What is a snowflake cataract?
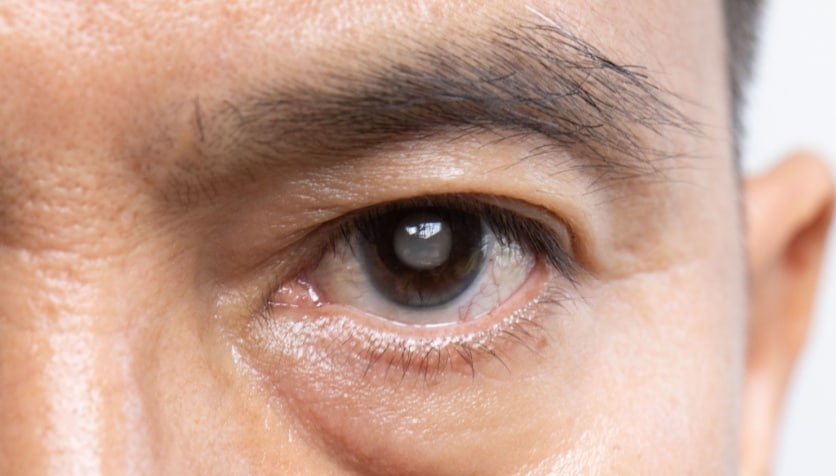
A snowflake cataract is a rare type of cataract often associated with diabetes. It can develop in patients with uncontrolled Type 1 diabetes. A snowflake cataract looks like white specks that resemble snowflakes. These specks are called opacities and can eventually cover the entire eye lens.
What causes a snowflake cataract?

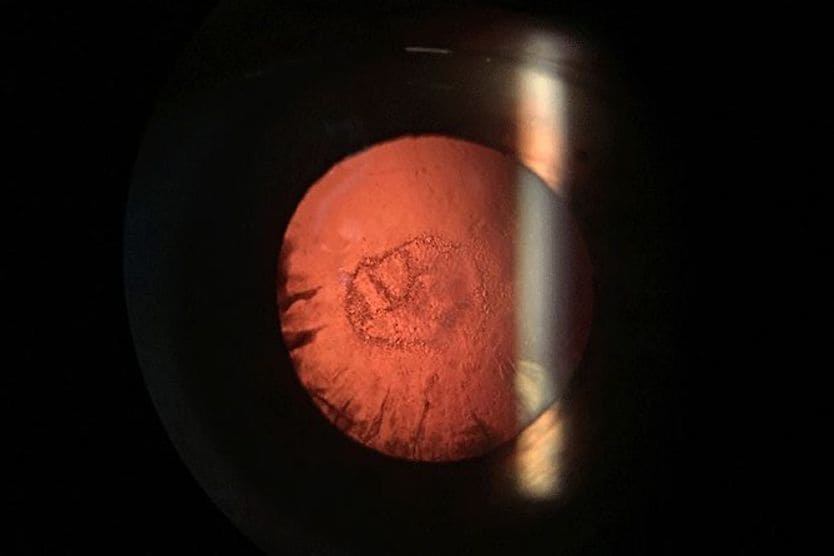
Diabetic "snowflake" cataract [Image credit: Permission granted by © 2022 American Academy Ophthalmology]
A cataract forms when the lens of the eye becomes clouded. Cataracts can be caused by many diseases or circumstances. There are also many different types of cataracts. A snowflake cataract in particular is a rare type of cataract that is connected to diabetes.
Cataracts can be common in diabetics with uncontrolled blood sugar. While snowflake cataracts are rare, many instances of this condition have been associated with uncontrolled juvenile diabetes. Snowflake cataracts can also form in people without diabetes, but this is uncommon.
When snowflake cataracts develop in people without Type 1 diabetes, the cause is unknown.
READ MORE: What are Christmas tree cataracts?
Relationship between diabetes and cataracts
There is a known connection between diabetes and a number of eye health concerns. When diabetes is not controlled properly, it can cause instability throughout the body. This includes the eyes.
Some eye health issues that can develop in diabetics include:
Diabetic retinopathy: This condition can cause the blood vessels in the retina to weaken or leak.
Diabetic macular edema: Diabetes can cause the macula to swell. This can cause partial vision loss or even blindness.
Glaucoma: Glaucoma is a category of eye diseases that damage the optic nerve. Without treatment, glaucoma can cause blindness
Cataracts: Cataracts affect the crystalline lens of the eye, making it cloudy.
There are many reasons uncontrolled diabetes can wreak havoc on your eye health. Blood sugar, which is what food is converted into, travels through the bloodstream. The high levels of sugar in the blood cause damage to many tissues in the body over time.
This encourages the pancreas to produce insulin, which helps blood sugar penetrate cells. This process allows the energy from blood sugar to be used all throughout the body.
Insulin is a hormone you can’t live without, and having diabetes or insulin resistance requires daily maintenance. When diabetes is not cared for properly, it affects the blood vessels in the retina and could make them leak. Leaking blood vessels can have complications that could become dire. Leaking blood vessels can also cause the lens of the eye to distort in shape, which leads to cataracts.
What are the symptoms of diabetic cataracts?
When a cataract first develops, you might not notice any symptoms. Signs of cataracts tend to form as the condition progresses over time.
As snowflake cataracts increase in number and cover more of the eye lens, you may start to notice:
Blurry or cloudy vision
Double vision
Changes in visual acuity
Poor night vision
Colors appearing dull or faded
Increased sensitivity to light (natural sunlight or artificial lights)
If a cataract is not treated or gets worse, this can lead to total vision loss. It’s important to schedule an eye exam with an ophthalmologist if you start to notice any of these symptoms.
Sudden changes in your sight should be identified and treated as soon as possible.
How are snowflake cataracts treated?
The goal for patients with diabetes is to prevent cataracts from developing. This is possible when blood sugar and insulin production are properly managed. However, it’s understood that prevention is not always an option.
When you start to notice cataract symptoms, or if a cataract is detected during an eye exam, immediate treatment might be necessary.
Treatment of cataracts varies greatly by the severity of the condition and the type of cataract. Snowflake cataracts are more prevalent among individuals with juvenile (Type 1)diabetes. This means that some of the people diagnosed with this condition could be children.
There are potential dangers associated with developing cataracts in childhood. If a cataract in a child goes untreated, it could potentially lead to vision loss.
Adults can also develop snowflake cataracts.
Some of the ways to treat cataracts include:
Making lifestyle changes, like using brighter lights or magnifying glasses to see more clearly
Updating your eyewear prescription to improve your vision
Surgery with a laser or other traditional techniques
If your cataract is in an earlier stage, it’s possible to slow the progression of the issue and manage it. But ultimately, the only way to completely remove a cataract is with surgery.
SEE RELATED: Cataract surgery
What does a snowflake cataract look like?
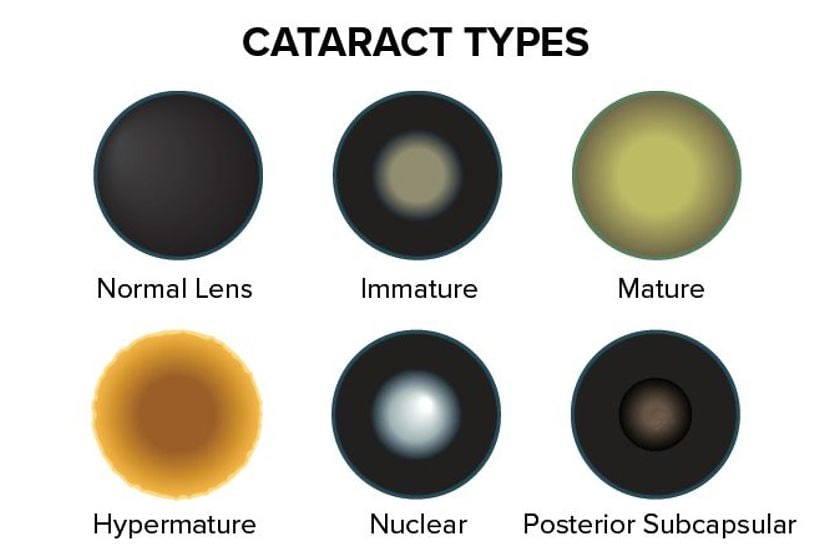
A typical cataract is not visible until it is considered “mature.” By the time this happens, a cataract takes on a cloudy appearance that covers a good portion of the natural, crystalline lens of the eye.
Snowflake cataracts, however, are characterized by their snowflake-like appearance. These cataracts form as smaller opacities on the lens of the eye that are white-gray in color. As these small opacities grow over time, they can cover more of the surface of the lens.
Are snowflake cataracts inherited or congenital?
Cataracts can develop with age or be congenital. But the development of snowflake cataracts is specifically associated with diabetes, particularly Type 1 diabetes. There does not seem to be many — if any — instances of snowflake cataracts occurring at birth.
Note : One congenital eye disease that shares a similar name to snowflake cataracts is snowflake vitreoretinal degeneration. But this is a retinal disease that shares no correlation with diabetes in patients.
When should I get medical help?
Any time you notice sudden changes in your vision, it’s important to seek out a professional. Conditions like cataracts can be hard to identify on your own. This is especially true for more rare versions of the condition.
The first step to having better eye health is making sure you see an eye doctor at least once a year. Diabetics in particular are at higher risk of developing certain eye health conditions. These include snowflake cataracts, diabetic retinopathy and a number of other diseases.
Being consistent with your routine eye exams allows trained ophthalmologists and optometrists to look for the early signs of eye health disorders. Early detection can delay the need for corrective surgery and make daily management more effective.
READ NEXT: What is a cortical cataract?