Eye infections: Types, symptoms and treatment
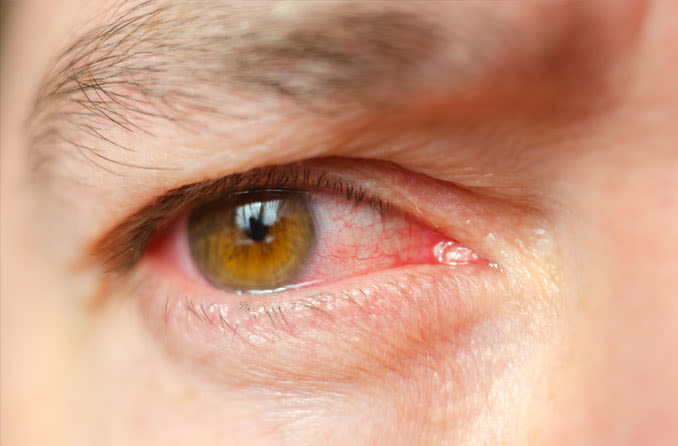
Eye infections occur when harmful microorganisms — bacteria, fungi and viruses — invade any part of the eyeball or surrounding tissues, including the clear front surface of the eye (cornea) and the thin membrane covering the outer eye and inner eyelids (conjunctiva).
Eye infection symptoms
Common symptoms of eye infections include:
Pain
Watery eyes
Swelling around the eyes
Itching
Blurry vision
Anytime you suspect an eye infection, you should always visit your optometrist for a consultation. Trying to self-diagnose your condition can delay effective treatment and potentially cause permanent vision loss.
If you wear contact lenses, you should wear only your glasses until you have visited your optometrist or GP for diagnosis and treatment.
There are many different types of eye infections, and your optometrist or GP needs to determine the particular type of eye infection you have in order to prescribe the proper treatment.
Your optometrist or GP may take a sample from the affected area of your eye for a culture to assess the exact type of infection you have, if any. This may help determine the most effective treatment, such as an antibiotic that selectively targets the type of bacteria causing the infection.
Types of eye infections
Examples of viral, fungal and bacterial eye infections include:
Conjunctivitis
Conjunctivitis, is a common, highly contagious eye infection that often is spread among children in nursery, classrooms and similar environments. Teachers and child-care workers also are at increased risk of conjunctivitis when they work in close quarters with young children.
Common infectious conjunctivitis types often have viral or bacterial origins. If their mother has a sexually transmitted disease, infants can acquire conjunctival eye infections (gonococcal and chlamydial conjunctivitis) during birth .
Other viral eye infections (viral keratitis)
Besides common conjunctivitis, other viral eye infections include ocular herpes, which occurs with exposure to the Herpes simplex virus. If you suffer from 'cold sores' it is extremely important to wash your hands immediately after touching or treating as sore and never use another person's towel.
Fungal keratitis
This type of eye infection made worldwide news in 2006 when a contact lens solution now withdrawn from the market was linked to an outbreak among contact lens wearers.
The fungal eye infection was associated with Fusarium fungi, commonly found in organic matter. This and other fungi can invade the eye in other ways, such as through a penetrating injury caused by e.g. a twig from a tree.
Acanthamoeba keratitis
Contact lens wearers are at increased risk of encountering parasites that can invade the eye and cause a serious sight-threatening infection called Acanthamoeba keratitis. This is why contact lens wearers should observe certain safety tips, such as avoiding swimming while wearing contacts.
If you do wear contact lenses when swimming or relaxing in a spa bath, make sure you remove and disinfect your lenses immediately afterwards.
Indeed, there is an increased risk of fungal and bacterial eye infections among contact lens wearers in general, and proper contact lens care must be followed.
Trachoma
A serious eye infection known as trachoma, related to Chlamydia trachomatis, is a leading cause of blindness in certain parts of the world, it was common among aboriginal populations. The infection is spread by flies in unsanitary environments and reinfection is a common problem.
Trachoma typically infects the inner eyelid, which begins to scar. Scarring then causes entropian (an "in-turning" of the eyelid), and eyelashes begin to brush against and destroy tissue on the cornea, with resulting permanent blindness. Good hygiene and availability of treatments such as oral antibiotics are essential to controlling trachoma.
Endophthalmitis
Usually caused by bacteria, endophthalmitis is a serious infection of the interior of the eye. The most common cause of endophthalmitis is a penetrating eye injury. It also can occur as a rare complication of eye surgery such as cataract surgery.
Prompt medical treatment with potent antibiotics is required to prevent serious vision loss or even blindness from endophthalmitis.
Eye infection complications
An infection also can affect interior portions of the upper and lower eyelids to create a stye or chalazion. Rubbing or “popping” a stye should be avoided, as this can cause a deeper, more serious infection called orbital cellulitis.
Orbital cellulitis is a serious infection of the tissues around the eyeball. It is a medical emergency which, if not promptly treated, can cause blindness, meningitis and even death.
Infection also can lead to inflammation and blockage of the eye's tear drainage system and cause dacryocystitis.
Infection also can be an underlying cause of a corneal ulcer, which resembles an abscess on the eye. If left untreated, a corneal ulcer can lead to severe vision loss.
Eye infection treatments
Fortunately, most common bacterial eye infections can be effectively treated with prescription antibiotic eye drops or ointments and compresses.
Many common viral eye infections resolve on their own. In cases of severe viral eye infections, an antiviral eye drop may be prescribed. Some viral eye infections require careful administration of steroid eye drops to reduce related inflammation.
Depending on the underlying cause of your eye infection, your doctor may need to prescribe antibiotics or antiviral medications that are taken orally. If your symptoms worsen or change, contact your optometrist or GP immediately.
How to prevent eye infections

Prevent eye infections by washing your hands before touching your eyes or eyelids and before handling contact lenses.
If you are near a person with a red eye, do not touch your own eyes until you wash your hands first.
You also can minimise the likelihood of catching common bacterial or viral eye infections by avoiding rubbing your eyes, washing your hands frequently throughout the day (especially before applying and removing contact lenses), washing towels and bed linen often, and using anti-bacterial cleaning products on bench tops and other common areas.
Page published on Monday, 16 March 2020






