Comprehensive eye examination: What to expect
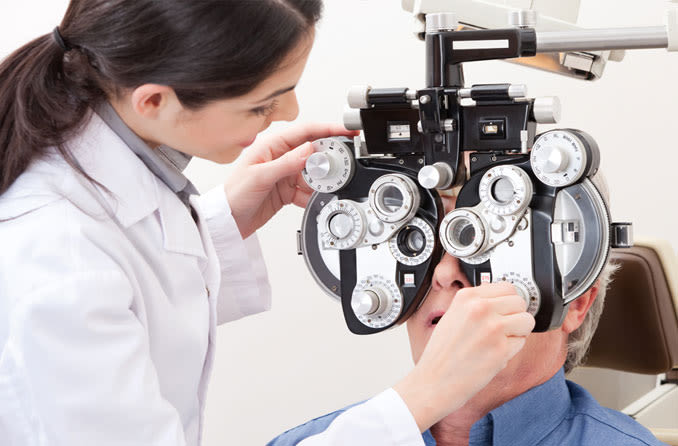
Optometrists use a wide variety of tests and procedures to examine your eyes. These tests range from simple ones, like having you read an eye chart, to complex tests, such as using a high-powered lens to visualise the tiny structures inside your eyes.
A comprehensive eye examination can take more than half an hour, depending on the optometrist and the number and complexity of tests required to fully evaluate your vision and the health of your eyes. This doesn't take into account any discussion about your visual needs and things that can be prescribed to help your vision overall.
Here are eye and vision tests that you are likely to encounter during a comprehensive eye exam:
Visual acuity tests
Among the first tests performed in a comprehensive eye exam are visual acuity tests that measure the sharpness of your vision.
These are usually performed using a projected eye chart to measure your distance visual acuity and a small, hand-held acuity chart to measure your near vision.
OVERDUE FOR AN EYE EXAM? Find an optometrist near you. .
Colour vision test
A screening test that checks your colour vision is often performed early in a comprehensive eye exam to rule out colour vision defects.
In addition to detecting hereditary colour vision deficiencies, colour vision tests can also alert your optometrist to possible eye health problems that may affect your colour vision.
Cover test
While there are many ways for your optometrist to check how your eyes work together, the cover test is among the simplest and most common.
During a cover test, your optometrist will ask you to focus on a small object across the room and will then cover each of your eyes alternately while you stare at the target. The test is then repeated with you looking at a near object.
During these tests, your optometrist will assess whether the uncovered eye must move to pick up the fixation target, which could indicate strabismus or other problem that could cause eye strain or amblyopia ("lazy eye").
Ocular motility testing (eye movements)
Ocular motility testing is performed to determine how well your eyes can follow a moving object and/or quickly move between and accurately fixate on two separate targets.
Testing of smooth eye movements ("pursuits") is more common. Your optometrist will have you hold your head still and ask you to follow the slow movement of a hand-held light or other target with just your eyes.
If quick eye movements ("saccades") also are tested, your optometrist might have you move your eyes back and forth between two targets positioned some distance apart from each other.
Problems with eye movements can cause eye strain and may affect reading ability, sports vision and other skills.
Stereopsis test (Depth perception)
Stereopsis is the term used to describe eye teaming that enables normal depth perception or our ability to see objects in 3-dimensions (3D).
In one commonly used stereopsis test, you wear a pair of "3D" glasses and look at a booklet of test patterns. Each pattern has four small circles, and your task is to point out which circle in each pattern looks closer to you than the other three circles.
If you can correctly identify the "closer" circle in each pattern, you probably have excellent eye teaming skills that should enable you to experience normal depth perception.
Retinoscopy
Your optometrist may perform this test early in the eye exam to obtain an approximation of your glasses prescription.
In retinoscopy, the room lights will be dimmed and you will be asked to focus on a large target (usually the big "E" on the eye chart). As you stare at the "E," your optometrist will shine a light at your eye and change lenses in front of your eyes. This test estimates which lens powers will best correct your distance vision.
Based on the way the light reflects from your eye, your optometrist is able to estimate the power of glasses required to correct your vision.
This test is especially useful for children and patients who are unable to accurately answer the optometrist questions.
Refraction
This is the test that your optometrist uses to determine your exact glasses prescription.
During a refraction, the optometrist puts the instrument called a phoropter in front of your eyes and shows you a series of lens choices. He or she will then ask you which of the two lenses in each choice looks clearer.
Based on your answers, your optometrist will continue to fine-tune the lens power until reaching a final glasses prescription.
The refraction determines your level of hyperopia (long sightedness), myopia (short sightedness), astigmatism and presbyopia.
Autorefractors and aberrometers
Your optometrist may also use an autorefractor and / or aberrometer to automatically estimate your glasses prescription. With both devices, a chin rest stabilises your head while you look into the instrument at a pinpoint of light or a detailed image.
An autorefractor, like a manual refraction, determines the lens power required to accurately focus light on your retina. Autorefractors are especially helpful for determining a glasses prescription for young children and other patients who may have trouble sitting still, paying attention and providing feedback that the optometrist needs to perform an accurate manual refraction.
Studies have shown that modern autorefractors are very accurate. They also save time. The autorefraction takes only a few seconds, and the results greatly reduce the time required for your optometrist to perform a manual refraction and determine your glasses prescription.
An aberrometer uses advanced wavefront technology to detect even obscure vision errors based on the way light travels through your eye.
Aberrometers primarily are used for custom or wavefront LASIK vision correction procedures, but many optometrist are now incorporating this advanced technology into their routine eye exams as well.
Slit lamp exam
A slit lamp is a binocular microscope (or "biomicroscope") that your optometrist uses to examine the structures of your eye under high magnification. It looks somewhat like a large, upright version of a microscope used in a science lab.
During the slit lamp exam, you will be asked to place your forehead and chin securely against the rests on the front of the instrument and your optometrist will begin by examining the structures of the front of your eyes — including your eyelids, cornea, conjunctiva, iris, and lens.
With the help of a hand-held lens, your optometrist may also use the slit lamp to examine structures located further back in the eye, such as the retina and optic nerve.
A wide range of eye conditions and diseases can be detected with the slit lamp exam, including cataracts, macular degeneration, corneal ulcers and diabetic retinopathy, etc.
"The glaucoma test"
Testing for glaucoma typically begins with measuring the pressure inside your eyes.
A common glaucoma test is the "puff-of-air" test, technically known as non-contact tonometry, or NCT.
For NCT, the test begins with you putting your chin on the machine's chin rest. While you look at a light inside the machine, the optometrist or a trained assistant will puff a small burst of air at your open eye. It is completely painless, and the tonometer does not touch your eye.
Based on your eye's resistance to the puff of air, the machine calculates your intraocular pressure (IOP). If you have high eye pressure, you may be at risk for or have glaucoma.
Another type of glaucoma test is performed with an instrument called an applanation tonometer. The most common of several versions of this instrument is mounted on the slit lamp.
For this test, your optometrist will put yellow fluroescein and anaesthetic drops in your eye to numb it. Your eyes will feel slightly heavy when the drops start working. This is not a dilating drop — it is a numbing agent combined with a yellow dye that glows under a blue light.
Then the optometrist will have you stare straight ahead into the slit lamp while he or she gently touches the surface of your eye with the tonometer to measure your IOP.
Like NCT, applanation tonometry is painless and takes only a few seconds. At most, you may feel the tonometer probe tickle your eyelashes.
You typically have no warning signs of glaucoma until you already have significant vision loss. For this reason, routine eye exams that include tonometry are essential to rule out early signs of glaucoma and protect your eyesight.
Pupil dilation
To obtain a better view of the eye's internal structures, your optometrist instills dilating drops to enlarge your pupils. Dilating drops usually take about 20 to 30 minutes to start working.
When your pupils are dilated, you will be sensitive to light (because more light is getting into your eye) and you may notice difficulty focusing on objects up close. These effects can last for up to several hours, depending on the strength of the drop used.
Once the drops have taken effect, your optometrist will use various instruments to look inside your eyes. You should bring sunglasses with you to your eye exam, to minimise glare and light sensitivity on the way home.
Pupil dilation is very important for people with risk factors for eye disease, because it allows for the most thorough evaluation of the health of the inside of your eyes.
Visual field test
In some cases, your optometrist may want to check for the possible presence of blind spots (scotomas) in your peripheral or "side" vision by performing a visual field test. These types of blind spots can originate from eye diseases such as glaucoma.
Analysis of blind spots may also help identify specific areas of brain damage caused by a stroke or tumour.
Other eye tests
In some cases, besides these common tests performed during a comprehensive eye examination, your optometrist may recommend other, more specialised eye tests. SOme of these tests may be performed by other eye care professionals, such as retinal specialists, on a referral basis.
About contact lens fittings
It's important to understand that a comprehensive eye test typically does not include a contact lens fitting, and therefore you will not be given a contact lens prescription at the end of a routine eye examination.
There is a possible exception: If you wear contacts currently and the lenses were fitted by the same optometrist who is performing your comprehensive eye exam, he or she may issue you an updated contact lens prescription at the end of your eye exam.
A contact lens exam that includes fitting services typically is done during a subsequent practice visit, when your pupils are not dilated.
Generally, it's better to have your eye test and your contact lens exam performed at the same practice.
Often, if you have these examinations performed at different locations, the optometrist conducting your contact lens fitting will want to repeat certain tests already performed at your comprehensive eye test. In part, this is done for liability reasons — to verify the accuracy of your glasses prescription and make sure your eyes are healthy enough to wear contacts.
This duplication of effort often will result in additional costs that you would not experience if your eye test and contact lens examination were performed at the same location.
[Note: Although a glasses prescription cannot be used to purchase contact lenses, the power of your glasses prescription gives your optometrist a starting point for determining the power of your contact lenses.
If you need or want to go elsewhere for your contact lens examination after having a comprehensive eye test, be sure to ask if additional fees will be required to repeat testing already performed.
ISN'T IT TIME YOU GET YOUR EYES CHECKED? Find an optometrist near you.
Page published on Tuesday, 17 March 2020






