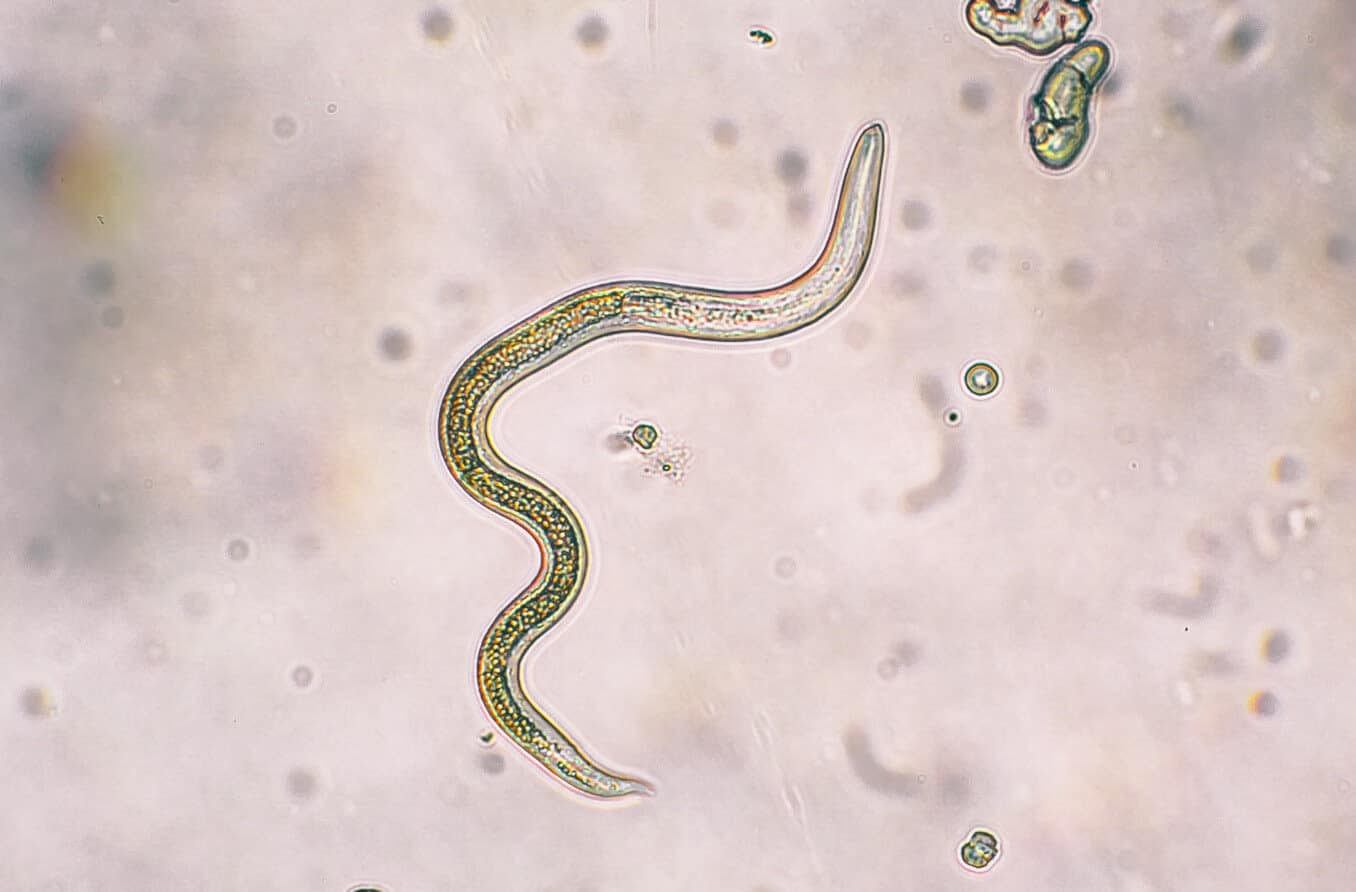
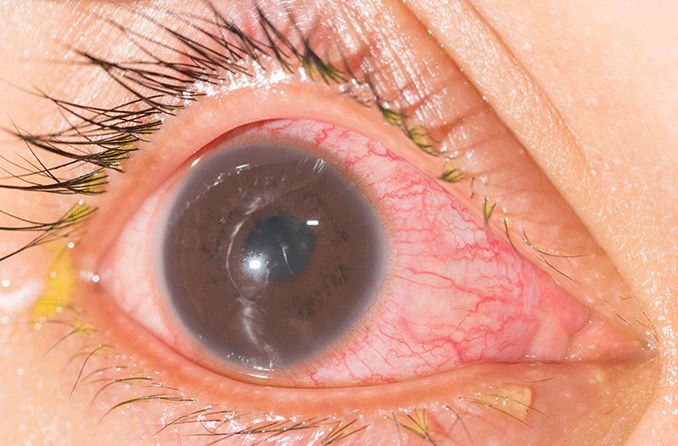
Onchocerciasis (pronounced “on·ko·ser·kai·a·sis”) is a disease caused by a parasitic worm called Onchocerca volvulus. The parasite is transmitted through bites from Simulium blackflies, which are known to live and breed near fast-flowing streams and rivers.
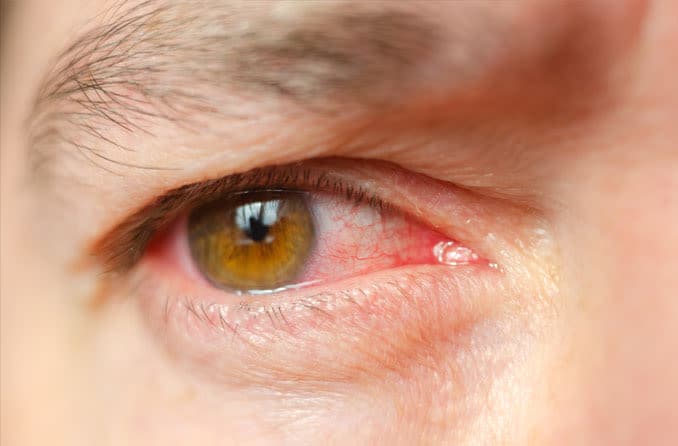
Those who are consistently bitten by infected flies may develop an itchy skin rash, sight-threatening eye disease and/or nodules beneath the skin. Treatment for the condition includes persistent administration of ivermectin and doxycycline until symptoms are no longer present.
What is river blindness?
The name “river blindness” — a common moniker for onchocerciasis — is a combination of the breeding place (typically a river or fast-flowing stream) of the flies that transmit the infection and a symptom of the disease (vision loss or blindness).
Incidents of river blindness tend to occur in tropical climates, with a majority of cases occurring in sub-Saharan African countries. Experts estimate that around 18 million to 25 million people are infected with onchocerciasis worldwide.
It usually takes several fly bites to become infected with a river blindness parasite. Those affected typically work or live in remote areas near rivers where the Simulium blackflies breed.
River blindness causes
Onchocerciasis is transmitted when a female blackfly infected with the parasitic worm (Onchocerca volvulus) bites a human host.
Baby worms (called larvae or microfilariae) are passed through the blackfly’s bite. Once transmitted, the larvae migrate to the skin and eyes, among other organs. The larvae use these locations to settle and mature into adult worms over 6 to 12 months.
Adult worms may live in nodules in the skin for up to 10 to 15 years, producing millions of microfilariae during their lifetime.
If an uninfected female blackfly bites a person who is infected with the parasite, the fly will become infected by ingesting the larvae in the infected person’s blood. The larvae will then grow and develop in the blackfly, which can then transmit the larvae to another human host.
SEE RELATED: Acanthamoeba keratitis: What contact lens wearers need to know
Onchocerciasis signs and symptoms
River blindness affects the eyes and skin and fluctuates, depending on where the parasites are in their life cycle. Symptoms commonly associated with the condition include:
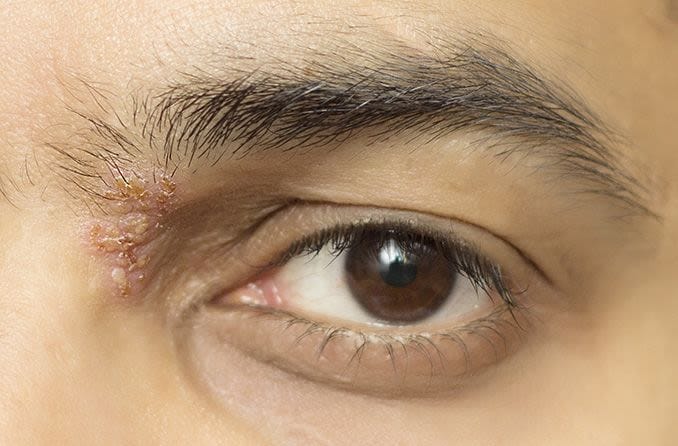
- Changes in the skin, such as pigmentation and elasticity, that make the skin appear thin
- Severe itching of the skin and eyes
- Eye lesions
- Nodules under the skin that form around adult worms
- Swollen femoral lymph nodes resulting in an enlarged groin
- Intense skin inflammation in response to the death of microfilariae
- Light sensitivity (photophobia)
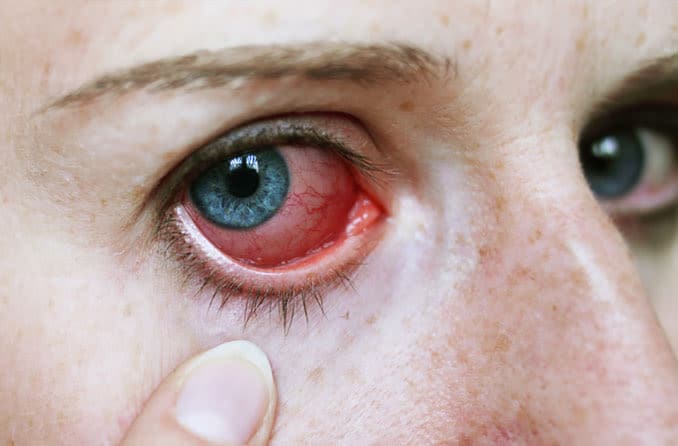
- Vision loss or blindness
It’s possible that symptoms won’t appear until microfilariae begin to die. However, the longer the infection, the worse the symptoms may become. In extreme, prolonged cases, blindness is the ultimate result. Onchocerciasis larvae cause blindness when they invade different tissues of the eye (including the cornea, retina, and optic nerve), causing inflammation, scars and damage.
Risk factors for river blindness
It’s very uncommon for casual tourists to become infected with onchocerciasis, as multiple and frequent bites are usually required before the infection is transmitted to a human.
However, if any of the following characteristics apply to you, you may be at a higher risk of contracting river blindness:
- You live in rural, agricultural regions of sub-Saharan Africa, Yemen, Latin America or parts of Asia.
- You work or reside near a fast-running stream or river, where Simulium blackflies are present.
- You are bitten by Simulium blackflies regularly.
Those who visit for extended stays in high-risk areas are also at a higher risk of becoming infected. This includes field researchers, missionaries, Peace Corps volunteers and other long-term tourists.
Diagnosis
Tourists who have been bitten several times by an infected female blackfly but have not had prolonged exposure can develop what’s considered a “light infection.” This is typically more difficult to diagnose than cases identified in infected residents.
River blindness can be diagnosed in several ways:
- Skin snip – The most common way to diagnose onchocerciasis, a skin snip involves shaving 1 to 2 mg of the skin from different areas of the body. The skin is put in a saline solution and observed under a microscope. Typically, any larvae present in the skin will emerge and be detected.
- Nodule examination – Affected individuals who present nodules under the skin can have the nodules surgically removed and biopsied for adult parasites.
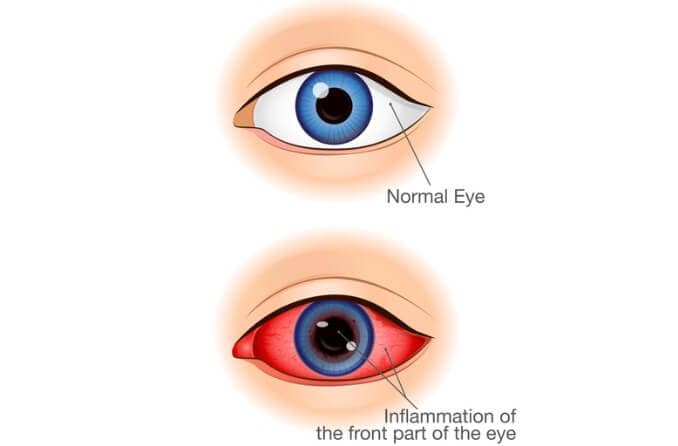
- Eye exam – Larvae that have migrated to the eyeballs can be detected through a slit-lamp eye exam. Larvae typically nest in the anterior (front) part of the eye, which results in the appearance of lesions. These lesions are visible and can be easily detected with an eye examination.
- Antibody test – Though not widely available, antibody tests can analyze for onchocerciasis infection. They are most useful for visitors who have been in high-risk areas, as the test cannot distinguish past infections from current ones. Certain antibody tests will specify if onchocerciasis is present, while other tests flag any sort of infectious parasite.
Onchocerciasis treatment
River blindness treatment consists of the drug ivermectin. Ivermectin is an anti-parasitic drug that can be taken orally or applied topically. For people infected with onchocerciasis, ivermectin should be administered every 6 to 12 months for the life cycle of an adult worm — about 10-15 years.
Ivermectin effectively kills the larvae but does not affect adult worms. Many physicians suggest having any nodules on the skin surgically removed, which eliminates the visible adult worms that may continue reproducing larvae over time.
For adult worms that are not visible, doxycycline is an effective antibiotic that kills the bacteria inside adult worms and microfilariae that are essential for onchocerciasis survival. Doxycycline is typically prescribed in six-week doses to treat river blindness and help stop or slow its spread.
When to see a doctor
If you’ve spent an extended period in a high-risk area and begin to notice changes in your skin and/or vision, it’s important to seek prompt medical attention.
As mentioned previously, it’s rare for casual tourists to become infected, as prolonged exposure is usually a factor in those who’ve contracted river blindness. However, if you’re exhibiting symptoms and are concerned you may be infected, a medical professional can help.
A doctor will perform the necessary tests and either put your suspicions to rest or confirm a diagnosis and establish thorough and effective treatment.
READ NEXT: Eye worms