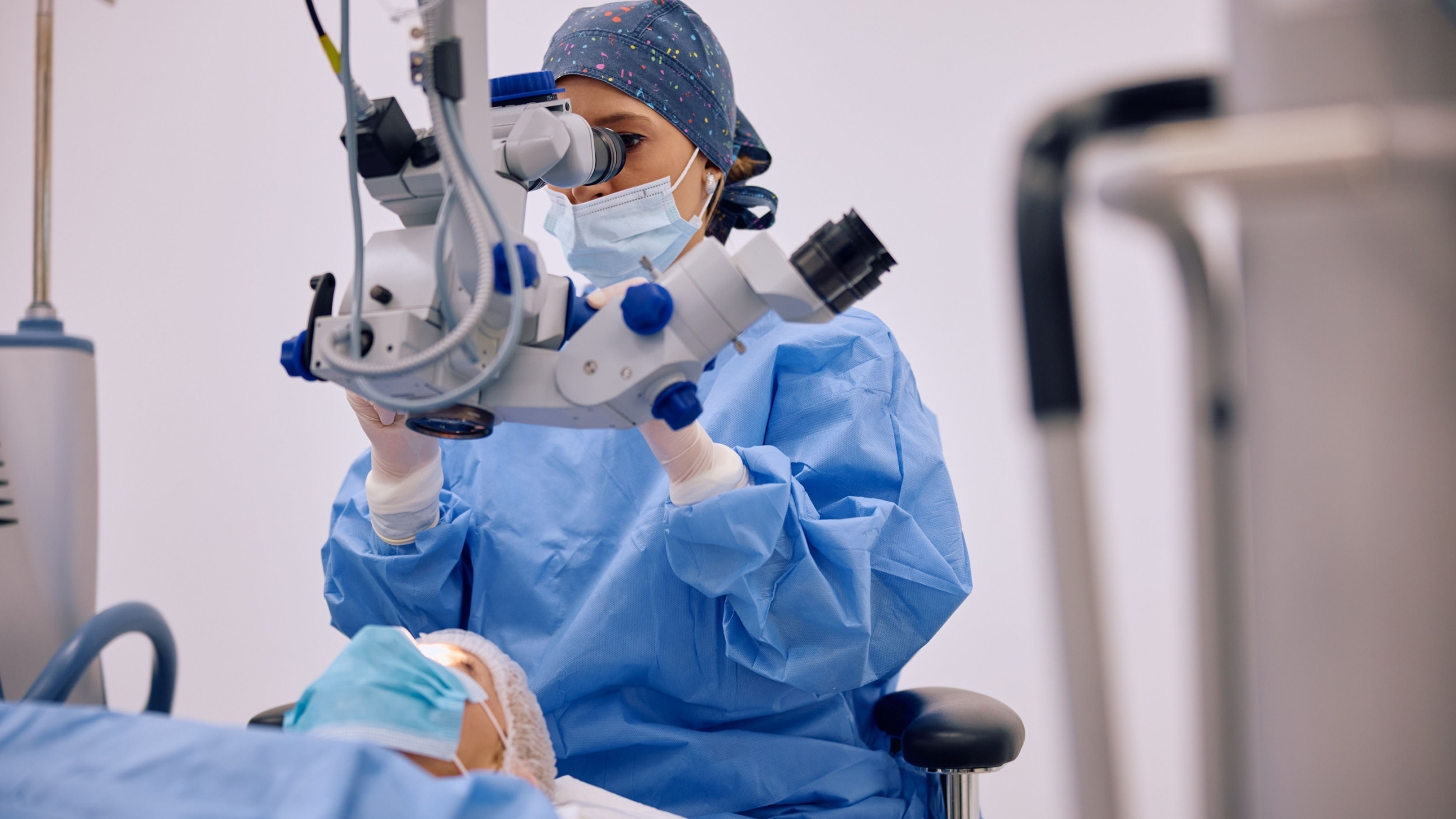
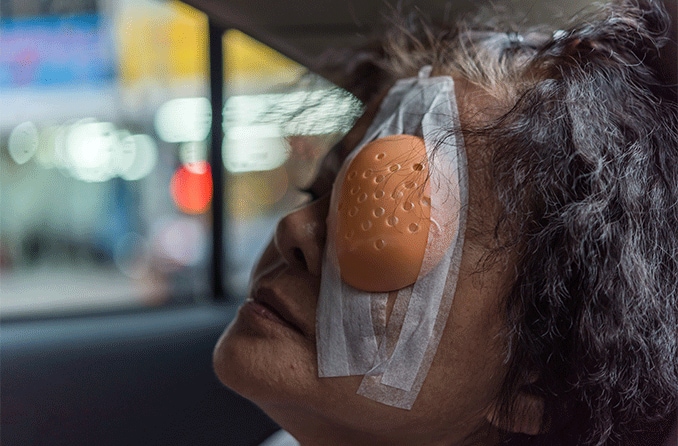
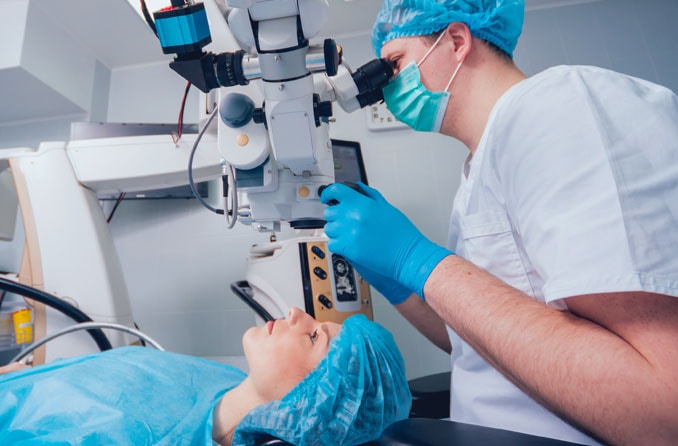
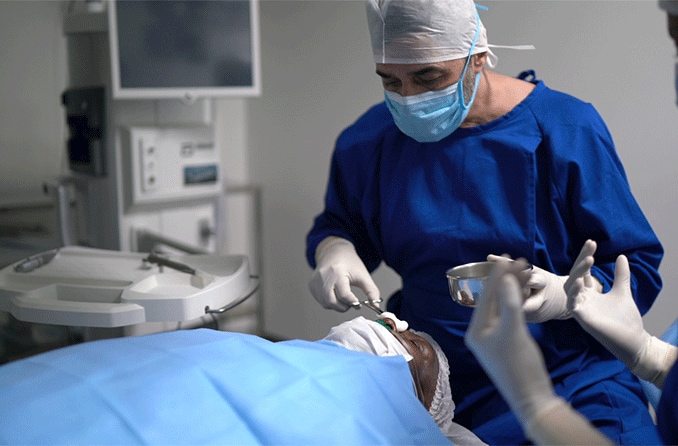
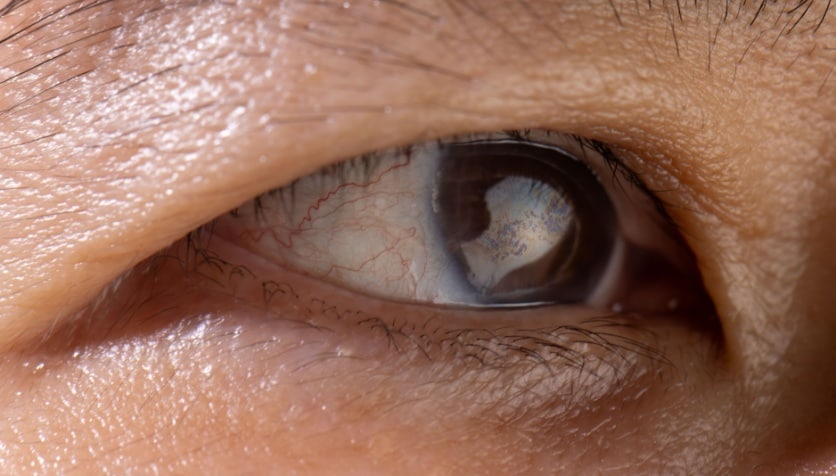
Does Medicare cover cataract surgery?
Yes, Medicare covers cataract surgery as long as your doctor says it's medically necessary. Medicare Part B (the medical insurance portion) covers some of the costs of surgery and a standard artificial lens that's inserted into your eye.
After you meet your yearly deductible, Medicare covers 80% of the surgery costs. You'll need to pay for the remaining 20% out of pocket.
The Part B deductible for 2026 is $283.
Here's how the different parts of Medicare can be used to cover your cataract surgery:
Part A
Medicare Part A covers inpatient (overnight) hospital stays.
Cataract surgery is rarely covered by Part A because it's an outpatient procedure (you go home the same day) with a typically low risk of serious complications.
Part B
Medicare Part B covers doctor visits and outpatient care.
Cataract surgery is covered by Part B.
Part B will also cover your appointments with your ophthalmologist — the doctor who performs your surgery. It also covers one pair of prescription glasses after your surgery.
Pre-surgery eye tests are only covered if they're medically necessary. Ask your eye doctor about any extra testing costs beforehand.
Medicare Advantage (Part C)
Medicare Advantage is the more common name for Medicare Part C. It's an optional alternative to Original Medicare (Part A and Part B) that can include extra coverage as part of a "bundle."
You could buy it through a private insurance company.
You need to be enrolled in Part A and B to join a Medicare Advantage plan. While Part B technically covers cataract surgery, your Medicare Advantage plan would pay for it instead. It should cover all the same services that Part B does.
However, specific details can vary from plan to plan, so it's recommended to contact your plan administrator to check your coverage.
Medicare doesn't include vision insurance, but you can customize a Medicare Advantage plan to include vision coverage. This can help pay for routine eye exams, eyeglasses and contact lenses.
Part D
Medicare Part D covers prescription drugs. It's optional, too.
Part D does not cover cataract surgery, but it could cover any prescription eye drops or medicine your eye doctor prescribes after the procedure.
These medications need to be on Medicare's list of approved drugs.
Medigap
Medigap is supplemental (extra) insurance you can buy to lower your medical costs more. It's also called Medicare Supplement Insurance.
You also buy Medigap plans through private insurance companies.
There are 10 standard Medigap plans: Plans A, B, C, D, F, G, K, L, M and N. Which plans you can enroll in depends on when you became eligible for Medicare.
Medigap is optional, but it could reduce your out-of-pocket (OOP) surgery costs if you choose to pay for it.
What does Medicare mean by "medically necessary"?
It means that the cataract(s) is causing visual symptoms that are affecting your daily life, including but not limited to driving at night, and surgery is the best way to help. An evaluation of visual acuity alone can neither rule in nor rule out the need for surgery.
If your eye doctor confirms this, your cataract surgery should be covered by Medicare. Always double-check with your doctor's office even if you think you're covered.
You need to meet certain requirements to have standard cataract surgery covered by Medicare:
- The cataract is causing blurry vision, glare problems or other symptoms that make it hard to do some of your everyday things (like driving or watching TV).
- Your vision is still too blurry with up-to-date prescription glasses or contact lenses.
- If you have another eye condition, the cataract is making your symptoms much worse or making it harder for your doctor to monitor the other eye condition.
- You had an eye exam, and your doctor agrees that surgery is the best option.
- You choose to have cataract surgery. You understand the benefits, risks and alternatives (if any are available).
READ MORE: Can you treat cataracts with eye drops?

How much does cataract surgery cost with Medicare?
In 2026, standard cataract surgery with Medicare costs an average of:
- $343 at a non-hospital surgical center
- $563 at a hospital outpatient center
A complex cataract surgery will cost a little more, on average:
- $377 at a non-hospital surgical center
- $597 at a hospital outpatient center
However, your costs can vary depending on your procedure and doctor appointments. The doctor's office will give you a price estimate before you approve surgery.
You'll also pay more if you haven't met your deductible yet this year.
In that case, you would pay 100% of the Part B deductible ($283) first, then 20% of anything over that amount. Medicare pays for the rest.
Sample cost breakdown
Here's an example of two different people who need the same standard cataract surgery. Their procedures cost $1,600 before Medicare.
Example #1
James has already met his $283 deductible for the year. He will pay for 20% of the surgery costs.
20% of $1,600 = $320
James will pay $320 out of pocket for his surgery.
Example #2
Unlike James, Jill hasn't spent any money on medical care this year. She will need to pay her deductible ($283) first, then 20% of the remaining costs.
$1,600 - $283 deductible = $1,317
20% of $1,317 = $263.40
$263.40 + $283 deductible = $546.40
Including the deductible, Jill will pay $546.40 out of pocket for her surgery.
What type of lens does Medicare cover for cataract surgery?
Medicare only covers "conventional" intraocular lenses (IOLs). Doctors call them monofocal IOLs. This type of lens usually only corrects your distance vision.
Other IOLs and procedures can help correct vision-related conditions like astigmatism and presbyopia, but Medicare usually doesn't cover them.
If you have to wear glasses or contacts to see close-up objects before surgery, you'll still need to wear them with a monofocal IOL.
Does Medicare cover surgery for secondary cataracts?
Yes, Medicare covers secondary cataract surgery too — as long as it's medically necessary.
The medical name for a secondary cataract is posterior capsular opacification, or PCO for short. It happens to a lot of people after cataract surgery.
PCO is when the lens capsule that holds the IOL develops a cloudy spot. It's treated with a simple procedure called YAG laser capsulotomy.
During the procedure, a doctor uses a special laser to create a tiny hole in the cloudy spot that lets light pass through. They won't need to replace the lens again.
How much does it cost with Medicare?
In 2026, the average standard YAG laser capsulotomy will cost you:
- $115 at a non-hospital surgical center
- $167 at a hospital outpatient center
Does Medicare pay for glasses after surgery?
Yes, Medicare Part B covers one standard set of prescription eyeglasses or contact lenses after cataract surgery. It will only cover glasses and contacts from companies enrolled in Medicare.
Medicare only covers standard eyeglass frames, so you will pay the entire cost of any optional upgrades you choose.
Your out-of-pocket cost will depend on which frames, lenses or contacts you choose.
Questions to ask your eye doctor before surgery
It can help to write down questions sometime before your consultation appointment.
If you already had your appointment, call your surgeon's office and ask to speak with someone in the billing department.
You might ask questions like:
- Do you accept Medicare?
- Does the surgery facility accept Medicare?
- How much can I expect to pay out of pocket?
- What is the specific Medicare code(s) for my surgery? (You can use this code with Medicare's price lookup tool)
- Will my surgery be performed in a non-hospital surgery center or a hospital?
- Will I go home the same day (outpatient), or will I stay in the hospital overnight (inpatient)?
- Will you prescribe any medications before or after surgery? If so, which drugs are they, and will my Medicare coverage help pay for them?
- Are there any other costs I should know about?
How to apply for a Medicare plan that covers cataract surgery
You need to have active Plan B coverage or your cataract surgery won't be covered by Medicare.
You also need to enroll in Plan B before you can buy optional plans through a private company, like Medicare Advantage or Medigap.
If you recently signed up for Social Security retirement or disability benefits, you may have automatically enrolled in Part B (and Part A). But your Part B coverage isn't active unless you're paying the premium every month.
In 2026, the monthly premium is $202.90. You'll pay more than that if:
- You reported an income above $109,000 on a 2024 individual tax return
- You reported an income above $218,000 on a 2024 joint tax return
If you aren't enrolled in Part B, you need to sign up before you schedule surgery. The Medicare website (Medicare.gov) has a short questionnaire that can guide you through the right steps.
What if I still have questions about Medicare?
You can call 1-800-MEDICARE or chat with an agent on Medicare.gov. Their representatives are available 24 hours a day, except on some federal holidays.
READ NEXT: What to expect during your cataract surgery recovery