What is primary acquired melanosis (PAM)?
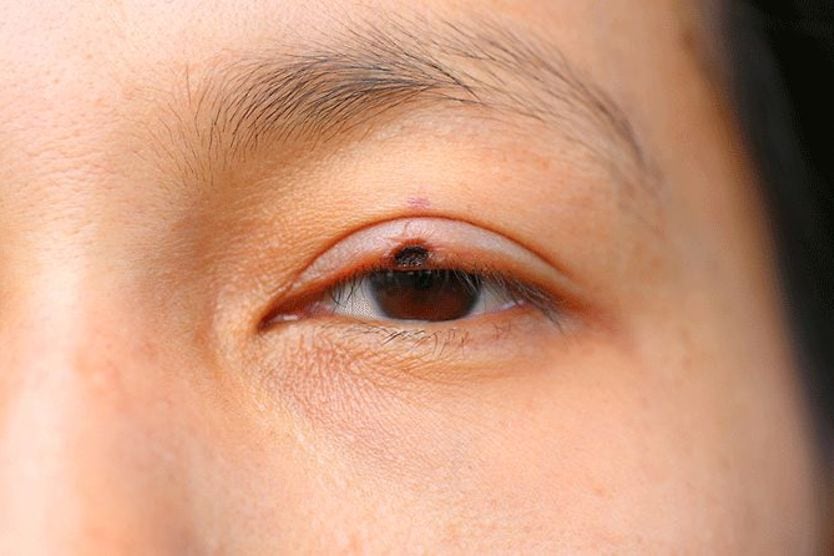
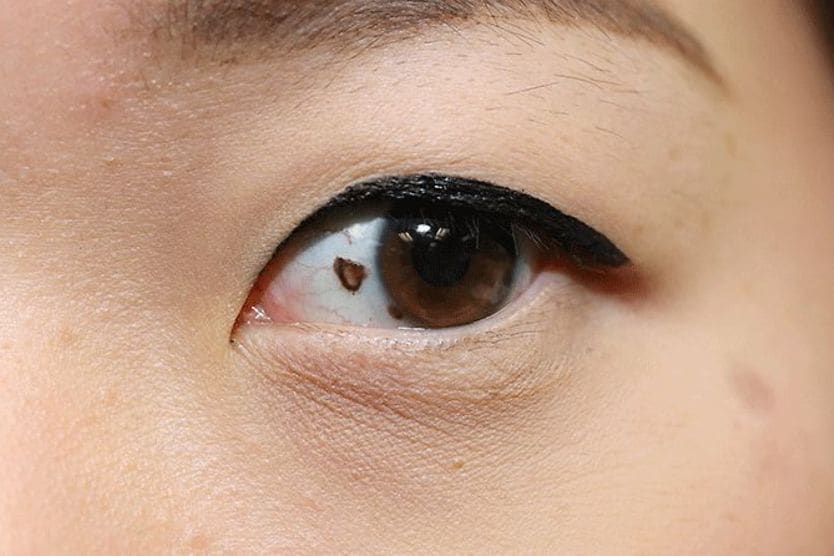
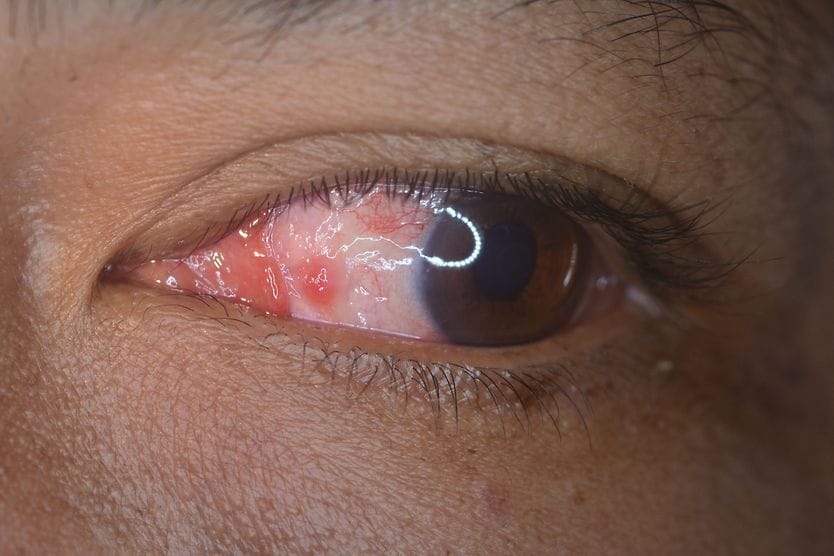
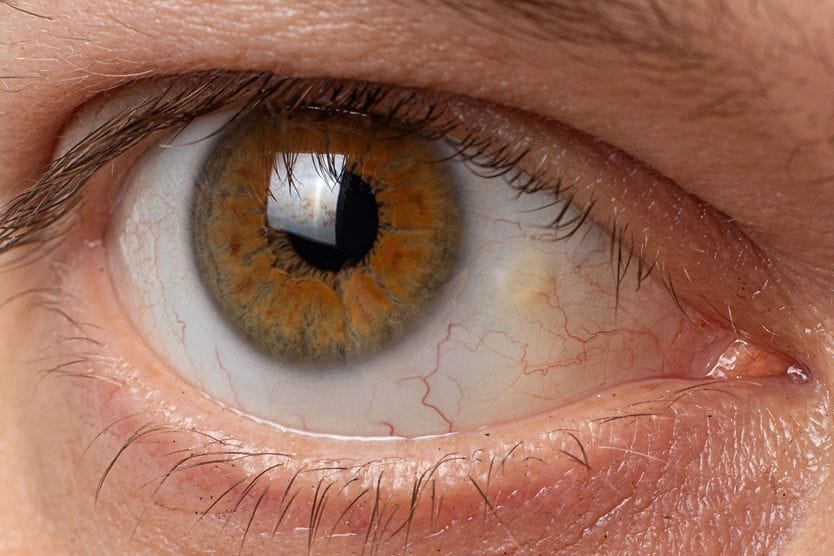
Conjunctival primary acquired melanosis (PAM) is a pigmented, brown, flat patch on the conjunctiva — the clear tissue that covers the white of the eye (the sclera). It is benign (not harmful) and painless and occurs in one eye. Although PAM changes slowly, it can lead to malignant ocular melanoma.
PAM is typically seen in middle-aged and older adults who are light-skinned. An eye doctor should evaluate any new pigmentation that develops in the eye. Conjunctival primary acquired melanosis can be precancerous and early detection is critical.
Conjunctival melanosis causes
A proliferation of melanin-producing cells causes primary acquired melanosis. Melanosis can occur anywhere on the body, but with PAM, it appears on the eye's conjunctiva. Over time, PAM has the potential to convert to malignancy (become cancerous).
The cells that produce melanin are called melanocytes. Hair, eyes and skin all have color due to melanin. Excess melanin production leads to hyperpigmentation, which manifests as discolored patches. Primary acquired melanosis (PAM) refers to the new development of pigmented patches on the conjunctiva.
Secondary acquired melanosis
If conjunctival melanosis develops due to another condition, it is called secondary acquired melanosis. This can result from:
- Another conjunctival lesion such as eye cancer (carcinoma)
- A benign growth such as squamous papilloma
- A disease affecting the entire body such as Addison disease
- Prior radiation
- Pregnancy
Other causes of conjunctival pigmentation
Other types of pigmentation can also occur on the conjunctiva, including racial melanosis and nevus, both of which are typically benign (not harmful). Racial melanosis occurs in people with naturally dark skin color. In contrast to PAM, racial melanosis often affects both eyes and remains present throughout a person’s life.
A nevus — the medical term for a simple eye freckle — can also occur on the conjunctiva. While a conjunctival nevus is likely benign, it should be monitored by your eye doctor for any changes.
Signs and symptoms
PAM does not typically affect vision. It appears as flat, patchy areas of tan or brown. The patches can change in size or color over time, or they may remain stable over the years.
The pigmentation is usually only in one eye and can extend to the junction between the conjunctiva of the inner eyelid and the conjunctiva covering the whites of the eyeball. These points are known as the inferior and superior fornices.
Changes in patch appearance and size can be brought on by hormonal changes or inflammatory conditions. If the pigmentation on the conjunctiva is raised or has blood vessels growing into it, your eye doctor is more likely to perform a biopsy.
Risks
The majority of instances of PAM are benign. Still, a sizable number may develop into melanoma. Although it’s not possible to anticipate with complete accuracy which cases will convert to cancer, the main indicators of higher risk are:
- Bigger size
- Pigment development in certain locations
Additional indicators of risk include:
- Continued growth
- Formation of nodules
- Growth of blood vessels into the pigmented area
- Thickening
The most crucial finding in predicting whether PAM will progress to malignant melanoma is to detect cellular atypia — the presence of abnormal cells that are not cancer but are at high risk for cancer. This is done with a biopsy, which means that some tissue is removed for evaluation in a laboratory.
Treatment and management
An eye doctor will perform a thorough examination of the eye’s surface. They will look at the inside of the eyelids by inverting them.
A biopsy will confirm whether a pigmented patch on the conjunctiva is primary acquired melanosis, an eye freckle (nevus) or malignant melanoma.
If the biopsy shows that the pigmented area is PAM, management will vary depending on the results:
- PAM without atypia – This type can simply be monitored because it has a minimal risk of becoming malignant. Your doctor may take a picture to document the changes and schedule a follow-up evaluation every 6 to 12 months.
- PAM with mild atypia – This type will be closely monitored for changes despite the low likelihood of malignant change.
- PAM with moderate to severe atypia – This type carries a considerable risk of progression to melanoma. Your ophthalmologist will remove all the pigmented areas on the conjunctiva before melanoma forms. This is typically done surgically with cryotherapy (freezing and removing of abnormal tissue) or with chemotherapy eye drops.
READ NEXT: Ocular melanosis
When to see a doctor
Any development of new pigmentation in the eye should be examined by an eye doctor. Early detection is crucial because primary acquired melanosis of the conjunctiva can be precancerous.
Routine comprehensive eye exams provide annual screening for the development of potentially serious conditions, including primary acquired melanosis.
And finally, always remember to protect your eyes from harmful UV exposure by wearing sunglasses that provide 100% of UVA and UVB light.
READ MORE: Ocular Melanoma Awareness Month