Uveitis, iritis and eye inflammation
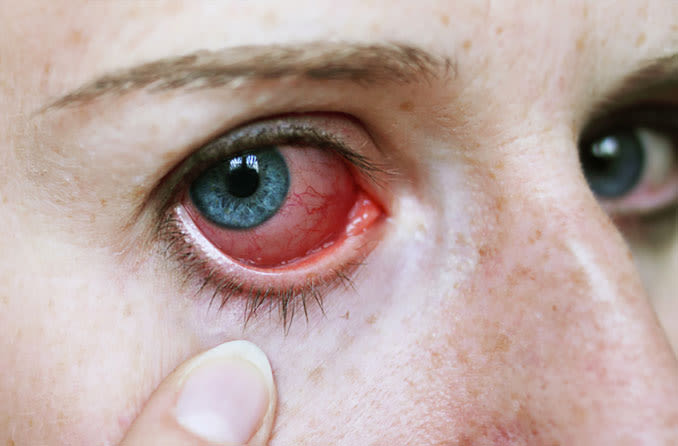
Uveitis is inflammation of the middle layer of the eyeball, which consists of the iris, ciliary, body and choroid. Collectively, these structures are called the uvea.
Uveitis can have many causes, including eye injury and inflammatory diseases. Exposure to toxic chemicals such as pesticides and acids used in manufacturing processes also can cause uveitis.
The type of uveitis you have is classified by where inflammation occurs in the uvea:
Anterior uveitis is inflammation of the iris (iritis) or the iris and ciliary body.
Intermediate uveitis is inflammation of the ciliary body.
Posterior uveitis is inflammation of the choroid.
Diffuse uveitis (also called pan-uveitis) is inflammation of all areas of the uvea.
This tiny drug implant (Retisert, Bausch+Lomb) is surgically implanted in the back of the eye, where it delivers sustained amounts of anti-inflammatory medication for treatment of uveitis.
Many cases of uveitis are chronic, and they can produce numerous possible complications, including clouding of the cornea, cataracts, elevated eye pressure (IOP), glaucoma, swelling of the retina or retinal detachment. These complications can result in permanent vision loss.
Statistics on the prevalence of uveitis vary in different regions of the world. However, researchers who reviewed 522 international articles concerning the causes and patterns of uveitis and 22 major epidemiology reviews concluded it affects 52.4 per 100,000 people.
Symptoms of uveitis
Symptoms of anterior uveitis include:
Intermediate and posterior uveitis usually are painless. Symptoms of these types of uveitis include blurred vision and floaters, typically in both eyes. Most people who develop intermediate uveitis are in their teens, 20s or 30s.
Diffuse uveitis has a combination of symptoms of all types of uveitis.
What causes uveitis?
Uveitis has dozens of causes, including viral, fungal and bacterial infections but in many cases, the cause is unknown.
Your optometrist often can identify the cause of uveitis if there has been trauma to the eye or you have an infectious or immunological systemic disorder.
Some of the many disorders that can cause uveitis include:
ankylosing spondylitis
herpes simplex (the cold sore virus)
herpes zoster (the virus that causes chicken pox and shingles)
inflammatory bowel disease
juvenile rheumatoid arthritis
leptospirosis
lupus
Lyme disease
multiple sclerosis
psoriatic arthritis
sarcoidosis
syphilis
toxocariasis
toxoplasmosis
tuberculosis
Also, smoking has been identified as a risk factor for uveitis.
Uveitis and iritis treatment
If your optometrist or ophthalmologist determines you have uveitis, he or she will likely prescribe a steroid to reduce the inflammation in your eye.
Whether the steroid is administered as an eye drop, pill or injection depends on the type of uveitis you have and whether it is being prescribed by an optometrist or ophthalmologist. As iritis affects the front of the eye, it's usually treated with eye drops.
Posterior uveitis usually requires tablets or injections. Depending on your symptoms, any of these treatments might be used for intermediate uveitis.
Steroids and other immunosuppressants can produce many serious side effects, such as kidney damage, high blood sugar, high blood pressure, osteoporosis and glaucoma.
This is especially true of steroids in pill form because the dose must be relatively high in order for enough of the drug to find its way to the back of the eye. So, it is important to follow your doctor or optometrist's dosage instructions carefully and to keep visiting him or her regularly to monitor the progress of the treatment.
If you have anterior uveitis, you will likely be prescribed, in addition to steroids, pupil-dilating eye drops to reduce pain. You also may need eye drops to lower your intraocular pressure if you develop high eye pressure due to uveitis.
If you have a known systemic condition that may be contributing your uveitis, your doctor will treat that as well.
If you suffer from sensitivity to light (photophobia) from chronic iritis or uveitis, ask your optometrist about photochromic lenses. These spectacle lenses darken automatically in sunlight to reduce photophobia-related discomfort when going outdoors.
Page published on Monday, 16 March 2020






