Corneal abrasion: Treatment of a scratched eye
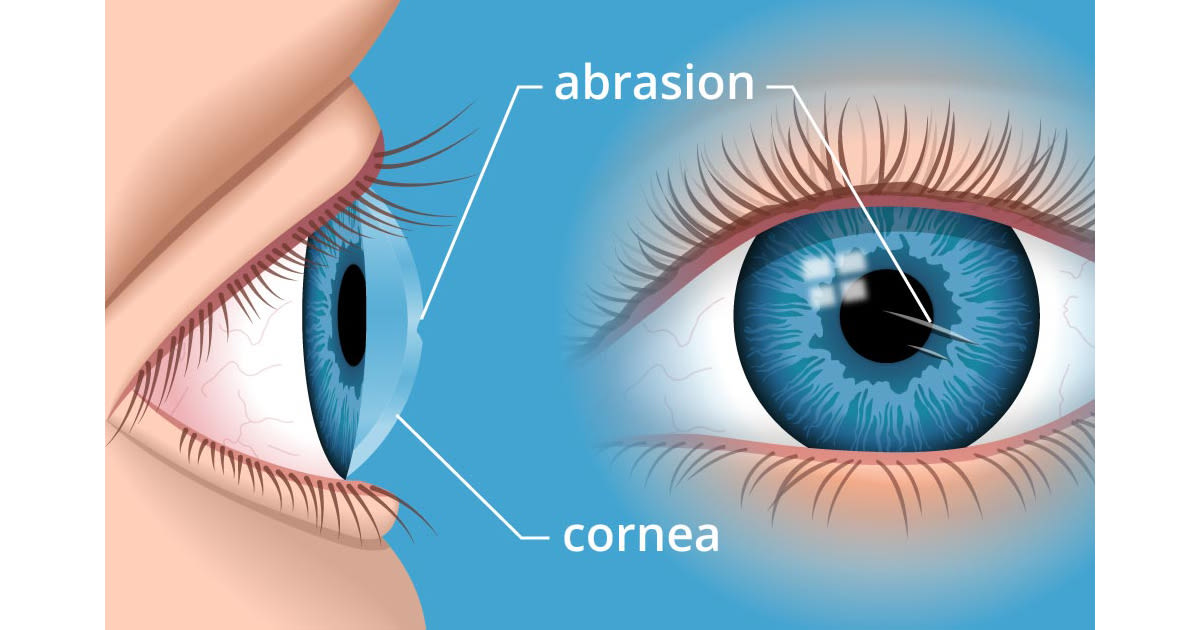
A corneal abrasion is a scratch on the clear front surface of the eye (the cornea). Corneal abrasions typically cause significant discomfort, red eyes, watery eyes and sensitivity to light.
In addition to being painful, a scratched cornea makes your eye more susceptible to infection, so it's important that you see your optometrist or visit the Emergency Department in hospital as soon as possible if you suspect you have a corneal abrasion.
What causes corneal abrasions?
Virtually any object that comes in direct contact with the front surface of you eye has the potential to cause a corneal abrasion.
Tree branches, paper, makeup brushes, a pet, a finger, workplace debris, sports equipment and more all pose a danger to the front surface of your eyes.
Many corneal abrasions aren't caused by a noticeable traumatic event, such as getting poked in the eye. Sand, dust and other small particles can often cause a corneal abrasion as well, especially if you rub your eyes.
Dry eyes increase your risk of a corneal abrasion, particularly when awakening from sleep. If your eyes dry out while you are sleeping, your eyelids may stick to your cornea. When you wake up and open your eyes, your eyelids rubbing across the dry surface of your eye can cause a corneal abrasion.
Poor fitting, damaged or dirty contact lenses also can cause a scratched cornea, so can wearing your contacts too long or while you are sleeping.
Symptoms of a scratched eye
The cornea is one of the most sensitive parts of your body, with millions of nerve ending in every square millimetre. Even a very small corneal abrasion can be extremely painful and feel much larger in size — as if you have a big, rough object in your eye.
In addition to pain and a gritty sensation, other signs and symptoms of a corneal abrasion include:
Redness
Watery eyes
Sensitivity to light
Headache
Blurry vision
Sometimes, a corneal abrasion can be so uncomfortable that it causes nausea.
If you think you may have suffered a corneal abrasion and are experiencing any of these symptoms, see an optometrist right away.
Preventing a scratched cornea
People have a tendency to rub their eyes when they feel like something is "in" them, but this can make matters much worse.
If you get something in your eye, you can attempt to flush it out with water, but don't rub your eye.

A cornea abrasion usually affects just one eye, and it can feel like something is on or in your scratched eye.
Also, don't cover your eye with a patch. This can speed bacterial growth and increase the risk of an eye infection.
If possible, rinse your eye with a sterile saline eye wash or a multipurpose contact lens solution avoid tap water or bottled water. Microorganisms such as Acanthamoeba have been found in tap water and even bottled water, and these pathogens can cause a serious, vision-threatening infection if introduced to an eye with a scratched cornea.
After flushing the eye, if redness, pain or foreign body sensation continues, seek immediate attention because corneal abrasions can cause serious harm in as little as 24 hours.
To diagnose a corneal abrasion, your optometrist may apply an eye drop to numb your eye so you can keep it open for the examination, plus another type of drop to help your them see the extent of the abrasion when viewing your eye with a blue light and an examining microscope called a slit lamp.
Depending on what may have caused the scratch and what your optometrist sees during the exam, your eye might be gently swabbed for a culture to ensure proper treatment in the event of infection.
Treatments for a scratched eye
Treatment for a corneal abrasion depends on the severity of the wound and the cause. Minor abrasions sometimes can be treated with non-preserved lubricating drops to keep your eye moist and comfortable while your eye's natural healing process takes place.
As a precaution, even superficial abrasions sometimes are also treated with antibiotic eye drops to prevent infection during healing. Superficial corneal abrasions tend to heal quickly, usually within two or three days.
Other corneal abrasions may require an antibiotic ointment that stays on the eye longer, a steroid to decrease inflammation and scarring, and something to relieve pain and light sensitivity. Large, deep corneal abrasions take longer to heal and can cause a permanent scar that might affect vision.
In some cases, scratched corneas are treated with what's known as a bandage contact lens. When used with prescription eye drops, these special lenses provide pain relief and sometimes can speed healing.
Typically, regular contact lenses should not when a corneal abrasion is present because of the increased risk of an infection developing under the lens. Your optometrist will tell you when it's safe to resume wearing your contacts following a scratched cornea.
Depending on the treatment and severity of the injury, your optometrist or ophthalmologist may schedule a follow-up visit as soon as 24 hours after initial treatment.
When treated right away, most corneal abrasions result in a full recovery with no permanent vision loss but some deeper abrasions that occur in the centre of the cornea, (directly in front of the pupil), can leave a scar and result in a loss of visual acuity.
If left untreated, some deep corneal abrasions can lead to a corneal ulcer that can cause severe vision loss. Abrasions caused by organic matter, (plants, dirt etc.) in particular, can increase the risk of corneal ulceration.
Attending your follow-up appointments is very important, because corneal abrasions don't always heal properly and can lead to recurrent corneal erosions and other complications that can affect your vision and comfort.
How to prevent a corneal abrasion
Although many causes of corneal abrasions are difficult to prevent, others can be avoided by taking some simple, common-sense precautions.
For example, always wear safety glasses or protective goggles in work environments with airborne debris, particularly in welding environments. Likewise, protective eye-wear should be used when working in the garden, using power tools or playing sports.
If you wear contact lenses, always follow your optometrist's instructions regarding how long to wear them, when to discard them, and the proper contact lens care solutions to use to help keep your corneas healthy and strong.
If you experience a corneal abrasion that appears to be related to dry eyes, see your optometrist and follow the dry eye treatment protocol they recommend.
Page published on Monday, 16 March 2020






