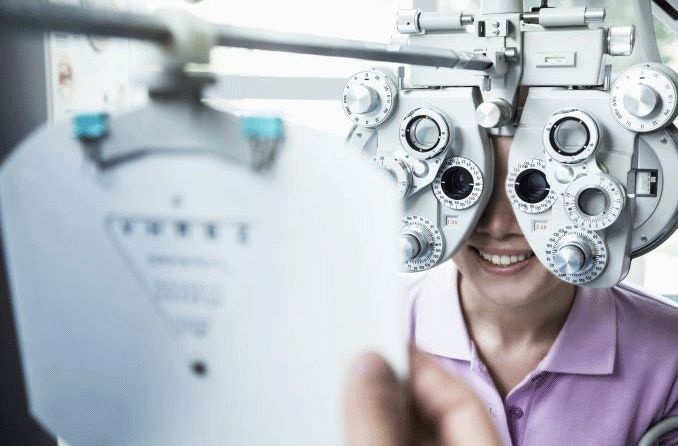
Does Medicaid cover eye exams? The answer depends on your age, your U.S. state and your Medicaid coverage.
For example:
For children and young adults under 21 who are eligible for Medicaid's Early and Periodic Screening, Diagnostic and Treatment (EPSDT) benefits, the costs of identifying and correcting vision issues is a covered expense. This means the costs of eye exams and eyeglasses are covered by Medicaid.
For adults over age 21, Medicaid in most U.S. states will cover routine eye exams for adults, though coverage varies by state. As of 2022, seven states provided no coverage for eye exams or eyeglasses under any Medicaid plan. Even in states with coverage, frequency limits and copays may apply.
Why does your state of residence matter? Medicaid benefits are determined by each state, but must meet federal guidelines by providing complete services that improve health concerns and conditions.
For this reason, it’s important for you to research your specific state’s coverage or contact your local Medicaid office for current information.
What is Medicaid and how does it work?
Medicaid is a state and federal program that supplies health insurance to very low-income people.
States use federal guidelines to provide their own set of benefits. Coverage often includes children and their parents or caretakers, pregnant women, older adults and those with disabilities.
Because each state has its own financial requirements for Medicaid eligibility, your income and assets will be assessed to determine whether or not you qualify. Typically, your income must fall below a certain level to be eligible for Medicaid benefits.
Those who qualify for Medicaid benefits typically receive coverage for:
- Physician services
- Pre- and post-natal care
- Laboratory services and X-rays
- Outpatient hospital care at specific locations
- In-hospital stays (excluding institutions for mental illness)
- Certain home health services
- Health screenings for people age 21 and younger
- Vision benefits (what's covered varies by state)
It’s possible someone may qualify for both Medicaid and Medicare. If this is the case, you’re able to enroll in both programs to cover expenses that may be covered by one plan but not the other. Case in point: Medicare does not normally cover long-term care, but Medicaid does.
Who accepts Medicaid for an eye exam?
Many eye care practices accept Medicaid for an eye exam, as long as it falls within the coverage schedule.
For instance, if your state covers only one eye exam every three years and you schedule an appointment after two years, that eye exam will not be covered. There are exceptions, such as if you have an underlying condition that qualifies you for more frequent exams.
To find eye care practices in your area that accept Medicaid, use All About Vision's Doctor Locator, which lets you search for eye doctors who accept your vision insurance. The locator will list eye doctors near you who accept Medicaid; then you can schedule an appointment.
How much does an eye exam cost with Medicaid?
Eye exam copays can vary, depending on your state. Most states also have different copays for children and adults.
Depending on the state, your copay also could cover eyeglasses, or there could be a separate fee. Check your state's Medicaid vision benefits so you will know what's covered and your expected costs.
How often does Medicaid pay for an eye exam?
States are required to adhere to the recommended schedule for child and adolescent vision and hearing screenings.
All screenings must meet a certain standard of medical practice, which is determined by a credible pediatric health organization.
For adults over age 21, the frequency of covered eye exams depends on which state you live in. On average, an eye exam is covered approximately every two or three years.
To get the most accurate information for your state’s Medicaid practices, contact a Medicaid representative in your state’s designated region.
TIME FOR AN EYE EXAM UNDER YOUR STATE'S MEDICAID PROGRAM? Find a local eye doctor who accepts Medicaid coverage.