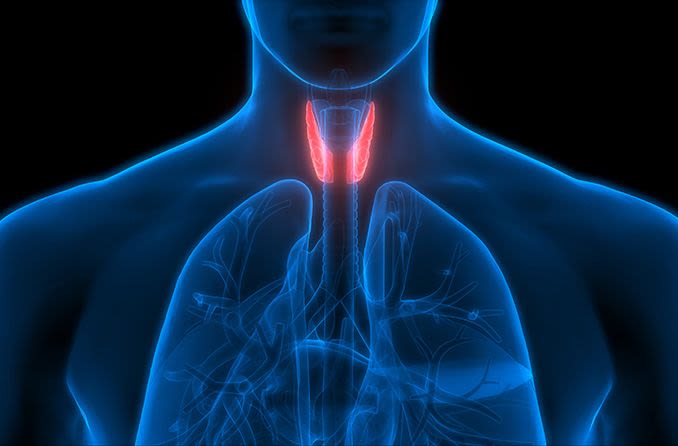
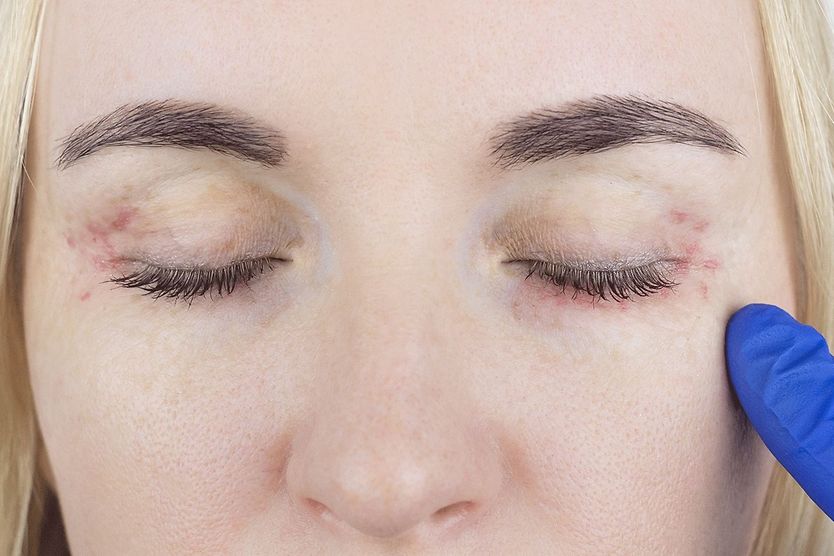
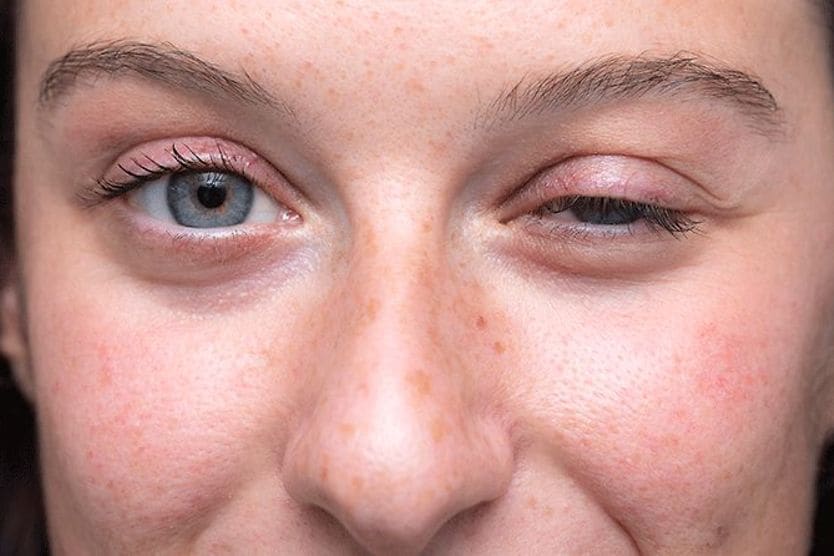
Thyroid eye disease (TED) is an autoimmune disorder that causes inflammation that can damage the fatty tissue, muscles and skin around the eyes. In autoimmune disorders, the immune system mistakenly attacks a healthy part of the body.
Inflammation and swelling from thyroid eye disease often cause the eyes to bulge outward and may lead to symptoms such as eye pain and double vision. The condition can vary from mild to moderate to severe.
There typically are two phases of thyroid eye disease:
Active phase – In the active phase, symptoms begin and get worse as tissue damage occurs, usually over a period of six months to two years.
Inactive phase – In the inactive phase, disease progress has stopped but some symptoms and eye changes may persist.
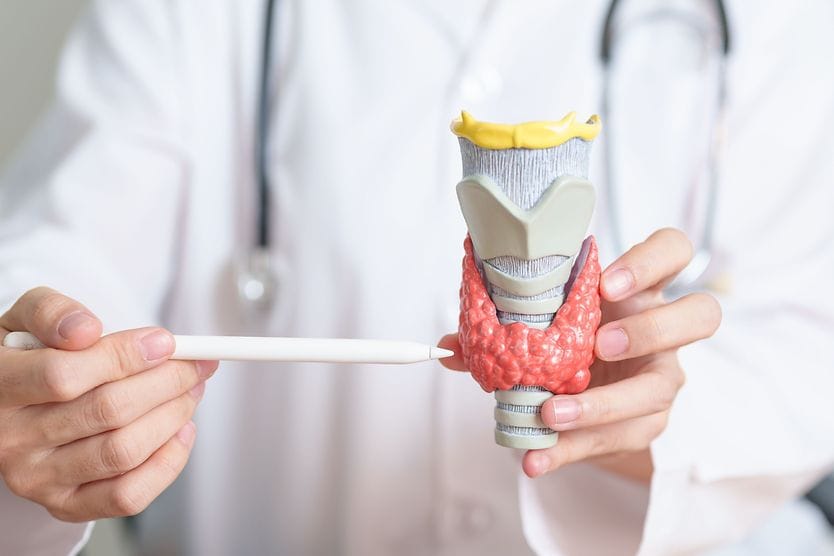
It is common for TED to occur along with Graves’ disease, an autoimmune disease that causes excess production of thyroid hormone (hyperthyroidism). For this reason, TED also may be referred to as Graves’ eye disease or Graves’ ophthalmopathy. The term thyroid eye disease is more accurate because the condition also may occur along with other types of thyroid disease.
Causes of thyroid eye disease
Doctors do not fully understand what causes TED. Some patients may have a genetic predisposition to developing it. That doesn't mean they will develop the disease, but they may if the gene gets “triggered” by other factors.
Several factors are linked with a higher risk of developing TED:
Certain health conditions – Patients with conditions such as Graves’ disease, type 1 diabetes or rheumatoid arthritis may be more likely to develop TED.
Family history – Patients who have a family member with TED or another autoimmune disease may be more likely to develop it.
Smoking – Patients who smoke have a higher risk of developing this disease than non-smokers.
Radioactive iodine therapy – This common treatment for hyperthyroidism increases the risk of developing TED.
Women also are more likely than men to be diagnosed with thyroid eye disease, and they make up 86% of all cases. TED occurs most commonly in middle-aged women.
About 90% of patients who develop the condition have an overactive thyroid (hyperthyroid) that produces too much thyroid hormone, such as with Graves’ disease. But about 1-3% of patients have an underactive thyroid (hypothyroid) that produces too little thyroid hormone. And up to 6% of patients may have normal thyroid function (euthyroid) and no diagnosed thyroid disease.
Eye problems with thyroid disease
It is common for patients with some types of thyroid disease to develop thyroid eye disease. Not all patients will develop eye problems, and the symptoms may vary in severity.
Thyroid eye disease symptoms
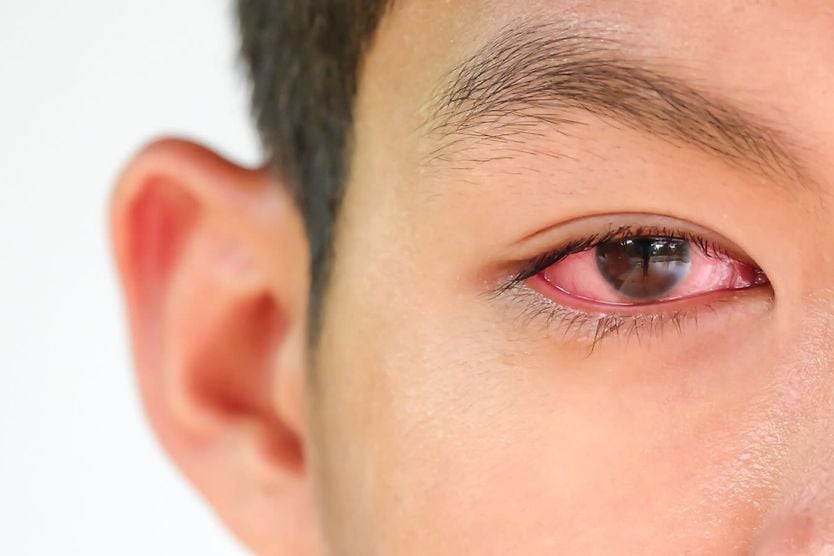
The symptoms of thyroid eye disease may become apparent during the active phase of the disease. Symptoms may include:
Bulging eyes (proptosis) or exophthalmos
Double vision (diplopia)
Eye pain
Feeling of grit or sand in the eye
Blurry vision
In severe cases, patients may have trouble moving their eyes. In a small percentage of cases (about 5%), patients may experience vision loss due to compression of the optic nerve.
Some patients also experience cosmetic changes around the eyes such as fat deposits or hollow areas that create shadows under the eyes.

Illustrated by Laurie O'Keefe
SEE RELATED: Puffy eyes
Frequency of symptoms
The frequency of eye problems associated with TED varies:
Eye surface problems that may result in blurry vision, a gritty feeling in the eyes and watery eyes occur in about 90% of patients with upper lid retraction.
Bulging eyes (proptosis) caused by inflammation and swelling of eye tissue occur in about 60% of patients.
Misalignment of the eyes (strabismus), along with double vision, occurs in about 40% of patients.
Patients may continue to experience some symptoms, such as bulging eyes and double vision, during the inactive phase of the disease.
The symptoms of TED may resemble the symptoms of other eye problems, so it’s important to see your eye doctor for an exam and diagnosis.
Getting a thyroid eye disease diagnosis
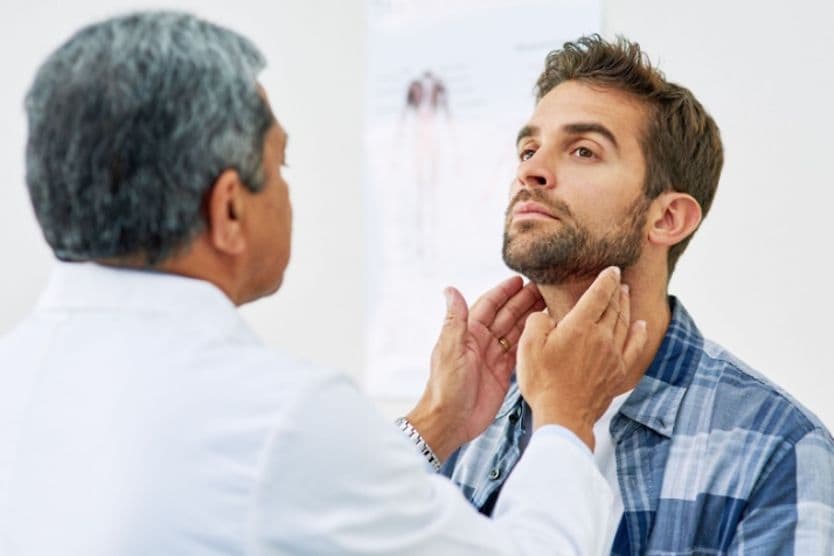
There may be several steps involved in getting a thyroid eye disease diagnosis. It’s important to visit your eye doctor for a comprehensive eye exam as a first step in determining whether your eye symptoms may be related to this condition.
There are several tests that you may need to undergo during the process of getting a diagnosis:
Eye measurement – During your eye exam, your eye doctor may use a measuring tool called an exophthalmometer to measure the degree of bulging (orbital proptosis) of your eyes.
Imaging – Your health care providers may use a computed tomography (CT) or magnetic resonance imaging (MRI) scan to visualize changes in muscle and fat tissue around the eyes to diagnose the disease.
Blood tests – Your doctor may order blood tests to check thyroid function and levels of thyroid hormones to detect hyperthyroidism or Graves’ disease.
In addition to visiting your eye doctor, you may also need to see additional doctors, such as an endocrinologist and/or an ear, nose and throat specialist. At some health centers or hospitals, a multi-specialty team of doctors works together to diagnose and treat TED.
The good news is that once diagnosed, most of the eye problems associated with TED can be managed by your collaborative care team.
Thyroid eye disease treatment
Treatment will depend on your symptoms and the phase and severity of the disease.
Current thyroid eye disease treatment options include drugs, surgery and an eye patch or special glasses for double vision. If you have Graves’ disease, you’ll need to seek treatment for it as well.
Common treatments that may help alleviate symptoms during the active phase of the disease include:
Using lubricating eye drops.
Wearing sunglasses.
Elevating the head of your bed to help reduce swelling.
An eye doctor also may prescribe glasses with prism for double vision, though this may not work for all patients.
Drugs for thyroid eye disease
In 2020, the U.S. Food & Drug Administration (FDA) approved a new infusion. The drug, teprotumumab-trbw, may significantly reduce eye-bulging and may improve double vision in TED patients.
Doctors may also use corticosteroids such as prednisone to reduce the inflammation and swelling caused by moderate to severe thyroid eye disease. However, steroids generally will not reduce eye-bulging or correct double vision.
Surgery for thyroid eye disease
Surgery is sometimes used to treat moderate to severe cases. Surgery usually is done during the inactive phase of the disease for cosmetic reasons and to treat symptoms such as double vision.
Not all patients will require all types of surgery. Types of surgery may include:
Orbital decompression surgery – This type of surgery involves removing fat around the eye (orbital fat) and possibly removing bone around the eye socket to allow the eye to sit further back. Orbital decompression surgery can help reduce eye-bulging and potentially prevent vision loss caused by pressure on the optic nerve.
Strabismus surgery – This surgery involves releasing tight muscles that result in misalignment of the eyes.
Eyelid surgery – Eyelid surgery may correct the retracted eyelids that occur in some patients.
Cosmetic surgery or procedures – Some patients seek surgery or other cosmetic procedures for fat deposits or undereye “bags” that result from TED. Instead of surgery, a doctor may be able to use botulinum toxin injections or “fillers” to fix these issues.
Thyroid eye disease may affect patients psychologically due to eye symptoms, vision loss or changes in appearance. For these reasons, patients may need to see a psychologist or other mental health professional for treatment for depression or anxiety related to the condition.
Regular eye exams and thyroid eye disease
Getting regular eye exams helps keep your eyes healthy and allows your doctor to spot any eye changes early. Catching a serious condition such as thyroid eye disease early may help mitigate or prevent serious damage that could result in vision loss.
If you haven't had an eye exam recently, consider making an appointment with your eye doctor today.