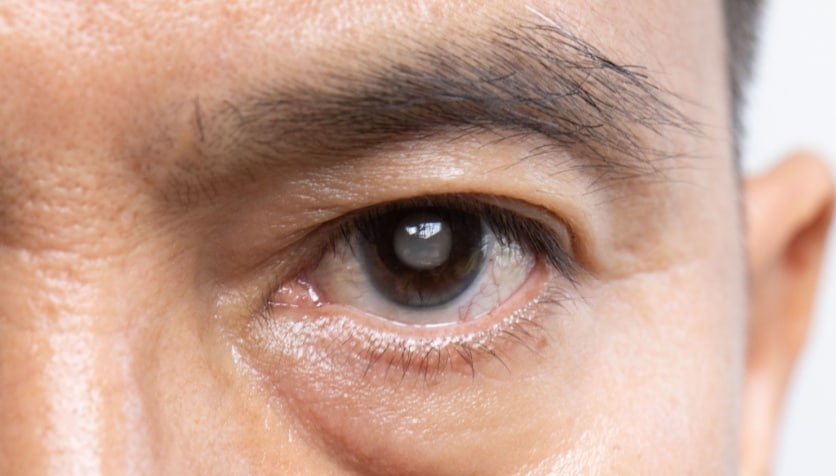
What are childhood cataracts?
A cataract is a clouding of the eye's natural lens. In children, these are called pediatric cataracts. They're also called childhood cataracts. Cataracts can distort the images a child sees. This can lead to blurry vision and other eyesight problems.
They can occur in one eye (a unilateral cataract) or both eyes (bilateral cataracts). Their size can range from tiny dots to thick clouds on or inside the lens.
Cataracts are typically rare in children. In the United States, about three to four in every 10,000 babies are born with them or develop them shortly after birth.
Why do some children develop cataracts?
Doctors don't always know why a child develops a cataract.
Around half of them are caused by genetic mutations. This can happen with genes inherited from either one or both parents.
They can also be caused by infections, injuries or health problems that affect the baby's metabolism.
Systemic (whole-body) diseases can cause cataracts in children too. Down syndrome is the most common condition associated with pediatric cataracts.
Symptoms
Not all types of pediatric cataracts affect a child's vision. But several types can cause visual problems.
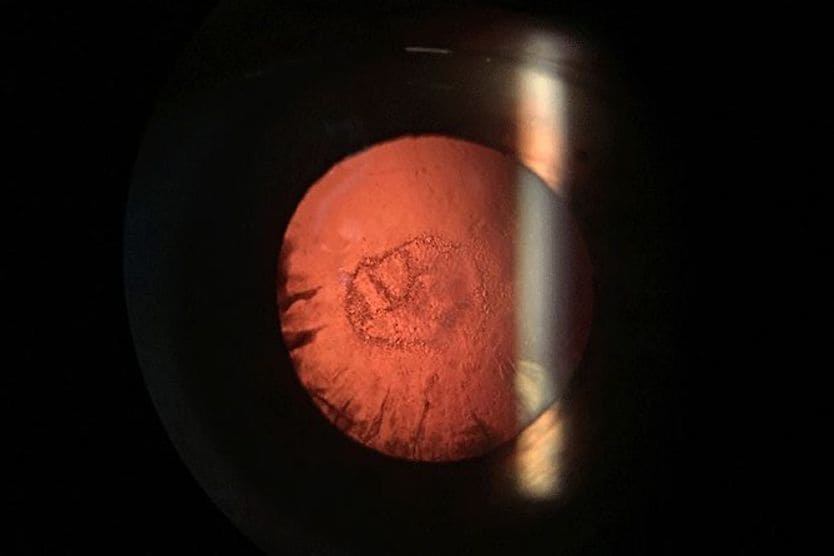
The natural lens inside the eye is a clear, flexible object located right behind the pupil. A cataract is a cloudy or opaque spot that forms on the lens. It changes how the lens looks, and it interferes with light that passes through it. It can also change the way a child's brain processes the light.
A childhood cataract can cause one or more symptoms:
- Problems recognizing people or things
- Problems following moving things with their eyes
- Sensitivity to bright lights
- Crossed eyes (strabismus)
- Jittery, uncontrolled eye movements (nystagmus)
- Lazy eye (amblyopia)
- In some cases, a milky white pupil
Sometimes, a large cataract can be visible in photographs taken with a flash. In these cases, one pupil may appear white, while the other pupil has a normal red light reflex.
Types of childhood cataracts
A pediatric cataract can develop during two different time frames:
- Infantile onset – Diagnosed as a newborn or infant.
- Juvenile onset – Diagnosed after infancy, sometime during childhood.
The cataract can be a:
- Congenital cataract – The cataract is there when the baby is born. Many (but not all) infantile cataracts are congenital. Some juvenile cataracts are also congenital.
- Acquired cataract – The cataract is caused by an illness, medical condition or injury. Many (but not all) juvenile cataracts are acquired. Some infantile cataracts are acquired, too.
There are many specific types of childhood cataracts. They can affect different parts of the lens.
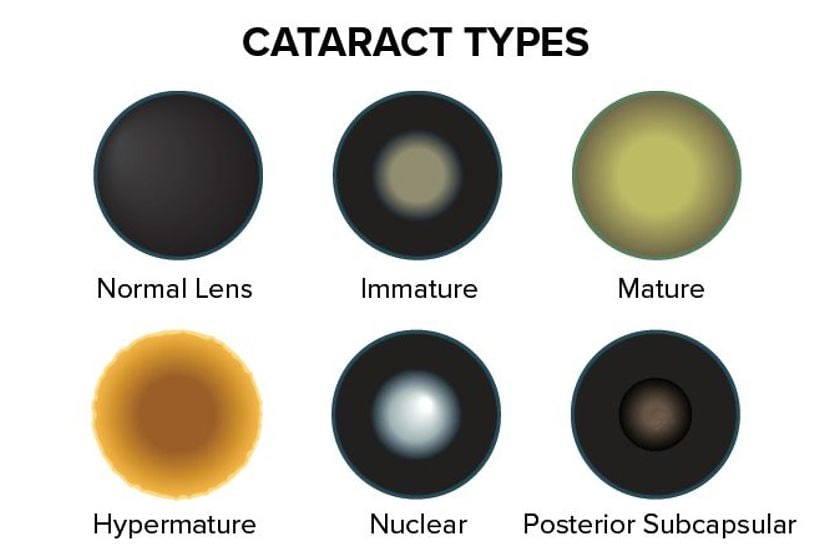
Some of the more common types are:
- Lamellar – Clouding between the cortex (outer layer) and the nucleus (the inner "core") of the lens.
- Nuclear – Clouding in the lens nucleus.
- Posterior subcapsular – Clouding along the back surface of the lens.
- Anterior polar – A dense opaque spot on the front center of the lens; often attached to the front of the lens capsule.
- Posterior polar – A dense opaque spot on the back center of the lens; often attached to the back of the lens capsule.
- Traumatic – Cloudiness that forms after an eye injury.
Some pediatric cataracts are caused by a condition called persistent fetal vasculature, or PFV for short. If it isn't treated, PFV can put a child at a much higher risk of developing a serious eye problem later in life.
Diagnosis
Many infant cataracts are found during the doctor's exam at birth. A pediatrician might also diagnose cataracts during a well-baby checkup.
Others might be diagnosed during a vision screening or after a traumatic eye injury.
An eye doctor can diagnose childhood cataracts during a comprehensive eye exam. Many parents choose to visit a pediatric ophthalmologist who specializes in children's eye health.
During the eye exam, the doctor will use certain tools and tests to help them get a better look inside a child's eyes.
SEE ALSO: Baby’s first eye exam: What to expect
Treatment
The treatment of a pediatric cataract depends on its type, size and severity.
In many cases, children need to have surgery to remove a cataract. But not every cataract requires surgery.
Some can be managed with regular observation by an eye doctor. But they may still need to have surgery in the future.
Surgery and recovery
If a child needs to have surgery, the doctor will remove the affected lens and replace it with an intraocular lens, or IOL. An IOL is a clear, artificial version of the natural lens that helps a child see clearly again.
Childhood cataract surgery is generally safe and effective. However, pediatric cataract surgery carries a higher long-term complication profile than adult cataract surgery, including secondary glaucoma (which can develop years to decades later), visual axis opacification often requiring additional procedures, and the need for ongoing amblyopia therapy and refractive correction.
Risks include:
- Infection
- Glaucoma
- Detached retina
- The need for more surgeries
If there are cataracts in both eyes, the doctor will usually only operate on one eye at a time. That helps lower the risk of complications happening in both eyes.
After surgery, a child will need to use medicated eye drops and wear a shield over the affected eye for a while.
Many children will still need to wear prescription glasses or contact lenses after surgery. Some children will still have reduced vision in that eye.
A child with a lazy eye may also need to wear a patch over the stronger eye to help vision in the weaker eye.
Over time, parents will typically need to schedule regular eye doctor check-ups to monitor their child's eyes and vision.
Outlook
Timely cataract surgery (when medically necessary) can have positive outcomes. However, the outcome can vary from child to child, depending on a few different factors. An eye doctor will discuss these with the parents. If surgery is recommended, it should not be delayed. Timely surgery could help to prevent long-term vision loss.
Parents will need to schedule routine follow-ups to monitor their child's eye health and make sure their vision prescription is up to date.
When to see an eye doctor
Schedule an eye exam with an optometrist or pediatric ophthalmologist any time you suspect something is wrong with your child's eyes or eyesight.
Young children typically aren't as good at noticing when something is wrong as adults are. Even if everything seems normal, comprehensive eye exams could reveal important problems that need to be corrected.
Following this schedule for your child’s exams is recommended:
- One exam between ages 6 and 12 months
- At least one exam between ages 3 and 5 years
- One exam before first grade, then one exam per year until and throughout adulthood
An eye doctor may recommend scheduling exams more often if a child is at a higher risk of developing an eye problem.
READ MORE: Everything you need to know about your baby’s vision