What is pink eye (conjunctivitis)?
Understanding what pink eye looks like
Pink eye is the common name for conjunctivitis, which is an inflammation or infection of the eye's conjunctiva. When the tiny blood vessels in the conjunctiva are inflamed, they become more visible. This causes the whites of your eyes to appear reddish pink and is where the name pink eye comes from.
The conjunctiva is a very thin, clear membrane that covers the white of the eye (sclera) and the inner surface of the eyelids. When it is inflamed, the insides of your eyelids may also look more red than usual. Sometimes, they may even feel a little swollen or sore. Rubbing your eyes can make the swollen, sore feeling and redness worse.
Rubbing or touching the eyes can also cause the infection to spread to the other eye or to other people. Some types of pink eye are very contagious, so you should avoid touching your eyes as much as possible. Eye rubbing in general can also lead to other serious eye problems.
What causes pink eye?
Viruses are the most common cause of contagious conjunctivitis, but it is often also caused by bacteria. If certain viruses or bacteria enter the eye, conjunctivitis can develop. It can also develop if a person has a virus or bacterial infection that works its way through the body to the eyes. The viral and bacterial forms are very contagious and spread extremely easily.
Allergic conjunctivitis is not contagious, since it’s not a viral or bacterial infection. This form is very common and develops when allergens irritate the eyes. The casual name pink eye typically only refers to the contagious forms.
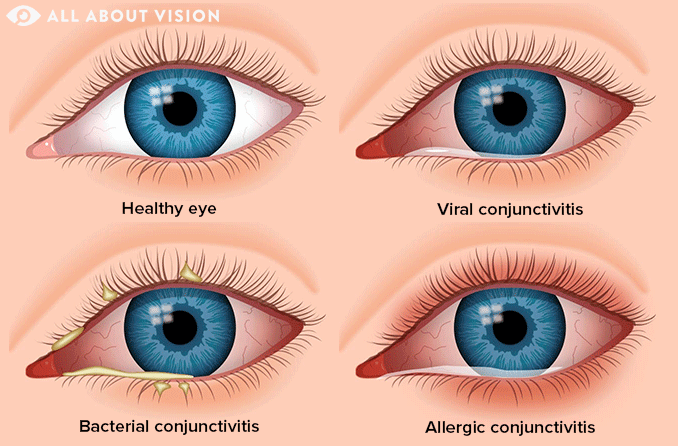
Viral conjunctivitis
Viral pink eye can be due to any of the viruses associated with the common cold, but the most common cause is adenoviruses. Adenoviruses are responsible for approximately 90% of cases. Coronaviruses (including the one that causes COVID-19), herpes simplex, varicella-zoster and Epstein-Barr viruses can also cause pink eye. The infections from these viruses are less common, but they are more serious than those caused by an adenovirus.
Bacterial conjunctivitis
Several different types of bacteria can cause pink eye. However, Haemophilus influenzae, Streptococcus pneumoniae and Staphylococcus aureus are behind most cases, especially in children. Less often, it can develop due to Neisseria meningitidis, the bacteria that causes meningitis. It can also be caused by STD bacteria such as Neisseria gonorrhoeae and Chlamydia trachomatis. All bacterial forms are usually spread by direct contact, like touching an infected person or item and then rubbing your eyes.
Allergic conjunctivitis
Any allergens that cause a reaction in the eyes can lead to allergic conjunctivitis. If your allergies inflame the conjunctiva of your eyes (making them red, swollen and extra itchy), they have caused allergic conjunctivitis. Many common allergens like pollen, dust and animal dander often lead to this condition. It can be seasonal (pollen), or it can flare up year round (dust; pet dander). Thankfully, allergic conjunctivitis is not contagious.
Other causes
Viruses, bacteria and allergies are the three main causes — but not the only causes. Conjunctivitis is, essentially, any inflammation of the conjunctiva. Any substance, condition or activity that irritates the eyes enough can cause conjunctivitis. Some of these other causes include:
Smoke, air pollution, and other irritants
Chemical splashes and fumes
Foreign objects in the eye, including dirt and cosmetics
Prolonged contact lens wear
SEE RELATED: Blepharoconjunctivitis
Pink eye signs and symptoms
Some signs and symptoms vary a little depending on the cause, but there is also some overlap.
The primary sign of all types of pink eye is the pink or reddish coloring of the sclera. Other visible signs include eye watering and eye discharge.
The primary symptoms of pink eye are burning, stinging and/or itchy eyes and a foreign body sensation. This is when it feels like there is something in the eye when there’s actually nothing there.
Viral pink eye tends to cause a thin, watery eye discharge. It may cause more of a burning sensation than soreness or itchiness. Some people may also experience some light sensitivity. It’s fairly common for people to also have other cold or flu-like symptoms at the same time as viral pink eye.
Bacterial pink eye typically has a thicker, stickier eye discharge that can be yellow or green. This can sometimes cause the eyelids to stick together during sleep. With bacterial pink eye, the eyes may feel more soreness than itching or stinging. They may also appear more red and swollen than with other types of conjunctivitis.
Allergic conjunctivitis usually causes the eyes to be extra watery or teary, but it may also cause some watery discharge. Extreme itchiness is mainly associated with allergic conjunctivitis. People experiencing this type may also have some puffiness or swelling around the eyes, as well as other common allergy symptoms.
Early stage symptoms
Viral pink eye symptoms can take five to 12 days to develop after a person is exposed. Bacterial pink eye symptoms develop much quicker and can be present within one to three days. After these incubation periods, both types can seem to show up quite suddenly.
In other words, the early symptoms are the same as later on: eye redness, irritation and discomfort, and discharge from your eye. However, they may worsen over the next few days before starting to get better. Bacterial forms may require treatment with antibiotics.
Both contagious types of pink eye can also begin in one eye and then spread to the other eye. In allergic conjunctivitis, both eyes will typically develop symptoms at the same time.
It can be difficult to tell the type of conjunctivitis you have by symptoms alone. There are also many other eye conditions with symptoms that look like conjunctivitis.
Any time you develop red, irritated eyes, schedule an eye exam with your optometrist or ophthalmologist as soon as possible.
Risk factors and complications
Anyone can get pink eye, but people (of all ages) who spend time in close contact with others are especially at risk. Contagious forms can spread very quickly in group, office or classroom environments.
Viral pink eye can be spread just like a cold: coughing, sneezing and not washing hands. And the viruses that cause it can live for up to two weeks on some surfaces. In addition, the viral forms are contagious even before symptoms appear.
People who wear contact lenses are also at a higher risk for pink eye. This risk increases even more if you:
Share contact lenses
Wear contacts that don’t fit well
Other risk factors include:
Not washing your hands frequently enough
Sharing cosmetics
Sharing towels, pillow cases, etc.
Newborn babies can also be at a higher risk for pink eye. This is called neonatal conjunctivitis, and it occurs if newborns are exposed to certain bacteria or viruses in the birth canal. Chlamydia, gonorrhea, strep and the herpes simplex virus are some of the common causes of neonatal conjunctivitis.
Most cases of pink eye clear up in a week or two without any complications. However, chronic or severe cases can lead to corneal inflammation, ulcers and even scarring. They may also lead to uveitis. These conditions can be vision threatening.
Pink eye treatment
In most cases, pink eye will resolve on its own in a week or two without any treatment. However, it’s still very important to see an eye doctor if you think you have it.
Some cases of bacterial pink eye do require treatment with antibiotics. Plus, conjunctivitis symptoms look very similar to many other eye conditions. An eye doctor needs to examine the eyes to make sure the symptoms are not due to something more serious.
Viral
Since it is caused by a virus, viral conjunctivitis can’t be treated with antibiotics. Fortunately, the viral form rarely requires treatment. In serious cases, a doctor may need to prescribe an antiviral medication.
Bacterial
Bacterial conjunctivitis usually clears up on its own, but it may require prescription antibiotic eye drops or ointment. In severe cases, it can lead to vision loss if left untreated.
Allergic
Oral allergy medications may help prevent the onset of allergic conjunctivitis. Over-the-counter lubricating and antihistamine eye drops can help relieve existing symptoms. In chronic or severe cases, a doctor may prescribe corticosteroid eye drops to reduce symptoms.
Usually, conjunctivitis treatment focuses on relieving symptoms. But it is important to remember that it is very difficult to self-diagnose. See an eye doctor right away if eye redness and other symptoms get worse or do not start to clear up in about a week.
How is conjunctivitis diagnosed?
An eye doctor will perform a comprehensive eye exam to diagnose pink eye. They will also ask about your medical history and your current symptoms to help determine what type of conjunctivitis you have. In rare cases, they may take a swab of eye discharge or conjunctival tissue to send for lab testing.
Does pink eye go away on its own?
This depends on the type of conjunctivitis you have. Most cases of viral conjunctivitis will run their course over the span of two weeks. The bacterial type can begin to improve within five days, or even more quickly if antibiotics are started.
Can you treat pink eye at home with natural remedies?
Over-the-counter and home remedies can help to safely ease the symptoms of conjunctivitis. Some of the most effective ways to reduce any discomfort are:
Using warm or cool compresses.
Using artificial tears to lubricate the eyes.
Taking over-the-counter anti-inflammatory or pain-relieving medication.
Avoiding use of any redness-reducing eye drops.
However, natural treatments are a different story. While some of them can be helpful, they may also be dangerous without a doctor’s guidance. Never use natural treatments for pink eye on yourself or your child without talking to your eye doctor first.
In fact, it’s important to see an eye doctor any time the symptoms are severe or last more than a few days. Certain types of conjunctivitis can have serious consequences, including vision loss. Plus, they share many of the same symptoms as other vision-threatening conditions, including:
Uveitis
Iritis
Corneal abrasion or ulcer
How to prevent pink eye from spreading
Conjunctivitis caused by bacteria or viruses is extremely contagious, so it’s important to avoid spreading it.
Viral pink eye is contagious well before symptoms appear and stays contagious until symptoms fully go away. Bacterial forms, if untreated, are also contagious as long as symptoms are present. However, you should stop being contagious about two days after beginning antibiotics.
Preventing the spread of pink eye comes down to practicing basic hygiene. Here are 10 ways to avoid spreading (and catching) conjunctivitis:

Wash your hands frequently, especially in shared or public spaces.
Avoid rubbing or touching your eyes.
Cover your nose and mouth when coughing or sneezing.
Keep hand sanitizer nearby and use it often.
Never share personal items such as washcloths, hand towels or cosmetics.
Disinfect countertops, bathroom surfaces, faucet handles and shared phones frequently.
Always follow your eye doctor's instructions for contact lens care and replacement. Remove contact lenses before showering.
Avoid swimming if you already have pink eye.
Wear swim goggles while swimming to prevent catching pink eye.
Ask your doctor how to minimize your seasonal allergy symptoms before they begin.
Despite these precautions, you or your child still may develop conjunctivitis.
If so, tell your child's teacher as soon as possible so they can sanitize the classroom or daycare center. Also, keep your child home until the contagious stage has passed. Wash your hands and your child’s hands often to help keep the infection from spreading.
Your eye doctor will let you know when the infection is no longer contagious. A child can usually go back to school or daycare about a week after their diagnosis.
RELATED READING: Pink eye in infants and Pink eye in children
When to see an eye doctor
See your eye doctor if you or your child develop a red, irritated eye or other symptoms of an eye infection.
Some types of conjunctivitis can be very serious if not treated. The symptoms of conjunctivitis can also look nearly identical to symptoms of other eye conditions. A red or pink eye can sometimes be a sign of a serious eye problem.
Causes of pink eye. National Eye Institute. July 2019.
Infective Conjunctivitis. Patient (Consumer). February 2017.
Conjunctivitis. Ada Health GmbH. July 2022.
Conjunctivitis: What is pink eye? American Academy of Ophthalmology. EyeSmart. April 2022.
Conjunctivitis (pink eye). American Optometric Association. Accessed August 2022.
Conjunctivitis or pink eye. MedlinePlus, National Library of Medicine. August 2020.
Are pink eye and conjunctivitis the same thing? American Academy of Ophthalmology. EyeSmart. January 2014.
Viral conjunctivitis. StatPearls [Internet]. May 2022.
Pink eye (conjunctivitis). Cleveland Clinic. April 2020.
Conjunctivitis information for clinicians. Centers for Disease Control and Prevention. August 2021.
Bacterial conjunctivitis. American Academy of Ophthalmology. EyeWiki. April 2022.
Meningitis. Centers for Disease Control and Prevention. March 2022.
Allergic conjunctivitis. MSD Manual Consumer Version. April 2021.
Causes of pink eye (conjunctivitis). Centers for Disease Control and Prevention. January 2019.
Pink eye. Johns Hopkins Medicine. Accessed August 2022.
Signs and symptoms of pink eye (conjunctivitis). Centers for Disease Control and Prevention. January 2019.
Pinkeye (conjunctivitis). Nemours KidsHealth. November 2020.
Conjunctivitis. South Dakota Department of Health. Accessed August 2022.
Pink eye. Virginia State University. Accessed August 2022.
Patient education: Conjunctivitis (pink eye) (Beyond the Basics). UpToDate. July 2022.
Treating pink eye (conjunctivitis). Centers for Disease Control and Prevention. January 2019.
Allergic conjunctivitis. Johns Hopkins Medicine. Accessed August 2022.
What is conjunctivitis? Association for Professionals in Infection Control and Epidemiology. Accessed August 2022.
Pink eye. National Eye Institute. August 2019.
Pink eye risk factors. Stanford Health Care. Accessed August 2022.
Preventing pink eye (conjunctivitis). Centers for Disease Control and Prevention. January 2019.
Pink eye: What parents should know. Children’s Health of Orange County. August 2017.
Neonatal conjunctivitis. American Academy of Ophthalmology. EyeWiki. January 2022.
Viral conjunctivitis. Ada Health GmbH. April 2022.
Bacterial conjunctivitis. Ada Health GmbH. July 2022.
Conjunctivitis. StatPearls [Internet]. May 2022.
What are eye allergies? American Academy of Ophthalmology. EyeSmart. January 2022.
Diagnosing pink eye (conjunctivitis). Centers for Disease Control and Prevention. January 2019.
Quick home remedies for pink eye. American Academy of Ophthalmology. EyeSmart. September 2021.
Page published on Monday, 16 March 2020
Page updated on Tuesday, 20 June 2023
Medically reviewed on Thursday, 18 August 2022






