
Corneal Surgery
Corneal procedures can help preserve or even restore sight for some patients. Learn about some of the different types of corneal surgery and which conditions they can help.
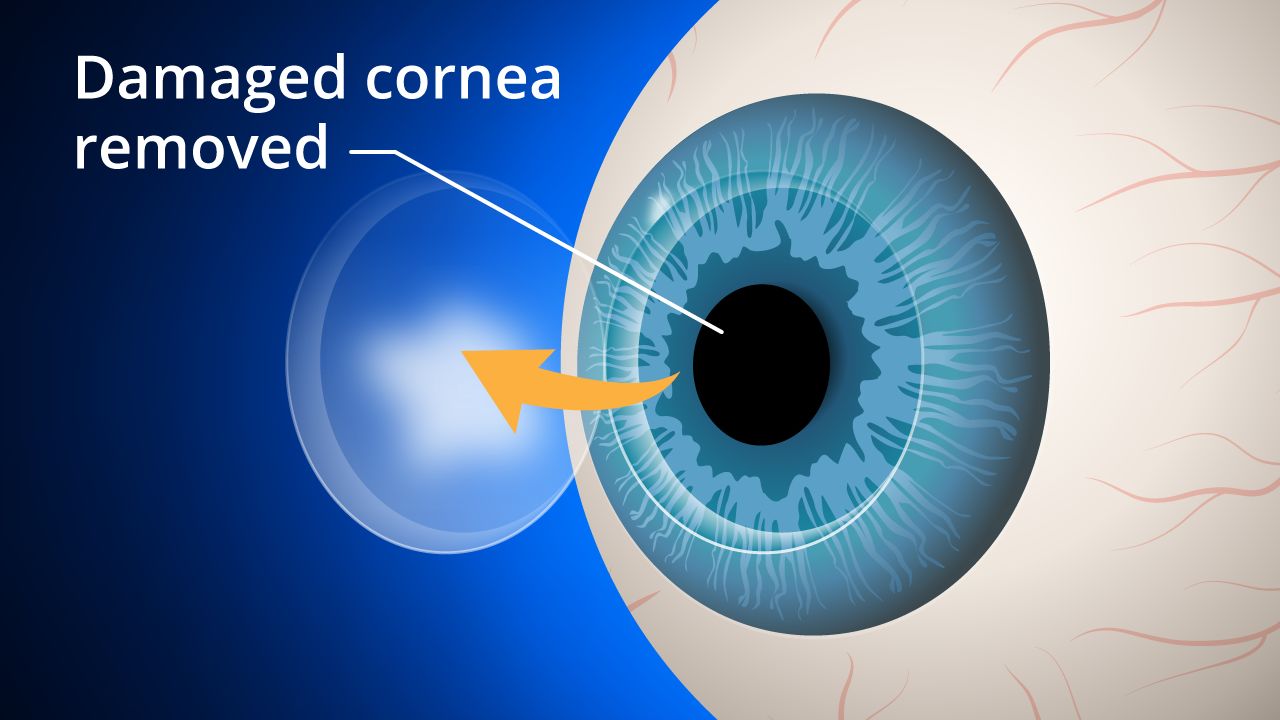
A corneal transplant (keratoplasty) involves replacing cornea damage with healthy donor tissue. Here’s what you can expect before, during and after surgery.
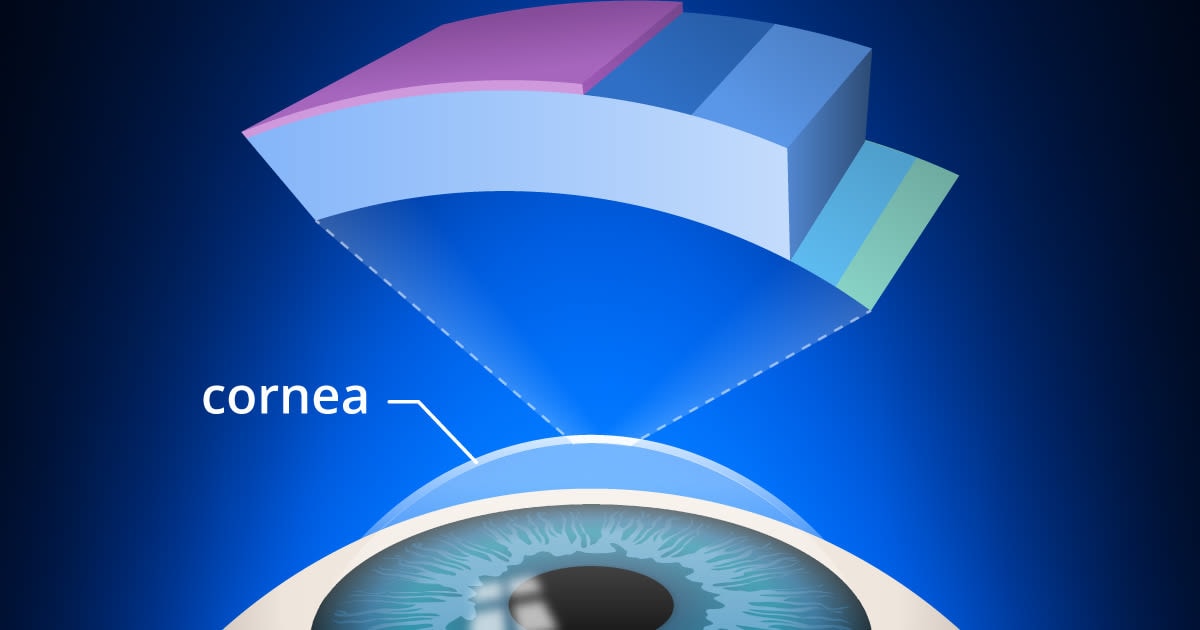
Discover the two types of corneal cross-linking for severe keratoconus and other cornea issues. Learn if corneal cross-linking surgery is for you and expectations.

How Intacs corneal implants for keratoconus flatten bulging eyes; also called corneal inserts.

Learn more about tarsorrhaphy, a procedure where the upper and lower eyelids are joined together to help heal and protect the corneal surface of the eye.

In tooth in eye surgery, specialists use one of your teeth to help create a prosthetic cornea. Learn how this surgery works and how it restores vision.
All About Vision and AllAboutVision.com are registered trademarks of AAV Media, LLC. © 2000-2025 AAV Media, LLC. The content on this site is for informational purposes only. All About Vision does not provide medical advice, diagnosis or treatment. Contact an eye doctor if you need medical attention.