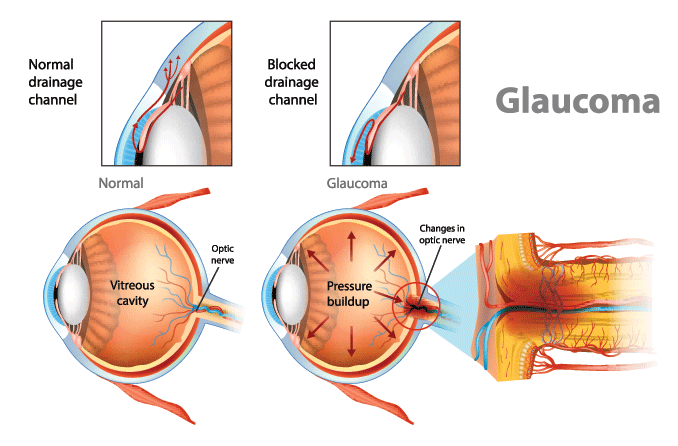
What is congenital glaucoma?
Congenital glaucoma is a rare eye condition present at birth in which fluid does not drain properly from the eye, leading to elevated eye pressure that can damage the optic nerve. This condition needs to be treated, or it can lead to irreversible vision loss.
Types
"Congenital glaucoma" isn't a medical condition on its own. Instead, some people use that term to talk about one of two separate conditions:
- Primary congenital glaucoma
- Secondary congenital glaucoma
Both are types of childhood glaucoma .
Primary congenital glaucoma (PCG)
Primary congenital glaucoma is present at birth. It happens on its own and isn't caused by another health condition. Some doctors call it PCG for short.
It's the most common type of childhood glaucoma that isn't caused by another problem. But it's still rare overall.
About one in 10,000 babies are born with PCG. This can be higher or lower depending on the parents' ethnicity.
PCG usually happens in both eyes, but it can happen in one eye, too. It affects more boys than girls.
Primary congenital glaucoma is classified in three different ways:
- Newborn onset – Diagnosed in babies between birth and one month old. Sometimes called newborn glaucoma or true congenital glaucoma. About one in four cases of PCG have a newborn onset.
- Infantile onset – Diagnosed between 1 and 36 months old. Sometimes called infantile glaucoma. Most cases of PCG have an infantile onset (about two in three cases).
- Juvenile onset – Diagnosed in kids older than 3, during childhood or adolescence. About one in 10 cases of PCG have a juvenile onset. It is called juvenile open-angle glaucoma (JOAG) which can cause high pressure in the eyes of children, teenagers, and young adults (typically between ages 3 and 40).
Secondary congenital glaucoma
Secondary congenital glaucoma also starts at birth, but it's caused by a separate eye condition or health problem.
Causes
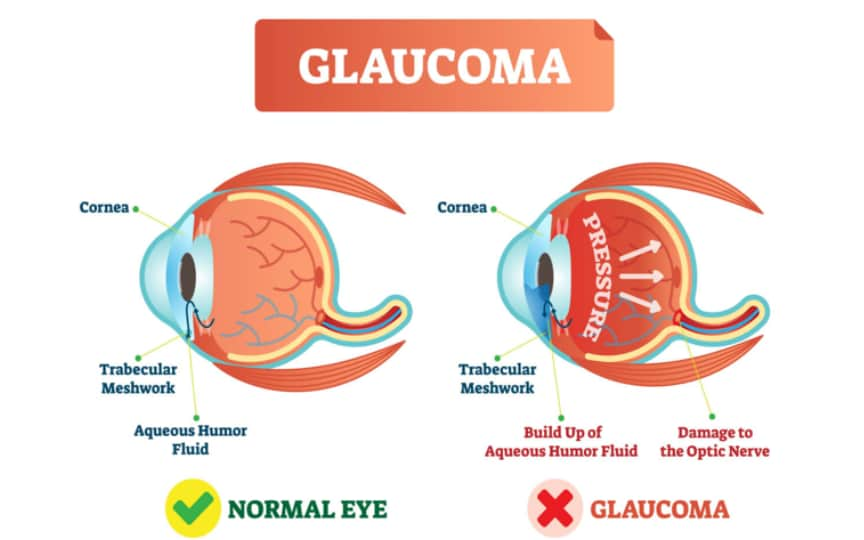
The eye is constantly making fluid to deliver nutrients and moisture to other parts of the eye. The extra fluid drains out of the eye through a microscopic web called the trabecular meshwork (TM). Then, it goes back into the bloodstream.
Primary congenital glaucoma often happens when:
- A child's trabecular meshwork (or the angle the fluid has to drain through), doesn't develop properly.
- The fluid can't drain out fast enough, and pressure builds up inside the eye.
- High pressure damages the eye.
An eye doctor's goal is to stop or reverse as many of these harmful changes as they can. Without treatment, damage can cause permanent vision loss.
Researchers aren't exactly sure what causes PCG to develop in the first place. They think that about four in every 10 cases of primary congenital glaucoma happen when a certain genetic trait is passed down from a parent.
Secondary congenital glaucoma is usually caused by an eye defect that develops before a baby is born.
Some of these conditions are:
- Axenfeld-Rieger syndrome
- Aniridia
- Peters anomaly spectrum
- Sturge-Weber syndrome
- Retinopathy of prematurity
- Microphthalmos
- Glaucoma following congenital cataract surgery
SEE RELATED: How pediatric ophthalmologists are different from other eye doctors
Signs and symptoms
Many parents first go to an eye doctor when they or the pediatrician notice something unusual about their child's eyes or eyesight.
The three most common symptoms of primary congenital glaucoma include:
- Sensitivity to light
- Watery eyes
- Unusual eyelid twitching or blinking
You might also notice:
- The front layer of their eye(s) looks cloudy
- The white part of their eye(s) has a blue tint
- One or both eyes look too big
An eye doctor will look for certain signs in your child's eyes that help them diagnose PCG. These will be hard or impossible for you to see on your own.
Signs of primary congenital glaucoma can include:
- An enlarged cornea (the clear layer at the front of the eye)
- Stretch marks on the inside of the cornea (called Haab’s striae)
- An unusually shaped pupil (the small, black hole in the front of the eye)
- Problems on the iris (the colored part of the eye)
- A high measurement of pressure inside the eye
The symptoms of secondary congenital glaucoma depend on the underlying cause.
For example, a child with Axenfeld-Rieger syndrome might look like they have off-center pupils or more than one pupil opening.
Meanwhile, a child with Peters anomaly will not have these symptoms. Instead, they'll have a cloudy white patch on the front of their eye.
Diagnosis
Diagnosing congenital glaucoma in children early can help you protect as much of their vision as possible.
Glaucoma can develop for a long time without any obvious symptoms. This is especially true for children, since they can't tell you when something is wrong with their eyesight.
This is why it's so important to have an eye doctor regularly examine your child's eyes.
A check-up can also help the doctor rule out eye conditions that can seem like primary congenital glaucoma or cause secondary congenital glaucoma.
Experts recommend following this schedule:
- The first eye exam between 6 and 12 months old
- One eye exam between ages 3 and 5
- One eye exam before first grade
- One eye exam per year from second grade onward
Your eye doctor might recommend getting eye exams more often if your child has an eye condition or is at high risk of developing one.
If you notice any changes in your child's eyes or vision, talk to your eye doctor. Don't wait for their next routine check-up.
During an eye exam, the eye doctor will use special tools to look at the surface of your child's eyes and inside their eyes. These tests don't hurt, but they can be hard to perform on a baby or very young child.
If your eye doctor thinks your child could have congenital glaucoma, they may recommend putting your child to sleep (general anesthesia) so they can examine their eyes.
SEE RELATED: Why kids' eye exams are so important
Treatment
Congenital glaucoma can't be prevented, but it can often be treated. Getting treatment early can help someone preserve vision later in life.
The success rate of treatment can be different for each child. Some children with congenital glaucoma go on to have normal vision or mild vision impairment. For more severe cases, the eye doctor may focus on saving as much of the child's eyesight as they can.
Many children with primary congenital glaucoma need to have surgery. An eye doctor could be more likely to try a non-surgical treatment (like medicated eye drops) when someone has secondary congenital glaucoma.
Eye doctors can use different types of glaucoma surgery to help lower their eye pressure, if surgery is needed.
Children are asleep or relaxed (sedated) during these procedures to make sure they aren't scared or in pain.
Their eye doctor will then use a tiny tool or laser to help their eye drain more fluid. This helps their eye pressure go down and protects the eye from damage.
Some children may need to have more than one surgery during their lives.
Management
Surgery can help lower the pressure inside someone's eyes, but the pressure may go back up over time. Most parents will need to manage their child's congenital glaucoma with medicine and routine check-ups.
Depending on someone's age and eye condition, the eye doctor may prescribe medicated eye drops or medicine taken by mouth to help manage their glaucoma over time. It's important to follow the medication schedule closely to keep their eye pressure down.
An eye doctor will likely recommend scheduling two or more routine eye exams per year to watch your child's eyes. These appointments can help the doctor find problems that may happen with congenital glaucoma.
These can include:
- High eye pressure and worsening eye damage
- Nearsightedness
- Crossed eyes
- Lazy eye
Many people who have congenital glaucoma need to get regular check-ups for the rest of their lives, since their eye pressure can go up again without warning.
Careful management and treatment can help many children live their lives with limited effects on their eyesight. However, children with severe glaucoma could experience significant vision loss.
Several nonprofit and government organizations work side by side with eye doctors to help kids with visual impairments thrive. These programs and support groups can help parents work through difficult times and provide valuable resources as their child grows up.
When to see an eye doctor
Schedule an appointment with an eye doctor any time you notice something unusual with your child's eyes or eyesight.
Even if everything seems normal, follow the recommended eye exam schedule for your child's age or risk factors. It could help diagnose an "invisible" problem like congenital glaucoma before it can cause any more harm.
Glaucoma treatment today is continually improving. An eye doctor can provide several surgery and management options to help your child live a fulfilling life.