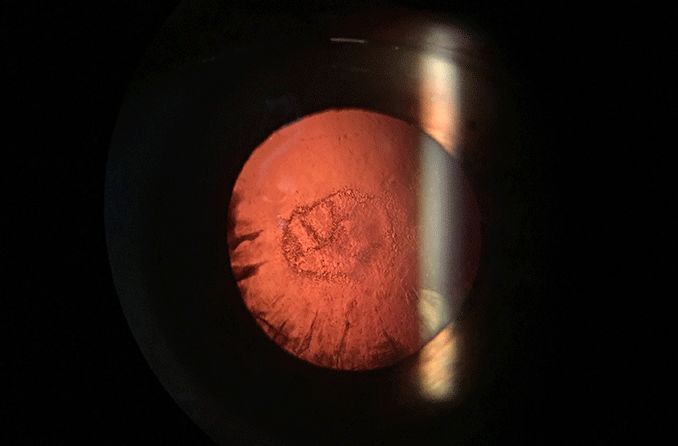
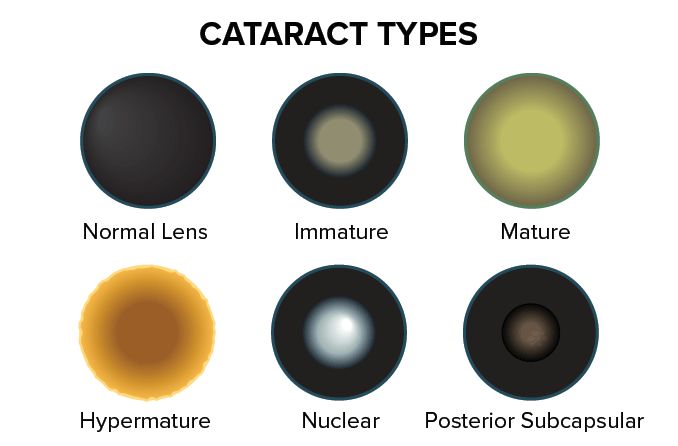
What is a posterior subcapsular cataract?
Posterior subcapsular cataract (PSC) is a fast-growing opacity in the rear of the natural lens. This cataract is most common in people who use steroids long-term or have diabetes. PSC symptoms can develop over a few months. They can include light sensitivity, glare and decreased vision, especially at near.
A wide variety of medical conditions and risk factors can contribute to the formation of PSC. Due to this, PSC occurs in younger people more often than other types of cataracts.
PSC is the least prevalent of the three common types of cataracts. According to the Beaver Dam Eye Study, the incidence of PSC was about 3% in one eye. The incidence of cortical cataracts was about 8%, and nuclear cataracts was about 13%.
What causes posterior subcapsular cataracts?
PSC is caused by the buildup and clumping of protein fibers in the back of the lens, just in front of the posterior lens capsule. This clumping of proteins disrupts the transparency of the lens fibers, resulting in opacities in the lens. Quality of vision decreases because light rays are scattered, and fewer light rays reach the retina.
The process of lens protein buildup and clumping occurs naturally with aging. Other factors that can contribute to the development of PSC include:
- Long-term use of corticosteroids
- Medical conditions such as diabetes
- Ocular conditions such as inflammation from uveitis, retinitis pigmentosa, trauma and radiation exposure
- High myopia and pathologic myopia
- Smoking
- Certain skin disorders such as atopic dermatitis
- High amounts of exposure to UV radiation
How are posterior subcapsular cataracts classified?
Your doctor may tell you that you have a 1+ to 3+ PSC. This is a classification system that grades the cataract according to size, in millimeters:
- PSC 1+ – 1 mm to 2 mm
- PSC 2+ – 2 mm to 3 mm
- PSC 3+ – 3+ mm
PSC is a fast-growing cataract that can progress fairly quickly from PSC 1+ to PSC 3+. Your eye doctor will monitor the PSC and recommend the appropriate management, including surgery.
What are the symptoms of posterior subcapsular cataracts?
A PSC limits and scatters the light that reaches the retina, causing visual disturbances. Symptoms from PSC may develop quickly as the PSC grows, and can include:
- Decreased vision, with near vision worse than distance vision
- Sensitivity to bright lights
- Glare, especially from headlights when driving at night
- Halos around lights
What is the treatment for posterior subcapsular cataract?
The treatment for a posterior subcapsular cataract is cataract surgery. It is a common surgery and is considered one of the safest procedures performed in the world. The surgeon removes the cloudy natural lens and replaces it with a clear artificial lens called an intraocular lens (IOL). The surgery takes about 15 minutes, and you will usually be able to go home that day.
What can I do to prevent posterior subcapsular cataract?
Your doctor can help you manage conditions such as diabetes or ocular inflammation and trauma that can be risk factors for developing a PSC.
Some additional steps that you could take to decrease your chances of developing a PSC are:
- Increase vitamin C, D and E intake with supplements and a diet of fruits and vegetables.
- Decrease alcohol consumption.
- Minimize UV exposure.
- Avoid obesity by maintaining a healthy weight.
- Stop smoking.
What does it mean if I have been told I have a posterior subcapsular cataract?
A posterior subcapsular cataract usually progresses quickly. If you are experiencing difficulty with blurry vision and glare while driving, you should talk to your eye doctor. They can help you to make an informed decision about your cataract surgery options.