Cataracts: Types, symptoms and treatments
Overview
A cataract is a clouding of the eye's natural lens, which lies behind the iris and the pupil. Cataracts usually develop in both eyes, but sometimes they only affect one. Most cataracts occur as a result of getting older, usually sometime after age 50.
Cataracts are the most common cause of vision loss worldwide but they are easily treatable.
Causes of cataracts
As we age, the proteins that make up the eye's natural lens can clump together. These clumps are the cataracts and are what cause the cloudiness. Over time, these areas may increase in size, clouding more of the lens, making it harder to see.
The lens inside the eye works much like a camera lens, focusing light onto the retina for clear vision. It also adjusts the eye's focus, letting us see things both up close and far away.
Water and protein make up most of the lens of the eye. The protein is arranged in a precise way that keeps the lens clear and lets light pass through it.
No one knows for sure why the eye's lens changes as we age, forming cataracts. Researchers worldwide have identified factors that may be related to cataract development. Besides advancing age, cataract risk factors include:
Ultraviolet radiation from sunlight and other sources
Diabetes
Hypertension
Obesity
Smoking
Prolonged use of corticosteroid medications
Statin medicines used to reduce cholesterol
Previous eye injury or inflammation
Previous eye surgery
Hormone replacement therapy
Significant alcohol consumption
High myopia
Family history
One current theory is that oxidative changes in the human lens may be the cause of cataracts. Studies have shown that fruits and vegetables high in antioxidants may help prevent some types of cataracts.
Cataract symptoms
A cataract starts out small and, at first, has little effect on your vision. Visual symptoms can take months or years to become noticeable. You may notice that your vision is a little blurred, like looking through a cloudy piece of glass.
Cataracts can progress at a different rate in each eye, resulting in visual symptoms in one eye and normal vision in the other. You may also notice the following symptoms with cataracts:
Light from the sun or a lamp seems bright or glaring.
Your eyes feel more sensitive to light.
When driving at night, glare from oncoming headlights is worse than before.
Visual halos around bright lights.
Seeing at night or in low light is more difficult.
Colours may not appear as bright as they once did.
Blurry, cloudy, hazy or dim vision.
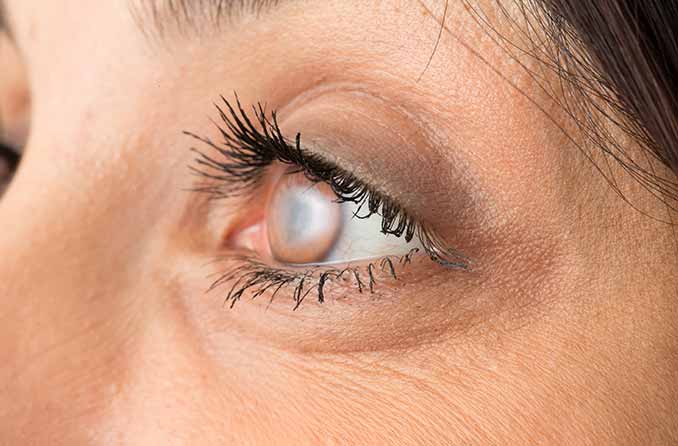
To the outside viewer, an advanced cataract can cause the pupil to appear light gray instead of black.
The type of cataract you have will affect exactly which symptoms you experience and how soon they will occur. If you think you have a cataract, see an optometrist for an eye test to find out for sure.
Types of cataracts
There are manytypes of cataract but a few are much more common.
Nuclear cataracts are the most common form of cataract. They form in the centre of the eye’s lens, gradually worsening and affecting vision.
Cortical cataracts usually are spoke-like opacities that begin near the edge of the lens and spread toward its centre. These make you experience more glare, making night driving particularly difficult.
Congenital cataracts are lens opacities that are present at birth in one or both eyes. They may be very small, with little effect on vision, or more severe.
Trauma-induced cataracts can form anywhere on the lens and often develop into a flower-petal or “rosette” shape.
Posterior subcapsular cataracts develop in the middle of the back surface of the lens. These types of cataracts tend to develop faster than the others. Symptoms usually affect your vision around bright light and colours.
Cataract treatment
When symptoms begin to appear, you may be able to improve your vision for a while using:
New glasses.
Stronger lenses for near vision.
Magnifiers.
Appropriate lighting or other visual aids.
Treatment options for cataracts that have progressed includes cataract surgery.
If cataracts start to affect your quality of life, then your optometrist may suggest surgery. This is generally seen as a low-risk and effective way to restore your vision.
Many people consider poor vision an inevitable fact of aging, but cataract surgery is a simple, relatively painless procedure to regain vision.
Cataract surgery is very successful in restoring vision. It is one of the most frequently performed surgery in Australia and New Zealand. More than 250,000 people in Australia undergo cataract surgery each year. According to Medibank, in 2018 there were more than 700,000 Australians living with cataracts.
Diagnosing cataracts
Optometrists can use different tests to diagnose cataracts.
Slit-lamp exam: A slit lamp is a large, binocular microscope with a bright light source that’s mounted on a small table. It enables your optometrist to closely examine your eye under high magnification (including checking the lens for cataracts).
Retinal exam: First, an optometrist will dilate your eyes with eye drops, causing the pupils to slowly open. This gives them a much better view inside your eye. The optometrist then examines the retina and optic nerve in the back of your eye. A dilated eye exam also provides the best view of any cataract formation in the lens.
Refraction: During a refraction, your optometrist determines the degree of your refractive errors and the glasses prescription that provides your best possible visual acuity. If your glasses prescription has changed and your vision can no longer be corrected to 6/6 (20/20), it’s possible you may have a cataract developing.
Cataracts don’t always require treatment after they’re diagnosed, especially if they aren’t bothering you. Initially, a simple change of your prescription may restore acceptable vision.
Preventing cataracts
Currently, there is no known way to stop cataracts from developing. However, if you can limit some of the risk factors listed above, it may slow their rate of progression. Ways to limit cataract risk factors can include:
Wearing sunglasses during the day to reduce your eyes’ exposure to the sun’s UV radiation.
Quitting smoking.
Eating a healthy diet and maintaining an exercise regimen.
Managing and reducing the effects of coexisting conditions like diabetes or hypertension.
Getting frequent eye tests to ensure any developing cataracts get diagnosed early.
Gary Heiting, OD, and Judith Lee also contributed to this article.
Cataracts. Prevent Blindness. Accessed April 2021.
Age-related cataract is associated with type 2 diabetes and statin use. Optometry and Vision Science. August 2012.
Diet, vegetarianism, and cataract risk. The American Journal of Clinical Nutrition, May 2011.
Prevalence and risk factors for cataract in diabetes: Sankara Nethralaya Diabetic Retinopathy Epidemiology and Molecular Genetics Study, report no. 17. Investigative Ophthalmology & Visual Science. December 2010.
Hormone replacement therapy in relation to risk of cataract extraction: A prospective study of women. Ophthalmology. March 2010.
Dietary carotenoids, vitamins C and E, and risk of cataract in women: A prospective study. Archives of Ophthalmology. January 2008.
Alcohol consumption and risk of cataract extraction: a prospective cohort study of women. Ophthalmology. April 2007.
Prospective study of dietary fat and risk of cataract extraction among U.S. women. American Journal of Epidemiology. May 2005.
Diabetes, hypertension, and central obesity as cataract risk factors in a black population: The Barbados Eye Study. Ophthalmology. January 1999.
Sunlight exposure and risk of lens opacities in a population-based study: The Salisbury Eye Evaluation Project. The Journal of the American Medical Association (JAMA). August 1998.
A prospective study of alcohol consumption and risk of cataract. American Journal of Preventive Medicine. May/June 1994.
The Lens Opacities Case-Control Study: Risk factors for cataract. Archives of Ophthalmology. February 1991.
Page published on Monday, 16 March 2020






