How the COVID-19 delta and omicron variants could affect your eyes

As of early January, nearly all new COVID-19 cases in the U.K. and U.S. were caused by the omicron variant.
The World Health Organization labeled omicron a "variant of concern" on November 26, 2021. Since then, omicron has been detected in more than 110 countries.
Like other coronavirus variants, omicron and delta may be able to cause certain eye-related symptoms, but we don't know for sure yet.
Vaccines are less effective against the omicron and delta variants, but they're still your best form of protection.
An eye test may soon be able to help detect cases of ‘long COVID’.
The COVID-19 omicron variant was discovered in November 2021, and it didn't take long to spread across most of the world. Whenever it's detected in a new location, it usually takes over delta variant infections and becomes the dominant COVID strain in a matter of weeks.
The CDC and UK Health Security Agency estimate that more than 90% of new COVID cases in America and the U.K. are now caused by omicron infections, as of January 1, 2022.
Does the omicron variant affect your eyes?
At this point, it's still too early to know how the newly discovered omicron variant might affect your eyes or vision. And that isn't the only thing we don't know about omicron.
We're still waiting for detailed information about:
How easily omicron spreads.
Exactly how well COVID-19 vaccines protect against omicron.
How severe of an illness it causes compared to other variants.
Early data suggests that the omicron variant could cause a more mild form of COVID-19 than delta and other variants. But that doesn't mean you should let your guard down.
"All variants of COVID-19 … can cause severe disease or death, in particular for the most vulnerable people," the World Health Organization notes.
They emphasize that "prevention is always key," no matter how omicron plays out.
Can the delta variant cause eye symptoms?
We don't know for sure — yet. Previous strains of COVID could cause eye-related symptoms, but there isn't enough scientific data available right now to say with certainty that delta does the same.
There have been isolated reports of delta infections causing eye symptoms, including one fully vaccinated person in Kentucky USA who had bloodshot eyes and flu-like symptoms. According to the Royal Australian College of General Practitioners, the most common symptoms of COVD remain: headache; sore throat; runny nose; fever and persistent cough.
Although not nearly as common as symptoms like cough and fever, other strains of the coronavirus were capable of causing:
Red, bloodshot eyes
Pink eye (conjunctivitis)
Sore eyes
Itchy eyes
Blurry vision
Sensitivity to light
It isn't a stretch to think that some delta infections are capable of causing similar eye symptoms, but, like other aspects of delta, we need to wait for more information.
While each infection is different, delta seems to be causing slightly different symptoms overall than earlier forms of COVID.
"It seems like cough and loss of smell are less common," said Dr. Inci Yildirim, a pediatric infectious disease specialist at Yale Medicine, in an article about the delta variant. "And headache, sore throat, runny nose and fever are present based on the most recent surveys in the U.K., where more than 90% of the cases are due to the Delta strain."
If a set of symptoms that includes runny nose, sore throat and headache sounds familiar, it's because many delta infection symptoms resemble a bad case of seasonal allergies.
This is where eye-related symptoms could get even more confusing.
If you have bad seasonal allergies, you probably know how much allergies can affect your eyes. Red, bloodshot eyes are a hallmark symptom; itchiness, watering and even blurry vision are also common.
The three most widely available COVID-19 vaccines — Pfizer, Moderna and Johnson & Johnson — will still protect you against the delta variant, but not as effectively as they did against previous strains. Fortunately, studies continue to show that these "breakthrough" cases are less common and less severe, on average.
MIS-C: A rare but growing concern in children
As delta finds ways to infect more young people than earlier strains, a rare but serious complication of COVID is also expected to be on the rise.
MIS-C — multisystem inflammatory syndrome in children — can cause vital organs and other parts of the body to become inflamed. It shares similarities with Kawasaki disease, a condition uncovered earlier in the pandemic.
We don't currently know why MIS-C happens to some children.
Symptoms of MIS-C can vary. It can also cause red, bloodshot eyes, but like COVID-19, it's unlikely that would be the only symptom. Additional symptoms occur alongside a fever, according to the CDC.
In addition to a fever, MIS-C symptoms can include:
Bloodshot eyes
Headache
Abdominal pain
Chest pain or tightness
Diarrhea
Fatigue
Neck pain
Low blood pressure
Rash
Vomiting
As of August 22, 2021, there have been 4,661 verified cases of MIS-C in the U.S., with others under investigation. Forty-one children have died from the complication.
While rare, the CDC recommends seeking emergency care if you notice symptoms such as difficulty breathing, chest pain or pressure, pale skin or any other severe symptoms.
The eyes could offer insight into long COVID cases
There's a lot we still don't know about long COVID, the symptoms that linger for weeks or months after the initial infection clears up. Sometimes, symptoms seem to continue indefinitely, significantly impacting a person’s quality of life.
Also known as "long COVID" or "post-acute COVID," long COVID can show up as one or more of a multitude of symptoms. In addition to many others, ongoing symptoms can include:
Fatigue
Changes in taste or smell
Difficulty breathing
Brain fog
Cough
Chest pain
Joint pain
Heart palpitations
Worsening symptoms after physical activity
We don't yet know how often long COVID occurs after a delta infection, or among vaccinated people. One February study found that roughly 30% of people were still experiencing symptoms between three and nine months after having COVID.
About one in 12 participants reported that symptoms affected their ability to complete at least one "activity of daily living," with household chores being the most common.
Long COVID is a developing issue that will continue to affect millions of people for the foreseeable future. Standardised treatment options may not be available yet, but clues to diagnosis could lie in — of all places — the eyes.
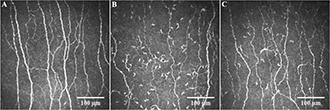
Corneal nerve fibers in a healthy person (A), a COVID-19 patient without long COVID (B) and one with long COVID (C). [Image courtesy: British Journal of Ophthalmology]
There may be a connection between long COVID and damage to microscopic nerve fibers in the cornea, the clear layer in front of the coloured iris, according to a study published in July.
Ophthalmologists used a painless, noninvasive test called a corneal confocal microscopy, a procedure used to diagnose several other conditions that affect the cornea.
While the study acknowledged that more research is needed, the discovery could eventually be a stepping stone toward recovery for people affected by ongoing symptoms, especially neurological.
Getting help from a medical professional
COVID-19's symptoms can be unpredictable, and, like other illnesses, it's important not to self-diagnose. People who experience symptoms are advised to follow the latest guidance from the World Health Organization (WHO) and from the CDC.
If you think that you or someone you know has COVID-19 or long COVID, speak with a medical professional.
If you notice emergency symptoms such as difficulty breathing, chest pain or pressure, confusion or skin discoloration, seek medical attention as soon as possible.
READ NEXT: Can COVID-19 vaccines cause eye-related side effects?
Weekly epidemiological update on COVID-19 - 10 August 2021. World Health Organization. August 2021.
Expert reaction to cases of variant B.1.617 (the ‘Indian variant’) being investigated in the UK. Science Media Centre. April 2021.
Tracking SARS-CoV-2 variants. World Health Organization. August 2021.
Tracking of variants. GISAID. Accessed August 2021.
CDC COVID data tracker. Centers for Disease Control and Prevention. August 2021.
Coronavirus pandemic (COVID-19): Which vaccines have been administered in each country? Our World in Data. August 2021.
About variants of the virus that causes COVID-19. Centers for Disease Control and Prevention. August 2021.
Sore eyes as the most significant ocular symptom experienced by people with COVID-19. BMJ Open Ophthalmology. November 2020.
5 things to know about the delta variant. Yale Medicine. August 2021.
Symptoms of the delta variant vs. previous COVID-19 strains. Baton Rouge General. July 2021.
Is It COVID-19 or allergies? American Academy of Ophthalmology. January 2021.
When you’ve been fully vaccinated. Centers for Disease Control and Prevention. Accessed 6 August 2021.
Health department-reported cases of multisystem inflammatory syndrome in children (MIS-C) in the United States. Centers for Disease Control and Prevention. Accessed 16 August 2021.
For parents: Multisystem inflammatory syndrome in children (MIS-C) associated with COVID-19. Centers for Disease Control and Prevention. Accessed 16 August 2021.
MIS-C and COVID-19: Rare inflammatory syndrome in kids and teens. Johns Hopkins Medicine. July 2021.
Post-COVID conditions. Centers for Disease Control and Prevention. Accessed 6 August 2021.
Sequelae in adults at 6 months after COVID-19 infection. JAMA Network Open. February 2021.
A pandemic that endures for COVID long-haulers. The Harvard Gazette. April 2021.
Corneal confocal microscopy identifies corneal nerve fibre loss and increased dendritic cells in patients with long COVID. British Journal of Ophthalmology. July 2021.
Clinical applications of corneal confocal microscopy. Clinical Ophthalmology. June 2008.
Coronavirus. Prevention. World Health Organization. Accessed August 2021.
Symptoms of COVID-19. Centers for Disease Control and Prevention. Accessed 6 August 2021.
COVID vaccines protect against delta, but their effectiveness wanes. Nature. August 2021.
Effectiveness of COVID-19 vaccines in ambulatory and inpatient care settings. New England Journal of Medicine. September 2021.
Page published on Friday, 20 August 2021






