Bell’s palsy and its effects on the eye
Bell’s palsy is a condition in which the muscles on one side of the face are weakened or paralyzed. This often occurs due to irritation or pinching of the 7th cranial nerve, which controls the facial muscles. It can also occur in response to a viral infection.
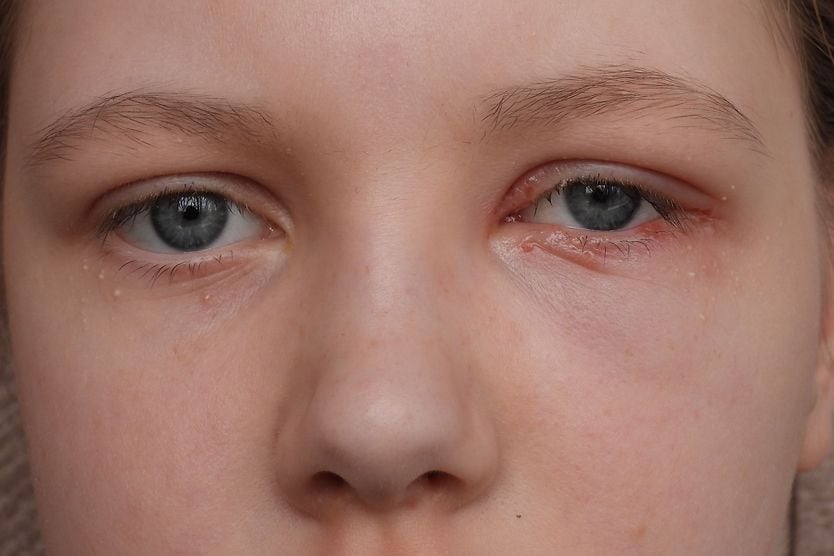
The main impact Bell’s palsy can have on eye health is that the affected eye may not close completely when blinking. This can cause blurred vision, dryness and irritation of the eye’s surface (the cornea). Without treatment, these issues can lead to other eye-related complications.
What is Bell’s palsy?
Bell’s palsy, sometimes called “facial palsy,” is the temporary paralysis or weakening of muscles on one half of the face. The name “Bell’s palsy” stems from Charles Bell, a Scottish neurologist who first identified and reported the condition, and palsy, which means paralysis.
The muscles affected by Bell’s palsy are controlled by the 7th cranial nerve (also called the facial nerve). The facial nerve extends from the base of the brain to the side of the face, where its fibers branch out and control:
- Facial muscles and expression
- Eyelid and forehead movement
- Taste sensations in certain areas of the tongue
- Our ability to moderate noise sensitivity
When the facial nerve becomes pinched or swollen, it can prevent the nerve fibers from working. This may cause one side of the face to become stiff or droopy, which is most noticeable when trying to smile. Difficulty closing the eye or raising the eyebrow on the affected side is also common.
Out of every 100,000 people, 15 to 30 develop Bell’s palsy every year. Though the average onset age is 40, it can affect people between the ages of 15 to 60. The condition affects men and women equally.
Bell’s palsy vs. facial palsy
Bell’s palsy and facial palsy are often used interchangeably. While this is not inaccurate, the two aren’t technically the same.
Facial palsy is the general term used to describe paralysis affecting areas of the face. There are different types of facial palsy, which include Bell’s palsy, the most common type.
Bell’s palsy vs. Ramsay Hunt syndrome
Bell’s palsy and Ramsay Hunt syndrome are both types of facial palsy. While many of the paralysis symptoms are the same, there are a few key differences between the two:
Cause
Cases of Ramsay Hunt syndrome are linked to the varicella-zoster virus (VZV). This is the same viral infection that causes chicken pox.
Bell’s palsy does not have a confirmed cause.
Ear pain
In addition to facial paralysis, ear pain and achiness are symptoms of Ramsay Hunt syndrome. It’s also possible for hearing to be affected or lost. While ear pain can be an early sign of Bell’s palsy, it, as well as hearing loss, is not common.
Facial rash
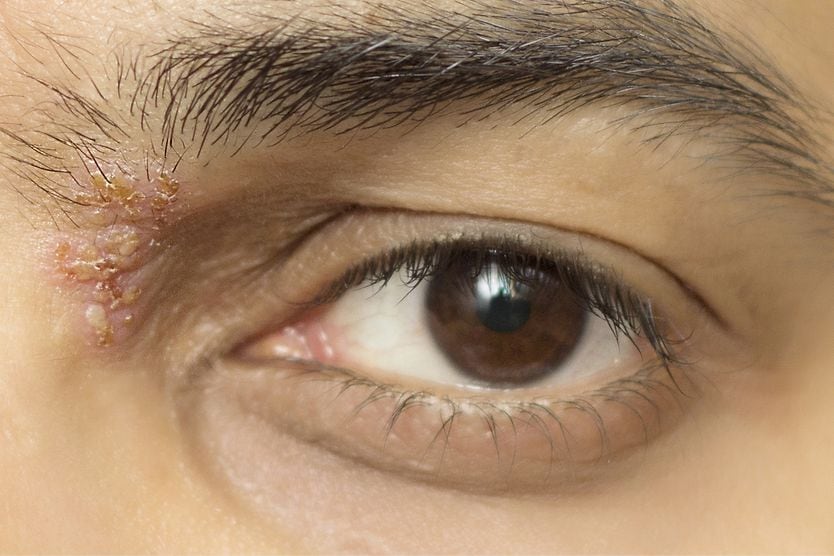
Perhaps the most significant difference between Ramsay Hunt syndrome and Bell’s palsy is the facial rash associated with Ramsay Hunt. A red, painful rash can develop on the face of those affected, and fluid-filled blisters may form around the mouth.
Symptoms of Bell’s palsy do not include a facial rash.
Bell’s palsy symptoms
Symptoms of Bell’s palsy show up suddenly and progressively worsen over 48 to 72 hours after the first signs appear. The most common symptom of Bell’s palsy is drooping of the face and mouth that affects only half of the face.
Early symptoms that may indicate the onset of Bell’s palsy are:
- Mild fever
- Stiffness in the neck
- Pain around the jaw or in/behind the ear
- Change in sensation, like weakness or stiffness, on one side of the face
- Increased or decreased sensitivity to sounds (hyperacusis)
- Loss of taste on half of the front part of the tongue
Additional facial palsy symptoms may include:
- Inability to control the muscles responsible for facial expressions, such as smiling and raising the eyebrows
- Headache
- Inability to close the mouth on the affected side, which can make it difficult to eat or drink
- Drooling or mouth dryness caused by the inability to fully close the mouth
- Numbness or loss of feeling in the face
Facial symptoms of Bell’s palsy may look similar to those of a stroke. However, Bell’s palsy has no other neurological symptoms and is not life-threatening.
If other stroke-like symptoms accompany your facial droopiness, such as slurred speech, blurred vision and arm weakness, call 911 immediately.
Common eye complications associated with Bell’s palsy
Facial paralysis caused by Bell’s palsy can affect the eyes, just like other facial features. Some of the ways it impacts the eyes include:
- Difficulty blinking, squinting or closing the eye on the affected side
- Watering or tearing
- Redness
- Burning
- Feeling like there is something in the eye
- Blurry vision
Blinking and closing the eyes fully helps distribute tear film across the eye’s surface. This tear film keeps the eyes healthy and comfortable. If facial palsy prevents proper blinking, dry eyes can occur. The other complications listed (watering, redness, burning and irritation) are secondary symptoms of dry eyes.
It’s important to take extra precautions to keep the eyes moisturized while experiencing Bell’s palsy symptoms. If left untreated, complications of dry eye may occur, such as infection and injury to the cornea.
Generally, Bell’s palsy symptoms are temporary. Many people see a significant improvement within three weeks. About 80% of people recover completely within a few months. However, some symptoms may be permanent. It’s also important to note that Bell’s palsy can recur in 5% to 10% of people who have had it in the past.
SEE RELATED: Is eye twitching a sign of a stroke?
Causes of Bell’s palsy
The exact cause of Bell’s palsy is unknown. However, people who experience the condition usually have swelling and inflammation of cranial nerve seven (facial nerve). When this nerve swells, it presses against the narrow pathway that leads it through the skull. This compression or pinching of the facial nerve can lead to partial facial paralysis.
Many medical professionals think a viral infection causes the body’s immune system to start targeting the facial nerve, resulting in inflammation and swelling. Viral infections that have been linked to Bell’s palsy symptoms include:
- COVID-19
- Herpes simplex, a virus associated with cold sores and genital herpes
- Herpes zoster, a virus related to shingles and chickenpox
- Epstein-Barr virus, associated with mononucleosis (mono)
- Sarcoidosis, which causes inflammation of various organs
- Coxsackievirus, which is associated with hand-foot-and-mouth disease
- Cytomegalovirus (CMV) infections
- Mumps virus
- Rubella, also called German measles
- Tumors
Cases of facial palsy may also be caused by injury or exposure to toxic chemicals.
Risk factors
Risk factors that may trigger the development of facial palsy include:
- Being pregnant
- Having preeclampsia
- Being diabetic
- Having high blood pressure
- Being obese
- Having a history of Bell’s palsy (you’ve had it before)
- Having a chronic middle ear infection (Otitis media)
- Having had inner ear or mastoid surgery
Several preexisting conditions raise a person’s likelihood of facial paralysis, such as:
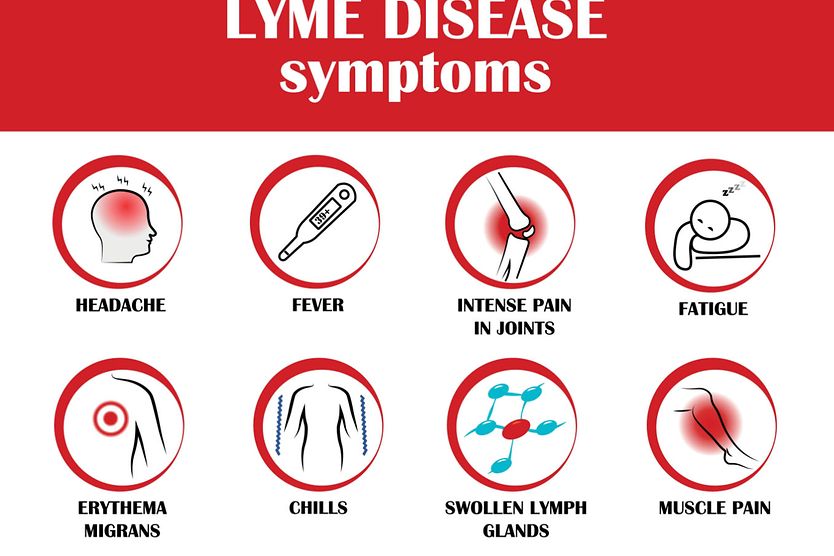
- Lyme disease
- Multiple sclerosis
- Guillain-Barré syndrome
- Myasthenia gravis
Diagnosis
There are no specific tests to diagnose Bell’s palsy. It can usually be diagnosed with a physical examination, meaning the doctor can determine a diagnosis by evaluating your physical appearance.
During an exam, your doctor will have you perform different facial tasks, such as smiling, whistling, raising your eyebrows and closing your eyes. While you perform these tasks, the doctor will watch your facial muscles to see if one side is weaker than the other.
To rule out a medical emergency, such as a stroke, your mobility, alertness, speech and other details may be examined.
Preexisting conditions may also be tested to ensure facial palsy is not a symptom of something more serious, including Lyme disease, brain tumor or diabetes. The tests used to accomplish this include:
- Electromyography (EMG) – This test provides information on nerve involvement, including whether there is any nerve damage, and its extent and severity.
- Magnetic resonance imaging (MRI) or computed tomography (CT) – These tests make sure a brain tumor or bone fracture isn’t compressing your nerves.
- Blood testing – Blood tests can determine whether Lyme disease, diabetes or other preexisting conditions are present.
SEE RELATED: Ophthalmoplegia
Bell’s palsy treatment
Symptoms of Bell’s palsy often improve over time without treatment. While facial muscle strength should return to normal after a few months, there are a few things you can do to aid in your recovery, such as:
Medical treatments
It’s important to consult with your eye doctor to determine what medical treatments will be optimal for your individual needs. Some things they may suggest are to:
- Apply eye drops regularly in the affected eye to keep the cornea moist and healthy.
- Reduce inflammation by taking corticosteroid drugs.
- Relieve pain and discomfort with ibuprofen, acetaminophen or other over-the-counter pain medications.
- Treat infection with antibacterial or antiviral therapy if it’s determined that a virus or bacteria caused your symptoms.
- Wear an eye patch or covering over the affected eye, or use special eyelid tape to keep the eye closed to prevent injury, irritation or drying.
Surgical options
Surgical intervention for Bell’s palsy is reserved for people who have little to no recovery after 10-12 months from the onset of symptoms. Some surgical options to consider include:
Botulinum toxin
Botulinum toxin is a non-invasive medical procedure in which a chemical is injected into specific muscles or muscle groups. It blocks neuromuscular signals, temporarily weakening the muscles in the injected area. This procedure, also called chemodenervation, can help restore balance in the face by relaxing muscles on the unaffected side.
Neuromyectomy or selective neuromyectomy
This outpatient procedure consists of surgeons altering nerves in the face. They first identify which nerve branches are interfering with the patient’s facial expressions. Then, they will disconnect or remove these nerve branches to provide a more balanced facial appearance.
Neuromyectomy is more invasive than chemodenervation. It is usually reserved for people who do not have the desired outcome from botulinum toxin injections. However, some doctors will combine treatments to potentially optimize outcomes.
Facial muscle excision
For patients whose smile is particularly affected by Bell’s palsy, a couple of excision procedures can help. These procedures can be performed under local anesthesia and consist of removing muscle fibers from facial muscles that interfere with a “normal” smile.
The two main muscles that affect this are:
- Depressor anguli oris (DAO) – The muscle connects the corner of the mouth to the lower jaw and helps the mouth frown.
- Depressor labii inferioris (DLI) – The muscle that lowers the bottom lip to reveal the teeth when smiling.
The procedures take around 30 minutes, and the incisions are made inside the mouth.
Cross-facial nerve graft
This procedure consists of taking bits of the facial nerve from the active side of the face and moving it to the paralyzed side.
Surgeons take from a leg of the active nerve and use it as a channel for new, healthy nerves to grow from. Doing this ensures the donating facial nerve isn’t compromised.
This treatment consists of two separate procedures:
- Part 1: Moving parts of the healthy nerve to the affected side of the face
- Part 2: Transplanting muscle from another area of the body and attaching it to the transplanted nerve
The recovery time for this procedure is longer than for others. Talk to your eye doctor about the pros and cons of cross-facial nerve grafting to help determine whether it’s a good fit.
Therapeutic interventions
If you prefer alternative medicine as a means of Bell’s palsy treatment, you may consider:
- Relaxation
- Electrical stimulation
- Vitamin therapy using B6, B12 and zinc
- Acupuncture
- Biofeedback training
- Physical therapy exercises to rebuild strength in the facial muscles
- Stimulating the facial muscles with a facial massage
Prognosis
While facial palsy may be an undesirable experience, your nerve function will likely return over time. In fact, 80% of people with symptoms of Bell’s palsy will recover within a few months, with children having the highest chance of making a complete recovery.
With this in mind, it’s important to know that the possibility of a full and quick recovery depends on the severity of symptoms and the level of nerve damage. Those who experience complete muscle paralysis will likely have a longer recovery period.
Potential complications
Complications of Bell’s palsy can have a direct effect on your vision. It’s usually difficult to fully close the eye on the affected side of the face, which can cause the eye to dry out. Excessive dryness in the eye can lead to:
- Corneal abrasions – Scratches on the eye’s surface caused by a foreign object
- Corneal ulcers – Open sores on the cornea
- Corneal erosions – Scratches on the eye’s surface due to dry eye and exposure
- Keratitis – Infection of the cornea
- Conjunctivitis – Infection of the membrane that covers the whites of the eyes (conjunctiva)
- Ingrown eyelashes (trichiasis)
- Madarosis (eyelash loss)
It’s important to maintain corneal protection by keeping the eyes hydrated. Some ways to accomplish this are to:
- Use eye drops throughout the day.
- Wear a sleep mask or a moisture chamber, or apply ointment to the eyes at bedtime.
- Stay hydrated by drinking plenty of water.
- Use a warm compress on the eyes to help meibomian gland function.
- Take regular breaks when using a digital screen.
Protecting your eye health with Bell’s palsy
Facial palsy can affect many facial features, including the eyes. While symptoms often resolve on their own, it’s important to keep your eyes hydrated, clear and safe while you recover. If you’ve been diagnosed with Bell’s palsy, talk to your eye doctor and create a game plan to maintain your eye health.
If you haven’t been diagnosed with Bell’s palsy but notice stiffness, tingling or numbness on one side of your face, seek medical attention. The sooner medical intervention occurs for your Bell’s palsy symptoms, the better your chance is for a quick and full recovery.
READ MORE: What is a neuro-ophthalmologist?