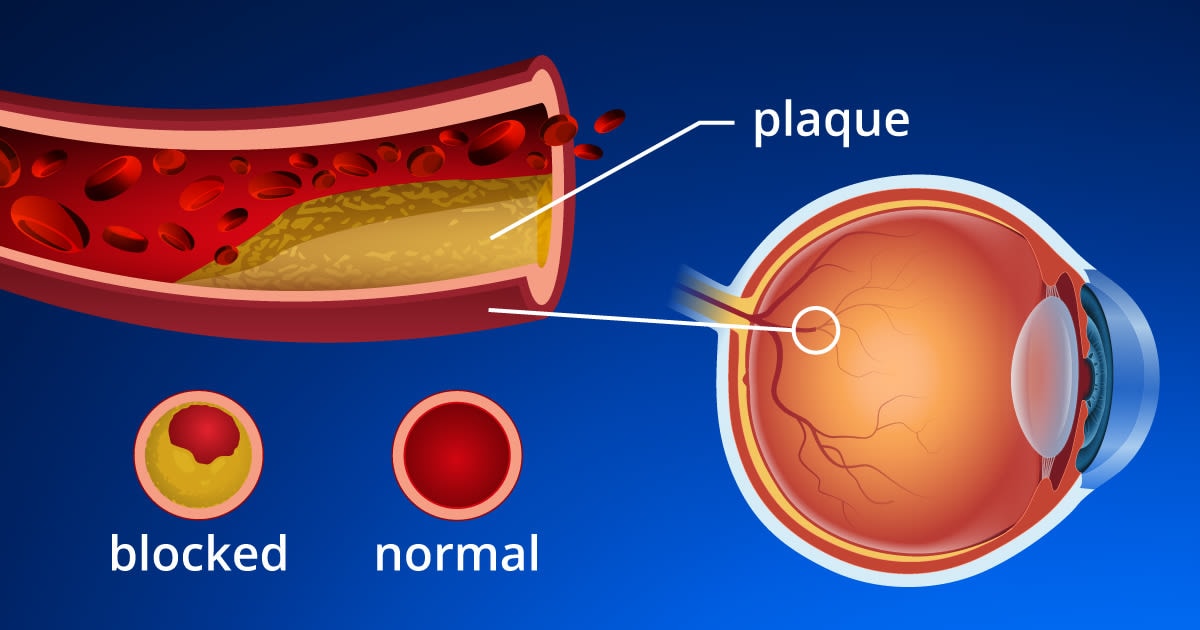
If your vision goes dark for a few minutes to a half-hour and then recovers, then you’re probably experiencing amaurosis fugax. People often suffer strokes within a few months after amaurosis fugax, so you must see a doctor as soon as possible if this happens to you.
A long list of problems can bring on amaurosis fugax. Usually, it’s due to an occlusion, or blockage, of the arteries carrying blood to the retina. Blindness that comes and goes in minutes can be alarming. If it happens to you, a crop of questions may arise:
- What exactly does amaurosis fugax mean?
- What are the main symptoms and what do they feel like?
- Which medical conditions cause amaurosis fugax?
- How do doctors diagnose amaurosis fugax?
- What are the most likely treatments?
- Can amaurosis fugax be prevented?
Let’s dive in and find the answers to these questions.
What is amaurosis fugax?
Amaurosis fugax, pronounced “am-au-ROE-sis FYU-gaks,” comes from the Greek and Latin terms for “darkening” and “fleeting.” Thus, amaurosis is common medical terminology for vision loss, while fugax means temporary.
Vision loss that lasts from 30 minutes to several hours is no longer considered temporary (transient). A short outbreak of blindness is quite different from a long one. Amaurosis fugax gives doctors a label to identify the shorter time span.
SEE RELATED: Sudden blurry vision
Amaurosis fugax symptoms
People with amaurosis fugax often say their vision goes dark like a window shade being pulled down. Amaurosis fugax can happen in one eye or both, lasting up to 30 minutes before vision returns. You might also feel a headache and neck pain.
Causes of amaurosis fugax
In the eyeball, arteries carry oxygen, fuel and vital nutrients to the retina. Light-sensitive nerves in the retina capture visual signals that travel over the optic nerve to the brain. The visual center of the brain translates these signals into eyesight.
The retina needs blood flow to do its job. Some diseases or conditions block blood flow in the optic arteries (or slow it down). Amaurosis fugax happens when this blockage or slowdown lasts up to 30 minutes and then goes away.
These are the most likely causes of amaurosis fugax:
- Plaque in the arteries - As people age, cholesterol, fat and other substances harden into plaque, which builds up in the linings of their arteries. A bit of plaque may break loose and become lodged in an artery of the eyeball for a few minutes, causing temporary vision loss. The carotid artery in the neck often releases plaque that sets off amaurosis fugax.
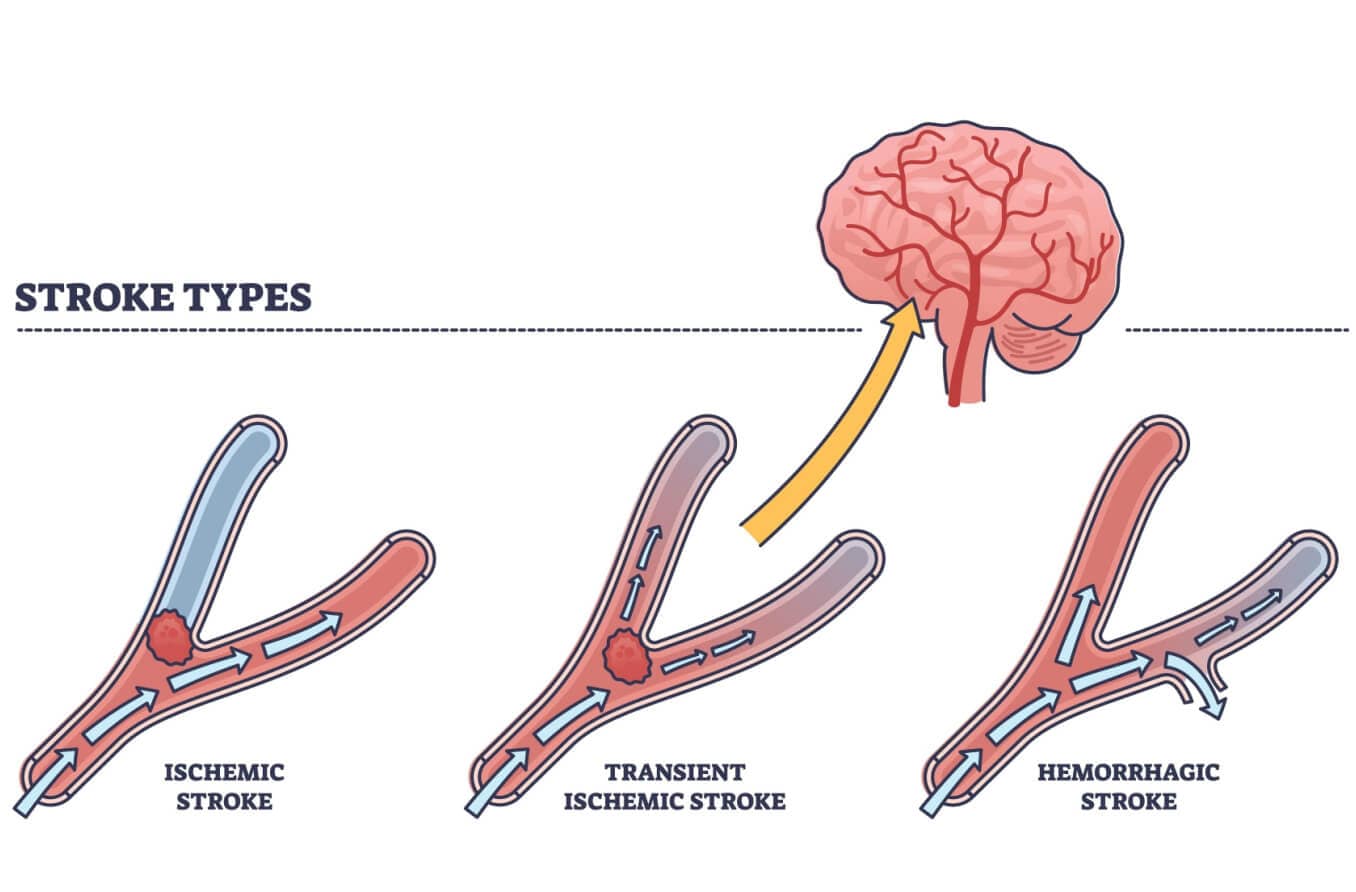
- Mini-strokes - A stroke happens when a buildup of plaque ruptures, releasing a blood clot that blocks an artery in the brain. This causes paralysis, loss of speech and other serious disabilities. A mini-stroke, often called a temporary ischemic attack (TIA), is a small clot that causes temporary stroke symptoms and then goes away. Amaurosis fugax happens when one of these clots gets stuck in an eye artery for a short time. A small clot is a warning sign of a larger clot that can cause a stroke. As a result, doctors advise taking amaurosis fugax seriously: If you experience sudden, even if short-term, vision loss, seek medical attention as soon as possible. [Read our article on how a stroke can change your vision.]
Amaurosis fugax also happens in response to:
- Optic nerve neuritis and other eye conditions in which blood flow is important
- Migraine headaches
- Brain tumors
- Head injuries
- Multiple sclerosis
- Sudden exposure to bright lights
These are some of the prime risk factors for amaurosis fugax:
- Aging
- Alcohol and cocaine abuse
- Diabetes
- High blood pressure and excessive cholesterol
- Smoking, especially more than a pack a day
- Family history of stroke
Because so many variables contribute to amaurosis fugax, you need to see a doctor to figure out what’s going on.
Amaurosis fugax: What’s the prognosis and diagnosis?
The prognosis for amaurosis fugax can be positive if you act quickly. Ignoring it, however, could bring serious problems, including permanent vision loss. And without immediate attention, you could be missing alarm bells warning of a future stroke.
These are the main ways that doctors diagnose amaurosis fugax:
- Eye exams that scan for signs of blockage to the retina.
- A medical history survey looking for risk factors like smoking and cocaine use.
- Assessments for diabetes, high blood pressure and cardiac disease.
- Listening (with a stethoscope) for signs of trouble in the heart and the carotid artery. An ultrasound will provide a more precise reading.
- Blood tests looking for evidence of cardiovascular disease.
- Magnetic resonance imaging (MRI) and computed tomography (CT) scans to assess the health of the carotid and other arteries.
With data from these sources in hand, doctors can create a plan for what to do next.
Treatment of amaurosis fugax
Because amaurosis fugax comes and goes so quickly, doctors usually cannot treat it while it’s happening. Instead, they treat the underlying causes.
That can be as simple as monitoring your situation or prescribing blood-thinning medications.
Doctors may also encourage you to:
- Exercise more frequently
- Avoid fatty foods
- Get your blood pressure under control
- Improve your cholesterol test results
- Halt risky activities like smoking, drinking alcohol and taking drugs
If tests discover blockage in your carotid artery, surgery can improve blood flow. Inserting a stent might be another option.
Your treatment plan will vary depending on your age, your health and the risk factors involved with each treatment.
How to prevent amaurosis fugax
Keeping your brain healthy is a great way to reduce the risk of stroke and, by extension, the mini-strokes that cause amaurosis fugax. The American Stroke Association recommends seven key activities to promote brain health.
- Manage blood pressure
- Control cholesterol
- Reduce blood sugar
- Get active
- Eat better
- Lose weight
- Stop smoking
It’s also imperative to stay on top of conditions like diabetes, multiple sclerosis and irregular heart rates, which may have an impact on amaurosis fugax.
SEE RELATED: How eyes can reveal potentially serious heart problems
When should I see the doctor?
Call your doctor immediately if you experience sudden vision loss. There’s no time to lose because treating a stroke quickly is key to preventing permanent damage.
Of course, it may not be a stroke, given all the possibilities outlined above. But you should treat amaurosis fugax as a serious condition — just in case.
RELATED READING: Fluctuating vision: Is it normal?