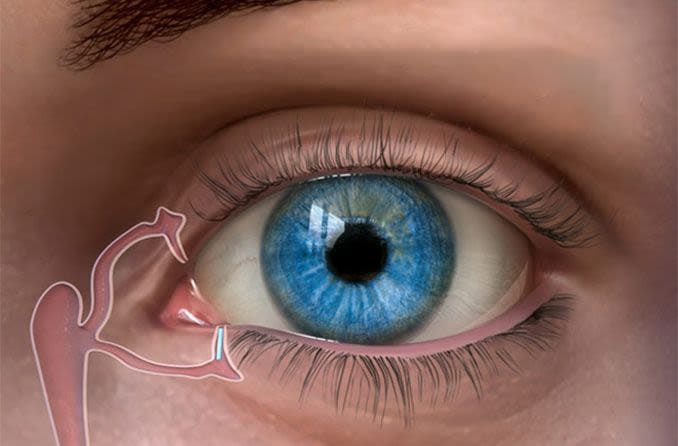
Punctal plugs are tiny, biocompatible devices that can be inserted into tear ducts to block drainage. This increases the eye's tear film and surface moisture to help relieve certain forms of dry eye. Also known as punctum plugs, lacrimal plugs or occluders, these devices often are no larger than a grain of rice.
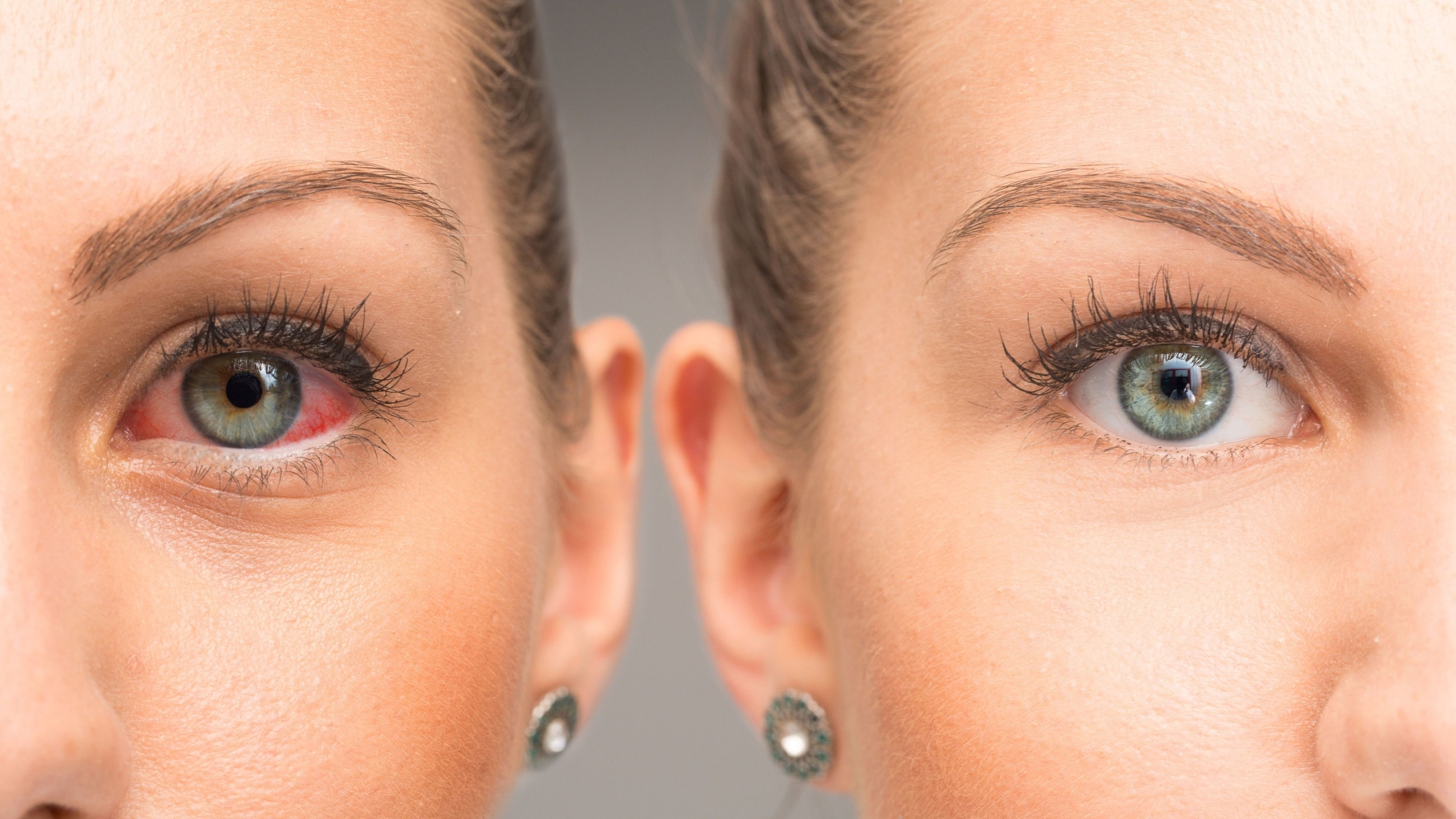
Punctal plugs usually are considered when non-prescription or prescription eye drops fail to relieve your dry eye condition.
Two general types of tear duct plugs are:
Semi-permanent, typically made of long-lasting materials such as silicone.
Dissolvable, made of materials such as collagen that the body eventually absorbs.
Temporary or dissolvable punctal plugs usually last from a few days to as long as several months. These types of plugs would be used in circumstances such as preventing dry eyes after LASIK, if you choose to have refractive surgery.
Dissolvable, temporary punctal plugs sometimes are used to determine if the treatment works for your dry eye condition. If so, then semi-permanent punctal plugs might be considered.
How are punctal plugs inserted in tear ducts?
Depending on the type of punctal plug selected, your eye doctor first may use a special instrument to measure the size of your tear duct openings (puncta). This helps determine the proper size of the punctal plug needed to block drainage within the channel and to keep it securely in place.
Many eye doctors need only a lighted, close-up examination of your eye to determine the size and type of punctal plug you need. In some cases, a one-size-fits-all style of punctal plug may be used.
To prepare you for the procedure, some eye doctors use a local anesthetic before inserting the punctal plug. In many cases, no anesthetic is needed.
Each eyelid has one punctum, located at its inner margin near the nose. Punctal plugs can be inserted in the puncta of the lower lids, the upper lids or both. An instrument may be used to dilate the tear duct opening for easier insertion.
Some punctal plugs are inserted just into the puncta so they still can be seen and mechanically removed if necessary.
Other punctal plugs are inserted deeper into the canaliculus, where they are out of sight. These types of tear duct plugs — technically called intracanalicular plugs — do not protrude from the punctum. They are not seen or felt, and automatically conform to the shape of the cavity. In the uncommon case where removal is needed, intracanalicular plugs are extracted by flushing them out.
Other than slight initial discomfort, you should not feel the punctal plug once it is in place. Immediately after the procedure, you should be able to drive yourself home and resume normal activities.
Punctal plugs side effects and problems
Usually, punctal plug insertion is uneventful and rarely involves serious side effects or problems.
Excessive tearing (epiphora) and watery eyes can occur when the punctal plug does its job too well. In this case, you may need to visit your eye doctor for removal of the plug or replacement with a different type to better control the amount of tears on your eye.
Displacement or loss of the plug is common and can occur for many reasons, such as when people rub their eyes and accidentally dislodge the device.
Eye infections may occur, though rarely, in association with the devices. Canaliculitis results from a rare reaction to punctal plugs, with symptoms such as swelling and yellowish secretions from the tear duct. Such infections may result from upper respiratory infections where blowing the nose under pressure may force germs from the nasal cavity backward into the canaliculus. In these cases, you may need treatment with topical antibiotics, oral antibiotics and/or removal of the punctum plug.
Other uncommon complications can occur when the plug unexpectedly migrates outside the target area and deeper into the eye's drainage channels. This can create blockages leading to conditions such as dacryocystitis, with swelling, pain and discomfort.
When should punctal plugs be removed?
While semi-permanent punctal plugs can last indefinitely, they also are easily removed.
If you feel discomfort or suspect you have an eye infection or other complication, be sure and notify your eye doctor.
If removal is considered necessary, your eye doctor may use forceps to grasp and extract the plug. Another method of removal involves flushing with a saline solution, which forces the punctal plug to exit into the nose or throat where tear ducts drain.
READ NEXT: Lacrimal gland