Treatment for pink eye
Diagnosis
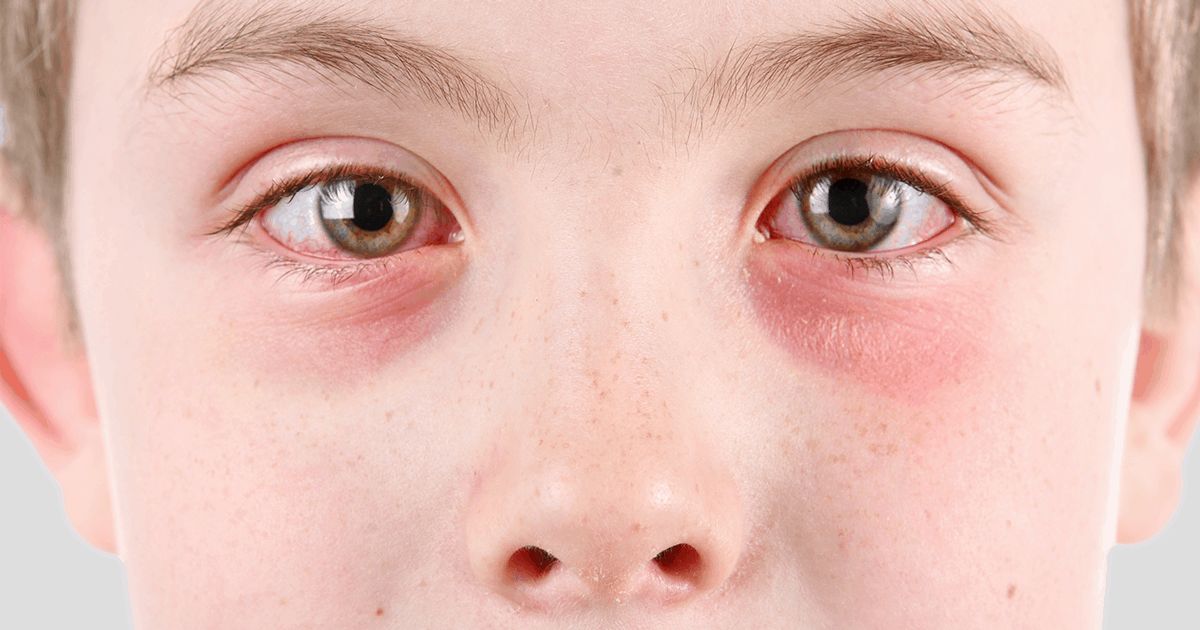
Usually, you will only need a formal diagnosis for pink eye (conjunctivitis) if it’s caused by a bacterial infection. Most types of pink eye will clear up on their own, but bacterial forms may require antibiotics. However, it is difficult to tell the difference between types of pink eye at home.
This is because every type has very similar symptoms. Conjunctivitis can be caused by viruses, bacteria, and allergies, as well as by other irritants that may enter the eyes. The viral and bacterial types of conjunctivitis are extremely contagious. And while the viral types are mostly harmless, some bacterial types can cause serious complications if left untreated.
Even though most cases of pink eye resolve without treatment, it’s often worth it to visit your eye doctor anyway. They can prescribe medications to help shorten the length and severity of your symptoms.
When to seek medical care
It’s important to see an eye doctor if your symptoms don’t start to improve within a week or so. This could indicate that you have a more serious type of viral or bacterial infection. Moreover, there are many other eye conditions with symptoms that look just like pink eye. You should see an eye doctor right away if:
Symptoms aren't improving after a few days
Symptoms start to get worse
Vision is affected
White part of the eye is extremely red (rather than pinkish-red)
Eyes are very painful (rather than mild stinging or soreness)
Symptoms spread to the other eye or other family members
For contagious pink eye (caused by bacterial or viral infections), you may need a doctor’s confirmation that it’s okay to return to school or work.
LEARN MORE: Signs and symptoms of pink eye
Pink eye treatment at home
Home treatment for conjunctivitis can help to relieve symptoms, but it can't cure it or shorten its duration. Most cases of pink eye simply have to run their courses.

Many people find that using cool or cold compresses can calm burning and stinging eyes. Warm compresses can be a comfortable, safe way to clear the eyes of mucous discharge. When using compresses, be careful not to spread the infection from one eye to the other.
For inflammation and redness, over-the-counter artificial tears and pain relievers (like ibuprofen) can be helpful. And though it seems counterintuitive, do not use redness-relief eye drops. They can cause more irritation and redness in the long run.
It's also best to not wear contact lenses as long as you have symptoms. If you must wear contacts, always throw them away after each use.
If you think you or your child has conjunctivitis, don’t try any other home treatments yourself. And never use any "natural remedies" for pink eye without first consulting an eye care professional.
LEARN MORE: Conjunctivitis in children
Pink eye treatment
When it comes to treatment for pink eye, it will almost certainly involve eye drops. The eye drops used for pink eye may be prescription, over-the-counter or a combination of both.
Most cases will resolve on their own without treatment. However, it’s possible that you may need a prescription from your doctor, depending on the cause. An eye doctor can tell you which type you actually have. Plus, this can help you determine the best way to soothe your pink eye symptoms until they clear up.
Viral conjunctivitis
Because this highly contagious form of pink eye is caused by a virus, there is no medical cure for it. Just like with the common cold, viral conjunctivitis treatment focuses on treating the symptoms, not the condition itself. In fact, sometimes this form of conjunctivitis is called an “eye cold.” It typically lasts between one and three weeks.
The best options for treating viral pink eye symptoms are some of the same home treatments mentioned earlier. Cool compresses and over-the-counter lubricating eye drops can help reduce irritation. Non-prescription pain relievers can also help with discomfort and swelling.
For cases caused by more serious types of viruses, your eye doctor may choose to prescribe steroid eye drops or antiviral medication.
Bacterial conjunctivitis
Bacterial conjunctivitis treatment usually comes in the form of antibiotics. They help to reduce recovery time and the chances of any potential complications. However, bacterial pink eye can often clear up on its own, so antibiotics aren’t always strictly necessary.
Your eye doctor will be able to tell you the best course of treatment for your bacterial infection. If they do recommend medical treatment, it is often antibiotic eye drops or ointments. In some cases, they may also prescribe an oral antibiotic.
You can also take advantage of home treatments to relieve your symptoms while the antibiotics do their job. Warm compresses, artificial tears and OTC anti-inflammatory medications are best for bacterial infections.
Allergic conjunctivitis
Like with the viral form, allergic conjunctivitis treatment focuses on easing uncomfortable symptoms. These symptoms may appear suddenly, seasonally or year-round, depending on which allergens are causing them.
Being proactive by taking oral allergy medication regularly and avoiding known allergens can go a long way in preventing allergic conjunctivitis. For those who can’t avoid their known allergens, antihistamine eye drops can help to relieve some of the itchiness and irritation. Cool compresses can also help you feel more comfortable.
In severe or chronic cases, your eye doctor may prescribe steroid eye drops. These can help speed up recovery but can also cause some unwanted side effects if used long-term.
SEE RELATED: Eye allergies vs. pink eye: What’s the difference?
Treating other forms of conjunctivitis
Most cases of conjunctivitis are caused by very common viruses, bacteria or allergens. But other factors can cause it too, and each cause has its own method of treatment.
Less common but more serious causes include bacterial sexually transmitted diseases (STDs). Herpes viruses can also cause more serious forms of conjunctivitis. It can also be caused by anything that really irritates the eyes. Irritants related to this type range from chlorine in swimming pools to a foreign object in the eye.
Neonatal conjunctivitis (pink eye in newborns) can be caused by STDs like chlamydia and gonorrhea. These infections are passed along from mother to baby in the birth canal. Chlamydial conjunctivitis in newborns is typically treated with oral antibiotics. The gonococcal form in newborns is typically treated with IV antibiotics.
Giant papillary conjunctivitis (GPC) is caused by an abnormal immune response to a foreign body in the eye. It occurs most often in people who wear soft contact lenses. The typical treatment for contact lens-related GPC is to stop wearing the lenses for at least a month. Afterward, switching to daily disposable contact lenses is key.
Daily disposables help ensure that patients cleanse and replace their contacts every day. For severe cases, mast cell stabilizers are sometimes prescribed.
Toxic conjunctivitis is usually caused by prescription eye drops that contain preservatives. It’s most common with prolonged use but can also occur after just the first or second use in some people.
The primary treatment for toxic conjunctivitis is to stop using the eye drops. Patients will need to switch to another type of drops once the condition clears up.
Irritant conjunctivitis can develop when anything bothersome gets in or near the eyes. The treatment for this type is to thoroughly rinse the eyes as soon as possible. Remove contact lenses (if worn) and do not rub the eyes.
It's best to use artificial tears or sterile saline solution to flush out the irritant. Tap water can also be used in emergencies. If any harsh chemical splashes into your eyes, flush it out and seek medical care immediately.
How long does pink eye last with treatment?
Around 80% of all cases of pink eye are caused by viruses. This means that most cases won’t respond to any medical treatment. However, viral pink eye tends to run its course in 1-3 weeks. Bacterial cases tend to last 1-2 weeks without treatment. With antibiotic treatment, they can begin to resolve in 3-4 days.
Special considerations for treating pink eye in kids or babies
The one main difference in treating babies is when to see the doctor. It’s important to take newborns in for an exam at the first sign of eye infection, rather than waiting a day or two to see if it starts to clear up. Newborns may require intravenous antibiotics.
Other than that, pink eye treatment for kids and babies is the same as for adults. Bacterial infections may be treated with antibiotic eye drops or ointment, and viral infections just need time to resolve on their own.
The same home treatments recommended above are also good for children—but never treat infants under 6 months old with ibuprofen.
Types of doctors who can treat pink eye
Optometrists, ophthalmologists and primary care physicians can all diagnose and treat pink eye. However, eye doctors have more in-depth knowledge of the conjunctiva and are better able to distinguish between types of conjunctivitis.
For example, eye care professionals are less likely to prescribe unnecessary antibiotics for viral pink eye. And they're more equipped to make an accurate diagnosis if you have a different type of eye infection. If your symptoms include eye pain, vision changes or sensitivity to light, you should see an eye doctor right away.
LOOKING FOR AN EYE DOCTOR? Find a great eye care professional near you with our comprehensive ECP locator.
Diagnosing pink eye (conjunctivitis). Centers for Disease Control and Prevention. January 2019.
Treatment for pink eye. National Eye Institute. June 2019.
Treating pink eye (conjunctivitis). Centers for Disease Control and Prevention. January 2019.
Quick home remedies for pink eye. American Academy of Ophthalmology. EyeSmart. September 2021.
Home remedies for pink eye relief. Cleveland Clinic. September 2022.
First aid: Pinkeye. Nemours KidsHealth. July 2022.
Pink eye (conjunctivitis). Cleveland Clinic. August 2022.
Redness-relieving eye drops. American Academy of Ophthalmology. EyeSmart. April 2021.
What are eye allergies? American Academy of Ophthalmology. EyeSmart. January 2022.
Conjunctivitis: What is pink eye? American Academy of Ophthalmology. EyeSmart. April 2022.
Conjunctivitis information for clinicians. Centers for Disease Control and Prevention. August 2021.
Causes of pink eye (conjunctivitis). Centers for Disease Control and Prevention. January 2019.
Conjunctivitis (pink eye) in newborns. Centers for Disease Control and Prevention. January 2019.
Giant papillary conjunctivitis. American Academy of Ophthalmology. Accessed August 2022.
Toxic conjunctivitis. UpToDate. February 2021.
Toxic conjunctivitis - External and internal eye. VisualDx. August 2021.
Ocular surface disease in patients with glaucoma. American Academy of Ophthalmology. EyeWiki. April 2022.
How to safely flush out your eye. Cleveland Clinic. Health Essentials. June 2022.
Medication for conjunctivitis. NYU Langone Health. Accessed September 2022.
Conjunctivitis (pink eye). American Optometric Association. Accessed September 2022.
Pinkeye (conjunctivitis). Nemours KidsHealth. November 2020.
Page published on Monday, 16 March 2020
Page updated on Tuesday, 22 August 2023
Medically reviewed on Wednesday, 21 September 2022






