Q: I was told RGP (rigid gas permeable contacts)will stop keratoconus from worsening. Is this true?
A: No, this old wives' tale is not true. When worn, the RGP lenses temporarily flatten the non-structural epithelium (skin) of the cornea. This creates the illusion of stopping the progression. The keratoconus continues to progress, and contacts must be updated to keep up with the worsening disease.
To say that RGP contact lenses somehow stop keratoconus from progressing is like saying that wearing a baseball hat stops a child's skull from growing. Because keratoconus is a progressive disease, there must be some medical intervention to stop it, such as corneal crosslinking. — Dr. Brian Boxer Wachler
Q: Intacs are referred to as prescription inserts. Does this mean that they will eliminate my need for contacts or glasses?
A: Good question. To start, we should clarify that Intacs are not like contact lenses. They are curved, clear plastic half-moon-shaped segments that are inserted under the surface of the cornea to reduce the steepness of the cornea by reshaping it.
They are referred to as "prescription inserts" because they are available by prescription only, meaning that they must be ordered and inserted by a trained surgeon. The Intacs themselves have no prescription and are not intended to provide vision correction.
In cases where patients have a very slight prescription, the need for glasses and/or contacts can be eliminated; however, we tell patients not to expect this as a result. What you can expect is a much easier time being fitted for glasses and contacts, and also possibly a wider variety of contact lens types to choose from. — Dr. Brian Boxer Wachler
Q: I've heard about corneal collagen crosslinking treatment. Will this improve my vision?
A: The primary goal of corneal cross-linking (CXL) is to strengthen and stabilize the cornea to prevent progression of keratoconus. In some cases, CXL may also improve corneal shape and reduce corneal astigmatism, and thereby improve uncorrected and best-corrected visual acuity. But there's no guarantee this additional benefit will occur.
If you’ve been told by your eye care provider that you have keratoconus, schedule a consultation with an eye doctor who performs corneal cross-linking to discuss the likely outcome of CXL in your particular case. — Dr. Gary Heiting
Q: Will I go blind from keratoconus?
A: Keratoconus does not typically lead to complete blindness. But the disease can degrade vision to a level where one will experience difficulty leading a normal life.
Corneal hydrops (extensive scarring) as well as contact lens intolerance can occur as the disease progresses. This can lead to legal blindness and will eventually lead to the need for a cornea transplant. — Dr. Brian Boxer Wachler
Q: If I have keratoconus treatment, will I not need to wear contacts or glasses?
A: If someone has very mild keratoconus, then it is possible that they may not require glasses or contact lenses after receiving keratoconus treatment. In the majority of cases, however, patients will benefit from some type of vision correction after receiving treatment. This can include glasses, contacts, or additional vision correction procedures.
Since each patient's keratoconus is different, the best vision correction option for one patient may not be indicated for another.
After having keratoconus treatments, it is important to be thoroughly assessed by your eye doctor and to discuss the best vision correction option for your specific case. — Dr. Brian Boxer Wachler
Q: I have been diagnosed with the beginning stage of keratoconus and was prescribed rigid gas permeable lenses to treat the condition. However, I could not tolerate wearing these lenses. What are any other treatment options relating to this condition? — M.C., Wisconsin
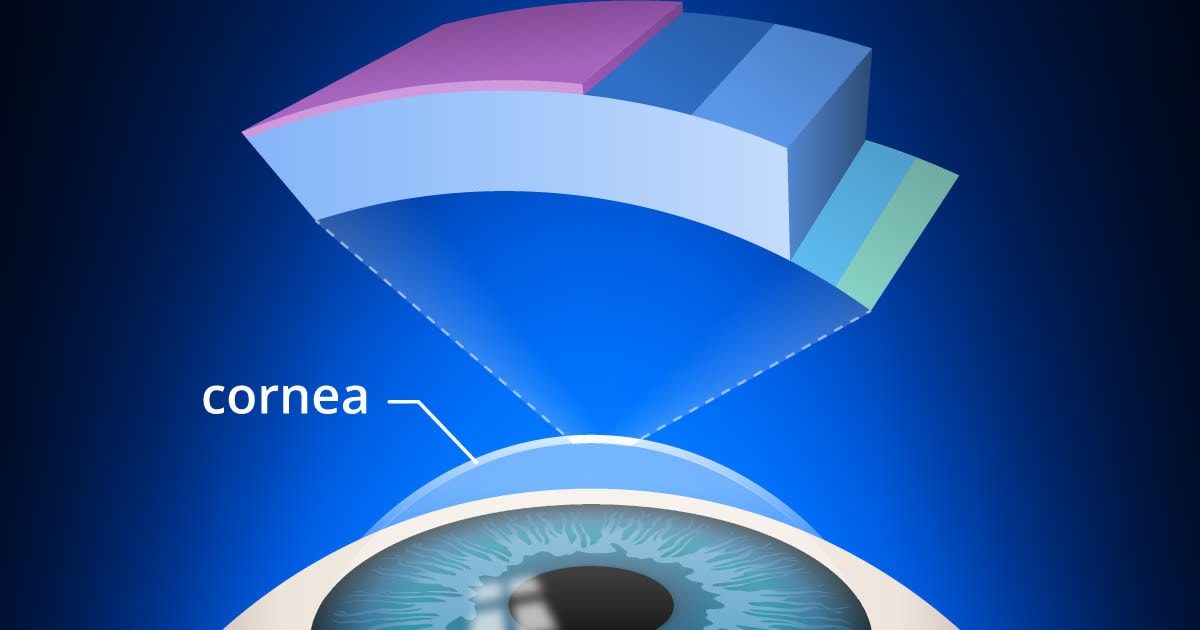
A: Keratoconus is an eye condition where the clear front surface of the eye, the cornea, gets thin and bulges outward into a cone shape. This usually begins in the teens or early 20s, but can affect children as young as 8 years old or people in their 50s and 60s. And one eye is usually worse than the other eye. It occurs in children of parents with keratoconus in about 6 percent of the time. So children are advised to get checked if one parent has keratoconus.
As the cornea thins and bulges, it becomes distorted and even droopy, creating blurred vision that is not very correctable with glasses. Certain types of contact lenses can vault over the irregularly shaped cornea to help focus light properly. Rigid gas permeable lenses (also called RGP or GP lenses) usually can be prescribed successfully.
There are a number of gas permeable lens designs that can be tried before turning to other options. Before you give up on GP lenses, ask your practitioner if he or she can prescribe specially made rigid lenses such as the Rose K design for keratoconus. Also, large-diameter scleral contact lenses made of GP material might work better than standard RGP lenses.
If GP lenses simply will not work, hybrid contact lenses might be an option. These lenses have a GP central zone, surrounded by a skirt of soft lens material for added comfort, and special designs are available for keratoconus.
Soft lenses also are made for people with keratoconus, but they are not rigid enough to help keep the cornea from bulging over time. On the other hand, often they can offer better vision than glasses.
Your eye care practitioner also can consider a contact lens fitting technique called piggybacking, which is an RGP lens fitted over a soft lens. This combination can make RGP lenses much more comfortable and give you excellent vision as well.
Please keep in mind that people with keratoconus usually have a harder time with contact lens comfort and vision. Their eyes are not normal, their tears are not normal, etc. Give your practitioner plenty of time to get you up and running, and expect more frequent tune-ups than a regular patient would need. Most importantly, look at the good side: Keratoconus is not a fatal disease and does not cause blindness. Hang in there! — Dr. Brian Boxer Wachler and Dr. Burt Dubow
Q: A doctor recently diagnosed me with keratoconus. He prescribed soft contact lenses, and my vision is back to 100 percent, but I was wondering if there are any other treatments for this condition. — Eric, Florida
A: Keratoconus is a condition where the front of the eye (cornea) bulges outward into a cone shape, distorting vision.
Intacs can flatten the cornea and reduce irregularities, helping people with keratoconus see much better.
Also, a surgical procedure called corneal crosslinking (CXL) can strengthen the collagen fibers within the cornea, making the front of the eye harder and less flexible to prevent the disease from progressing.
Some people also may be candidates for a cornea transplant, where the center of the cornea is removed and a donor cornea is put in its place. This should be reserved as a last resort, since a cornea transplant is invasive and carries serious risks.
Follow your eye doctor's advice. He or she will advise you of the best options to successfully manage your keratoconus. — Dr. Brian Boxer Wachler and Dr. Burt Dubow
Q: I was just told that I have severe keratoconus and glaucoma. I suspect I can see colors only from my left eye. Will I be able to get a driver's license? — A.J.
A: Each state's requirements vary somewhat. Typically it's required to have vision (without or with contact lenses or glasses)of 20/40 or better in at least one eye. Please check with the Department of Motor Vehicles for your state. — Dr. Brian Boxer Wachler
Q: Should people with keratoconus be driving a motor vehicle? — D.
A: As long as they meet the driving requirements. — Dr. Brian Boxer Wachler
Q: I'm totally confused about this: Is my cornea an oval shape or is my eye an oval shape if I have keratoconus? — L.S.
A: With keratoconus, the cornea (the clear front surface of the eye) loses its essentially spherical shape and becomes progressively elongated, like the tip of an American football or a rugby ball. The rest of the eyeball retains its normal shape. — Dr. Brian Boxer Wachler
Q: Does this eye condition cause night blindness and make it hard to see when driving? — S.S.
A: Keratoconus can result in difficulty driving at night from starbursts, glare, halos and multiple images. — Dr. Brian Boxer Wachler
Q: Does early diagnosis make any difference in keratoconus progression? — A.
A: Definitely. Early diagnosis means vision may be only minimally affected. In those cases, corneal crosslinking should be considered to stabilize and prevent future vision loss. — Dr. Brian Boxer Wachler
Q: I wear RGP contacts, but one of the contacts was too tight on my eye. Now I see worse with that eye! So could the tightness of the contact have caused that? — H.
A: You should discuss with your optometrist the particulars of your situation. — Dr. Brian Boxer Wachler
Q: I was told by my doctor that I am in the moderate stage of keratoconus. I have started using RGP lenses. Can you please tell me whether RGP lenses reduce the progression of the disease and what the side effects are of wearing RGP lenses? — S.
A: Some doctors mistakenly tell patients that RGP contact lenses halt the disease from progressing. This is like saying a baseball cap will prevent a skull from expanding. The only proven method to halt progression is with corneal collagen crosslinking. — Dr. Brian Boxer Wachler
Q: My 13-year-old son was just recently diagnosed with keratoconus in both eyes. We have had him fitted for soft contact lenses. Will that control it or will he need to try other options? One eye is not so bad, but the other eye is very bad. — A.
A: Contacts improve vision, but they do not control the disease. Corneal collagen crosslinking is the only proven method of halting the progression of keratoconus. — Dr. Brian Boxer Wachler
Q: I took my daughter to the eye doctor, and he said that my daughter may have keratoconus. They took a picture of inside her eye and said she needs to come back in three weeks. How hard is this to detect? — V.
A: Corneal topography mapping of the cornea is the gold standard test to detect keratoconus. — Dr. Brian Boxer Wachler
Q: Can you go blind if you have keratoconus? — M.B.
A: It's possible to lose vision to the point of being legally blind (20/200 vision or worse). — Dr. Brian Boxer Wachler
Q: Is it possible to apply the crosslinking procedure on an eye where another cornea graft was inserted previously? If so, would it be a success? (I mean, the visual acuity would not get worse after this procedure?) Please tell me if the procedure carries risk. — C.V.
A: We have had success in performing corneal collagen crosslinking to a cornea transplant that re-developed keratoconus. — Dr. Brian Boxer Wachler
Q: Is pellucid marginal degeneration the same as or a subcategory of keratoconus? I've been told I have both but am finding information online indicating that they are not the same thing. — M.
A: Pellucid marginal degeneration is a subtype of keratoconus. It's the same disease, but in "pellucid" the steepening is in the far periphery of the cornea. — Dr. Brian Boxer Wachler
Q: I have keratoconus, and currently I wear hard rigid gas permeable (RGP) lenses. I'm very sensitive to sunlight. What sunglasses should I use? — W.
A: People with keratoconus should always wear sunglasses, in my opinion, because they protect the corneas from the harmful ultraviolet light of the sun, which has been shown to increase free radicals (cellular byproducts) that can accelerate keratoconus progression. — Dr. Brian Boxer Wachler
Q: My eye doctor told me that with kerataconus I would need contacts that have a steeper cone than the contact resting on the eye. I've been wearing contacts (soft perm) for more than 15 years and have had no problem with these types of contacts. Unfortunately, they no longer make them. The contacts have always rested on the eyes, and during these 15 years the doctors have told me that I needed the contact resting on the eyes. This new doctor says scar tissue will develop if this is continued. Is this true? — C.
A: There is a risk of scar tissue developing from keratoconus progression. There may be an increased risk if the RGP contacts are not fit properly. — Dr. Brian Boxer Wachler
Please note: If you have an urgent question about your eye health, contact your eye care practitioner immediately. This page is designed to provide general information about vision, vision care and vision correction. It is not intended to provide medical advice. If you suspect that you have a vision problem or a condition that requires attention, consult with an eye care professional for advice on the treatment of your own specific condition and for your own particular needs. For more information, read our Terms of Use.