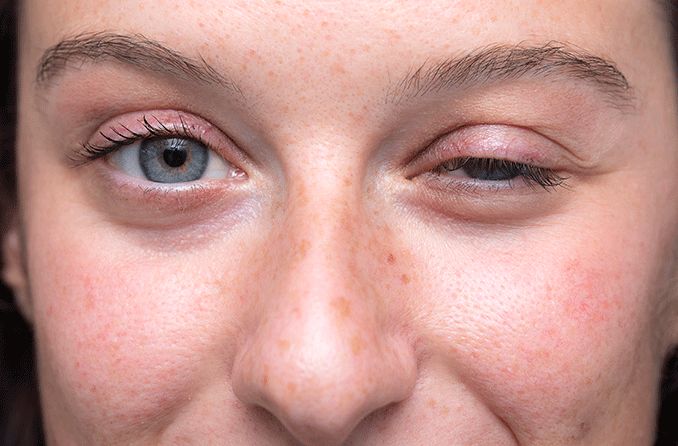
What is ocular rosacea?
Ocular rosacea is related to a common inflammatory condition affecting skin of the face and chest, as well as the eyes. While the exact cause of rosacea is unknown, the condition may be associated with inherited tendencies and environmental factors such as excessive sun exposure.
Rosacea occurs more frequently in women, but men are more likely to have severe forms of the disease. Eye involvement with rosacea is not unusual, although there is no definitive study indicating just how many people have eye or eyelid problems when they are diagnosed with the skin condition.
Recent studies indicate that between 6 to 18 percent of people diagnosed with acne rosacea — so named because it resembles acne — also have ocular symptoms.* Other reports say the number of rosacea patients with eye symptoms could be as high as 60 percent.
Rosacea itself seems to occur in 1 to 10 percent of the general population.**
Symptoms of rosacea and ocular rosacea
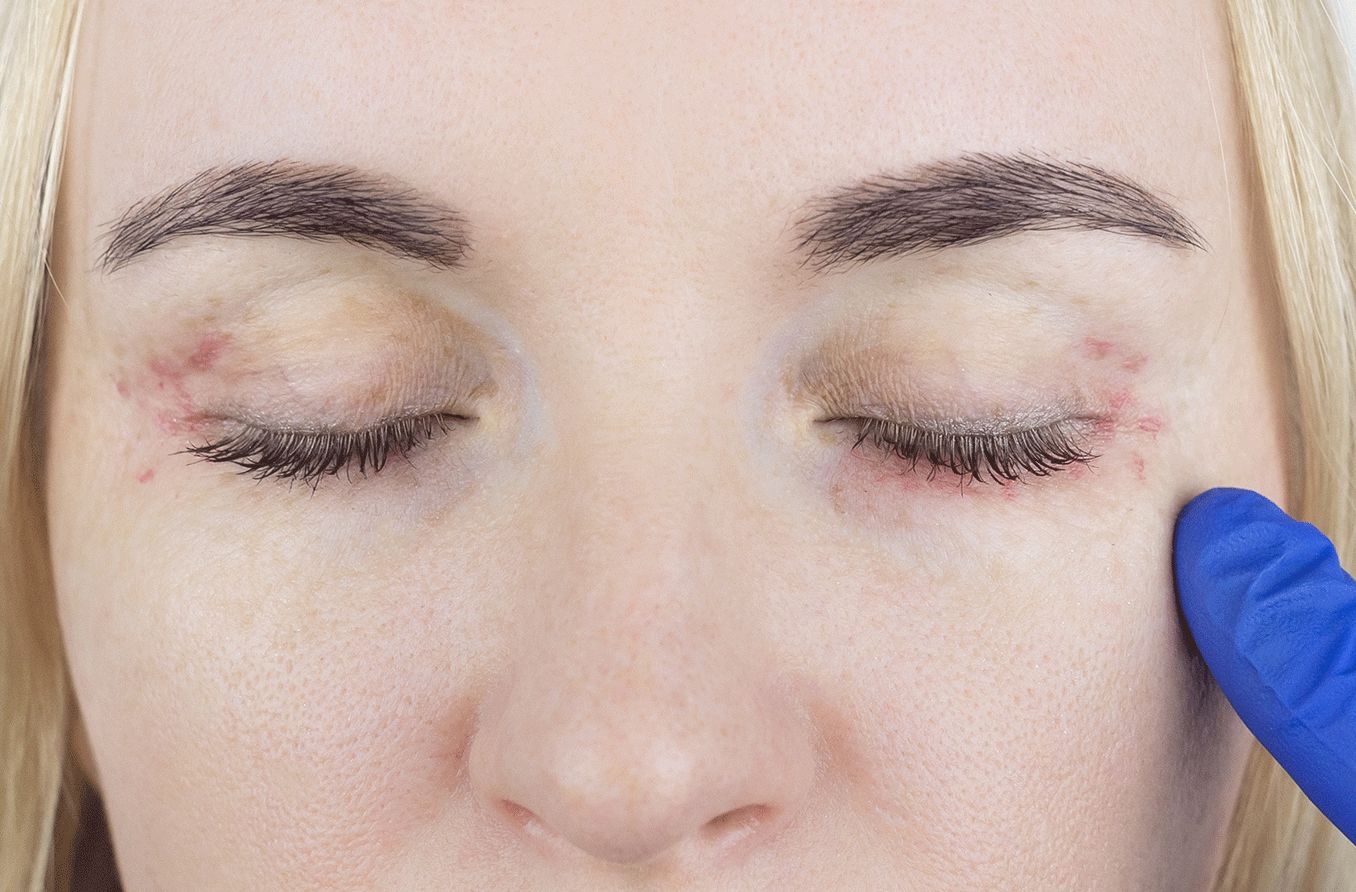
People with rosacea often have a "ruddy" complexion in the early stages, such as a reddish nose and cheeks. These symptoms often progress to include development of bumpy red skin lesions, pimples, and tiny, tortuous vessels in the skin known as telangiectasias (tel-an-jee-ek-TAY-zee-ahs).
The most severe cases of rosacea progress to a condition called rhinophyma (rie-no-FIE-mah), in which the skin thickens along with connective tissues of the nose. Rhinophyma can result in some degree of disfigurement.
When you have rosacea affecting the skin, you may not realize that your eyes also are involved if accompanying symptoms such as eye itchiness and eye redness are relatively mild.
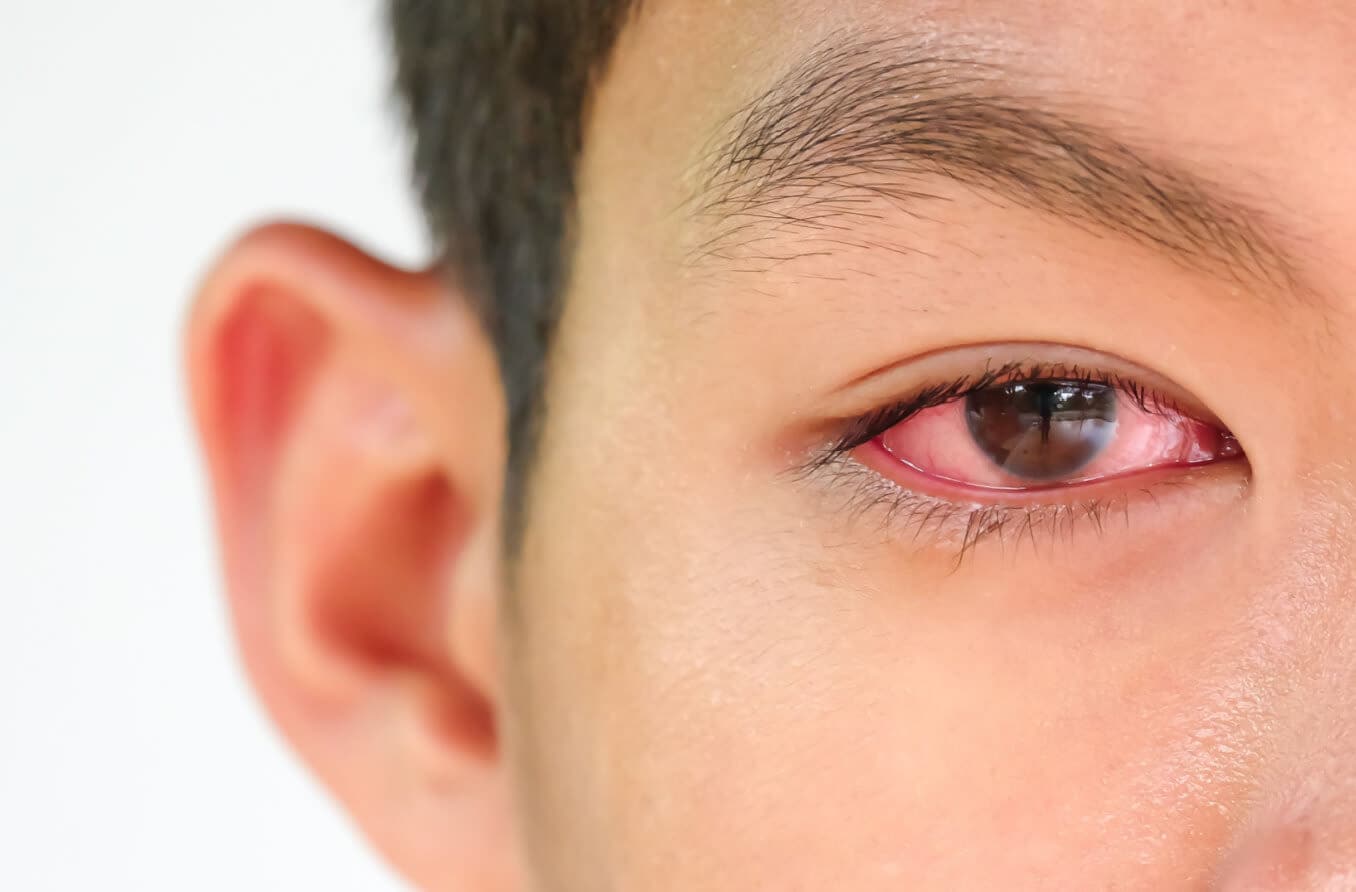
People diagnosed with ocular rosacea commonly have chronically bloodshot eyes, dry eyes and blepharitis.
Ocular rosacea can cause photophobia (unusual sensitivity to light). If you are bothered by bright light, ask your eye care professional about photochromic lenses that automatically darken in response to sunlight.
In cases of severe ocular rosacea, inflammation of the cornea may lead to a corneal ulcer with infection. If left untreated, the corneal ulcer may even perforate the eye. This is a serious and potentially blinding complication.
SEE RELATED: Eyelid eczema: Causes, symptoms and treatment

Treatments for ocular rosacea
Effective treatment of rosacea requires a highly motivated patient willing to devote the time it takes to control the condition.
When ocular rosacea is present, treatment usually consists of lid hygiene measures that include daily cleansing:
- Moistened Q-tips can remove debris and oily secretions.
- Some eye doctors advise cleansing with dilute baby shampoo, while others believe plain water is best.
Often, an antibiotic or combination antibiotic-steroid ointment is prescribed for varying periods of time, depending on response. For example, tetracyclines tend to work well for rosacea, not only because of the antibiotic effect, but because tetracyclines tend to decrease the viscosity of naturally secreted oils, thereby reducing the oil gland "plugging" that occurs with this disease.
Most eye doctors will prescribe long-acting tetracyclines such as doxycycline, which can be taken once or twice a day. Furthermore, doxycycline, unlike traditional tetracycline, can be taken with food and milk products without preventing absorption in the body.
If you have rosacea, avoid "triggers" such as spicy foods and alcohol, which can cause inflammation.
Dry eye syndrome, which often accompanies rosacea, should be treated with non-preserved artificial tears (eye drops) as often as four times daily or more. A home humidifier also may help.
If these measures are insufficient, punctal plugs can easily close the tear drainage ducts. Punctal plugs can be removed if necessary, but another possible measure is punctal cautery (burning of the tear duct openings), which is relatively permanent.
Finally, topical metronidazole (an anti-parasitic agent) may be used on the skin and in many people is very effective for the rosacea-related dermatitis. The medicine appears to have local anti-inflammatory and immunosuppressive effects. Because this treatment is not available in ophthalmic preparations, you should not apply the medicine directly to eyelids.
If you have rosacea, your doctor will likely advise you to avoid triggers that may cause inflammation, such as stress, spicy foods and alcohol.
SEE RELATED: Eyelid psoriasis: Causes, symptoms and treatment
Marilyn Haddrill also contributed to this article.