What is the trigeminal nerve?
The trigeminal nerve, also known as cranial nerve 5, is a nerve that provides both sensory and motor function to different parts of the face and head. Sensory functions include sending touch, temperature and pain signals from the face to the brain. Motor functions include chewing and swallowing.
Of the 12 cranial nerves, the trigeminal nerve is the largest. It has three branches that split off into the upper, middle and lower parts of the head and face.
Damage or irritation to the trigeminal nerve can result in severe pain or numbness.
Cranial nerve 5 anatomy
There are two trigeminal nerves — one on each side of the body. The nerves start in the brain and extend throughout the face and head.
The trigeminal nerve starts as four different nuclei: Three sensory and one motor. The sensory nuclei combine to form what’s known as the “sensory root.” By itself, the motor nucleus creates the “motor root.”
Both the sensory root and the motor root are located near the pons (the largest part of the brainstem). Because three nuclei make up the sensory root, it is fairly large. Meanwhile, the motor root is slim because it consists of only one nucleus.
As the sensory root exits the brainstem on each side, it becomes the trigeminal ganglion (a cluster of sensory neurons). For perspective, the trigeminal ganglion is positioned in front of each ear, near your temples. The trigeminal ganglion then splits into three branches that spread to and service various parts of the face.
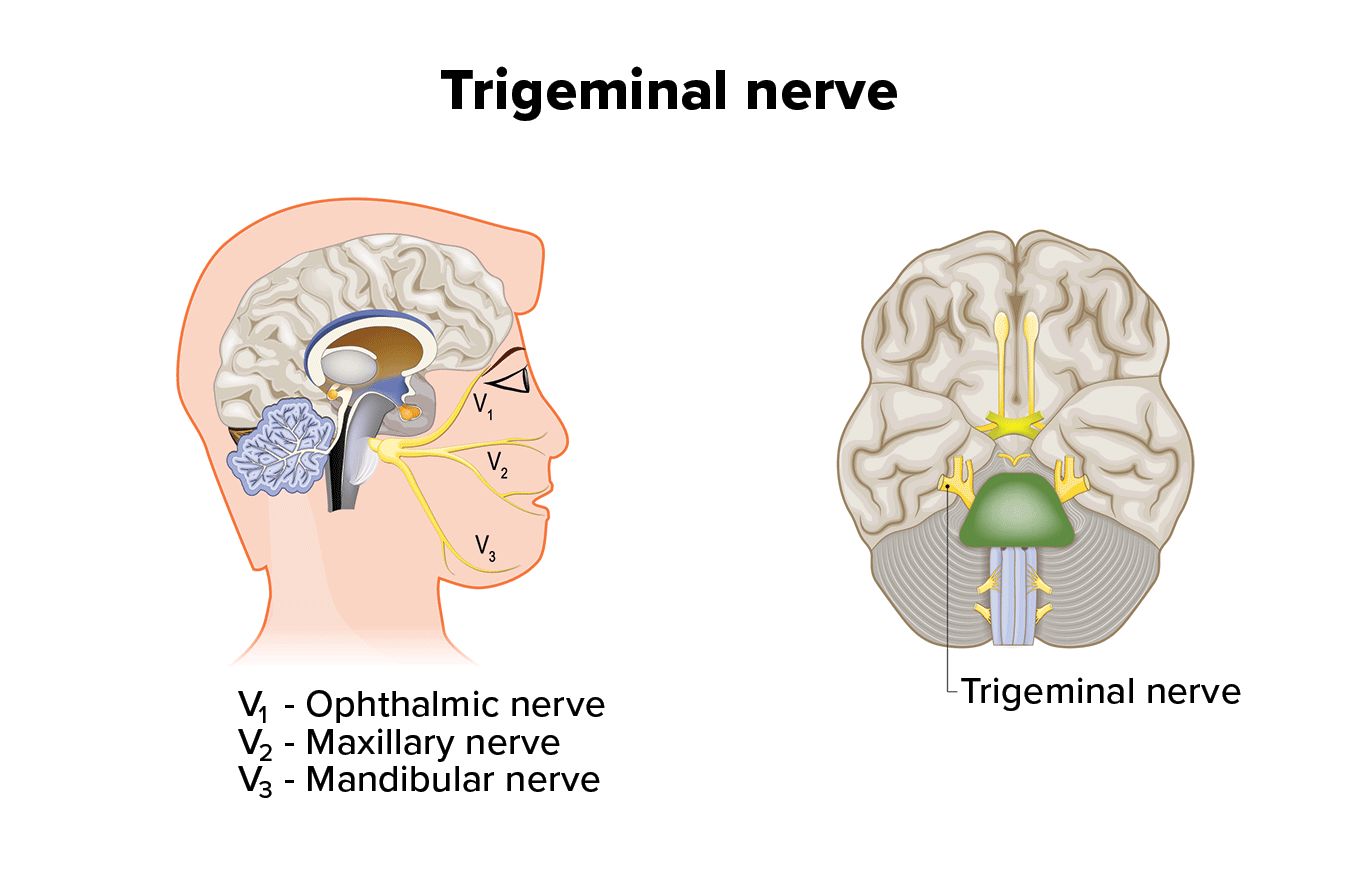
The three trigeminal nerve branches include:
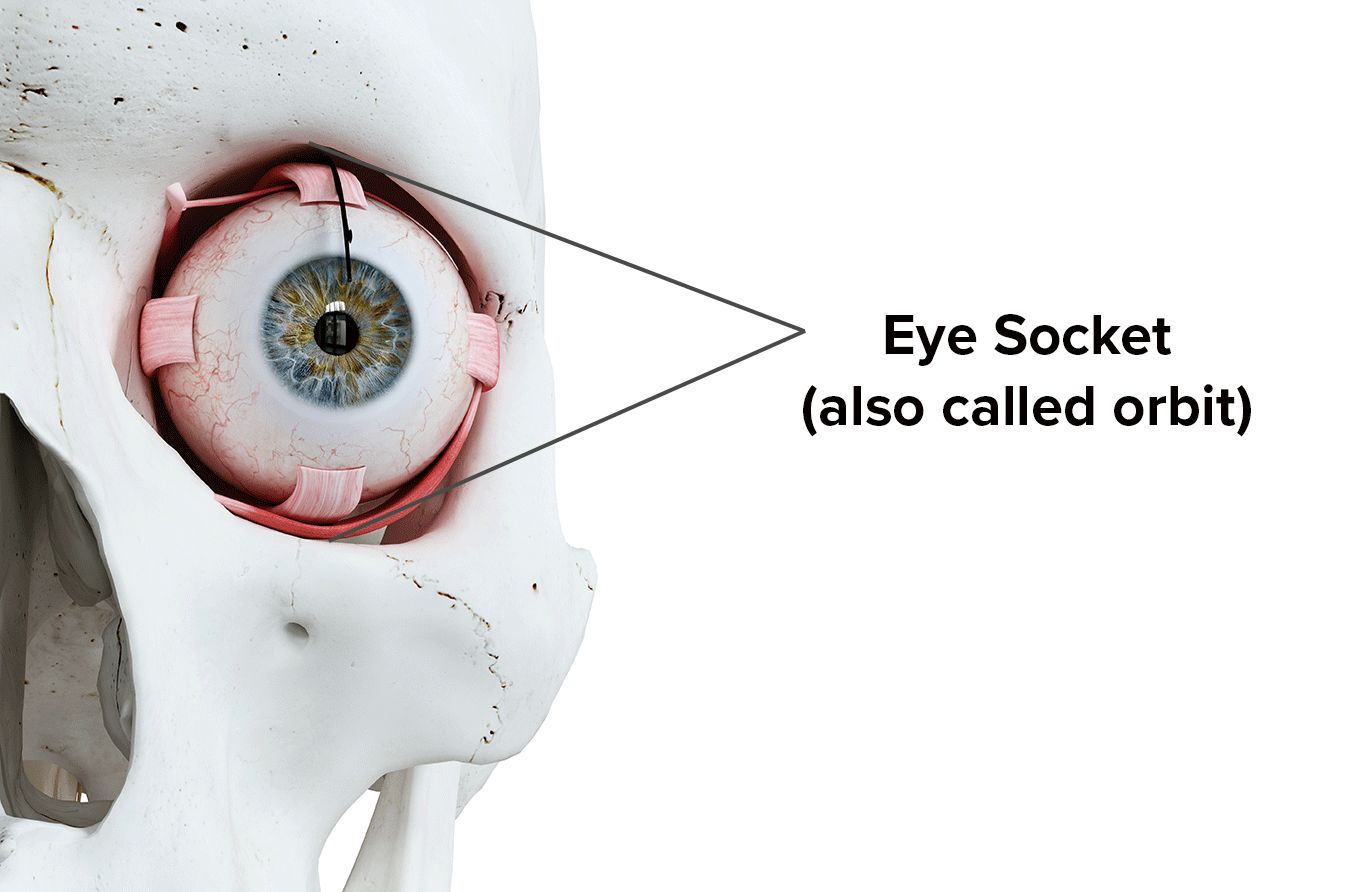
- The ophthalmic nerve – This nerve is connected to sensory receptors in parts of the eyes, such as the eyelid and cornea. The forehead and parts of the nasal cavity are also controlled.
- The maxillary nerve – This nerve gives sensation to the sides of the nose, cheeks, upper lip, teeth and gums, and lower eyelid.
- The mandibular nerve – This nerve is connected to the jaws, tongue, lower lip, teeth and gums, and mucosa in the mouth.
When the motor root exits the brainstem, it bypasses the trigeminal ganglion and meets back up with the mandibular branch. It helps the mandibular branch by supplying nerves to the muscles used in mastication (chewing).
The motor root also innervates the tensor tympani muscle located in the middle ear. Because of this, the mandibular branch is considered both a sensory and motor nerve.
Trigeminal nerve function
The function of the trigeminal nerve includes sending sensory and motor signals to the face. Sensory information provided by the nerve includes temperature, pain and touch.
The motor portion in the mandibular branch connects to the primary muscles used in chewing.
This includes the:
- Masseter muscle – allows you to move the lower jaw (mandible) forward and backward
- Lateral pterygoid muscle – controls the opening of the mandible and its side-to-side movement
- Medial pterygoid muscle – works with the lateral pterygoid muscle for side-to-side movement, and allows you to lift the jaw from open to close
- Temporalis muscle – assists the medial pterygoid muscle in jaw elevation, and helps the masseter muscle with jaw retraction
The motor portion also connects to muscles in the inner ear.
The trigeminal nerve also supplies motor nerves to the front two-thirds of the tongue, but does not supply the sense of taste.
SEE RELATED: 7th Cranial Nerve
Problems that can affect the trigeminal nerve
Damage, irritation and/or compression of the trigeminal nerve can affect it. This can happen when a tumor is present and pressing on the trigeminal nerve. It may also occur from an accident or dental surgery that results in trauma to the nerve.
Problems with the trigeminal nerve often present as pain, numbness and weakness in the affected area. The area may be as small as a portion of your gum, or as large as half of your face, depending on the location and extent of the damage.
Injury to the trigeminal nerve often heals and returns to normal over time. When severe damage affects the nerve, surgery to repair or replace the nerve may be needed.
SEE RELATED: Sixth nerve palsy
Trigeminal neuralgia
Trigeminal neuralgia (TN) is a condition in which damage to cranial nerve 5 causes severe pain in an area of the face. The pain is sudden and sporadic, and is often compared to an electric shock.
There are two types of trigeminal neuralgia that are differentiated by their symptoms.
Type 1 (TN1) is characterized by intermittent but intense facial pain that may last anywhere from a few seconds to a couple of minutes. Episodes can occur periodically or constantly during the day and night. They are often triggered by talking, chewing or touching the affected area.
Type 2 (TN2) affects patients differently in that it creates a constant, duller pain than what’s experienced in TN1. While stabbing pain is possible, people with TN2 usually describe their pain as burning or aching.
What causes trigeminal neuralgia?
Damage to cranial nerve 5 is what causes TN. Nerve damage could be caused by one or more of the following:
- Injury – The trigeminal nerve can be injured during sinus or dental surgery, facial trauma or stroke.
- Nerve compression – A blood vessel, tumor or cyst can press on the trigeminal nerve. This can erode or damage the coating that protects the nerve (myelin sheath).
- Autoimmune disorders – an autoimmune disorder, such as multiple sclerosis, can attack and deteriorate the trigeminal nerve’s myelin sheath.
- Arteriovenous malformation – an artery or vein can get tangled around the trigeminal nerve, resulting in irritation.
How do you treat trigeminal neuralgia?
Treatment for TN depends on the cause. Usually, doctors will start by prescribing medication to relieve or eliminate the symptoms. This is because surgery for TN carries a number of risks. If pharmaceuticals do not effectively treat the condition, surgery will be done.
Wallenberg syndrome (lateral medullary syndrome)
Wallenberg syndrome is a condition that occurs when a portion of the brainstem, called the medulla, gets damaged. Damage to the medulla usually occurs due to a stroke.
Lesions in the medulla can result in sensory loss in areas of the trigeminal nerve as well as trigeminal nerve pain. Treatment for this condition is symptomatic, which means the problem itself cannot be treated; only the symptoms you experience from it.
Reports say that gabapentin, an anti-epileptic drug, is often successful in treating patients who experience pain related to the condition.
When to see a doctor
It’s important to see a doctor if you notice sudden intense nerve pain in your face, or anywhere else on your body. This also goes for a sudden, unexplained headache with sharp, intense pain.
Seek medical attention if you experience any unexplained numbness or weakness, especially if it’s only on one side of the body. While this may indicate a nerve problem, it may also be a sign of a stroke.
Remember what to look for if you believe you or someone else is having a stroke. A helpful acronym to recognize symptoms is BE FAST:
B – balance problems, such as dizziness, stumbling, etc.
E – eye problems, such as blurry vision or double vision
F – facial drooping or numbness
A – arm weakness, or the inability to raise both arms equally at the same time
S – speech difficulties, such as slurring or rearranging words in sentences
T – time to call 911
READ MORE: Optic nerve