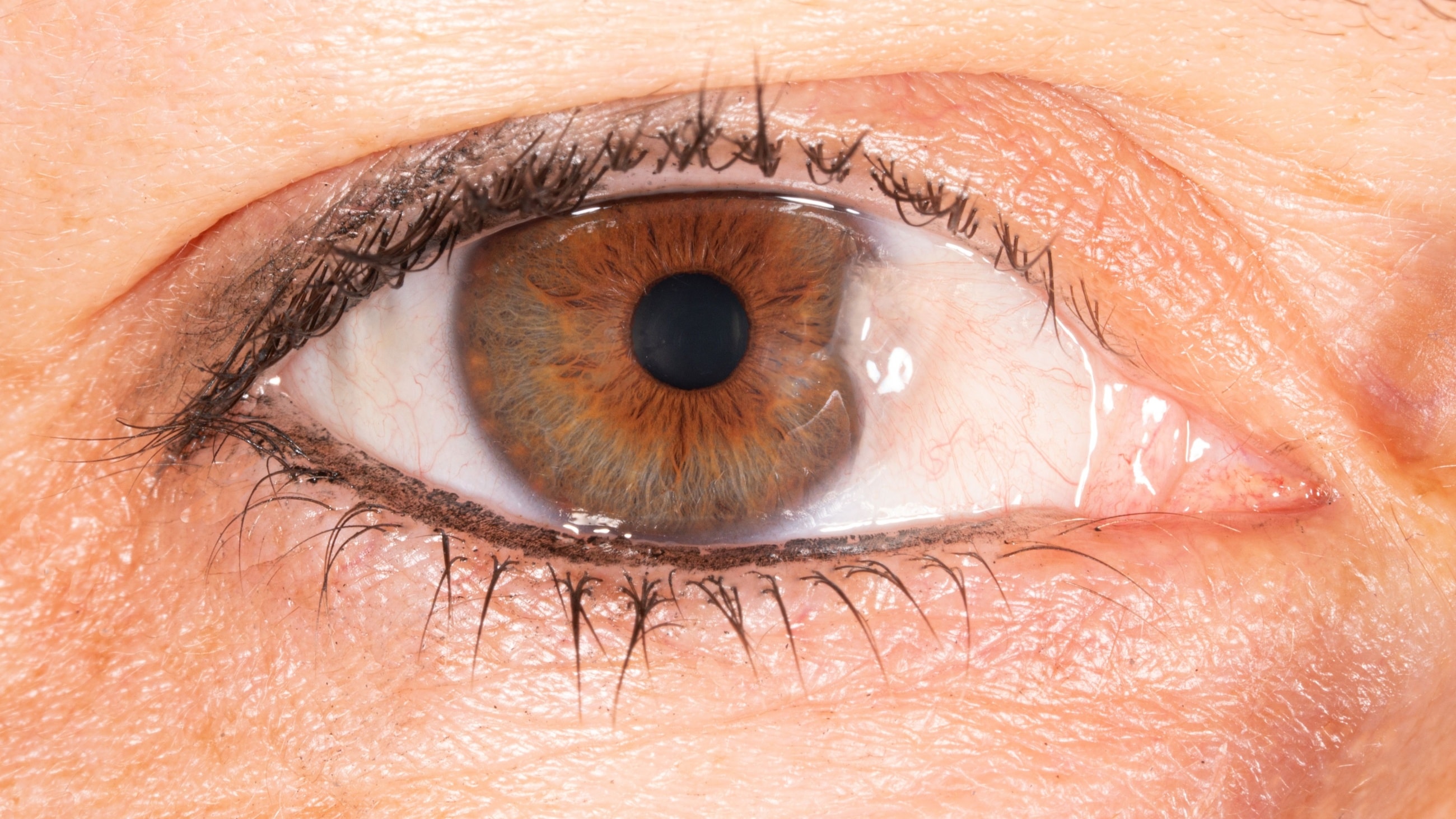
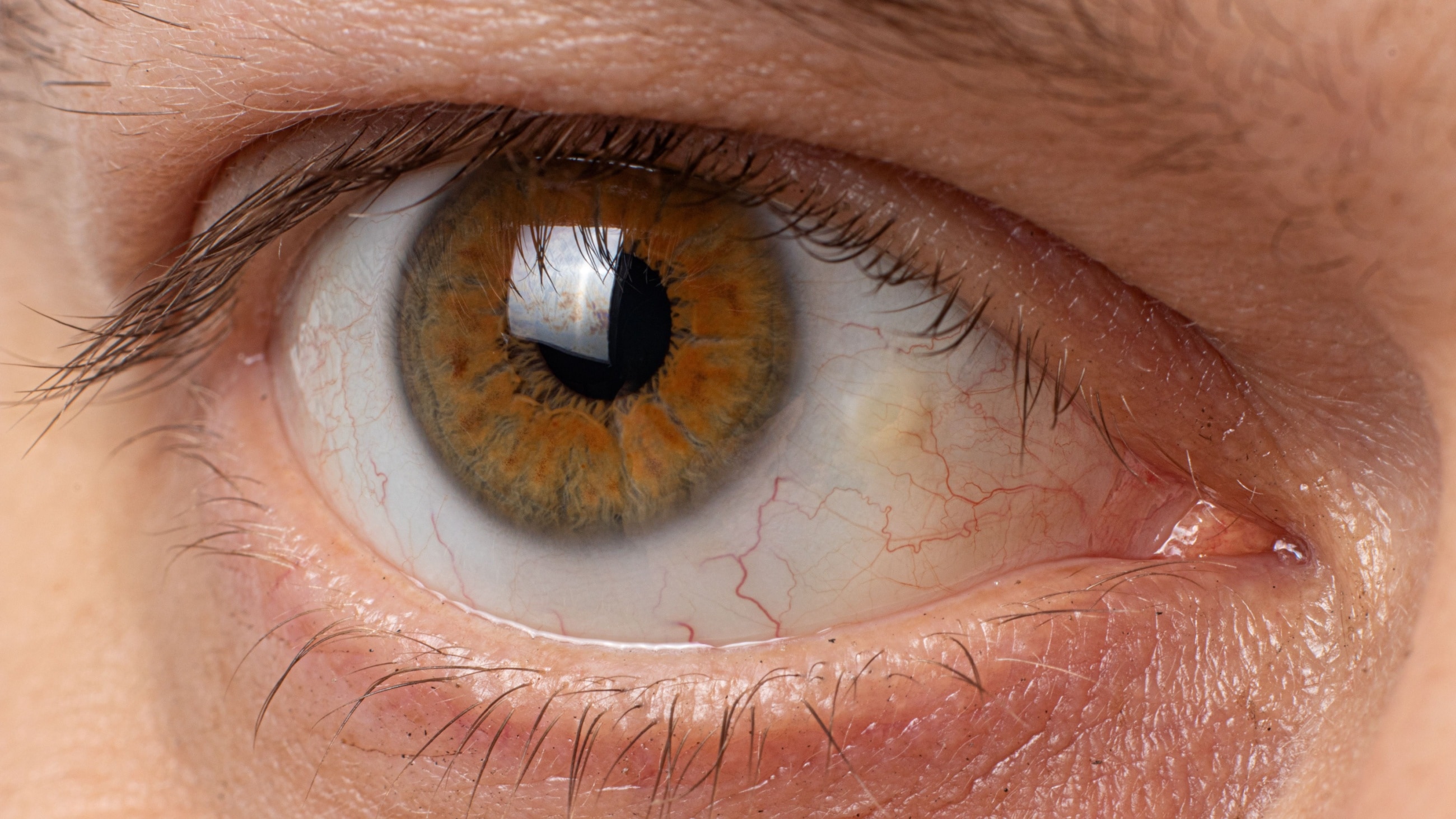
Ocular melanoma, or eye melanoma, is a cancer that develops in the eye’s melanocytes, which are the cells responsible for producing melanin (pigment). It is a cancerous (malignant)tumor that usually develops in the middle layer of the eye, called the uvea.
Since most cases of ocular melanoma begin inside the eye and usually cause few to no early symptoms, the condition is difficult to detect without comprehensive, routine eye exams.
What is ocular melanoma?
Ocular melanoma is a condition in which melanocytes in the eye become cancerous. Melanocytes in the uvea are similar to those that produce the pigment that determines eye, skin, and hair color.
Melanoma is often associated with skin cancer, the most common cancer in the U.S. and worldwide. Eye melanoma accounts for about 5% of all melanomas. While skin cancer occurs much more frequently than ocular melanoma, the same type of cells that are affected by melanoma in the skin can become cancerous in the eyes.
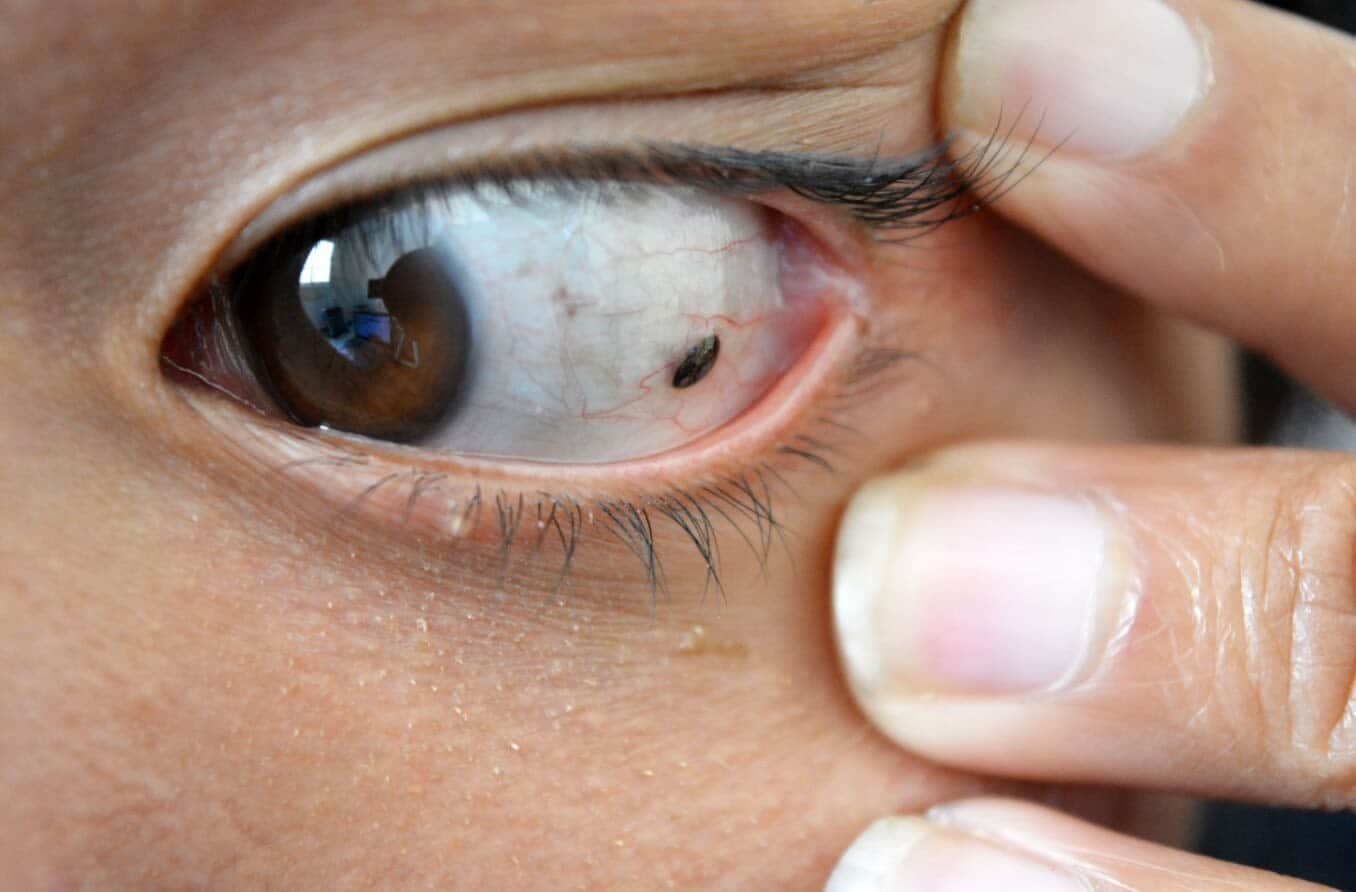
Melanoma can develop in various parts of the eye, just as it can on different areas of the skin. While skin cancer is directly related to sun damage, there is not a clear-cut association with all types of ocular melanoma. There is some evidence that melanoma located on the conjunctiva (the clear membrane that covers the whites of your eye)may be associated with prolonged exposure to ultraviolet (UV)radiation.
There are approximately five cases of ocular melanoma for every one million people under 50 years old — instances jump to 21 per million after age 50.
While ocular melanoma is very rare, it’s the most common primary eye cancer in adults. The term “primary” is used to describe a cancer that originated in that area — in this case, the eye — and did not spread from somewhere else in the body.
Parts of the eye affected by ocular melanoma
There are three layers in the eye. The sclera (the whites of the eyes)is the outermost layer. The retina (the light-sensitive tissue at the back of the eye)is the innermost layer. The middle layer located between the retina and sclera is the uvea.
Cells in the uveal layer, also called the uveal tract, are where ocular melanoma develops most often. This is known as uveal melanoma. The uveal tract has three parts that make up different subtypes of uveal melanoma:

Iris — The colored part in the front of the eye. If this area is affected, the condition is known as iris melanoma.
Ciliary body — A structure in the front of the eye that produces a fluid called aqueous humor and includes the ciliary muscle. This muscle allows the eye to focus by adjusting the shape of the lens. It’s called ciliary body melanoma if this part is affected.
Choroid layer — A layer of connective tissue and blood vessels between the sclera and the retina. Having tumors in this area is called choroidal melanoma. Most uveal melanomas begin in the choroid layer.
Though it is very rare, melanoma can also develop on the eyelid, in the eye socket, or on the membrane that covers the front of the eye, the conjunctiva.
Metastatic ocular melanoma
Metastatic ocular melanoma describes melanoma that has spread (metastasized)to other areas of the body — usually the liver. What triggers the cancer to spread is still unknown, though a number of risk factors have been linked.
Metastasis happens in approximately half of all ocular melanoma cases and is often fatal.
SEE RELATED: Eye cancer
Causes
Eye melanoma is a result of abnormalities or mutations that form in DNA, the carrier of the body’s genetic code. When healthy melanocytes (pigment cells)in the eye develop an error in their DNA that affects their ability to regulate their growth, they grow and multiply uncontrollably.
Rather than dying off like they normally would, the mutated cells continue to live and accumulate in the eye, resulting in eye melanoma.
The root cause — the trigger for this cancer — is still not clearly understood. However, several factors may raise a person’s risk of developing eye melanoma.
Ocular melanoma risk factors
You are more likely to develop ocular melanoma if you:
Have fair skin.
Have light-colored eyes.
Are over 50 years old.
Have a strong family history of systemic and ocular cancers.
Have certain inherited skin conditions like dysplastic nevus syndrome, which is characterized by having abnormal moles.
Have ocular melanocytosis, which describes increased uvea pigmentation.
Are prone to developing moles or freckles.
Have one or more freckles in the eye (iris nevi).
Whether you fall under the high-risk category or not, it is important to wear sunglasses whenever the sun is out. Shielding your eyes from the sun’s harmful rays can lower your risk of developing several eye conditions.
SEE RELATED: UV and sunglasses: How to protect your eyes
Symptoms
It’s possible to have ocular melanoma with no signs or symptoms — these cases would only be detected with an eye exam. For this reason, it’s important to take note and see an eye doctor if you experience any of the following:
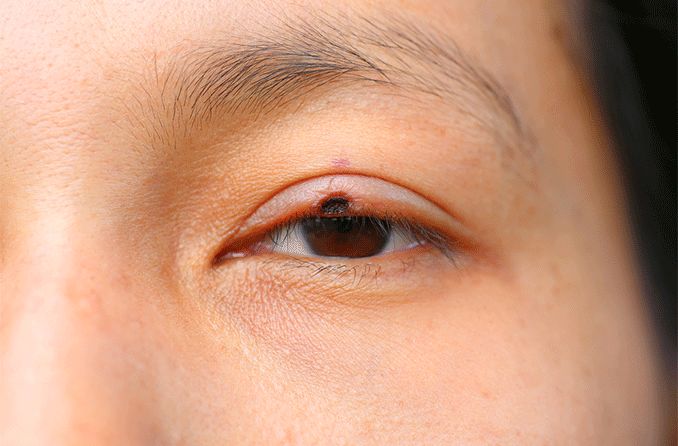
Appearance of a dark spot on the iris that may grow over time
Seeing eye floaters or flashes of light
Change in the shape of the pupil
Reduced peripheral vision in one eye
Poor or blurred vision in one eye
Pain in or around the eye (this occurrence is less common).
If you are experiencing any of these symptoms, it does not necessarily indicate ocular melanoma, but it is important to be evaluated by an eye doctor so they can determine the underlying cause.
As the melanoma grows, complications such as increased eye pressure (a risk factor for glaucoma)and vision loss may result.
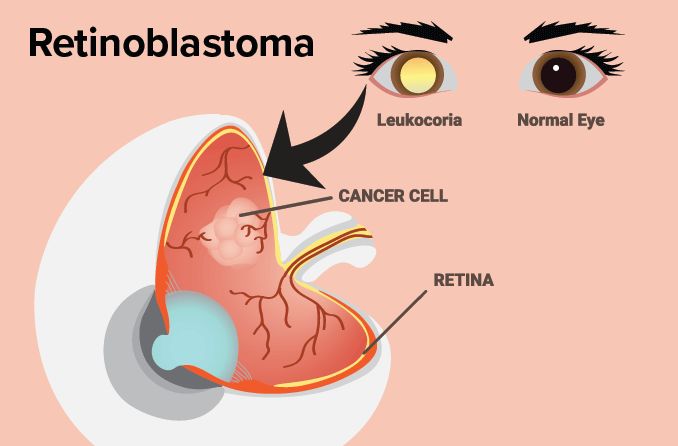
READ MORE: What is retinoblastoma?
How do you treat ocular melanoma
Treatment for ocular melanoma depends on its type, size, location, and the patient’s general health. For small melanomas that have shown no growth, your doctor may recommend monitoring the melanoma before proceeding with surgery or other treatment. If treatment is necessary, surgery or radiation may be recommended.
Surgery
Surgical procedures remove the melanoma and the affected parts of the eye. This is typically only done on melanomas that are still very small.
If vision has become affected, constant eye pain is present, or the melanoma poses additional health risks, enucleation, the removal of the entire eyeball, may be necessary.
After the eyeball is removed, an implant can be inserted into the eye socket and attached to the muscles that control the eye. Once the eye has healed from the procedure, a prosthetic eye painted to match the natural eye color is inserted.
Radiation
Melanomas may also be treated with radiation therapy. Radiation consists of using high-powered energy to destroy cancer cells. The most common form of radiation treatment is known as brachytherapy.
Brachytherapy, or plaque therapy, uses a radioactive plaque that is stitched into the eyewall on the eye’s outer surface. The plaque is left on the eye for several days so it can destroy the tumor.
Additional types of treatments also exist, which the cancer specialist may recommend depending on the type and stage of the melanoma.
Importance of routine eye exams
Ocular melanoma does not typically show symptoms until it has progressed. For this reason, having dilated, routine eye exams is critical.
If you are at higher risk for eye melanoma, annual eye exams make it possible to detect and treat ocular melanoma early. Additionally, it’s important to be mindful of any changes in your vision, persistent eye pain or changes in your eyes’ appearance.
READ MORE: Ocular Melanoma Awareness Month