Dry eye syndrome: 12 ways to get relief

Dry eye syndrome is a chronic and typically progressive condition. Depending on its cause and severity, it may not be completely curable.
But in most cases, dry eyes can be managed successfully, usually resulting in noticeably greater eye comfort, fewer dry eye symptoms, and sometimes sharper vision.
Dry eye disease can have a number of causes, and a variety of treatment approaches are used.
The following is a list of dry eye treatments that are commonly used to reduce the signs and symptoms of dry eyes. Your optician may recommend only one of these dry eye treatments or a combination of treatments, depending on the cause(s) and severity of your condition.
Also, some optometrists and ophthalmologists will have you complete a questionnaire about your symptoms prior to initiating dry eye treatment. Your answers to this survey are then used as a baseline, and the questionnaire may be administered again after several weeks of treatment to evaluate the effectiveness of the chosen treatment approach.
Successful treatment of dry eyes requires that you are willing to follow your opticians recommendations and that you use the products he or she recommends consistently and as frequently as directed.
NEED AN EYE EXAM? Find a dry eye specialist near you and make an appointment.
1. Artificial tears
For mild cases of dry eyes caused by computer use, reading, schoolwork and other situational causes, the best dry eye treatment may simply be frequent use of artificial tears or other lubricating eye drops.
Artificial tears usually are the first step in dry eye treatment.
There are many brands of artificial tears that are available without a prescription. The challenge with using artificial tears is not lack of product availability — it's the confusing number of brands and formulations available to choose from.
Artificial tears and other over-the-counter (OTC) lubricating eye drops are available in a wide variety of ingredients and viscosity ("thickness").
Artificial tears with low viscosity are "thin" and watery. They often provide quick relief with little or no blurring of your vision when you apply them. But often their soothing effect is very short-lived, and sometimes you must use these drops very frequently to get adequate dry eye relief.
On the other hand, artificial tears that have a high viscosity are more gel-like and can provide longer-lasting lubrication. But typically these drops cause significant blurring of your vision for several minutes immediately after you apply them. For this reason, these drops often are not a good choice for use during your work day or when you need immediate clear vision for tasks such as driving. Sometimes high-viscosity artificial tears are recommended for bedtime use only.
Also, the ingredients in certain brands of artificial tears may determine which type of dry eye condition they are better suited for. For example, one brand might work better if you don't produce enough natural tears (aqueous-deficiency dry eye) while another brand may be more effective if your natural tears evaporate too quickly (evaporative dry eye).
It is important for you to try different combinations of drops and treatments to determine which ones work best for you and your lifestyle. Your optometerist can help you determine which drops will be most appropriate for different symptoms.
2. Cyclosporine
Instead of artificial tears (or in addition to them), your ophthalmologist might recommend daily use of a prescription eye drop called Cyclosporine for your dry eye treatment.
Cyclosporine does more than simply lubricate the surface of your eye. It includes an agent that reduces inflammation associated with dry eye syndrome and helps your body produce more natural tears to keep your eyes moist, comfortable and healthy.
It's important to know, however, that the therapeutic effect is not immediate. You must use the drops daily for a minimum of 90 days to experience the full benefits of this dry eye treatment.
Some people who try Cyclosporine will experience burning eyes early during the first few weeks of treatment.
3. Steroid eye drops
Over the past several years, inflammation has been recognized as a significant cause of dry eyes. Inflammation frequently causes the redness and burning associated with dry eye disease.
Artificial tears usually do not adequately address these inflammatory changes, and your doctor may recommend steroid eye drops to better manage the underlying inflammation associated with dry eyes.
Steroid eye drops generally are used short-term to quickly manage symptoms. They often are used in conjunction with artificial tears or Cyclosporine, as a complement to these more long-term dry eye treatment strategies.
Steroid eye drops (especially if used for relatively long periods) have the potential of causing side effects. So, it's important to make your optician aware of your full medical history before starting steroid eye drops.
For example, steroid eye drops can increase the risk of developing high eye pressure or even cataracts if used for extended periods of time. But these risks are low when the drops are used only on a short-term basis for dry eye treatment.
SEE ALSO: How to Use Eye Drops Without Spilling Them All Over Your Face!
4. Lacrisert
Lacrisert (Bausch + Lomb) is a sterile, slow-release lubricant that is placed under the lower eye lid where the conjunctiva of the inside of the eyelid meets the conjunctiva of the eyeball.
It is a solid insert composed of a preservative-free lubricating agent (hydroxypropyl cellulose) that slowly liquefies over time, providing an all-day moistening effect.
For most people with dry eyes, a single Lacrisert is applied once a day. The device has been proven to relieve dryness, burning, watery eyes, foreign body sensation, itching, light sensitivity and blurred vision, according to the company.
Lacrisert typically is recommended for patients with moderate to severe dry eye symptoms, especially if dry eye treatment with artificial tears alone proves unsuccessful.
If placed under the eyelid improperly, it's possible Lacrisert can cause a corneal abrasion. Also, Lacrisert may cause transient blurred vision, eye discomfort or irritation, matting or stickiness of eyelashes, red eyes and sensitivity to light.
5. Punctal plugs
Punctal plugs sometimes are used in dry eye treatment to help tears remain on the surface of the eye longer.
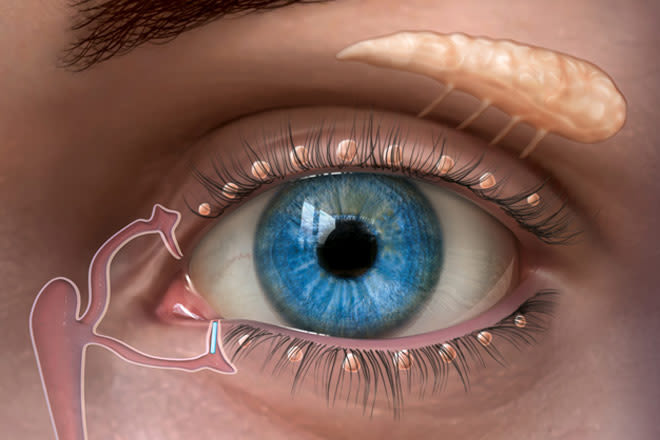
This drawing shows the lacrimal glands and tear ducts. A lacrimal plug (or punctal plug) has been inserted into the lower tear duct to keep the eye's moisture from draining away too quickly. Image: Oasis Medical, Inc.
A punctal plug is a small, sterile device that is inserted into one of the small openings (puncta) of tear drainage ducts that are located in the inner corner of the upper and lower eyelids.
After these openings have been plugged, tears can no longer drain away from the eye through these ducts. This results in the tear film remaining intact longer on the surface of the eye, relieving dry eye symptoms.
So where do the tears go? Usually they will simply evaporate from the eye surface without symptoms. But if insertion of punctal plugs causes watery eyes, one or more of the plugs can be removed.
6. Meibomian gland expression
A very significant percentage of dry eye cases are caused by inadequate oil (meibum) being secreted from meibomian glands located along the margin of the eyelids.
The openings of these glands are near the base of the eyelashes. If these openings get clogged, the oil that's critical to keeping the tear film from evaporating too quickly cannot do its job. This is called meibomian gland dysfunction (MGD), which is a significant cause of evaporative dry eye symptoms.
To treat MGD and evaporative dry eye, your eye doctor may perform an in-office procedure called meibomian gland expression. In this procedure, warm compresses may or may not first be applied to your eyelids; then a forceps-type device is used to squeeze the clogged contents (hardened meibum and possibly other substances) from the meibomian glands.
To fully express the contents of the meibomian glands and get them functioning properly, significant pressure must be applied to the eyelids, which can be uncomfortable. But the results usually make any short-term discomfort from the procedure worth it.
7. Warm compresses
An alternative (and potentially more comfortable) way to help open clogged meibomian glands to treat dry eyes is to simply apply warm compresses to the closed eyelids to soften the hardened meibum.
A warm flannel or a specially developed EyeBag which is heated in the microwave, is applied to your eyes for a few minutes. This is then followed by massaging your eyelids to help flow of the oil within the meibomian glands. If performed regularly this can help soothe the feelings of discomfort.
8. LipiFlow
The LipiFlow Thermal Pulsation System (TearScience) is an automated dry eye treatment that combines the best features of warm compress therapy and meibomian gland expression.
Watch a video about how LipiFlow works.
The patented device fits over the eyelids and applies precisely-controlled heat to the lids to soften hardened meibum trapped in the meibomian glands. At the same time, the LipiFlow system applies pulsed pressure to the eyelids to open and express the clogged glands, thereby restoring the correct balance of oils in the tear film to relieve dry eye syndrome.
Lipiflow treatment takes approximately 12 minutes per eye. In a clinical study of the effectiveness of the procedure, 76% of patients reported improvement of their dry eye symptoms within two weeks of treatment. Most patients also showed improvement in the quality and quantity of meibomian gland secretions and the duration of time their tear film remained on the eye before evaporating.
In some cases, however, it can take a few months for improvements from the LipiFlow procedure to become apparent.
Typically, the beneficial effects of the LipiFlow procedure last one to three years or longer.
Potential side effects from LipiFlow dry eye treatment include corneal abrasion, eye pain, swollen eyelids, eyelid irritation or inflammation, chalazion, transient blurred vision, itching, and red eyes.
LipiFlow dry eye treatment typically is not covered by health insurance. Fees for the procedure can vary from one practitioner to another.
9. Intense pulsed light
For well over a decade, doctors have used intense pulsed light (IPL) to treat rosacea on the skin. Rosacea on the skin and eyelid often occur together.
Ocular rosacea is characterised by dilated blood vessels coursing along the eyelash margin in patients suffering from blepharitis and may contribute to dry eye symptoms.
In IPL treatment, a hand-held device flashes bright light onto the skin. The light is filtered to allow only wavelengths that can be absorbed by the dilated blood vessels. The effect of this treatment may be the resolution of the dilated vessels and associated inflammation that contributes to dry eye symptoms.
Many patients experience relief from their dry eye symptoms after IPL and become less dependent on artificial tears and other routine measures to keep their eyes comfortable. For this reason, IPL treatment may be well-suited for dry eye patients who don't want to be troubled by the inconvenience of frequent eye drop use.
Patients usually require four to six monthly IPL treatments for optimum effects. Typically, the treatments are well-tolerated and are not associated with any down-time. However, it's important to discuss with your doctor how much time you spend in the sun, as the treatments will make your eyelids more light-sensitive.
IPL treatment generally is not covered by health insurance and it may not be appropriate for patients with certain skin pigmentations.
10. Nutritional supplements
Doctors sometimes recommend nutritional supplements as part of a holistic dry eye treatment plan.
Studies have found that supplements containing omega-3 fatty acids can decrease dry eye symptoms. Good sources of omega-3s include cold-water fish such as salmon, sardines, herring and cod. For a vegetarian source of omega-3s, some eye doctors recommend flaxseed oil to relieve dry eye.
Also, simply drinking more water might help relieve dry eye symptoms. Mild dehydration often makes dry eye problems worse. This is especially true during hot, dry and windy weather.
11. Home remedies for dry eyes
If you have mild dry eye symptoms, there are several things you can try to get relief before going to the opticians:
Blink more frequently. Research has shown that people tend to blink much less frequently than normal when viewing a computer, smartphone or other digital display. This decreased blink rate can cause or worsen dry eye symptoms. Make a conscious effort to blink more often when using these devices. Also, perform full blinks — gently squeezing your eyelids together — to fully spread a fresh layer of tears over your eyes.

Wraparound-style eyewear with side shields can protect your eyes from moisture-robbing wind and irritating debris. Shown here are Churada sunglasses with removable foam eyecups and Nereus eyewear with removable silicone eyecups.
Take frequent breaks during computer use. A good rule of thumb here is to look away from your screen at least every 20 minutes and look at something that is at least 20 feet from your eyes for at least 20 seconds. Eye doctors call this the "20-20-20 rule," and abiding by it can help relieve dry eyes and computer eye strain.
Thoroughly remove eye makeup. Eyeliner and other eye makeup can clog the openings of the meibomian glands at the base of the eyelashes, leading to meibomian gland dysfunction and evaporative dry eye. At the end of the day, be diligent about removing all traces of makeup from your lids and lashes.
Clean your eyelids. When washing your face before bedtime, gently wash your eyelids to remove bacteria that can cause blepharitis and meibomian gland problems that lead to dry eye symptoms. Apply a warm, moist washcloth to your closed lids for at least 20 seconds. Then gently wash your lids and lashes with a mild cleanser, such as diluted baby shampoo or pre-moistened eyelid wipes sold in drugstores.
Wear quality sunglasses. When outdoors in daylight hours, always wear sunglasses that block 100% of the sun's UV rays. For the best protection, choose sunglasses that also feature a wrap-style frame to protect your eyes from wind, dust and other irritants that can cause or worsen dry eye symptoms.
Other dry eye treatment considerations
In addition to the dry eye treatments listed above, your optician may recommend one or more of the following supplemental measures if any of the conditions below apply to you:
Medication adjustment. Many medicines — including antihistamines, antidepressants, birth control pills, certain blood pressure medications and more — can cause or worsen dry eye symptoms. Even over-the-counter (nonprescription) medications for allergies and other conditions can cause dry eyes.
Be sure to discuss all medications you are taking with your eye doctor if you are experiencing dry eye problems. In some cases, adjusting the type and number of medications you are taking may help reduce dry eye symptoms without causing adverse health effects.
However, never discontinue a prescription medication without first discussing the matter with your physician. If your optician feels an adjustment to one of your medications may help relieve dry eye symptoms, he or she can discuss it with your physician (or have you discuss it with your doctor) to see if such a change is possible.
Treating eyelid conditions. If you have blepharitis, meibomian gland dysfunction or other eyelid conditions, these often are associated with dry eye disease and should be addressed as part of your overall dry eye treatment regimen. For example, if you have blepharitis, your optician may recommend use of an antibiotic and/or steroid ointment or eye drop in addition to daily eyelid cleansing with a non-irritating shampoo.
Discontinuing or reducing contact lens wear. If you wear contact lenses, it can be difficult to tell if an underlying dry eye condition is causing contact lens discomfort or if your contact lenses are causing dry eye symptoms. If you wear contacts, it's often best to discontinue wearing them (or perhaps switch to daily disposable contact lenses) while your dry eye treatment is in progress.
Page published on Wednesday, 16 March 2022






