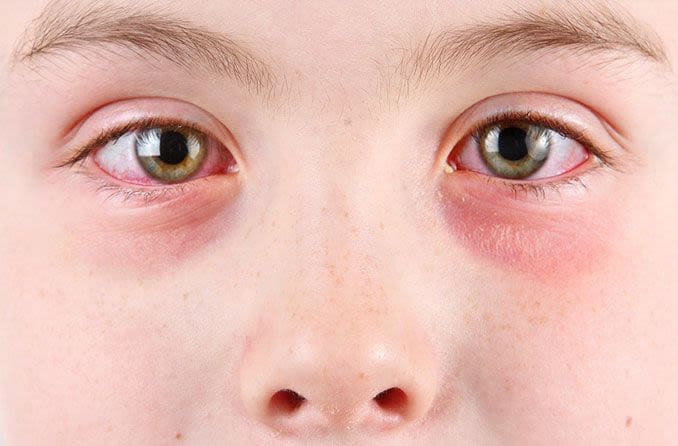
Causes of pink eye
Pink eye (conjunctivitis) does not have a single, universal cause. It can be caused by viruses, bacteria, allergens and several kinds of eye irritants. The name pink eye is generally used when it’s caused by a virus, which is the most common type of conjunctivitis. Other primary causes include:

Bacterial infections
Contact lens irritation
Foreign objects (dirt, eyelash, pet fur, etc.) in the eye
Chemical fumes, smoke, etc.
Viral pink eye
Viruses cause an estimated 80% of pink eye cases. Of that number, around 90% are caused by adenoviruses — the same viruses responsible for the common cold. Because of this, the viral form is sometimes referred to as an “eye cold.” It can occur alongside a cold, flu or other upper respiratory infection.
Less commonly, it may be caused by more serious viruses. These include the coronavirus responsible for COVID-19, herpes simplex, varicella-zoster and Epstein-Barr.
Viral pink eye is very contagious. Anyone who has it can spread it to others, just like the common cold. It transfers easily through coughs and sneezes, as well as via shared personal items. You can also spread or contract it by touching your eyes before washing your hands. It's even possible to reinfect yourself in these ways. Conjunctivitis in adults is usually viral.
SEE RELATED: How long does pink eye last?
Pink eye caused by bacteria
Bacterial pink eye is also extremely contagious. It is often due to staph and strep bacteria. The bacteria that cause pneumonia (Haemophilus influenzae) and ear and sinus infections (Moraxella catarrhalis) can also cause this type of infection.
However, it can also be caused by more threatening types of bacteria. Sexually transmitted bacterial infections, such as gonorrhea and chlamydia, can cause pink eye in adults and newborns.
The bacterial form spreads in ways much like the viral form. These include coughs and sneezes, infrequent hand washing and physical contact with an infected person. Children are equally likely to contract bacterial or viral pink eye.
In some cases, bacterial conjunctivitis can cause serious damage to the eye if left untreated. Schedule an appointment with an eye doctor if symptoms get worse or don’t start to go away within a few days.
Allergic conjunctivitis
Common allergens like pollen, dust and animal dander can often lead to allergic conjunctivitis. This is especially true for people who are susceptible to eye allergies. Itchy, red eyes may be seasonal (e.g., pollen) or flare up year-round (e.g., dust and pet dander).
The whites of our eyes are covered with a thin, clear membrane called the conjunctiva. When tiny allergen particles come into contact with the conjunctiva, it can become inflamed. This inflammation is what causes itchy, watery, bloodshot eyes. Unlike the viral and bacterial types, allergic conjunctivitis is not contagious.
Treating the body’s response to the allergen can reduce or eliminate the eye-related symptoms. But whenever possible, the best course of action is to avoid the allergen altogether.
SEE RELATED: How is pink eye treated?
Other conjunctivitis causes

Most other causes of conjunctivitis fall under the broad umbrella of “irritants.” However, irritant conjunctivitis is often broken into subtypes based on the kinds of irritants that cause it.
The viral, bacterial and allergic forms can also be broken into subtypes. For example, they may be acute (short-lived) or chronic (lingering). Neonatal conjunctivitis is a subtype based on age — it is pink eye that occurs in newborns.
SEE RELATED: Gonococcal Conjunctivitis
Pink eye caused by irritants
An eye irritant can be anything from a foreign object in the eye to strong fumes. The basic definition of conjunctivitis is an inflammation or infection of the eye’s conjunctiva. So, beyond viruses, bacteria and allergens, nearly anything that irritates the eye can lead to conjunctivitis.
For example, a loose eyelash, strong chemical fumes, smoke and perfume sprays can all inflame the eyes. The irritant forms of conjunctivitis are not contagious.
Giant papillary conjunctivitis (GPC)
GPC is a combination of the allergic and irritant types. It is caused by a foreign body in the eye, most usually soft contact lenses. It can also develop due to wearing a prosthetic eye or to having sutures after an eye surgery.
GPC is characterized by bumps (called papillae) that appear inside the upper eyelid. These bumps are part of an abnormal immune response to eyelid irritation. In GPC, the irritation may be due to protein deposits on the foreign object, friction from the object, or both.
Chemical pink eye
Chemical conjunctivitis is another subtype of the irritant form. It’s the name sometimes used for cases that are caused specifically by a chemical irritant.
Chemical fumes and splashes, swimming pool chlorine, smoke and air pollution are all types of chemical irritants. The name can also refer to neonatal conjunctivitis caused by eye drops given to newborns.
Toxic conjunctivitis
This form is another example of irritant conjunctivitis caused by a chemical. It can develop as a toxicity reaction or as an immune response to certain types of eye drops.
Usually, it is due to the preservatives in the eye drops, but it can also be a reaction to the drops’ active ingredient. Toxic conjunctivitis generally develops gradually, over many weeks of using the eye drops.
Ophthalmia neonatorum
Also called neonatal conjunctivitis, ophthalmia neonatorum is the name used for pink eye in newborns. It is often caused by the sexually transmitted bacterial infections chlamydia and gonorrhea. Newborns can contract these infections when passing through the birth canal.
Rarely, ophthalmia neonatorum can also be caused by the eye drops given to newborns to prevent these bacterial infections.
Recurring pink eye
There are a few different reasons that pink eye may recur (keep coming back). Some are related to the cause of the infection or inflammation. However, most recurring cases are due to re-exposure or not following treatment instructions.
Bacterial pink eye, like any bacterial infection, can come back if antibiotic treatment is stopped too soon. Bacterial and viral forms can both keep reappearing if you don’t take steps to prevent reinfecting yourself. You should wash your hands frequently, change your pillowcases nightly and avoid reusing towels. You should also throw out any contaminated cosmetics and discard contact lenses after each wear.
You may also be reinfected if others in your home, office or classroom have pink eye. As long as symptoms are present, everyone should be extra cautious about spreading and contracting the infection.
Allergic conjunctivitis is not contagious, but it will typically recur any time you are exposed to your trigger allergens.
Chronic conjunctivitis means that the symptoms have lasted for four weeks or longer. It’s not the same as recurring pink eye, but in some cases, the symptoms may seem to come and go.
Chronic forms are typically related to other eye conditions that are causing the primary inflammation. For example, blepharitis, meibomian gland dysfunction and dacryocystitis can lead to chronic conjunctivitis.
Bacterial pink eye can also become chronic in some cases. The viral forms generally do not become chronic. However, the molluscum contagiosum virus, if it spreads to the eyes, can lead to chronic conjunctivitis.
Risk factors and complications
The primary risk factors for developing conjunctivitis are related to a person’s environment and hygiene habits. There is no age limit — pink eye is common in all age groups.
Classrooms, offices and similar shared spaces are perfect breeding grounds for outbreaks of contagious pink eye. This is particularly true if people aren’t washing their hands often enough. Environment is also a factor with non-contagious types. Being exposed to eye irritants and allergens will increase the risk of developing conjunctivitis.
Wearing contact lenses can also be a risk factor. Improper cleaning and storing of contacts can lead to eye inflammation and infection. And wearing contact lenses for too long can lead to inflammation, GPC and other more serious eye conditions. You should never wear contact lenses past their recommended life cycle. And never sleep in them, unless specifically prescribed by your eye doctor.
The most common types of pink eye do not generally cause any harmful complications. But complications are possible, especially in newborns and in severe or chronic cases. If left untreated, these cases can cause vision-threatening corneal damage and other problems.
When to see an eye doctor
You should see an eye doctor if your symptoms haven’t begun to get better after a few days or if they continue to get worse. Extended or worsening symptoms may mean you have a more serious form of pink eye, or they could be due to a totally different eye condition.
It's also important to see an eye doctor if your symptoms do not respond to antibiotic treatment within three to five days. This could indicate a misdiagnosis or an underlying eye condition.
While serious conditions or complications are rare, they can happen. An eye care professional will be able to diagnose your condition and rule out any other type of eye infection. They’ll also prescribe any necessary treatment and give you the best advice on how to ease your symptoms at home.
Any time you experience extreme eye redness or pain, or if your vision is affected, you should schedule an appointment with an eye doctor as soon as possible.