What it means to have a tear duct infection
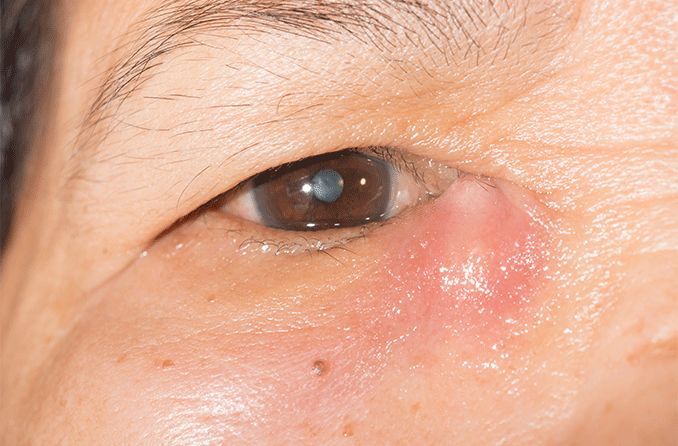
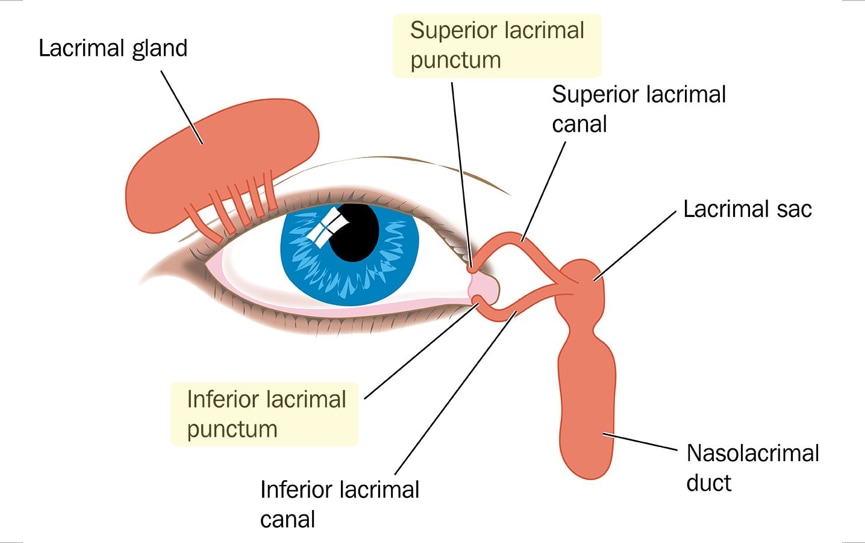
Dacryocystitis is an inflammation of the tear (or nasolacrimal) sac located in the inner corner of your eye. It is often due to blockage of the tear duct that leads tears from the tear sac into the nasal cavity. An infection can cause pain, swelling, watery eyes and discharge.
The condition, though not life-threatening, can be painful or irritating. Fortunately, dacryocystitis is treatable with antibiotics and, in some cases, surgery.
What is dacryocystitis?
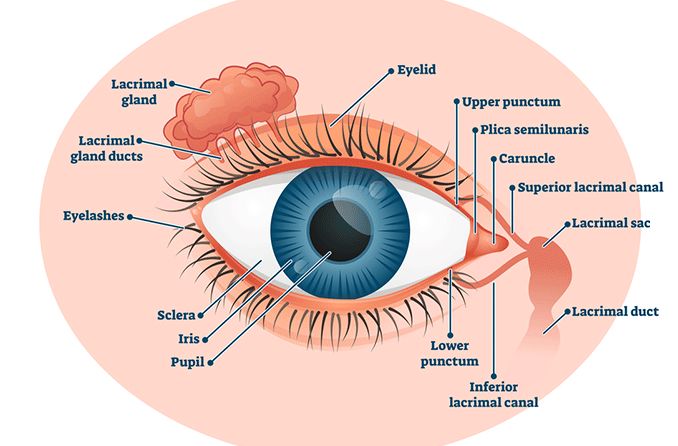
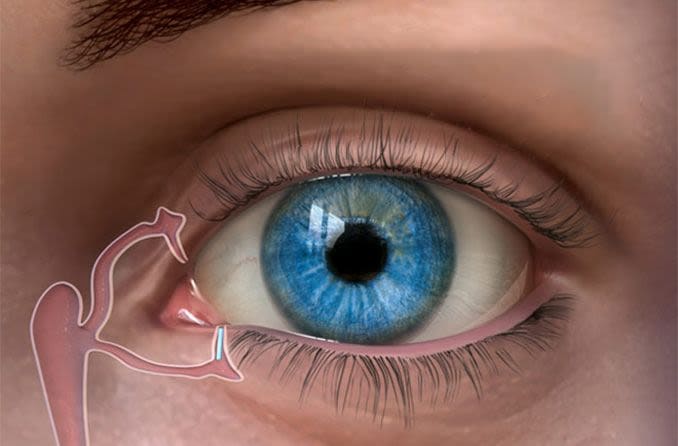
Dacryocystitis is the clinical name for inflammation or infection of the lacrimal sac. The lacrimal sac is located between the corner of the eye and the bridge of the nose. It is responsible for holding and releasing tears.
“Releasing tears” from the eye is most often associated with crying. But the lacrimal gland constantly releases small amounts of tears to keep the eye lubricated. Whenever you blink, the tears are spread across the eyes, keeping them clean, moist and healthy.

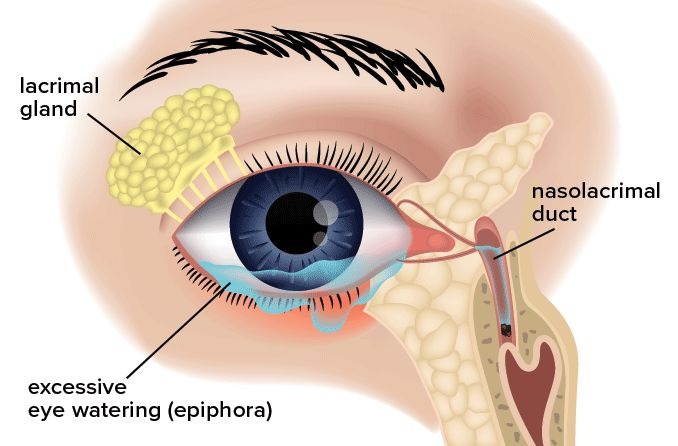
Attached to the lacrimal sac is the nasolacrimal duct (or tear duct). The lacrimal sac works as a channel to drain tears from the eye to the nasal cavity. Sometimes the tear duct becomes blocked due to infection, trauma, inflammation or other factors. When this happens, your tears are unable to drain correctly.
This causes the tears in the lacrimal sac to become backed up and stagnant, allowing bacteria to grow and infection to develop.
Acute dacryocystitis vs. chronic dacryocystitis
Dacryocystitis can be acute or chronic. Which one is determined by how long the condition lasts.
Acute dacryocystitis symptoms will develop quickly and be more severe than chronic dacryocystitis. However, symptoms will typically resolve in less than three months (even as little as a few days) with antibiotic treatment.
Chronic dacryocystitis symptoms appear gradually and are more mild than in acute cases. In fact, it’s possible for the only symptoms experienced to be eye watering and discharge.
While the symptoms may be relatively minor, chronic dacryocystitis symptoms will last for a prolonged period of time. Often, they can last more than three months. Plus, surgical treatment may be required.
SEE RELATED: Meibomian gland dysfunction (MGD): The cause of your dry eyes?
Dacryocystitis causes
Dacryocystitis is typically caused by a blockage in the nasolacrimal duct. This reduces tear flow and leads to bacteria growth and inflammation. Conditions that cause a tear duct blockage include:
- Sinus infections. Particularly in the maxillary sinuses located beneath your cheeks, near your nose.
- Exposure to the same bacteria that causes staph infection or strep.
- Abnormal tissue growth or tumors in the nasolacrimal system.
- Nasal inflammation or abscess.
- Trauma to the affected region. This is sometimes caused by nasal or sinus surgery. For example, endonasal or endoscopic procedures.
Dacryocystitis symptoms
Dacryocystitis symptoms vary depending on whether your condition is acute or chronic. As mentioned earlier, acute symptoms will appear quickly and may persist for up to three months.
These symptoms include:
- Fever
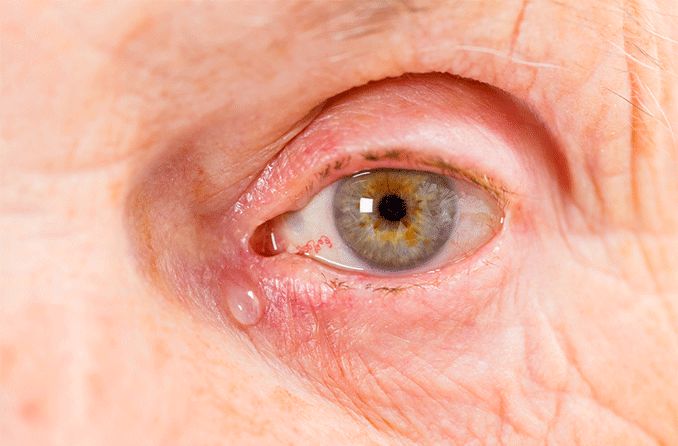
- Pain and redness in the inner corner of the eye
- Yellow or green eye discharge
- Swelling and, in severe cases, bruising in the inner corner of the eye, near the nose
- Watery eyes
- Eye redness
Symptoms of chronic dacryocystitis are not usually as severe as acute cases. The most common symptoms observed are excessive tearing and eye discharge. Fever and inflammation are not typically present in chronic dacryocystitis.
SEE RELATED: Pink eye (conjunctivitis): Symptoms, causes and treatment
Risk factors
Dacryocystitis is normally caused by a blockage in the tear duct. Certain characteristics can make an individual more susceptible to developing dacryocystitis. Risk factors include:
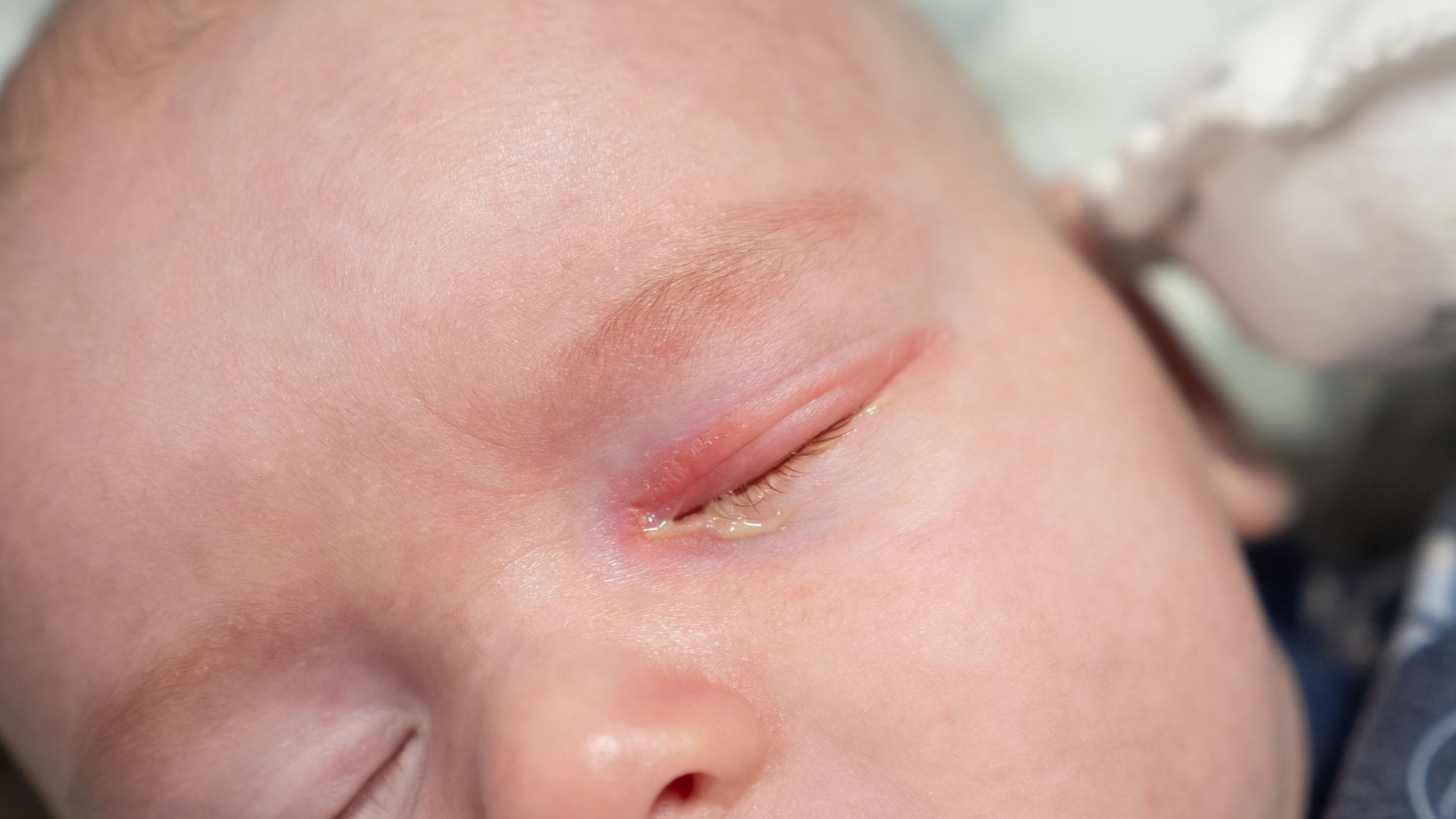
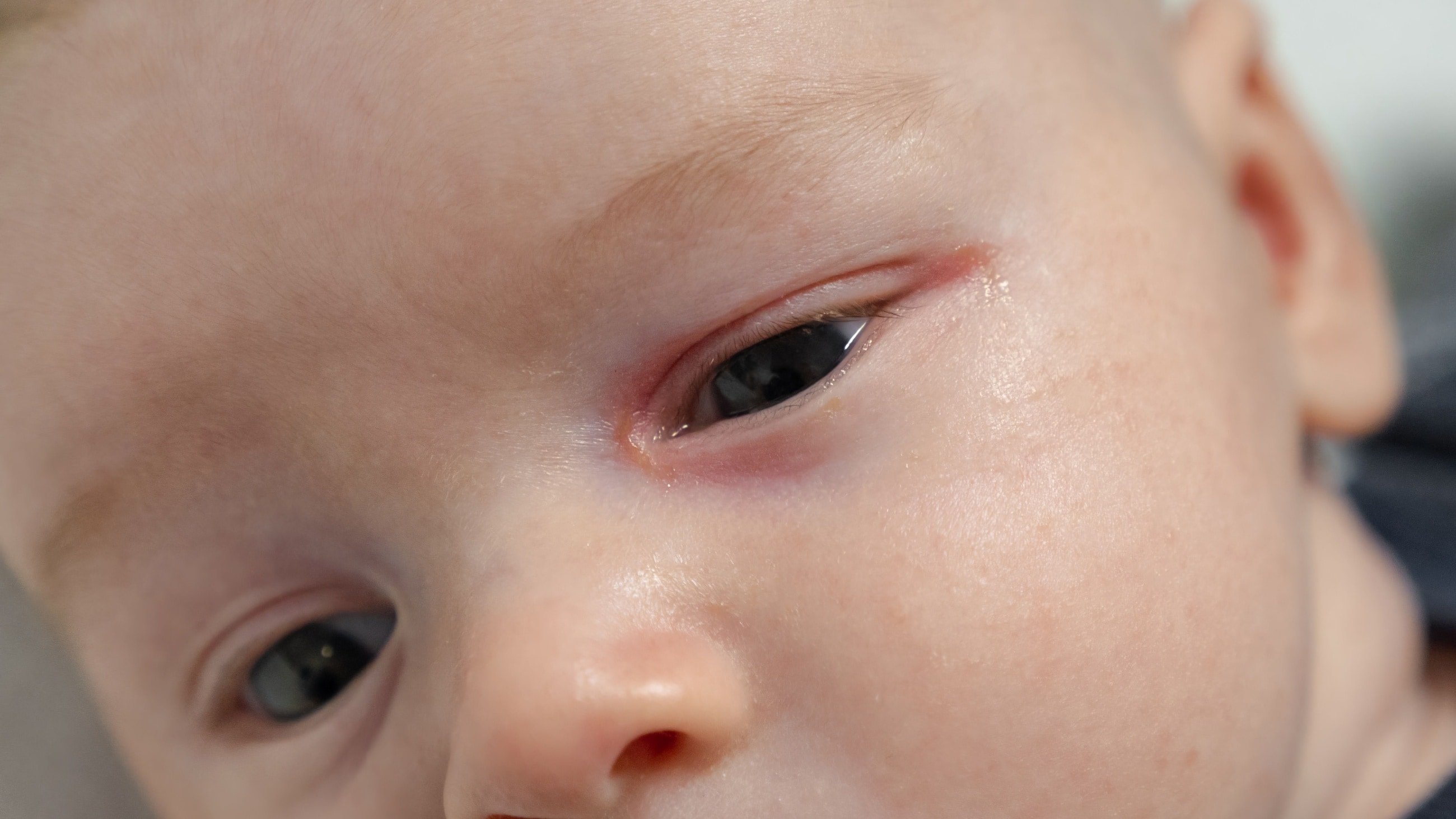
- Congenital tear duct obstruction. Babies can be born with one or more blocked tear ducts due to an underdeveloped tear drainage system or a duct abnormality. For this reason, it’s common for infants to develop dacryocystitis more than once during the first year of life. However, they will likely grow out of the blockage between 9 and 12 months.
- Certain medications. Examples include prescription eye drops to treat glaucoma, such as timolol and pilocarpine. Also antiviral medications such as trifluridine and idoxuridine. These have been known to increase the chance of tear duct infections.
- Being a woman. Females have tear ducts that are narrower than in males. This makes them more susceptible to having the ducts obstructed.
- Being over age 40. Punctual openings, which drain tears, narrow as you get older. This slows the draining process for tears and raises the risk of obstruction.
- Abnormal nasal structure. Conditions like nasal septum deviation, rhinitis (swelling of the nasal mucous membranes) or turbinate hypertrophy (inflammation of the tissue on the walls inside the nose). These can raise one’s risk of a blockage.
SEE RELATED: What vision issues are unique to women?
Dacryocystitis treatment
It is important to see your doctor if you suspect that you are experiencing dacryocystitis. Treatment for acute dacryocystitis mainly consists of antibiotics, which kill the infection-causing bacteria. Antibiotics can be administered orally with a pill, topically with an ointment or, in severe cases, intravenously (through an IV). Symptoms should resolve fairly quickly once antibiotic treatment begins.
You can relieve swelling or pain associated with acute dacryocystitis at home. For example, your doctor may recommend that you apply a clean, warm compress (a washcloth will work). You should apply to the affected area for 10 to 15 minutes, several times a day.
Over-the-counter pain relievers may also be recommended to manage pain or fever associated with dacryocystitis. These can provide relief until the antibiotics begin to work.
Surgery to widen the tear ducts may be necessary for chronic dacryocystitis sufferers. The first line of surgical treatment is probing, and is an in-office procedure.
This may be followed by additional surgical procedures. Procedures may include balloon dacryoplasty, intubation or stenting. If these surgeries are not successful, dacryocystorhinostomy may be necessary. This surgery uses a laser to remove pieces of bone surrounding the tear duct.
The goal of these procedures is to widen the duct passageways and removes any blockages.
Individuals with chronic dacryocystitis due to inflammatory causes may be prescribed steroid eye drops. The drops work by reducing inflammation and swelling that can cause the nasolacrimal duct to narrow.
When to see a doctor
It is recommended that you see an eye doctor if you suspect dacryocystitis symptoms. Acute dacryocystitis that goes untreated can develop into chronic dacryocystitis.
In rare cases — specifically in babies — the infection could spread to the eye socket. This can lead to orbital cellulitis, meningitis or a brain abscess. Each of these is an emergency condition.
If you or your child are showing dacryocystitis symptoms, schedule an appointment to see an eye doctor. They will be able to assess symptoms and make an official diagnosis. They can then help establish the best method of treatment for a quick recovery.
RELATED READING: Dacryoadenitis (lacrimal gland inflammation)